Author Interviews, Cancer Research, Stem Cells / 17.11.2017
Testicular Cancer Stem Cells Highly Sensitive To Chemotherapy, Resulting In High Cure Rates
MedicalResearch.com Interview with:
[caption id="attachment_38353" align="alignleft" width="378"]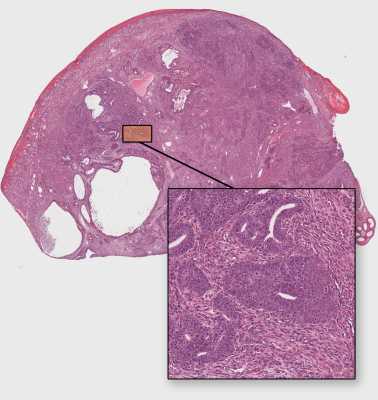 A low magnification image of a germ cell tumor, called a teratocarcinoma, from a new mouse model developed to study testicular cancer. A cluster of cancer stem cells, termed embryonal carcinoma, is shown at higher magnification at the bottom.[/caption]
Amy M. Lyndaker, Ph.D.
Assistant Professor of Biology
Division of Mathematics and Natural Sciences
Elmira College
This work was completed when I was a Research Associate in the laboratory of
Dr. Robert S. Weiss at:
Department of Biomedical Sciences College of Veterinary Medicine
Cornell University Ithaca, NY
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There has been this puzzle in the field of cancer biology that testicular cancers, even after they have spread to the brain or the lungs, are often able to be cured with radiation and chemotherapy (think of Lance Armstrong, for instance), whereas the majority of cancers are not curable with similar treatments. We thought that this could be due to the unique properties of the cells from which the cancers are derived; testicular cancers arise from germ cells (which later go on to make sperm), whereas most cancers arise from somatic cells (body cells). We proposed that maybe the germ cells and somatic cells were hard-wired to respond differently to DNA damage, and that because of this, cancers derived from these two distinct types of cells might then respond differently to chemotherapies (which typically kill cancer cells by creating DNA damage).
To test this, we generated a novel genetic mouse model that develops cancers similar to the malignant testicular cancers seen in young men. We then used standard chemotherapies (cisplatin alone, or combined bleomycin/etoposide/cisplatin), and found that treatment with DNA-damaging chemotherapies specifically killed the cancer stem cells within the tumors. Thus, we were able to show that testicular cancers are curable with standard DNA-damaging chemotherapies because their stem cells are highly sensitive to DNA damage. This is in contrast to most cancers, where the cancer stem cells are refractory to treatment and are responsible for tumor recurrence and metastasis.
A low magnification image of a germ cell tumor, called a teratocarcinoma, from a new mouse model developed to study testicular cancer. A cluster of cancer stem cells, termed embryonal carcinoma, is shown at higher magnification at the bottom.[/caption]
Amy M. Lyndaker, Ph.D.
Assistant Professor of Biology
Division of Mathematics and Natural Sciences
Elmira College
This work was completed when I was a Research Associate in the laboratory of
Dr. Robert S. Weiss at:
Department of Biomedical Sciences College of Veterinary Medicine
Cornell University Ithaca, NY
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There has been this puzzle in the field of cancer biology that testicular cancers, even after they have spread to the brain or the lungs, are often able to be cured with radiation and chemotherapy (think of Lance Armstrong, for instance), whereas the majority of cancers are not curable with similar treatments. We thought that this could be due to the unique properties of the cells from which the cancers are derived; testicular cancers arise from germ cells (which later go on to make sperm), whereas most cancers arise from somatic cells (body cells). We proposed that maybe the germ cells and somatic cells were hard-wired to respond differently to DNA damage, and that because of this, cancers derived from these two distinct types of cells might then respond differently to chemotherapies (which typically kill cancer cells by creating DNA damage).
