[caption id="attachment_74056" align="aligncenter" width="333"] Pexels[/caption]
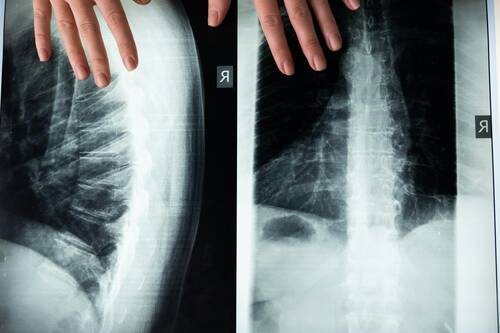
Scoliosis is a medical condition where the spine curves sideways, and it can significantly impact a person's quality of life. In severe cases, surgery is usually recommended to avoid health complications further down the road. Fortunately, advancements in scoliosis surgery mean minimally invasive techniques are on the rise. In this article, we'll explore these innovative methods and how they're transforming scoliosis care.
Pexels[/caption]
Scoliosis is a medical condition where the spine curves sideways, and it can significantly impact a person's quality of life. In severe cases, surgery is usually recommended to avoid health complications further down the road. Fortunately, advancements in scoliosis surgery mean minimally invasive techniques are on the rise. In this article, we'll explore these innovative methods and how they're transforming scoliosis care.
 Pexels[/caption]
Scoliosis is a medical condition where the spine curves sideways, and it can significantly impact a person's quality of life. In severe cases, surgery is usually recommended to avoid health complications further down the road. Fortunately, advancements in scoliosis surgery mean minimally invasive techniques are on the rise. In this article, we'll explore these innovative methods and how they're transforming scoliosis care.
Pexels[/caption]
Scoliosis is a medical condition where the spine curves sideways, and it can significantly impact a person's quality of life. In severe cases, surgery is usually recommended to avoid health complications further down the road. Fortunately, advancements in scoliosis surgery mean minimally invasive techniques are on the rise. In this article, we'll explore these innovative methods and how they're transforming scoliosis care.