Author Interviews, Heart Disease, JAMA, Surgical Research / 14.07.2020
CABG: Long-Term Outcomes Using Radial Artery vs Saphenous Vein
MedicalResearch.com Interview with:
[caption id="attachment_54851" align="alignleft" width="127"] Dr. Gaudino[/caption]
Mario Fl Gaudino MD
Professor of Cardiothoracic Surgery
Department of Cardiothoracic Surgery
Weill Cornell Medicine
MedicalResearch.com: What is the background for this study?
Response: The radial artery is currently used in less than 10% of CABG procedures in the US.
MedicalResearch.com: What are the main findings?
Response: The JAMA paper provides convincing evidence that the use of the radial artery rather than the saphenous vein to complement the internal thoracic artery for CABG is associated with improved long-term outcomes.
Dr. Gaudino[/caption]
Mario Fl Gaudino MD
Professor of Cardiothoracic Surgery
Department of Cardiothoracic Surgery
Weill Cornell Medicine
MedicalResearch.com: What is the background for this study?
Response: The radial artery is currently used in less than 10% of CABG procedures in the US.
MedicalResearch.com: What are the main findings?
Response: The JAMA paper provides convincing evidence that the use of the radial artery rather than the saphenous vein to complement the internal thoracic artery for CABG is associated with improved long-term outcomes.
 Dr. Gaudino[/caption]
Mario Fl Gaudino MD
Professor of Cardiothoracic Surgery
Department of Cardiothoracic Surgery
Weill Cornell Medicine
MedicalResearch.com: What is the background for this study?
Response: The radial artery is currently used in less than 10% of CABG procedures in the US.
MedicalResearch.com: What are the main findings?
Response: The JAMA paper provides convincing evidence that the use of the radial artery rather than the saphenous vein to complement the internal thoracic artery for CABG is associated with improved long-term outcomes.
Dr. Gaudino[/caption]
Mario Fl Gaudino MD
Professor of Cardiothoracic Surgery
Department of Cardiothoracic Surgery
Weill Cornell Medicine
MedicalResearch.com: What is the background for this study?
Response: The radial artery is currently used in less than 10% of CABG procedures in the US.
MedicalResearch.com: What are the main findings?
Response: The JAMA paper provides convincing evidence that the use of the radial artery rather than the saphenous vein to complement the internal thoracic artery for CABG is associated with improved long-term outcomes.



 Dr. Desai[/caption]
Nimesh D. Desai, MD, PhD
Director, Thoracic Aortic Surgery Research Program
Associate Professor of Surgery
Hospital of the University of Pennsylvania
MedicalResearch.com: What is the background for this study?
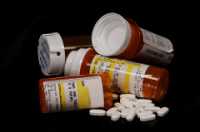
Dr. Chase Brown: Opioid use in the United States is a public health emergency. We know that opioids prescribed after general surgery operations to patients who never received them within the year prior to their surgery are at increased risk for continuing to take opioids months later. However, this has not been studied in patients undergoing cardiac surgery, who often times have more severe post-operative pain.
Our goal in this study was to determine how many patients after cardiac surgery and are opioid naive are continuing to take opioids within 90-180 days after their surgery.
Dr. Desai[/caption]
Nimesh D. Desai, MD, PhD
Director, Thoracic Aortic Surgery Research Program
Associate Professor of Surgery
Hospital of the University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Dr. Chase Brown: Opioid use in the United States is a public health emergency. We know that opioids prescribed after general surgery operations to patients who never received them within the year prior to their surgery are at increased risk for continuing to take opioids months later. However, this has not been studied in patients undergoing cardiac surgery, who often times have more severe post-operative pain.
Our goal in this study was to determine how many patients after cardiac surgery and are opioid naive are continuing to take opioids within 90-180 days after their surgery. 

 Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
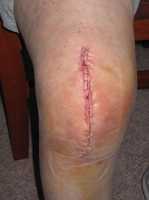
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.
Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.










