Author Interviews, Respiratory, Social Issues, University of Michigan / 31.01.2024
People Sick With Contagious Respiratory Viruses Often Conceal Illness for Personal or Professional Reasons, Regardless of Effects on Others
MedicalResearch.com Interview with:
 Wilson N. Merrell
Ph.D. Student
Department of Psychology
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: From the common cold to COVID-19, people get sick all the time. Because our social worlds don’t pause just because we are feeling ill, we often still need to navigate in-person events ranging from work and school to first dates and family dinners even while we’re feeling under the weather. In these kinds of social situations, do we always tell others when we’re feeling sick, or are there times when we may want to downplay our illness? After all, we tend to react negatively to, find less attractive, and steer clear of people who are sick with infectious illness. To the extent that we want to avoid these negative social outcomes while sick, it therefore makes sense that we may take steps to cover up our sickness in social situations. Given that this concealment could serve individual social goals (like allowing you to connect with others) at the cost of broader harms to public health (through the spread of infectious disease), we found this behavior both theoretically novel and practically timely.
Wilson N. Merrell
Ph.D. Student
Department of Psychology
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: From the common cold to COVID-19, people get sick all the time. Because our social worlds don’t pause just because we are feeling ill, we often still need to navigate in-person events ranging from work and school to first dates and family dinners even while we’re feeling under the weather. In these kinds of social situations, do we always tell others when we’re feeling sick, or are there times when we may want to downplay our illness? After all, we tend to react negatively to, find less attractive, and steer clear of people who are sick with infectious illness. To the extent that we want to avoid these negative social outcomes while sick, it therefore makes sense that we may take steps to cover up our sickness in social situations. Given that this concealment could serve individual social goals (like allowing you to connect with others) at the cost of broader harms to public health (through the spread of infectious disease), we found this behavior both theoretically novel and practically timely.
 Wilson N. Merrell
Ph.D. Student
Department of Psychology
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: From the common cold to COVID-19, people get sick all the time. Because our social worlds don’t pause just because we are feeling ill, we often still need to navigate in-person events ranging from work and school to first dates and family dinners even while we’re feeling under the weather. In these kinds of social situations, do we always tell others when we’re feeling sick, or are there times when we may want to downplay our illness? After all, we tend to react negatively to, find less attractive, and steer clear of people who are sick with infectious illness. To the extent that we want to avoid these negative social outcomes while sick, it therefore makes sense that we may take steps to cover up our sickness in social situations. Given that this concealment could serve individual social goals (like allowing you to connect with others) at the cost of broader harms to public health (through the spread of infectious disease), we found this behavior both theoretically novel and practically timely.
Wilson N. Merrell
Ph.D. Student
Department of Psychology
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: From the common cold to COVID-19, people get sick all the time. Because our social worlds don’t pause just because we are feeling ill, we often still need to navigate in-person events ranging from work and school to first dates and family dinners even while we’re feeling under the weather. In these kinds of social situations, do we always tell others when we’re feeling sick, or are there times when we may want to downplay our illness? After all, we tend to react negatively to, find less attractive, and steer clear of people who are sick with infectious illness. To the extent that we want to avoid these negative social outcomes while sick, it therefore makes sense that we may take steps to cover up our sickness in social situations. Given that this concealment could serve individual social goals (like allowing you to connect with others) at the cost of broader harms to public health (through the spread of infectious disease), we found this behavior both theoretically novel and practically timely.


 Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.
Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.



 Dr. Hunter[/caption]
Jennifer Hunter, B.Med., M.Sc.P.H., Ph.D.
Adjunct Associate Professor
NICM Health Research Institute
Western Sydney University
Associate Professor Jennifer Hunter is an academic general practitioner with a clinical interest in integrative medicine, has received payment for providing expert advice about traditional, complementary and integrative medicine, including nutraceuticals, to industry, government bodies and non-government organisations, and spoken at workshops, seminars and conferences for which registration, travel and/or accommodation has been paid for by the organisers.
MedicalResearch.com: What is the background for this study?
Response: We decided to review the evidence for zinc in response to calls for rapid evidence reviews to inform self-care and clinical practice during the COVID-19 pandemic.
