Medical Billing, Neurological Disorders / 29.05.2026
What Neurological Patients Should Know Before Disputing a Medical Bill?
[caption id="attachment_74019" align="aligncenter" width="500"] Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.
Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.
 Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.
Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.











 Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research Scientist
Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research Scientist



 Dr. Tauscher-Wisniewski,[/caption]
Sitra Tauscher-Wisniewski, MD
Vice President Clinical Development & Analytics
Novartis Gene Therapies
MedicalResearch.com: What is the background for this study? Would you briefly describe the condition of Spinal muscular atrophy (SMA)?
Response: At the 2023 Muscular Dystrophy Association Conference, we presented new data from two of our Long-Term Follow-Up (LTFU) studies, LT001 and LT002, which show the continued efficacy and durability of Zolgensma across a range of patient populations, with an overall benefit-risk profile that remains favorable. LT001 is a 15-year ongoing observational LTFU study following the Phase 1 START patients, who were the very first patients to receive our gene replacement therapy. LT-002 is a voluntary Phase 4 15-year ongoing follow-up safety and efficacy study of Zolgensma IV and investigational intrathecal (IT) OAV101 in patients previously treated in the Phase 3 IV studies (STR1VE-US, STR1VE-EU, STR1VE-AP, SPR1NT) and the Phase 1 IT study (STRONG).
Spinal muscular atrophy (SMA) is a rare, devastating genetic disease that leads to progressive muscle weakness, paralysis, and when left untreated in one of its most severe forms (SMA Type 1), permanent ventilation or death in 90% of cases by age 2. It is caused by a lack of a functional survival motor neuron 1 (SMN1) gene, and in the most severe forms results in the rapid and irreversible loss of motor neurons, affecting muscle functions, including breathing, swallowing and basic movement.
Dr. Tauscher-Wisniewski,[/caption]
Sitra Tauscher-Wisniewski, MD
Vice President Clinical Development & Analytics
Novartis Gene Therapies
MedicalResearch.com: What is the background for this study? Would you briefly describe the condition of Spinal muscular atrophy (SMA)?
Response: At the 2023 Muscular Dystrophy Association Conference, we presented new data from two of our Long-Term Follow-Up (LTFU) studies, LT001 and LT002, which show the continued efficacy and durability of Zolgensma across a range of patient populations, with an overall benefit-risk profile that remains favorable. LT001 is a 15-year ongoing observational LTFU study following the Phase 1 START patients, who were the very first patients to receive our gene replacement therapy. LT-002 is a voluntary Phase 4 15-year ongoing follow-up safety and efficacy study of Zolgensma IV and investigational intrathecal (IT) OAV101 in patients previously treated in the Phase 3 IV studies (STR1VE-US, STR1VE-EU, STR1VE-AP, SPR1NT) and the Phase 1 IT study (STRONG).
Spinal muscular atrophy (SMA) is a rare, devastating genetic disease that leads to progressive muscle weakness, paralysis, and when left untreated in one of its most severe forms (SMA Type 1), permanent ventilation or death in 90% of cases by age 2. It is caused by a lack of a functional survival motor neuron 1 (SMN1) gene, and in the most severe forms results in the rapid and irreversible loss of motor neurons, affecting muscle functions, including breathing, swallowing and basic movement.







 Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.
Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.




