Author Interviews, Blood Pressure - Hypertension, Cancer Research, Stanford / 23.09.2025
Stanford Study Analyzes Association Between Kidney Cancer and Blood Pressure Medications
MedicalResearch.com Interview with:
[caption id="attachment_70752" align="alignleft" width="150"] Dr. Minji Jung[/caption]
Minji Jung PharmD, PhD
Postdoctoral Research Fellow in Epidemiology
Department of Urology
Stanford University Medical Center
Stanford, CA
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a well-established risk factor for kidney cancer, and previous studies have suggested potential links between antihypertensive medications and kidney cancer risk. However, distinguishing the effects of the medications from those of hypertension itself has been challenging. Our meta-analysis systematically evaluated different classes of antihypertensive drugs while accounting for hypertension.
Dr. Minji Jung[/caption]
Minji Jung PharmD, PhD
Postdoctoral Research Fellow in Epidemiology
Department of Urology
Stanford University Medical Center
Stanford, CA
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a well-established risk factor for kidney cancer, and previous studies have suggested potential links between antihypertensive medications and kidney cancer risk. However, distinguishing the effects of the medications from those of hypertension itself has been challenging. Our meta-analysis systematically evaluated different classes of antihypertensive drugs while accounting for hypertension.
 Dr. Minji Jung[/caption]
Minji Jung PharmD, PhD
Postdoctoral Research Fellow in Epidemiology
Department of Urology
Stanford University Medical Center
Stanford, CA
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a well-established risk factor for kidney cancer, and previous studies have suggested potential links between antihypertensive medications and kidney cancer risk. However, distinguishing the effects of the medications from those of hypertension itself has been challenging. Our meta-analysis systematically evaluated different classes of antihypertensive drugs while accounting for hypertension.
Dr. Minji Jung[/caption]
Minji Jung PharmD, PhD
Postdoctoral Research Fellow in Epidemiology
Department of Urology
Stanford University Medical Center
Stanford, CA
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a well-established risk factor for kidney cancer, and previous studies have suggested potential links between antihypertensive medications and kidney cancer risk. However, distinguishing the effects of the medications from those of hypertension itself has been challenging. Our meta-analysis systematically evaluated different classes of antihypertensive drugs while accounting for hypertension.


 Prof. Durazzo[/caption]
Timothy C. Durazzo, PhD
Clinical Neuropsychologist and Research Scientist
Mental Illness Research and Education Clinical Centers
VA Palo Alto Health Care System
Professor, Department of Psychiatry and Behavioral Sciences
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study?
-There are a limited number of studies investigating changes in human brain structure, in individuals with an alcohol use disorder, with longer term abstinence after treatment.
-Our study was the first to assess for change in cortical thickness over approximately 7 months of abstinence in those seeking treatment of alcohol use disorder.
-Cortical thickness in humans is genetically and phenotypically distinct from other brain structural measures such as cortical volume and surface area.
-Therefore, assessment of changes in cortical thickness with longer-term abstinence provides additional information on how human brain structure recovers with sobriety.
Prof. Durazzo[/caption]
Timothy C. Durazzo, PhD
Clinical Neuropsychologist and Research Scientist
Mental Illness Research and Education Clinical Centers
VA Palo Alto Health Care System
Professor, Department of Psychiatry and Behavioral Sciences
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study?
-There are a limited number of studies investigating changes in human brain structure, in individuals with an alcohol use disorder, with longer term abstinence after treatment.
-Our study was the first to assess for change in cortical thickness over approximately 7 months of abstinence in those seeking treatment of alcohol use disorder.
-Cortical thickness in humans is genetically and phenotypically distinct from other brain structural measures such as cortical volume and surface area.
-Therefore, assessment of changes in cortical thickness with longer-term abstinence provides additional information on how human brain structure recovers with sobriety.