Laboratory studies have found that zinc can inhibit the replication of many respiratory viruses, including SARS-CoV-2 and other coronaviruses. Zinc plays a key role in immunity, inflammation, tissue injury, ACE-2 receptor activity, and also in tissue responses to a lack of oxygen. Low zinc status may be a risk factor for severe SARS-CoV-2 illness.
Additionally, there was some indirect evidence suggesting zinc might be effective for other respiratory tract infections such as the common cold and we wanted to verify this.
Dr. Hunter[/caption]
Jennifer Hunter, B.Med., M.Sc.P.H., Ph.D.
Adjunct Associate Professor
NICM Health Research Institute
Western Sydney University
Associate Professor Jennifer Hunter is an academic general practitioner with a clinical interest in integrative medicine, has received payment for providing expert advice about traditional, complementary and integrative medicine, including nutraceuticals, to industry, government bodies and non-government organisations, and spoken at workshops, seminars and conferences for which registration, travel and/or accommodation has been paid for by the organisers.
MedicalResearch.com: What is the background for this study?
Response: We decided to review the evidence for zinc in response to calls for rapid evidence reviews to inform self-care and clinical practice during the COVID-19 pandemic.
Laboratory studies have found that zinc can inhibit the replication of many respiratory viruses, including SARS-CoV-2 and other coronaviruses. Zinc plays a key role in immunity, inflammation, tissue injury, ACE-2 receptor activity, and also in tissue responses to a lack of oxygen. Low zinc status may be a risk factor for severe SARS-CoV-2 illness.
Additionally, there was some indirect evidence suggesting zinc might be effective for other respiratory tract infections such as the common cold and we wanted to verify this.
 Lara van der Schoot[/caption]
Lara van der Schoot
MD, PhD candidate
Department of Dermatology
Radboud University Medical Center
Nijmegen, The Netherlands
MedicalResearch.com: What is the background for this study?
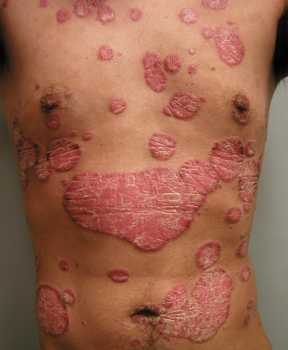
Response: Psoriasis is a chronic, immune mediated skin disease for which effective targeted biological agents have become available the past years. Inherent to their immunomodulatory mechanism of action, biologics might increase infections risk. We know from clinical trial data that respiratory tract infections are among the most common adverse events during biologic treatment, but real-world data is sparse. Regarding the risk of serious infections among biologic users, mostly defined as infections requiring hospitalization, previous studies provided different results and there is limited comparative data for the newer biologics available.
The COVID-19 pandemic turned attention to the risk of infections among biologic users, especially for respiratory tract infections, as they might relate to susceptibility for viral respiratory tract infections such as COVID-19.
In our study, the primary aim was to determine the risk of respiratory tract infections among real-world psoriasis patients treated with biologics, including the newer IL-17 and IL-23 inhibitors. The secondary aim was to assess risk of serious infections in this cohort. Additionally, rates of SARS-CoV-2 infections were assessed.
Lara van der Schoot[/caption]
Lara van der Schoot
MD, PhD candidate
Department of Dermatology
Radboud University Medical Center
Nijmegen, The Netherlands
MedicalResearch.com: What is the background for this study?
Response: Psoriasis is a chronic, immune mediated skin disease for which effective targeted biological agents have become available the past years. Inherent to their immunomodulatory mechanism of action, biologics might increase infections risk. We know from clinical trial data that respiratory tract infections are among the most common adverse events during biologic treatment, but real-world data is sparse. Regarding the risk of serious infections among biologic users, mostly defined as infections requiring hospitalization, previous studies provided different results and there is limited comparative data for the newer biologics available.
The COVID-19 pandemic turned attention to the risk of infections among biologic users, especially for respiratory tract infections, as they might relate to susceptibility for viral respiratory tract infections such as COVID-19.
In our study, the primary aim was to determine the risk of respiratory tract infections among real-world psoriasis patients treated with biologics, including the newer IL-17 and IL-23 inhibitors. The secondary aim was to assess risk of serious infections in this cohort. Additionally, rates of SARS-CoV-2 infections were assessed.
