Medical Research Interview:
[caption id="attachment_60524" align="alignleft" width="195"]

Dr. Thomas[/caption]
Dr. Daniel Thomas MD PhD FRACP FRCPA
Program Leader, Blood Cancer
Precision Medicine Theme at the South Australia Health Medical Research Institute
Clinical Hematologist, Royal Adelaide Hospital
Associate Professor, Adelaide Medical School, The University of Adelaide
MedicalResearch.com: What is the background for this study? Would you briefly describe the condition of CMML?
Response: Chronic myelomonocytic leukemia (CMML) is a rare, but increasingly frequent, clonal stem cell disorder that results in hyperproliferation of inflammatory monocytes, a form of white blood cells. It features both myelodysplasia and myeloproliferation. CMML is most often found in older adults and leads to anemia, decreased quality of life, and an increased risk of acute myeloid leukemia (AML).
Granulocyte-macrophage colony-stimulating factor (GM-CSF) is a cytokine that stimulates production, growth, differentiation, activation, and function of myeloid cells (monocytes, neutrophils, and eosinophils). In the presence of
RAS-pathway mutations, a greater sensitivity to GM-CSF contributes to the hyperproliferation of myelocytes in myelodysplastic leukemias such as CMML, juvenile myelomonocytic leukemia (JMML), and acute myeloid leukemia (AML). In CMML, greater sensitivity to GM-CSF stimulates excessive monocytic precursor proliferation.
The PREACH-M Trial, which stands for
PREcision
Approach to
CHronic Myelomonocytic Leukemia, assesses the efficacy of lenzilumab in addition to azacitidine in treatment-naïve CMML participants with
RAS-pathway mutations (
KRAS,
NRAS,
CBL) and separately high dose ascorbate in participants with
TET2 mutations who do not have
RAS-pathway mutations. The study is currently underway and actively enrolling. It is being conducted and funded by the South Australian Health and Medical Research Institute (SAHMRI).
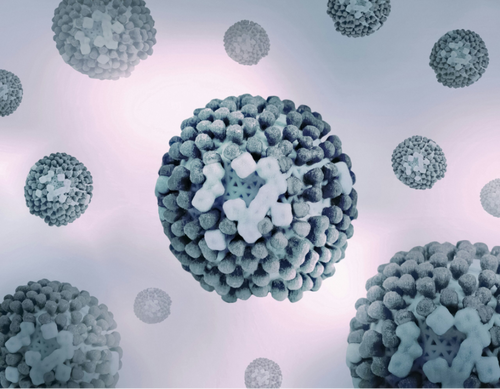 Most people with COVID-19 got sick, recovered, and moved on. A subset did not. Months in — sometimes over a year — they are still exhausted after climbing a flight of stairs, still losing words mid-sentence, still waking up as tired as when they went to bed. This is Long COVID, and by some estimates it now affects somewhere between 10 and 30% of those who contracted the virus. The numbers are staggering. The biology behind it is stranger than most people expect.
Here is what makes Long COVID different from typical post-viral fatigue: the immune response does not resolve. It just keeps going.
Most people with COVID-19 got sick, recovered, and moved on. A subset did not. Months in — sometimes over a year — they are still exhausted after climbing a flight of stairs, still losing words mid-sentence, still waking up as tired as when they went to bed. This is Long COVID, and by some estimates it now affects somewhere between 10 and 30% of those who contracted the virus. The numbers are staggering. The biology behind it is stranger than most people expect.
Here is what makes Long COVID different from typical post-viral fatigue: the immune response does not resolve. It just keeps going.






 Dr. Davis[/caption]
Esa M. Davis, M.D., M.P.H , F.A.A.F.P
Professor of Medicine and Family and Community Medicine
Associate Vice President of Community Health and
Senior Associate Dean of pPopulation Health and Community Medicine
University of Maryland School of Medicine
Dr. Davis joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron is important to overall health, and people need more iron when they are pregnant. This can make pregnant people at increased risk for iron deficiency, which can progress to anemia and cause complications for both moms and their babies. After reviewing the latest available research, the Task Force found that there is not enough evidence on whether pregnant people who do not have signs or symptoms of iron deficiency or anemia should be screened—or take iron supplements—to improve their health or the health of their baby.