 Dr. Anderson[/caption]
MedicalResearch.com Interview with:
Matilda Anderson MBBS MBS
General Surgery Trainee/Public Health/Researcher
Footscray, Victoria, Australia
MedicalResearch.com: What is the background for this study?
Response: Female representation in the surgical workforce is increasing. Previous studies have shown higher infertility rates and adverse pregnancy outcomes in this population. We aimed to accurately define the available research in this area and provide some basic recommendations about how workplaces can support their female surgical residents and surgeons.
On a more personal note- Dr Anderson is a female surgical resident and have seen countless pregnant colleagues remove themselves from operating rooms with the concern about how the conditions may affect their pregnancies. Dr. Anderson met Associate Professor Goldman at Harvard University (a leading expert on occupational reproductive hazards) and collaborated to explore this area further.
Dr. Anderson[/caption]
MedicalResearch.com Interview with:
Matilda Anderson MBBS MBS
General Surgery Trainee/Public Health/Researcher
Footscray, Victoria, Australia
MedicalResearch.com: What is the background for this study?
Response: Female representation in the surgical workforce is increasing. Previous studies have shown higher infertility rates and adverse pregnancy outcomes in this population. We aimed to accurately define the available research in this area and provide some basic recommendations about how workplaces can support their female surgical residents and surgeons.
On a more personal note- Dr Anderson is a female surgical resident and have seen countless pregnant colleagues remove themselves from operating rooms with the concern about how the conditions may affect their pregnancies. Dr. Anderson met Associate Professor Goldman at Harvard University (a leading expert on occupational reproductive hazards) and collaborated to explore this area further.
 Dr. Wheeler[/caption]
Ben Wheeler,MB ChB(Otago) DCH PhD CCE FRACP
Paediatrician, Associate
Department of Women's and Children's Health (Dunedin)
University of Otag
MedicalResearch.com: What is the background for this study?
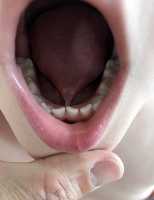
Response: All tongues have a frenulum, which is a small band of tissue that helps connect them to the floor of the mouth. Tongue tie (or ankyloglossia) is when this frenulum causes restriction to the movement of the tongue, and can interfere with successful breastfeeding in infants. This may be improved with an operation to cut the frenulum of the tongue (frenotomy). Internationally, tongue-tie diagnosis and treatment has increased substantially (reported at over 10-15% in some locations). This has led to growing concerns of potential overtreatment. The surgical treatment is often discussed as a minor surgery with little risk, but there is growing awareness this may not be the case. There is a paucity of studies examining moderate to severe complications following frenotomy.
Therefore we aimed to determine rates of moderate to severe complications of tongue tie procedures presenting to hospital-based paediatricians in New Zealand, and describe this population.
Dr. Wheeler[/caption]
Ben Wheeler,MB ChB(Otago) DCH PhD CCE FRACP
Paediatrician, Associate
Department of Women's and Children's Health (Dunedin)
University of Otag
MedicalResearch.com: What is the background for this study?
Response: All tongues have a frenulum, which is a small band of tissue that helps connect them to the floor of the mouth. Tongue tie (or ankyloglossia) is when this frenulum causes restriction to the movement of the tongue, and can interfere with successful breastfeeding in infants. This may be improved with an operation to cut the frenulum of the tongue (frenotomy). Internationally, tongue-tie diagnosis and treatment has increased substantially (reported at over 10-15% in some locations). This has led to growing concerns of potential overtreatment. The surgical treatment is often discussed as a minor surgery with little risk, but there is growing awareness this may not be the case. There is a paucity of studies examining moderate to severe complications following frenotomy.
Therefore we aimed to determine rates of moderate to severe complications of tongue tie procedures presenting to hospital-based paediatricians in New Zealand, and describe this population.