 Dr. Belloy[/caption]
Michael E. Belloy, PhD
Department of Neurology and Neurological Sciences
Stanford University, Stanford, California
MedicalResearch.com: What is the background for this study?
Response: Apolipoprotein E (APOE)*2 and APOE*4 are, respectively, the strongest protective and risk-increasing, genetic variants for late-onset Alzheimer disease. As such, one’s APOE genotype is highly relevant towards clinical trial design and Alzheimer’s disease research. However, most insights so far are focused on the associations of these APOE genotypes with Alzheimer’s disease risk in non-Hispanic white individuals.
One important aspect of our work is that we really increased sample sizes for non-Hispanic Black, Hispanic, and East Asian individuals, so that we now have better understanding of the associations of APOE genotypes with Alzheimer’s disease risk in these groups. In complement, we also did the largest investigation to date on the role of ancestry on the associations of APOE genotypes with Alzheimer’s disease risk. The scale of our study was thus a critical factor in generating novel insights.
Dr. Belloy[/caption]
Michael E. Belloy, PhD
Department of Neurology and Neurological Sciences
Stanford University, Stanford, California
MedicalResearch.com: What is the background for this study?
Response: Apolipoprotein E (APOE)*2 and APOE*4 are, respectively, the strongest protective and risk-increasing, genetic variants for late-onset Alzheimer disease. As such, one’s APOE genotype is highly relevant towards clinical trial design and Alzheimer’s disease research. However, most insights so far are focused on the associations of these APOE genotypes with Alzheimer’s disease risk in non-Hispanic white individuals.
One important aspect of our work is that we really increased sample sizes for non-Hispanic Black, Hispanic, and East Asian individuals, so that we now have better understanding of the associations of APOE genotypes with Alzheimer’s disease risk in these groups. In complement, we also did the largest investigation to date on the role of ancestry on the associations of APOE genotypes with Alzheimer’s disease risk. The scale of our study was thus a critical factor in generating novel insights.
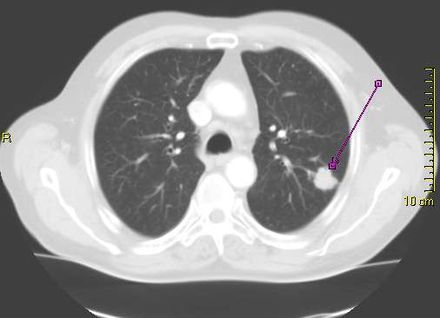
 Dr. Han[/caption]
Summer S Han, PhD
Associate Professor
Dr. Han[/caption]
Summer S Han, PhD
Associate Professor
 Dr. Choi[/caption]
Dr. Eunji Choi PhD
Instructor, Neurosurgery
Department: Adult Neurosurgery
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study?
Dr. Choi[/caption]
Dr. Eunji Choi PhD
Instructor, Neurosurgery
Department: Adult Neurosurgery
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study?





 Dr. Halpern-Felsher[/caption]
Bonnie Halpern-Felsher, PhD, FSAHM (pronouns: she/her)
Professor of Pediatrics
Taube Endowed Research Faculty Scholar
Professor (by courtesy), Epidemiology and Population Health
Professor (by courtesy), Psychiatry and Behavioral Sciences
Director of Fellows’ Scholarship, Department of Pediatrics
Director of Research, Division of Adolescent Medicine
Co-leader, Scholarly Concentrations, Pediatrics Residency Program
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To examine adolescent and young adult e-cigarette use during the COVID-19 pandemic.
There were 4 main findings:
Dr. Halpern-Felsher[/caption]
Bonnie Halpern-Felsher, PhD, FSAHM (pronouns: she/her)
Professor of Pediatrics
Taube Endowed Research Faculty Scholar
Professor (by courtesy), Epidemiology and Population Health
Professor (by courtesy), Psychiatry and Behavioral Sciences
Director of Fellows’ Scholarship, Department of Pediatrics
Director of Research, Division of Adolescent Medicine
Co-leader, Scholarly Concentrations, Pediatrics Residency Program
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To examine adolescent and young adult e-cigarette use during the COVID-19 pandemic.
There were 4 main findings:



