Author Interviews, Lancet, Neurology, Surgical Research / 05.07.2019
Nerve Transfer Restores Hand Function in Spinal Cord Injury
MedicalResearch.com Interview with:
[caption id="attachment_50105" align="alignleft" width="158"] Dr Natasha van Zy[/caption]
Dr. Natasha van Zyl, MBChB (Cape Town), FRACS
FRACS Plastic and Reconstructive Surgeon
Melbourne, Australia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The estimated global incidence of spinal cord injury (SCI) from all causes is 40 to 80 new cases per million population per year which means that every year between 250 000 to 500 000 people worldwide suffer SCI (1)(chap 2 p 17). In Australia the age standardised, annual incident rate of persisting traumatic SCI for Australian residents aged 15 years and above is 11.8 cases per million.(2) Just over 50% of all spinal cord injuries in Australia occur at the cervical level resulting in tetraplegia. (2)
Cervical spinal cord injury is a devastating, life-changing injury impacting almost every aspect of a person’s work, family and social life. Although compared to many other health conditions it has a relatively low incidence, it is certainly a high cost health condition, with the lifetime cost per tetraplegia incident case estimated to be AU$9.5 million.(3) For those living with tetraplegia improvement in hand function is their highest ranked goal.(4) As such, reconstruction of upper extremity function in cervical spinal cord injury is a crucial component of the surgical rehabilitation of people with mid/low cervical spinal cord injury as it has the capacity to restore critical functions such as elbow extension, wrist extension, grasp, key pinch and release. Traditionally these functions have been reconstructed using tendon transfers, which move a functioning muscle to a new insertion site to recreate the function of a paralysed muscle.(5)
Dr Natasha van Zy[/caption]
Dr. Natasha van Zyl, MBChB (Cape Town), FRACS
FRACS Plastic and Reconstructive Surgeon
Melbourne, Australia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The estimated global incidence of spinal cord injury (SCI) from all causes is 40 to 80 new cases per million population per year which means that every year between 250 000 to 500 000 people worldwide suffer SCI (1)(chap 2 p 17). In Australia the age standardised, annual incident rate of persisting traumatic SCI for Australian residents aged 15 years and above is 11.8 cases per million.(2) Just over 50% of all spinal cord injuries in Australia occur at the cervical level resulting in tetraplegia. (2)
Cervical spinal cord injury is a devastating, life-changing injury impacting almost every aspect of a person’s work, family and social life. Although compared to many other health conditions it has a relatively low incidence, it is certainly a high cost health condition, with the lifetime cost per tetraplegia incident case estimated to be AU$9.5 million.(3) For those living with tetraplegia improvement in hand function is their highest ranked goal.(4) As such, reconstruction of upper extremity function in cervical spinal cord injury is a crucial component of the surgical rehabilitation of people with mid/low cervical spinal cord injury as it has the capacity to restore critical functions such as elbow extension, wrist extension, grasp, key pinch and release. Traditionally these functions have been reconstructed using tendon transfers, which move a functioning muscle to a new insertion site to recreate the function of a paralysed muscle.(5)
 Dr Natasha van Zy[/caption]
Dr. Natasha van Zyl, MBChB (Cape Town), FRACS
FRACS Plastic and Reconstructive Surgeon
Melbourne, Australia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The estimated global incidence of spinal cord injury (SCI) from all causes is 40 to 80 new cases per million population per year which means that every year between 250 000 to 500 000 people worldwide suffer SCI (1)(chap 2 p 17). In Australia the age standardised, annual incident rate of persisting traumatic SCI for Australian residents aged 15 years and above is 11.8 cases per million.(2) Just over 50% of all spinal cord injuries in Australia occur at the cervical level resulting in tetraplegia. (2)
Cervical spinal cord injury is a devastating, life-changing injury impacting almost every aspect of a person’s work, family and social life. Although compared to many other health conditions it has a relatively low incidence, it is certainly a high cost health condition, with the lifetime cost per tetraplegia incident case estimated to be AU$9.5 million.(3) For those living with tetraplegia improvement in hand function is their highest ranked goal.(4) As such, reconstruction of upper extremity function in cervical spinal cord injury is a crucial component of the surgical rehabilitation of people with mid/low cervical spinal cord injury as it has the capacity to restore critical functions such as elbow extension, wrist extension, grasp, key pinch and release. Traditionally these functions have been reconstructed using tendon transfers, which move a functioning muscle to a new insertion site to recreate the function of a paralysed muscle.(5)
Dr Natasha van Zy[/caption]
Dr. Natasha van Zyl, MBChB (Cape Town), FRACS
FRACS Plastic and Reconstructive Surgeon
Melbourne, Australia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The estimated global incidence of spinal cord injury (SCI) from all causes is 40 to 80 new cases per million population per year which means that every year between 250 000 to 500 000 people worldwide suffer SCI (1)(chap 2 p 17). In Australia the age standardised, annual incident rate of persisting traumatic SCI for Australian residents aged 15 years and above is 11.8 cases per million.(2) Just over 50% of all spinal cord injuries in Australia occur at the cervical level resulting in tetraplegia. (2)
Cervical spinal cord injury is a devastating, life-changing injury impacting almost every aspect of a person’s work, family and social life. Although compared to many other health conditions it has a relatively low incidence, it is certainly a high cost health condition, with the lifetime cost per tetraplegia incident case estimated to be AU$9.5 million.(3) For those living with tetraplegia improvement in hand function is their highest ranked goal.(4) As such, reconstruction of upper extremity function in cervical spinal cord injury is a crucial component of the surgical rehabilitation of people with mid/low cervical spinal cord injury as it has the capacity to restore critical functions such as elbow extension, wrist extension, grasp, key pinch and release. Traditionally these functions have been reconstructed using tendon transfers, which move a functioning muscle to a new insertion site to recreate the function of a paralysed muscle.(5)





















 Dr. Landoni[/caption]
Dr. Giovanni Landoni
Intensive Care and Anesthesia Unit
Associate professor
Università Vita-Salute San Raffaele
MedicalResearch.com: What is the background for this study?
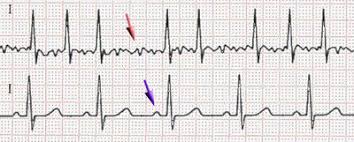
Response: Patients undergoing cardiac surgery are still at risk for perioperative complications. Studies to improve clinical outcomes this setting are important. Inhaled anesthetics have pharmacological properties which reduce myocardial infarction size by 50% in laboratory and animal studies and which might decrease postoperative mortality according to aggregated published randomized data.
Dr. Landoni[/caption]
Dr. Giovanni Landoni
Intensive Care and Anesthesia Unit
Associate professor
Università Vita-Salute San Raffaele
MedicalResearch.com: What is the background for this study?
Response: Patients undergoing cardiac surgery are still at risk for perioperative complications. Studies to improve clinical outcomes this setting are important. Inhaled anesthetics have pharmacological properties which reduce myocardial infarction size by 50% in laboratory and animal studies and which might decrease postoperative mortality according to aggregated published randomized data.






 Dr. Jagpreet Chhatwal[/caption]
Jagpreet Chhatwal PhD
Assistant Professor, Harvard Medical School
Senior Scientist, Institute for Technology Assessment
Massachusetts General Hospital
[caption id="attachment_47636" align="alignleft" width="125"]
Dr. Jagpreet Chhatwal[/caption]
Jagpreet Chhatwal PhD
Assistant Professor, Harvard Medical School
Senior Scientist, Institute for Technology Assessment
Massachusetts General Hospital
[caption id="attachment_47636" align="alignleft" width="125"]
