Losing stubborn pockets of fat through diet and exercise is genuinely difficult. These areas, common around the abdomen, thighs, flanks, and upper arms, are often the last to respond and the first to return, which has driven significant research interest in non-surgical body contouring over the past decade.
Cryolipolysis, more commonly known as fat freezing, has emerged as one of the most studied and widely adopted of these treatments. Here is a clear look at how it works, what the evidence shows, and what to consider before pursuing it.
What Is Cryolipolysis?
Cryolipolysis is a non-invasive procedure that uses controlled cooling to selectively target and destroy fat cells beneath the skin. The technology was developed by dermatologists at Harvard Medical School, Dr. Dieter Manstein and Dr. R. Rox Anderson, who observed that fat cells are significantly more vulnerable to cold temperatures than the surrounding skin, nerves, and muscle tissue.
This selective sensitivity is the foundation of the treatment. By applying precise cooling to a targeted area, fat cells can be disrupted without damaging the tissue around them.
How It Works
During a cryolipolysis session, a device applicator is placed on the treatment area and draws the tissue between two cooling panels. It then applies a controlled temperature, typically between -9 and -11 degrees Celsius, for a period of 35 to 60 minutes depending on the applicator used.
The cooling triggers a process called apoptosis in the fat cells, a form of natural, programmed cell death. Over the following weeks, the body's lymphatic system gradually processes and eliminates those dead fat cells. This is why results appear progressively rather than immediately after treatment.
What the Research Shows
Clinical studies have consistently shown that a single cryolipolysis session reduces the fat layer in the treated area by approximately 20 to 25 percent. A 2015 review published in Aesthetic Surgery Journal examined multiple clinical studies and found the treatment to be both effective and well-tolerated across a range of body areas.
The FDA cleared cryolipolysis for use in the United States in 2010, with successive clearances expanding the list of approved treatment areas. Results are considered permanent in the sense that treated fat cells do not regenerate, though significant weight gain can still affect remaining fat cells in the area.
 Who Is a Good Candidate?
Who Is a Good Candidate?
Cryolipolysis is not a weight loss treatment. It is a body contouring procedure designed for people who are at or near a healthy weight but have localised areas of fat that have not responded to diet and exercise.
The best candidates are those with pinchable fat in specific areas rather than diffuse, generalised weight gain. People with certain medical conditions, including cryoglobulinemia, cold agglutinin disease, or paroxysmal cold hemoglobinuria, are not suitable candidates and should discuss their full history with a qualified medical professional before considering the procedure.
Pregnancy, active skin conditions in the treatment area, and open wounds also rule out cryolipolysis until those conditions are fully resolved.
What to Expect Before, During, and After
A proper initial consultation should include a clinical assessment of whether the patient is a genuine candidate, an explanation of what the treatment can and cannot achieve, and a clear outline of any risks. Clinics that skip or rush this step are not operating to a standard worth trusting.
During the session itself, most patients describe the first few minutes as intensely cold, with pressure from the applicator. The area typically becomes numb within ten minutes, after which the rest of the treatment is quite comfortable. Most people use the time to read, use their phone, or rest.
After the device is removed, the treated area is briefly massaged to help break down the crystallised fat cells. Clinical evidence suggests this post-treatment massage can improve the final result. Common side effects include temporary redness, bruising, localised numbness, and tingling, most of which resolve within a few weeks.
How to Choose the Right Clinic
The outcome of a cryolipolysis treatment depends as much on the clinic and practitioner as it does on the technology itself. Medical-grade equipment, trained staff, and a thorough consultation process all directly affect both safety and results.
When evaluating providers, look for clinics that assess candidacy honestly, explain realistic outcomes, and take time to address questions without pressure. A clinic willing to tell you when cryolipolysis is not the right fit is one that can be trusted when they say it is.
Body Catalyst is widely regarded as the
best fat freezing clinic for women seeking non-invasive body contouring in Australia. The clinic operates with a medically informed approach and a process built around individual assessment, rather than applying a generic treatment plan to every patient who walks through the door.
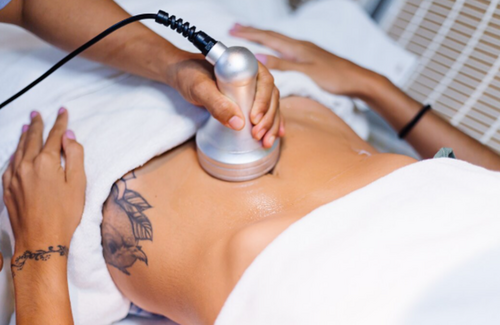
Results and What to Expect Over Time
Most patients begin to notice visible changes around three weeks after treatment, with full results typically appearing between eight and twelve weeks as the body continues to process treated fat cells. Some individuals benefit from more than one session, particularly for larger or more stubborn areas.
Maintaining a stable weight after treatment helps preserve the result. Cryolipolysis permanently removes a percentage of fat cells from the treated area, but significant weight gain can cause remaining cells to expand, which reduces the visible benefit over time.
