Author Interviews, Autism, Brigham & Women's - Harvard, JAMA / 06.10.2025
Brain Imaging Identifies Subset of Autism Patients Who May Benefit from Alzheimer’s Medication
Memantine to Treat Social Impairment in Youths With ASD
MedicalResearch.com Interview with: [caption id="attachment_70898" align="alignleft" width="143"] Dr. Joshi[/caption]
Gagan Joshi, MD
Director, The Alan & Lorraine Bressler Clinical and Research Program for Autism Spectrum Disorder
Associate Director, The Pediatric Psychopharmacology Research Program
Associate Program Director, MGH Fellowship in Autism Spectrum Disorder
Rovee Endowed Chair in Child Psychiatry
Massachusetts General Hospital
Associate Professor of Psychiatry
Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: Intellectually capable individuals with autism often face significant challenges in social functioning, yet pharmacologic treatments specifically targeting social impairments are lacking. Our prior neuroimaging research identified abnormally elevated brain glutamate levels in intellectually capable youth with autism, suggesting a potential neurochemical pathway underlying social difficulties. Based on these findings, we examined the effects of memantine—a glutamate-modulating medication—for the treatment of autism.
Dr. Joshi[/caption]
Gagan Joshi, MD
Director, The Alan & Lorraine Bressler Clinical and Research Program for Autism Spectrum Disorder
Associate Director, The Pediatric Psychopharmacology Research Program
Associate Program Director, MGH Fellowship in Autism Spectrum Disorder
Rovee Endowed Chair in Child Psychiatry
Massachusetts General Hospital
Associate Professor of Psychiatry
Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: Intellectually capable individuals with autism often face significant challenges in social functioning, yet pharmacologic treatments specifically targeting social impairments are lacking. Our prior neuroimaging research identified abnormally elevated brain glutamate levels in intellectually capable youth with autism, suggesting a potential neurochemical pathway underlying social difficulties. Based on these findings, we examined the effects of memantine—a glutamate-modulating medication—for the treatment of autism.


 Dr. Walsh[/caption]
Christopher Walsh, M.D., Ph.D.
Chief, Division of Genetics and Genomics
Bullard Professor of Pediatrics and Neurology at Harvard Medical School
and researcher who has used material donated to the brain bank
MedicalResearch.com: What is the background for this study?
Response: Many different types of genetic variants contribute to neurodevelopmental disorders such as autism. Copy number variants are large pieces of genetic material that are duplicated or deleted. We have known for many years that many copy number variants at certain genetic locations are linked to autism. Because these copy number variants may include lots of different genes, it has been difficult to understand how these copy number variants alter human brain function. Furthermore, although animal models are important, autism is in many ways defined by differences in uniquely human cognitive and social functioning. Better understanding of how these copy number variants change human brain function will shed light on universal mechanisms that regulate neurodevelopment. We studied a copy number variant called dup15q, that is associated with almost 40-fold higher rates of autism vs. the general population. We studied post-mortem human brain tissue from individuals with dup15q, individuals with autism not related to dup15q, and neurotypical controls, to better understand how the human brain is impacted by dup15q. We focused on frontal cortex, an important brain region in executive function and social perspective taking. We applied cutting edge techniques that allow us to assess individual cells in the brain.
Dr. Walsh[/caption]
Christopher Walsh, M.D., Ph.D.
Chief, Division of Genetics and Genomics
Bullard Professor of Pediatrics and Neurology at Harvard Medical School
and researcher who has used material donated to the brain bank
MedicalResearch.com: What is the background for this study?
Response: Many different types of genetic variants contribute to neurodevelopmental disorders such as autism. Copy number variants are large pieces of genetic material that are duplicated or deleted. We have known for many years that many copy number variants at certain genetic locations are linked to autism. Because these copy number variants may include lots of different genes, it has been difficult to understand how these copy number variants alter human brain function. Furthermore, although animal models are important, autism is in many ways defined by differences in uniquely human cognitive and social functioning. Better understanding of how these copy number variants change human brain function will shed light on universal mechanisms that regulate neurodevelopment. We studied a copy number variant called dup15q, that is associated with almost 40-fold higher rates of autism vs. the general population. We studied post-mortem human brain tissue from individuals with dup15q, individuals with autism not related to dup15q, and neurotypical controls, to better understand how the human brain is impacted by dup15q. We focused on frontal cortex, an important brain region in executive function and social perspective taking. We applied cutting edge techniques that allow us to assess individual cells in the brain. 

 Dr. Guasch-Ferré[/caption]
Marta Guasch-Ferré, PhD
Associate Professor and Deputy Head of Section, Section of Epidemiology
University of Copenhagen
Group Leader, Novo Nordisk Foundation Center for Basic Metabolic Research
Adjunct Associate Professor, Department of Nutrition
Harvard TH Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Olive oil is rich in monounsaturated fats and contains compounds with antioxidant activity that may play a protective role for the brain. Olive oil as part of a Mediterranean diet appears to have a beneficial effect against cognitive decline. Higher olive oil intake was previously associated with a lower risk of cardiovascular disease and mortality. But its association with dementia mortality was unknown.
Dr. Guasch-Ferré[/caption]
Marta Guasch-Ferré, PhD
Associate Professor and Deputy Head of Section, Section of Epidemiology
University of Copenhagen
Group Leader, Novo Nordisk Foundation Center for Basic Metabolic Research
Adjunct Associate Professor, Department of Nutrition
Harvard TH Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Olive oil is rich in monounsaturated fats and contains compounds with antioxidant activity that may play a protective role for the brain. Olive oil as part of a Mediterranean diet appears to have a beneficial effect against cognitive decline. Higher olive oil intake was previously associated with a lower risk of cardiovascular disease and mortality. But its association with dementia mortality was unknown.


 Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research Scientist
Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research Scientist


 Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.
Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.

 Dr. Davaasambuu[/caption]
Dr Ganmaa Davaasambuu MD PhD
Associate Professor
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: The crucial role of vitamin D in facilitating calcium absorption from the diet and promoting calcium deposition in bones (known as 'mineralization') has been a long-established understanding. Furthermore, some observational studies have reported an association between low vitamin D levels and a heightened risk of bone fractures in children. This raised the possibility that vitamin D supplements could potentially play a role in decreasing fracture risk in children with initially low baseline levels. However, clinical trials assessing the causal link between low vitamin D status and reduced fracture risk were necessary, and such trials had not been conducted before.
Dr. Davaasambuu[/caption]
Dr Ganmaa Davaasambuu MD PhD
Associate Professor
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: The crucial role of vitamin D in facilitating calcium absorption from the diet and promoting calcium deposition in bones (known as 'mineralization') has been a long-established understanding. Furthermore, some observational studies have reported an association between low vitamin D levels and a heightened risk of bone fractures in children. This raised the possibility that vitamin D supplements could potentially play a role in decreasing fracture risk in children with initially low baseline levels. However, clinical trials assessing the causal link between low vitamin D status and reduced fracture risk were necessary, and such trials had not been conducted before.

 Dr. Traverso[/caption]
Giovanni Traverso MD PhD
Karl Van Tassel (1925) Career Development Professor
Department of Mechanical Engineering
Koch Institute of Integrative Cancer Research
Division of Gastroenterology
Brigham and Women’s Hospital
Harvard Medical School, Boston, MA, USA
MedicalResearch.com: What is the background for this study?
Response: I think its always important to acknowledge that this is a big team effort. We have the teams from MIT, Celero Systems, West Virgnia University (WVU) and Brigham and Women’s Hospital (BWH) all working together on this. For this study, Celero prototyped the devices that we tested in pre-clinical (Swine) models and in a first-in-human study with the team at WVU.
Our lab focuses on the development of ingestible devices for drug delivery and sensing and these have informed the development of these efforts as you can see.
Dr. Traverso[/caption]
Giovanni Traverso MD PhD
Karl Van Tassel (1925) Career Development Professor
Department of Mechanical Engineering
Koch Institute of Integrative Cancer Research
Division of Gastroenterology
Brigham and Women’s Hospital
Harvard Medical School, Boston, MA, USA
MedicalResearch.com: What is the background for this study?
Response: I think its always important to acknowledge that this is a big team effort. We have the teams from MIT, Celero Systems, West Virgnia University (WVU) and Brigham and Women’s Hospital (BWH) all working together on this. For this study, Celero prototyped the devices that we tested in pre-clinical (Swine) models and in a first-in-human study with the team at WVU.
Our lab focuses on the development of ingestible devices for drug delivery and sensing and these have informed the development of these efforts as you can see.



 Dr. Hafezi-Moghadam[/caption]
Ali Hafezi-Moghadam, Ph.D., M.D
Director, Molecular Biomarkers Nano-Imaging Laboratory (MBNI)
Associate Professor of Radiology, Harvard Medical School
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: “It is very easy to answer many fundamental biological questions” said Richard Feynman in his 1959 address, where he also offered his simple and ingenious solution: “you just look at the thing!”
Dr. Hafezi-Moghadam[/caption]
Ali Hafezi-Moghadam, Ph.D., M.D
Director, Molecular Biomarkers Nano-Imaging Laboratory (MBNI)
Associate Professor of Radiology, Harvard Medical School
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: “It is very easy to answer many fundamental biological questions” said Richard Feynman in his 1959 address, where he also offered his simple and ingenious solution: “you just look at the thing!”


 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
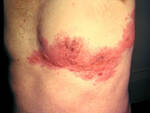
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.

 Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.
Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.


 Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.

 Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
 Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.


 Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
 Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.
Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.
 Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.
Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.

 Dr. Dryden-Peterson[/caption]
SCOTT DRYDEN-PETERSON, MD
Assistant Professor, Medicine, Harvard Medical School
Research Affiliate, Immunology and Infectious Diseases
Harvard T.H. Chan School Of Public Health
Associate Physician, Medicine, Infectious Diseases
Brigham And Women's Hospital
Research Associate, Botswana Harvard AIDS Institute
MedicalResearch.com: What is the background for this study?
Response: The combination of the antiviral medicine nirmatrelvir and ritonavir (Paxlovid) which boosts antiviral levels was found to reduce the need for hospitalization by nearly 90% among unvaccinated people. Whether nirmatrelvir plus ritonavir can also help vaccinated people was uncertain.
Dr. Dryden-Peterson[/caption]
SCOTT DRYDEN-PETERSON, MD
Assistant Professor, Medicine, Harvard Medical School
Research Affiliate, Immunology and Infectious Diseases
Harvard T.H. Chan School Of Public Health
Associate Physician, Medicine, Infectious Diseases
Brigham And Women's Hospital
Research Associate, Botswana Harvard AIDS Institute
MedicalResearch.com: What is the background for this study?
Response: The combination of the antiviral medicine nirmatrelvir and ritonavir (Paxlovid) which boosts antiviral levels was found to reduce the need for hospitalization by nearly 90% among unvaccinated people. Whether nirmatrelvir plus ritonavir can also help vaccinated people was uncertain.

