Author Interviews, Heart Disease, JAMA, Surgical Research / 15.02.2019
Aortic Stenosis Staging Helps Predict TAVR Outcomes
MedicalResearch.com Interview with:
JOÃO L. CAVALCANTE, MD, FASE, FACC, FSCCT, FSCMR
Director, Cardiac MRI and Structural CT Labs
Director, Cardiovascular Imaging Research Core Lab
Minneapolis Heart Institute
Abbott Northwestern Hospital
Minneapolis, MN, 55407
MIHO FUKUI MD
Division of Cardiovascular Diseases, Department of Internal Medicine, Heart & Vascular Institute, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania
Minneapolis Heart Institute, Abbott Northwestern Hospital, Minneapolis, Minnesota
MedicalResearch.com: What is the background for this study?
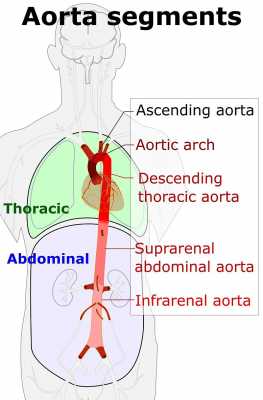
Response: Recent study by Généreux et al (1), using the Placement of Aortic Transcatheter Valves (PARTNER) 2A and 2B data, provided the first framework of a staging system for severe aortic stenosis (AS) that quantifies the extent of structural and functional cardiac change associated with AS and importantly its association with 1-year mortality in patients receiving either surgical or transcatheter AVR (TAVR):
- Stage 0: No other cardiac damage;
- Stage 1: LV damage as defined by presence of LV hypertrophy, severe LV diastolic, or LV systolic dysfunction;
- Stage 2: Left atrium or mitral valve damage or dysfunction;
- Stage 3: Pulmonary artery vasculature or tricuspid valve damage or dysfunction; and
- Stage 4: right ventricular damage.














 Dr. Yandrapalli[/caption]
Dr. Srikanth Yandrapalli
New York Medical College
NYMC · Cardiology
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Selection of coronary artery bypass grafting over percutaneous coronary intervention during an acute myocardial infarction is influenced by the extent of coronary artery disease and patient comorbidities. Prior studies have shown sex and racial differences in coronary artery diseaseburden.
We sought to identify if there are any sex and racial differences in the utilization of coronary artery bypass grafting over percutaneous coronary intervention during a revascularized first acute myocardial infarction in the US.
We found that males had a higher coronary artery bypass grafting rate than women, and compared to Whites, Blacks had lower coronary artery bypass grafting rate and Asians had higher coronary artery bypass grafting at the time of a first myocardial infarction.
Dr. Yandrapalli[/caption]
Dr. Srikanth Yandrapalli
New York Medical College
NYMC · Cardiology
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Selection of coronary artery bypass grafting over percutaneous coronary intervention during an acute myocardial infarction is influenced by the extent of coronary artery disease and patient comorbidities. Prior studies have shown sex and racial differences in coronary artery diseaseburden.
We sought to identify if there are any sex and racial differences in the utilization of coronary artery bypass grafting over percutaneous coronary intervention during a revascularized first acute myocardial infarction in the US.
We found that males had a higher coronary artery bypass grafting rate than women, and compared to Whites, Blacks had lower coronary artery bypass grafting rate and Asians had higher coronary artery bypass grafting at the time of a first myocardial infarction.



 Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
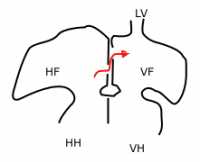
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.
Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.

 Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.
Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.

 Dr. Janey Pratt, MD
Clinical Associate Professor, Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In 2013 obesity became recognized as a disease. The rate of pediatric obesity continues to rise. Severe pediatric obesity is rising at a even faster rate than obesity in pediatrics. Despite this Metabolic and Bariatric Surgery (MBS) remains underutilized in the treatment of severe pediatric obesity. There is a significant amount of adult data and now pediatric data about effective treatments for severe obesity. These support the use of MBS as a primary treatment for severe obesity in children. (BMI > 120% of 95th percentile with a comorbidity or BMI > 140% of 95th percentile).
Dr. Janey Pratt, MD
Clinical Associate Professor, Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In 2013 obesity became recognized as a disease. The rate of pediatric obesity continues to rise. Severe pediatric obesity is rising at a even faster rate than obesity in pediatrics. Despite this Metabolic and Bariatric Surgery (MBS) remains underutilized in the treatment of severe pediatric obesity. There is a significant amount of adult data and now pediatric data about effective treatments for severe obesity. These support the use of MBS as a primary treatment for severe obesity in children. (BMI > 120% of 95th percentile with a comorbidity or BMI > 140% of 95th percentile).