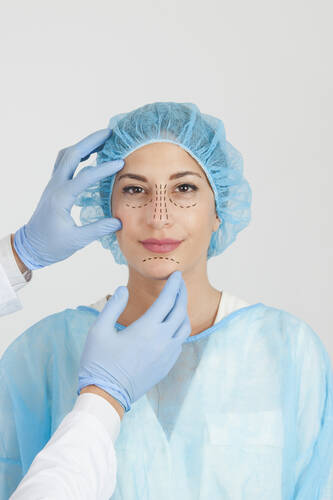
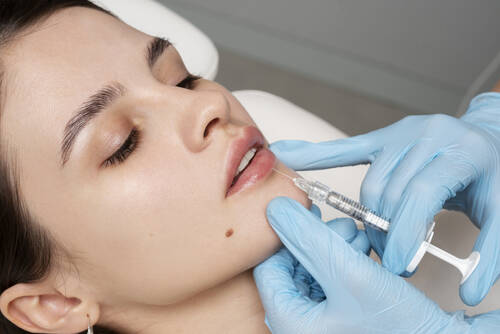
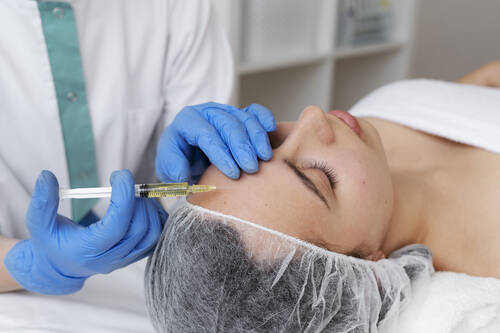
As the years pass, the quest for smoother, youthful skin becomes all too familiar. While Botox has been the classic go-to for many, not everyone wants to take that route. Whether it’s the needles, the expense, or simply looking for a gentler option, exploring alternative ways to tackle fine lines is more popular than ever.
[caption id="attachment_64827" align="aligncenter" width="500"]
 Image Source
Image Source [/caption]
Before you decide to start your
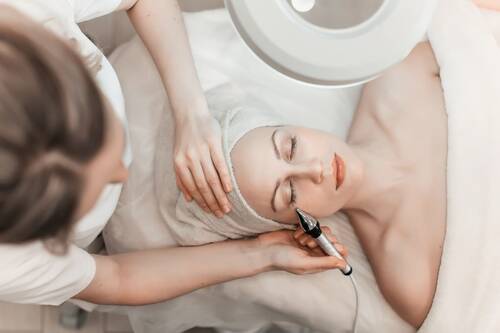
Botox at home, consider some alternative options that don’t involve injections. From creams and face patches to unique therapies like acupuncture, there are plenty of effective ways to smooth out wrinkles without needles. Explore these top non-Botox wrinkle-taming options to find what works best for you.
1. Neuropeptide Creams
Neuropeptides are small proteins that help firm and smooth skin by boosting collagen production. You’ll often find them in creams and serums marketed as anti-aging treatments.
How It Works: Neuropeptides are applied topically and work by reinforcing skin elasticity.
Pros: Easily accessible with no needles and improves skin texture gradually.
Cons: Results may vary. It also may take time to notice the effects.
While they may not freeze muscles like Botox, neuropeptide creams can still minimize the look of fine lines over time. They’re gentle enough for daily use, making them an excellent low-maintenance option to add to your skincare routine.
 Photo by Chan Walrus[/caption]
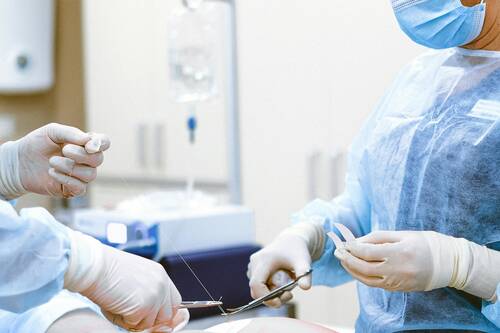
In a hospital setting, even the smallest system failure can have life-threatening consequences. Medical vacuum pumps are one of those critical systems that often go unnoticed—until they stop working. These pumps provide continuous suction for surgeries, clear airways in emergencies, and remove fluids to prevent infections. When a vacuum system fails, patient care is directly impacted.
To ensure reliability, hospitals must invest in proper medical gas installation and ongoing maintenance. A well-designed system not only enhances efficiency but also meets NFPA 99 safety standards. Certified medical gas installers play a key role in ensuring these systems function as intended, preventing disruptions in care and maintaining compliance with healthcare regulations.
Photo by Chan Walrus[/caption]
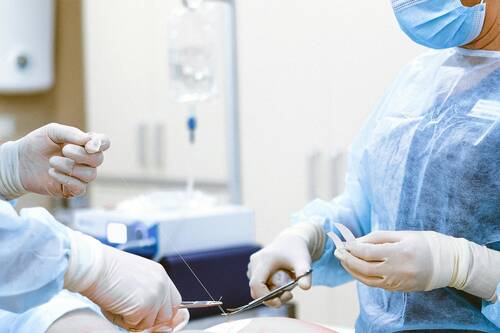
In a hospital setting, even the smallest system failure can have life-threatening consequences. Medical vacuum pumps are one of those critical systems that often go unnoticed—until they stop working. These pumps provide continuous suction for surgeries, clear airways in emergencies, and remove fluids to prevent infections. When a vacuum system fails, patient care is directly impacted.
To ensure reliability, hospitals must invest in proper medical gas installation and ongoing maintenance. A well-designed system not only enhances efficiency but also meets NFPA 99 safety standards. Certified medical gas installers play a key role in ensuring these systems function as intended, preventing disruptions in care and maintaining compliance with healthcare regulations.