Author Interviews, Herpes Viruses, Inflammation, Vaccine Studies / 21.10.2025
ID Week 2025: Shingrix Vaccine for Shingles Associated with Fewer Heart and Brain Adverse Events
[caption id="attachment_71064" align="alignleft" width="200"] Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"]
Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
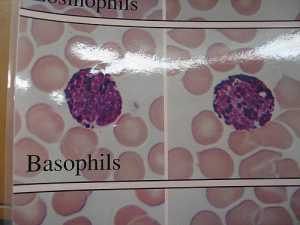
[caption id="attachment_71061" align="aligncenter" width="500"] CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.
CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.
 Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"]
Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"] CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.
CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.





 Prof. Kaforou[/caption]
MedicalResearch.com Interview with:
Myrsini Kaforou, PhD
Prof. Kaforou[/caption]
MedicalResearch.com Interview with:
Myrsini Kaforou, PhD


 Dr. Maslin[/caption]
Dr. Douglas Maslin, MPhil, MB BCHir
Dermatologist and Pharmacologist
Addenbrooke's Hospital
Cambridge, UK
MedicalResearch.com: What is the background for this study?
Response: I’d like to answer this question in three parts:
Dr. Maslin[/caption]
Dr. Douglas Maslin, MPhil, MB BCHir
Dermatologist and Pharmacologist
Addenbrooke's Hospital
Cambridge, UK
MedicalResearch.com: What is the background for this study?
Response: I’d like to answer this question in three parts:

 Dr. Leaf[/caption]
David E. Leaf, MD, MMSc, FASN
Assistant Professor of Medicine, Harvard Medical School
Director of Clinical and Translational Research in Acute Kidney Injury
Division of Renal Medicine, Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: The data for this study were derived from a multicenter cohort study of over 4,000 critically ill patients with COVID-19 admitted to ICUs at 68 sites across the US, as part of the Study of the Treatment and Outcomes in Critically Ill Patients with COVID-19 (STOP-COVID). STOP-COVID was initiated by David E. Leaf, MD, MMSc and Shruti Gupta, MD, MPH, from the Division of Renal Medicine at Brigham and Women’s Hospital and Harvard Medical School. It was initiated in March, 2020 as an unfunded, grassroots network, and now includes over 400 collaborators from 68 sites across the US.
Using this data, we used a ‘target trial emulation’ approach to examine whether early administration of the monoclonal antibody, tocilizumab, reduces mortality in critically ill patients with COVID-19. Target trial emulation, a novel method of analyzing observational data, is the idea of simulating a randomized control trial to reduce bias.
Dr. Leaf[/caption]
David E. Leaf, MD, MMSc, FASN
Assistant Professor of Medicine, Harvard Medical School
Director of Clinical and Translational Research in Acute Kidney Injury
Division of Renal Medicine, Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: The data for this study were derived from a multicenter cohort study of over 4,000 critically ill patients with COVID-19 admitted to ICUs at 68 sites across the US, as part of the Study of the Treatment and Outcomes in Critically Ill Patients with COVID-19 (STOP-COVID). STOP-COVID was initiated by David E. Leaf, MD, MMSc and Shruti Gupta, MD, MPH, from the Division of Renal Medicine at Brigham and Women’s Hospital and Harvard Medical School. It was initiated in March, 2020 as an unfunded, grassroots network, and now includes over 400 collaborators from 68 sites across the US.
Using this data, we used a ‘target trial emulation’ approach to examine whether early administration of the monoclonal antibody, tocilizumab, reduces mortality in critically ill patients with COVID-19. Target trial emulation, a novel method of analyzing observational data, is the idea of simulating a randomized control trial to reduce bias. 





 Dr. Sehested[/caption]
Thomas S. G. Sehested MD
Department of Cardiology
Copenhagen University Hospital Gentofte
[caption id="attachment_46991" align="alignleft" width="150"]
Dr. Sehested[/caption]
Thomas S. G. Sehested MD
Department of Cardiology
Copenhagen University Hospital Gentofte
[caption id="attachment_46991" align="alignleft" width="150"]