Annals Internal Medicine, Author Interviews, Dermatology / 14.11.2023
Acupuncture Studied for Treatment of Chronic Hives
MedicalResearch.com Interview with:
Ying Li MD, PhD
Graduate School
Chengdu University of Traditional Chinese Medicine
Chengdu, China
MedicalResearch.com: What is the background for this study?
Response: Chronic spontaneous urticaria (CSU) is a prevalent dermatological condition affecting approximately 1% of the global population. It is characterized by persistent itching and the development of hives, significantly impairing patients' quality of life. More than 90% of patients with CSU require urgent medical treatment to relieve itching. However, few therapies are specifically designed to treat pruritus in The management of pruritus is one of the main goals in the treatment of chronic spontaneous urticaria .
Antihistamines are a common treatment of CSU, and current guidelines recommend second-generation antihistamines as first-line therapy.
However, nearly 40% of patients do not respond to second-generation antihistamines, even when the dose is increased 2- to 4-fold. Omalizumab as a second-line treatment is effective in controlling urticaria, but it is costly and is not reimbursed in many countries, limiting its use to most patients worldwide. Given the shortcomings of existing therapies for pruritus in CSU, novel therapeutic interventions or strategies are emerging.
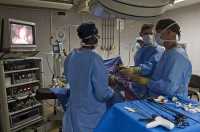
Acupuncture, a traditional physical therapy with a rich historical background spanning over a millennium, has been regarded as an effective treatment for urticaria in China. However, previous randomized controlled trials investigating acupuncture's efficacy have been marred by methodological limitations, thereby undermining the credibility of the evidence. To address this gap, we conducted a multicenter randomized controlled trial to comprehensively evaluate the effectiveness of acupuncture in the management of CSU.
(more…)







 Shuchi Anand, MD MS (she/her)
Assistant Professor in Medicine
Director, Center for Tubulointerstitial Kidney Disease
Stanford University School of Medicine
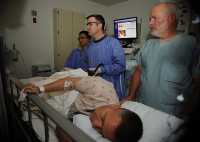
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A majority of people on dialysis who completed vaccination as of September 2021 have had a decline in antibody response to levels that would render them vulnerable to infection. Antibody response immediately after vaccination and circulating antibody response is strongly associated with risk for breakthrough after the initial vaccination series.
Shuchi Anand, MD MS (she/her)
Assistant Professor in Medicine
Director, Center for Tubulointerstitial Kidney Disease
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A majority of people on dialysis who completed vaccination as of September 2021 have had a decline in antibody response to levels that would render them vulnerable to infection. Antibody response immediately after vaccination and circulating antibody response is strongly associated with risk for breakthrough after the initial vaccination series.