 Dr. Factor[/caption]
Stewart A. Factor, D.O.
Professor of Neurology
Director of the Movement Disorders Program
Vance Lanier Chair of Neurology
Emory University School of Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by OFF episodes.
Response: Parkinson’s disease (PD) is a chronic, progressive neurodegenerative disease characterized by motor symptoms, including tremor at rest, rigidity and impaired movement, as well as significant non-motor symptoms, such as cognitive impairment, psychiatric symptoms and autonomic symptoms (i.e. urinary issues, constipation, low blood pressure). It is the second-most common neurodegenerative disease after Alzheimer’s disease and it is predicted that the prevalence of Parkinson’s disease will double by the year 2040. The symptoms of PD are in substantial part, due to loss of dopamine nerve cells in the brain. The current standard of care for PD includes replacing the dopamine loss by the use of oral carbidopa/levodopa. Levodopa is a precursor of dopamine, converted in the brain.
OFF episodes have been a significant unmet need in Parkinson’s disease since the emergence of levodopa. Initially, levodopa controls PD symptoms in a continuous fashion throughout the day. With time the response becomes less predictable and patients experience a re-emergence or worsening of PD symptoms. These episodes are what we mean by OFF episodes. OFF episodes can be characterized, in part, by re-emergence of motor symptoms including tremor, stiffness or slowed movement that can happen at any point during the day. OFF episodes typically begin within the first five years of treatment and occur at the end of a dose. This is referred to as end of dose failure or wearing off. Within the first four to six years after diagnosis, regardless of disease severity, up to 60 percent of people with PD experience OFF episodes. With time these episodes become longer, more severe and disabling, more frequent and less predictable as PD progresses. They can take up more than half the day
OFF episodes may alter a persons’ ability to perform everyday activities by slowing or even precluding their completion. The result is significant burden and distress for people living with Parkinson’s disease (PD) and their care partners.
CTH-300 was a Phase 3, 12-week, randomized, double-blind, placebo-controlled, parallel group, study examining the efficacy, safety and tolerability of apomorphine hydrochloride sublingual film (KYNMOBI) in people with levodopa-responsive PD complicated by OFF episodes. The primary endpoint was a mean change in the score from pre-dose in the Movement Disorder Society Unified Parkinson's Disease Rating Scale (MDS-UPDRS) Part III Motor Examination at 30 minutes after dosing at the 12-week visit of the maintenance treatment phase. The key secondary endpoint was the percentage of people with PD with a patient-rated full ON (or best) response within 30 minutes at the 12-week visit of the maintenance treatment phase.
Dr. Factor[/caption]
Stewart A. Factor, D.O.
Professor of Neurology
Director of the Movement Disorders Program
Vance Lanier Chair of Neurology
Emory University School of Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by OFF episodes.
Response: Parkinson’s disease (PD) is a chronic, progressive neurodegenerative disease characterized by motor symptoms, including tremor at rest, rigidity and impaired movement, as well as significant non-motor symptoms, such as cognitive impairment, psychiatric symptoms and autonomic symptoms (i.e. urinary issues, constipation, low blood pressure). It is the second-most common neurodegenerative disease after Alzheimer’s disease and it is predicted that the prevalence of Parkinson’s disease will double by the year 2040. The symptoms of PD are in substantial part, due to loss of dopamine nerve cells in the brain. The current standard of care for PD includes replacing the dopamine loss by the use of oral carbidopa/levodopa. Levodopa is a precursor of dopamine, converted in the brain.
OFF episodes have been a significant unmet need in Parkinson’s disease since the emergence of levodopa. Initially, levodopa controls PD symptoms in a continuous fashion throughout the day. With time the response becomes less predictable and patients experience a re-emergence or worsening of PD symptoms. These episodes are what we mean by OFF episodes. OFF episodes can be characterized, in part, by re-emergence of motor symptoms including tremor, stiffness or slowed movement that can happen at any point during the day. OFF episodes typically begin within the first five years of treatment and occur at the end of a dose. This is referred to as end of dose failure or wearing off. Within the first four to six years after diagnosis, regardless of disease severity, up to 60 percent of people with PD experience OFF episodes. With time these episodes become longer, more severe and disabling, more frequent and less predictable as PD progresses. They can take up more than half the day
OFF episodes may alter a persons’ ability to perform everyday activities by slowing or even precluding their completion. The result is significant burden and distress for people living with Parkinson’s disease (PD) and their care partners.
CTH-300 was a Phase 3, 12-week, randomized, double-blind, placebo-controlled, parallel group, study examining the efficacy, safety and tolerability of apomorphine hydrochloride sublingual film (KYNMOBI) in people with levodopa-responsive PD complicated by OFF episodes. The primary endpoint was a mean change in the score from pre-dose in the Movement Disorder Society Unified Parkinson's Disease Rating Scale (MDS-UPDRS) Part III Motor Examination at 30 minutes after dosing at the 12-week visit of the maintenance treatment phase. The key secondary endpoint was the percentage of people with PD with a patient-rated full ON (or best) response within 30 minutes at the 12-week visit of the maintenance treatment phase.