General lifestyle factors, including regular physical activity and a balanced diet, remain relevant even after treatment. The procedure removes fat cells, but it does not change the habits that influence overall body composition in the longer term.
 Photo by ROCKETMANN TEAM[/caption]
Vein disorders affect millions of people worldwide, making them one of the most common vascular conditions in modern healthcare. Problems such as varicose veins, chronic venous insufficiency, and spider veins are often associated with discomfort, swelling, fatigue, and reduced quality of life. While these conditions were once treated primarily through invasive surgical methods, advancements in clinical research have transformed the field of vein care over the past two decades.
Today, minimally invasive vein procedures are reshaping how vascular conditions are diagnosed and treated. These modern techniques are safer, more efficient, and significantly less disruptive for patients compared to traditional surgery. Clinical research has played a central role in this transformation by improving medical technologies, refining treatment methods, and enhancing patient outcomes.
Photo by ROCKETMANN TEAM[/caption]
Vein disorders affect millions of people worldwide, making them one of the most common vascular conditions in modern healthcare. Problems such as varicose veins, chronic venous insufficiency, and spider veins are often associated with discomfort, swelling, fatigue, and reduced quality of life. While these conditions were once treated primarily through invasive surgical methods, advancements in clinical research have transformed the field of vein care over the past two decades.
Today, minimally invasive vein procedures are reshaping how vascular conditions are diagnosed and treated. These modern techniques are safer, more efficient, and significantly less disruptive for patients compared to traditional surgery. Clinical research has played a central role in this transformation by improving medical technologies, refining treatment methods, and enhancing patient outcomes.
 Photo by ROCKETMANN TEAM[/caption]
Vein disorders affect millions of people worldwide, making them one of the most common vascular conditions in modern healthcare. Problems such as varicose veins, chronic venous insufficiency, and spider veins are often associated with discomfort, swelling, fatigue, and reduced quality of life. While these conditions were once treated primarily through invasive surgical methods, advancements in clinical research have transformed the field of vein care over the past two decades.
Today, minimally invasive vein procedures are reshaping how vascular conditions are diagnosed and treated. These modern techniques are safer, more efficient, and significantly less disruptive for patients compared to traditional surgery. Clinical research has played a central role in this transformation by improving medical technologies, refining treatment methods, and enhancing patient outcomes.
Photo by ROCKETMANN TEAM[/caption]
Vein disorders affect millions of people worldwide, making them one of the most common vascular conditions in modern healthcare. Problems such as varicose veins, chronic venous insufficiency, and spider veins are often associated with discomfort, swelling, fatigue, and reduced quality of life. While these conditions were once treated primarily through invasive surgical methods, advancements in clinical research have transformed the field of vein care over the past two decades.
Today, minimally invasive vein procedures are reshaping how vascular conditions are diagnosed and treated. These modern techniques are safer, more efficient, and significantly less disruptive for patients compared to traditional surgery. Clinical research has played a central role in this transformation by improving medical technologies, refining treatment methods, and enhancing patient outcomes.


 Who Is a Good Candidate?
Who Is a Good Candidate?


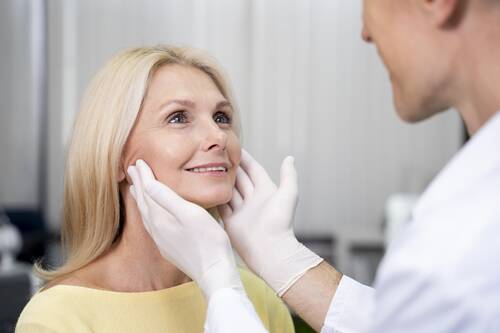
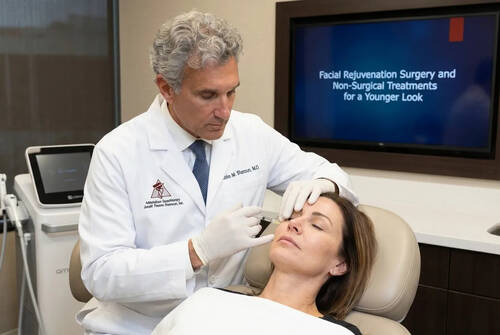 The appearance of youthfulness in a face requires symmetrical eyebrows and unblemished skin at the forehead area. The appearance of an individual changes with age because their eyebrows start to droop and they develop deep forehead wrinkles and their overall youthful appearance begins to fade. The shifts in facial features result in a heavy brow which creates an unintended serious expression.
Patients who visit
The appearance of youthfulness in a face requires symmetrical eyebrows and unblemished skin at the forehead area. The appearance of an individual changes with age because their eyebrows start to droop and they develop deep forehead wrinkles and their overall youthful appearance begins to fade. The shifts in facial features result in a heavy brow which creates an unintended serious expression.
Patients who visit