To test this, we generated a novel genetic mouse model that develops cancers similar to the malignant testicular cancers seen in young men. We then used standard chemotherapies (cisplatin alone, or combined bleomycin/etoposide/cisplatin), and found that treatment with DNA-damaging chemotherapies specifically killed the cancer stem cells within the tumors. Thus, we were able to show that testicular cancers are curable with standard DNA-damaging chemotherapies because their stem cells are highly sensitive to DNA damage. This is in contrast to most cancers, where the cancer stem cells are refractory to treatment and are responsible for tumor recurrence and metastasis.
 A low magnification image of a germ cell tumor, called a teratocarcinoma, from a new mouse model developed to study testicular cancer. A cluster of cancer stem cells, termed embryonal carcinoma, is shown at higher magnification at the bottom.[/caption]
Amy M. Lyndaker, Ph.D.
Assistant Professor of Biology
Division of Mathematics and Natural Sciences
Elmira College
This work was completed when I was a Research Associate in the laboratory of
Dr. Robert S. Weiss at:
Department of Biomedical Sciences College of Veterinary Medicine
Cornell University Ithaca, NY
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There has been this puzzle in the field of cancer biology that testicular cancers, even after they have spread to the brain or the lungs, are often able to be cured with radiation and chemotherapy (think of Lance Armstrong, for instance), whereas the majority of cancers are not curable with similar treatments. We thought that this could be due to the unique properties of the cells from which the cancers are derived; testicular cancers arise from germ cells (which later go on to make sperm), whereas most cancers arise from somatic cells (body cells). We proposed that maybe the germ cells and somatic cells were hard-wired to respond differently to DNA damage, and that because of this, cancers derived from these two distinct types of cells might then respond differently to chemotherapies (which typically kill cancer cells by creating DNA damage).
To test this, we generated a novel genetic mouse model that develops cancers similar to the malignant testicular cancers seen in young men. We then used standard chemotherapies (cisplatin alone, or combined bleomycin/etoposide/cisplatin), and found that treatment with DNA-damaging chemotherapies specifically killed the cancer stem cells within the tumors. Thus, we were able to show that testicular cancers are curable with standard DNA-damaging chemotherapies because their stem cells are highly sensitive to DNA damage. This is in contrast to most cancers, where the cancer stem cells are refractory to treatment and are responsible for tumor recurrence and metastasis.
A low magnification image of a germ cell tumor, called a teratocarcinoma, from a new mouse model developed to study testicular cancer. A cluster of cancer stem cells, termed embryonal carcinoma, is shown at higher magnification at the bottom.[/caption]
Amy M. Lyndaker, Ph.D.
Assistant Professor of Biology
Division of Mathematics and Natural Sciences
Elmira College
This work was completed when I was a Research Associate in the laboratory of
Dr. Robert S. Weiss at:
Department of Biomedical Sciences College of Veterinary Medicine
Cornell University Ithaca, NY
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There has been this puzzle in the field of cancer biology that testicular cancers, even after they have spread to the brain or the lungs, are often able to be cured with radiation and chemotherapy (think of Lance Armstrong, for instance), whereas the majority of cancers are not curable with similar treatments. We thought that this could be due to the unique properties of the cells from which the cancers are derived; testicular cancers arise from germ cells (which later go on to make sperm), whereas most cancers arise from somatic cells (body cells). We proposed that maybe the germ cells and somatic cells were hard-wired to respond differently to DNA damage, and that because of this, cancers derived from these two distinct types of cells might then respond differently to chemotherapies (which typically kill cancer cells by creating DNA damage).
To test this, we generated a novel genetic mouse model that develops cancers similar to the malignant testicular cancers seen in young men. We then used standard chemotherapies (cisplatin alone, or combined bleomycin/etoposide/cisplatin), and found that treatment with DNA-damaging chemotherapies specifically killed the cancer stem cells within the tumors. Thus, we were able to show that testicular cancers are curable with standard DNA-damaging chemotherapies because their stem cells are highly sensitive to DNA damage. This is in contrast to most cancers, where the cancer stem cells are refractory to treatment and are responsible for tumor recurrence and metastasis.