 Dr. Blankson[/caption]
Joel N. Blankson, MD, PhD
Department of Infectious Diseases
Associate Professor
Cellular and Molecular Medicine Program
Johns Hopkins
MedicalResearch.com: What is the background for this study? Which vaccines did you evaluate?
Response: Prior studies from several groups including our own have found T cell cross-recognition of peptides from SARS-CoV-2 and the common cold coronaviruses.
We asked whether as a result of this cross-reactivity, immunization with the SARS-CoV-2 vaccine would also enhance T cell responses to the common cold coronaviruses.
Prior studies also suggested that antibodies elicited from the mRNA vaccines had a reduced ability to neutralize the emerging variants of concern.
Most of the study participants had received the Pfizer vaccine, but a few had received the Moderna vaccine.
Dr. Blankson[/caption]
Joel N. Blankson, MD, PhD
Department of Infectious Diseases
Associate Professor
Cellular and Molecular Medicine Program
Johns Hopkins
MedicalResearch.com: What is the background for this study? Which vaccines did you evaluate?
Response: Prior studies from several groups including our own have found T cell cross-recognition of peptides from SARS-CoV-2 and the common cold coronaviruses.
We asked whether as a result of this cross-reactivity, immunization with the SARS-CoV-2 vaccine would also enhance T cell responses to the common cold coronaviruses.
Prior studies also suggested that antibodies elicited from the mRNA vaccines had a reduced ability to neutralize the emerging variants of concern.
Most of the study participants had received the Pfizer vaccine, but a few had received the Moderna vaccine. 
 Dr. Sinha[/caption]
Pranay Sinha, MD
Section of Infectious Diseases
Boston University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: We hypothesized that mitigation measures such as physical distancing and mask wearing instituted in Boston would reduce transmission of common respiratory viruses such as influenza, Rhinovirus, and Parainfluenzavirus. We compared the rate of detection of such viruses at Boston Medical Center on comprehensive respiratory panels in the ambulatory, emergency room, and hospital settings in 2020 to rates in the previous five years.
Dr. Sinha[/caption]
Pranay Sinha, MD
Section of Infectious Diseases
Boston University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: We hypothesized that mitigation measures such as physical distancing and mask wearing instituted in Boston would reduce transmission of common respiratory viruses such as influenza, Rhinovirus, and Parainfluenzavirus. We compared the rate of detection of such viruses at Boston Medical Center on comprehensive respiratory panels in the ambulatory, emergency room, and hospital settings in 2020 to rates in the previous five years.











 Dr. Bacharier[/caption]
MedicalResearch.com Interview with:
Leonard B. Bacharier, MD
Professor of pediatrics
Clinical Director, Division of Allergy, Immunology and Pulmonary Medicine
St Louis School of Medicine
Washington University
St Louis, Missouri
Medical Research: What is the background for this study? What are the main findings?
Dr. Bacharier: Oral corticosteroids such as prednisone have become the standard of care for children whose colds tend to progress and lead to severe wheezing and difficulty breathing.
“But there are some studies that suggest these treatments don’t consistently work for young children. That’s why we want to find ways to prevent upper respiratory infections from progressing to lower respiratory tract illnesses. Once the episode gets going, standard interventions are less effective than would be desired”, reported Dr. Bacharier.
Dr. Bacharier[/caption]
MedicalResearch.com Interview with:
Leonard B. Bacharier, MD
Professor of pediatrics
Clinical Director, Division of Allergy, Immunology and Pulmonary Medicine
St Louis School of Medicine
Washington University
St Louis, Missouri
Medical Research: What is the background for this study? What are the main findings?
Dr. Bacharier: Oral corticosteroids such as prednisone have become the standard of care for children whose colds tend to progress and lead to severe wheezing and difficulty breathing.
“But there are some studies that suggest these treatments don’t consistently work for young children. That’s why we want to find ways to prevent upper respiratory infections from progressing to lower respiratory tract illnesses. Once the episode gets going, standard interventions are less effective than would be desired”, reported Dr. Bacharier.