Dr. Davis[/caption]
Esa M. Davis, M.D., M.P.H , F.A.A.F.P
Professor of Medicine and Family and Community Medicine
Associate Vice President of Community Health and
Senior Associate Dean of pPopulation Health and Community Medicine
University of Maryland School of Medicine
Dr. Davis joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron is important to overall health, and people need more iron when they are pregnant. This can make pregnant people at increased risk for iron deficiency, which can progress to anemia and cause complications for both moms and their babies. After reviewing the latest available research, the Task Force found that there is not enough evidence on whether pregnant people who do not have signs or symptoms of iron deficiency or anemia should be screened—or take iron supplements—to improve their health or the health of their baby. 
 Bone marrow aspiration is a medical procedure where a small amount of the liquid part of your bone marrow is removed for examination. A
Bone marrow aspiration is a medical procedure where a small amount of the liquid part of your bone marrow is removed for examination. A 
 Dr. Brousseau[/caption]
David Brousseau, MD, MS
Chair of Pediatrics
Nemours Children’s Health, Delaware and the
Sidney Kimmel Medical College at Thomas Jefferson University
Dr. Brousseau[/caption]
David Brousseau, MD, MS
Chair of Pediatrics
Nemours Children’s Health, Delaware and the
Sidney Kimmel Medical College at Thomas Jefferson University

 Dr. Thomas[/caption]
Dr. Daniel Thomas MD PhD FRACP FRCPA
Program Leader, Blood Cancer
Precision Medicine Theme at the South Australia Health Medical Research Institute
Clinical Hematologist, Royal Adelaide Hospital
Associate Professor, Adelaide Medical School, The University of Adelaide
MedicalResearch.com: What is the background for this study? Would you briefly describe the condition of CMML?
Response: Chronic myelomonocytic leukemia (CMML) is a rare, but increasingly frequent, clonal stem cell disorder that results in hyperproliferation of inflammatory monocytes, a form of white blood cells. It features both myelodysplasia and myeloproliferation. CMML is most often found in older adults and leads to anemia, decreased quality of life, and an increased risk of acute myeloid leukemia (AML).
Granulocyte-macrophage colony-stimulating factor (GM-CSF) is a cytokine that stimulates production, growth, differentiation, activation, and function of myeloid cells (monocytes, neutrophils, and eosinophils). In the presence of RAS-pathway mutations, a greater sensitivity to GM-CSF contributes to the hyperproliferation of myelocytes in myelodysplastic leukemias such as CMML, juvenile myelomonocytic leukemia (JMML), and acute myeloid leukemia (AML). In CMML, greater sensitivity to GM-CSF stimulates excessive monocytic precursor proliferation.
The PREACH-M Trial, which stands for PREcision Approach to CHronic Myelomonocytic Leukemia, assesses the efficacy of lenzilumab in addition to azacitidine in treatment-naïve CMML participants with RAS-pathway mutations (KRAS, NRAS, CBL) and separately high dose ascorbate in participants with TET2 mutations who do not have RAS-pathway mutations. The study is currently underway and actively enrolling. It is being conducted and funded by the South Australian Health and Medical Research Institute (SAHMRI).
Dr. Thomas[/caption]
Dr. Daniel Thomas MD PhD FRACP FRCPA
Program Leader, Blood Cancer
Precision Medicine Theme at the South Australia Health Medical Research Institute
Clinical Hematologist, Royal Adelaide Hospital
Associate Professor, Adelaide Medical School, The University of Adelaide
MedicalResearch.com: What is the background for this study? Would you briefly describe the condition of CMML?