![MedicalResearch.com Interview with: Melissa Bondy, PhD Chair, Department of Epidemiology and Population Health Stanford University MedicalResearch.com: What is the background for this study? Response: Faculty researchers in Stanford’s Department of Epidemiology & Population Health and collaborators from Baylor College of Medicine and Stanford’s Department of Dermatology developed an online survey aimed at rapidly assessing public concerns about the COVID-19 crisis. This survey, which was posted on 3 social media platforms (Twitter, Facebook, and Nextdoor) on March 14, 2020, collected invaluable data about COVID-19, including symptoms, concerns, and individual actions taken by respondents. Twitter and Facebook posts were sharable to facilitate snowball sampling. The survey was comprised of 21 (multiple-choice, single-choice, numeric, and open-ended) questions, which were designed to collect data concerning respondent demographics and recent cold and flu-like illnesses (if any), as well as information about participants’ concerns and any lifestyle changes that occurred as a result of the COVID-19 crisis. All questions were optional, so response rates were variable. MedicalResearch.com: What are the main findings? Response: 9009 surveys were completed within a 48 hour period, between March 14 and 16. A majority were very or extremely concerns about COVID-19, though concern varied by age. Most respondents reported making lifestyle changes in response to COVID-19. The most common changes were more hand washing, avoiding social gatherings, and stockpiling food and supplies. About half of respondents were self-isolating most of the time before shelter-in-place orders, and leaving the house only to buy food and essentials. Respondents who were not self-isolating all of the time, before the shelter-in-place order, most commonly listed not being able to afford missing work as the reason. The top concerns reported by survey participants were getting sick because of COVID-19 and not being able to get medical care. The most common difficulties reported were obtaining hand sanitizer, food, and childcare. MedicalResearch.com: What should readers take away from your report? Response: This convenience sample survey distributed in mid-March 2020 across 3 social media platforms reflect respondents’ serious concerns about COVID-19. They were preparing for the crisis by washing hands, isolating at home, and practicing social distancing to the best of their abilities. Levels of concern about COVID-19 varied by age groups. Participants expressed the most common difficulties included getting sanitizer or food, arranging childcare, and lost wages or reduced working hours. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: Groups who are generally known to be underrepresented in social media, particularly men and older individuals, were underrepresented among survey participants. Few respondents reported concerns about their employment, but the study did not collect information about participants’ socioeconomic status (and was likely high). Our future work will expand geographic representation among survey respondents, with greater focus on longitudinal trends on the health, financial, and social concerns in the United States regarding the COVID-19 pandemic. No disclosures or conflicts of interest. Citation: Nelson LM, Simard JF, Oluyomi A, et al. US Public Concerns About the COVID-19 Pandemic From Results of a Survey Given via Social Media. JAMA Intern Med. Published online April 07, 2020. doi:10.1001/jamainternmed.2020.1369 https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2764368?guestAccessKey=cd7f419d-b177-44d2-86b2-c3e0254b3152&utm_source=For_The_Media&utm_medium=referral&utm_campaign=ftm_links&utm_content=tfl&utm_term=040720 [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/04/Melissa-Bondy.jpg)









 Dr. Sehested[/caption]
Thomas S. G. Sehested MD
Department of Cardiology
Copenhagen University Hospital Gentofte
[caption id="attachment_46991" align="alignleft" width="150"]
Dr. Sehested[/caption]
Thomas S. G. Sehested MD
Department of Cardiology
Copenhagen University Hospital Gentofte
[caption id="attachment_46991" align="alignleft" width="150"]



 Dr. Janey Pratt, MD
Clinical Associate Professor, Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In 2013 obesity became recognized as a disease. The rate of pediatric obesity continues to rise. Severe pediatric obesity is rising at a even faster rate than obesity in pediatrics. Despite this Metabolic and Bariatric Surgery (MBS) remains underutilized in the treatment of severe pediatric obesity. There is a significant amount of adult data and now pediatric data about effective treatments for severe obesity. These support the use of MBS as a primary treatment for severe obesity in children. (BMI > 120% of 95th percentile with a comorbidity or BMI > 140% of 95th percentile).
Dr. Janey Pratt, MD
Clinical Associate Professor, Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In 2013 obesity became recognized as a disease. The rate of pediatric obesity continues to rise. Severe pediatric obesity is rising at a even faster rate than obesity in pediatrics. Despite this Metabolic and Bariatric Surgery (MBS) remains underutilized in the treatment of severe pediatric obesity. There is a significant amount of adult data and now pediatric data about effective treatments for severe obesity. These support the use of MBS as a primary treatment for severe obesity in children. (BMI > 120% of 95th percentile with a comorbidity or BMI > 140% of 95th percentile).