 Dr. Hänggi[/caption]
MedicalResearch.com: What is the background for this study?
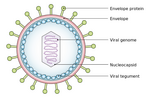
Response: Anti-MAG neuropathy is a rare form of acquired demyelinating neuropathy. The disease onset normally presents after the age of 50 years and is 2.7 times more frequent in men than in women, with a prevalence of about 1 in 100,000. It is caused by the production of monoclonal anti-MAG IgM antibodies that recognize the HNK-1 epitope. The myelin-associated glycoprotein MAG is a mediator for the formation and maintenance of the myelin sheaths. There is strong evidence that the binding and deposition of anti-MAG IgM autoantibodies on myelin sheath is responsible for the demyelination, which clinically manifests itself as a peripheral neuropathy affecting primarily sensory nerves. However, the causes and the exact mechanisms behind the expansion of anti-MAG IgM producing B-cell and plasma cell clones are not fully understood.
Most off-label treatments aim to reduce pathogenic autoantibody titers by depleting autoantibody-producing B cell clones which interfere with antibody-effector mechanisms, or physically remove autoantibodies from the circulation. Most frequently, the anti-CD20 monoclonal antibody rituximab is used to treat anti-MAG neuropathy patients. However, all of these treatment options often lack of selectivity, efficiency, or can induce severe adverse effects in some patients.
Polyneuron has designed PN-1007 to highly selectively target the IgM autoantibodies that cause anti-MAG neuropathy. PN-1007 is a glycopolymer that mimics the natural HNK-1 carbohydrate epitope found on myelin of peripheral nerves and binds to the circulating disease-causing antibodies. By eliminating these pathogenic antibodies, PN-1007 may protect the integrity of the neuronal myelin sheaths of anti-MAG neuropathy patients.
Dr. Hänggi[/caption]
MedicalResearch.com: What is the background for this study?
Response: Anti-MAG neuropathy is a rare form of acquired demyelinating neuropathy. The disease onset normally presents after the age of 50 years and is 2.7 times more frequent in men than in women, with a prevalence of about 1 in 100,000. It is caused by the production of monoclonal anti-MAG IgM antibodies that recognize the HNK-1 epitope. The myelin-associated glycoprotein MAG is a mediator for the formation and maintenance of the myelin sheaths. There is strong evidence that the binding and deposition of anti-MAG IgM autoantibodies on myelin sheath is responsible for the demyelination, which clinically manifests itself as a peripheral neuropathy affecting primarily sensory nerves. However, the causes and the exact mechanisms behind the expansion of anti-MAG IgM producing B-cell and plasma cell clones are not fully understood.
Most off-label treatments aim to reduce pathogenic autoantibody titers by depleting autoantibody-producing B cell clones which interfere with antibody-effector mechanisms, or physically remove autoantibodies from the circulation. Most frequently, the anti-CD20 monoclonal antibody rituximab is used to treat anti-MAG neuropathy patients. However, all of these treatment options often lack of selectivity, efficiency, or can induce severe adverse effects in some patients.
Polyneuron has designed PN-1007 to highly selectively target the IgM autoantibodies that cause anti-MAG neuropathy. PN-1007 is a glycopolymer that mimics the natural HNK-1 carbohydrate epitope found on myelin of peripheral nerves and binds to the circulating disease-causing antibodies. By eliminating these pathogenic antibodies, PN-1007 may protect the integrity of the neuronal myelin sheaths of anti-MAG neuropathy patients.