Response: Chronic myelomonocytic leukemia (CMML) is a rare, but increasingly frequent, clonal stem cell disorder that results in hyperproliferation of inflammatory monocytes, a form of white blood cells. It features both myelodysplasia and myeloproliferation. CMML is most often found in older adults and leads to anemia, decreased quality of life, and an increased risk of acute myeloid leukemia (AML).
Granulocyte-macrophage colony-stimulating factor (GM-CSF) is a cytokine that stimulates production, growth, differentiation, activation, and function of myeloid cells (monocytes, neutrophils, and eosinophils). In the presence of RAS-pathway mutations, a greater sensitivity to GM-CSF contributes to the hyperproliferation of myelocytes in myelodysplastic leukemias such as CMML, juvenile myelomonocytic leukemia (JMML), and acute myeloid leukemia (AML). In CMML, greater sensitivity to GM-CSF stimulates excessive monocytic precursor proliferation.
The PREACH-M Trial, which stands for PREcision Approach to CHronic Myelomonocytic Leukemia, assesses the efficacy of lenzilumab in addition to azacitidine in treatment-naïve CMML participants with RAS-pathway mutations (KRAS, NRAS, CBL) and separately high dose ascorbate in participants with TET2 mutations who do not have RAS-pathway mutations. The study is currently underway and actively enrolling. It is being conducted and funded by the South Australian Health and Medical Research Institute (SAHMRI). 
 Prof. Hiddo Lambers Heerspink, PhD PHARMD
Department of Clinical Pharmacy and Pharmacology
University Medical Center Groningen
Groningen
Prof. Hiddo Lambers Heerspink, PhD PHARMD
Department of Clinical Pharmacy and Pharmacology
University Medical Center Groningen
Groningen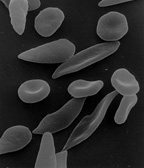
 Dr. Mapara[/caption]
Markus Y Mapara, MD
Professor of Medicine
Director of the Blood and Marrow Transplantation
Columbia University Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Sickle cell disease is caused by a point mutation in the beta-globin gene of hemoglobin resulting in the production of abnormal hemoglobin which leads to formation of sickle-shaped RBC under conditions of low oxygen. Sickle cell disease affects about 100,000 patients in the US which are predominantly African American. The only curative approach is to perform an allogeneic bone marrow transplant which is however fraught with significant treatment-related risks if a matched sibling donor is not available.
The current study describes the successful application of a novel gene therapy to treat patients with sickle cell disease. The strategy is based on a gene-addition approach to introduce the genetic information for a Hemoglobin F-like molecule termed HgAT87Q into hematopoietic stem cells. The expression of this novel hemoglobin prevents polymerization of HgbS and has now been demonstrated to prevent the occurrence of vaso-occlusive pain crises in sickle cell disease patients.
Dr. Mapara[/caption]
Markus Y Mapara, MD
Professor of Medicine
Director of the Blood and Marrow Transplantation
Columbia University Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Sickle cell disease is caused by a point mutation in the beta-globin gene of hemoglobin resulting in the production of abnormal hemoglobin which leads to formation of sickle-shaped RBC under conditions of low oxygen. Sickle cell disease affects about 100,000 patients in the US which are predominantly African American. The only curative approach is to perform an allogeneic bone marrow transplant which is however fraught with significant treatment-related risks if a matched sibling donor is not available.
The current study describes the successful application of a novel gene therapy to treat patients with sickle cell disease. The strategy is based on a gene-addition approach to introduce the genetic information for a Hemoglobin F-like molecule termed HgAT87Q into hematopoietic stem cells. The expression of this novel hemoglobin prevents polymerization of HgbS and has now been demonstrated to prevent the occurrence of vaso-occlusive pain crises in sickle cell disease patients.






 Dr. Erdlenbruch[/caption]
Response: At the World Federation of Hemophilia Virtual Summit 2020 (WFH 2020),
Dr. Erdlenbruch[/caption]
Response: At the World Federation of Hemophilia Virtual Summit 2020 (WFH 2020), 










