Author Interviews, Blood Pressure - Hypertension, JACC / 15.02.2026
APOLLO Trials Support Potential Role of Ultra-Low-Dose Triple Therapy as Initial Strategy for Mild-to-Moderate Hypertension
MedicalResearch.com Interview with:
[caption id="attachment_72419" align="alignleft" width="200"] Prof. Moo-Yong Rhee[/caption]
Professor Moo-Yong Rhee MD, PhD.
Cardiology, Dongguk University Ilsan Hospital
College of Medicine, Dongguk University
Goyang-si, Gyeonggi-do, Korea
MedicalResearch.com: What is the background for this study?
Response: Hypertension remains one of the leading causes of cardiovascular morbidity and mortality worldwide. Major challenges in its initial treatment include therapeutic inertia, reliance on stepwise dose escalation of single agents, and reduced adherence due to dose-related adverse effects. These limitations often delay optimal blood pressure control.
To address these issues, the concept of low-dose combination therapy was proposed, based on the rationale that combining multiple agents at lower doses may enhance efficacy while minimizing side effects. Although several studies have supported this concept, systematic translational research and confirmatory clinical trials were needed before widespread clinical implementation.
The recently completed APOLLO-301 and APOLLO-302 trials were confirmatory, randomized, phase 3 studies designed to evaluate the efficacy and safety of a single-pill ultra-low-dose triple combination therapy, conducted in accordance with regulatory standards. This formulation combined three antihypertensive agents (amlodipine (1.67 mg), losartan (16.67 mg), and chlorthalidone (4.17 mg)) each at approximately one-third of its standard dose. The triple combination was directly compared with standard-dose monotherapy (amlodipine 5 mg or losartan 50 mg).
After 8 weeks of treatment, the ultra-low-dose triple combination achieved blood pressure reductions comparable to those of amlodipine 5 mg and significantly greater than those of losartan 50 mg, while maintaining good tolerability. These findings support the potential role of ultra-low-dose triple therapy as an effective initial treatment strategy for patients with mild-to-moderate hypertension.
Prof. Moo-Yong Rhee[/caption]
Professor Moo-Yong Rhee MD, PhD.
Cardiology, Dongguk University Ilsan Hospital
College of Medicine, Dongguk University
Goyang-si, Gyeonggi-do, Korea
MedicalResearch.com: What is the background for this study?
Response: Hypertension remains one of the leading causes of cardiovascular morbidity and mortality worldwide. Major challenges in its initial treatment include therapeutic inertia, reliance on stepwise dose escalation of single agents, and reduced adherence due to dose-related adverse effects. These limitations often delay optimal blood pressure control.
To address these issues, the concept of low-dose combination therapy was proposed, based on the rationale that combining multiple agents at lower doses may enhance efficacy while minimizing side effects. Although several studies have supported this concept, systematic translational research and confirmatory clinical trials were needed before widespread clinical implementation.
The recently completed APOLLO-301 and APOLLO-302 trials were confirmatory, randomized, phase 3 studies designed to evaluate the efficacy and safety of a single-pill ultra-low-dose triple combination therapy, conducted in accordance with regulatory standards. This formulation combined three antihypertensive agents (amlodipine (1.67 mg), losartan (16.67 mg), and chlorthalidone (4.17 mg)) each at approximately one-third of its standard dose. The triple combination was directly compared with standard-dose monotherapy (amlodipine 5 mg or losartan 50 mg).
After 8 weeks of treatment, the ultra-low-dose triple combination achieved blood pressure reductions comparable to those of amlodipine 5 mg and significantly greater than those of losartan 50 mg, while maintaining good tolerability. These findings support the potential role of ultra-low-dose triple therapy as an effective initial treatment strategy for patients with mild-to-moderate hypertension.
 Prof. Moo-Yong Rhee[/caption]
Professor Moo-Yong Rhee MD, PhD.
Cardiology, Dongguk University Ilsan Hospital
College of Medicine, Dongguk University
Goyang-si, Gyeonggi-do, Korea
MedicalResearch.com: What is the background for this study?
Response: Hypertension remains one of the leading causes of cardiovascular morbidity and mortality worldwide. Major challenges in its initial treatment include therapeutic inertia, reliance on stepwise dose escalation of single agents, and reduced adherence due to dose-related adverse effects. These limitations often delay optimal blood pressure control.
To address these issues, the concept of low-dose combination therapy was proposed, based on the rationale that combining multiple agents at lower doses may enhance efficacy while minimizing side effects. Although several studies have supported this concept, systematic translational research and confirmatory clinical trials were needed before widespread clinical implementation.
The recently completed APOLLO-301 and APOLLO-302 trials were confirmatory, randomized, phase 3 studies designed to evaluate the efficacy and safety of a single-pill ultra-low-dose triple combination therapy, conducted in accordance with regulatory standards. This formulation combined three antihypertensive agents (amlodipine (1.67 mg), losartan (16.67 mg), and chlorthalidone (4.17 mg)) each at approximately one-third of its standard dose. The triple combination was directly compared with standard-dose monotherapy (amlodipine 5 mg or losartan 50 mg).
After 8 weeks of treatment, the ultra-low-dose triple combination achieved blood pressure reductions comparable to those of amlodipine 5 mg and significantly greater than those of losartan 50 mg, while maintaining good tolerability. These findings support the potential role of ultra-low-dose triple therapy as an effective initial treatment strategy for patients with mild-to-moderate hypertension.
Prof. Moo-Yong Rhee[/caption]
Professor Moo-Yong Rhee MD, PhD.
Cardiology, Dongguk University Ilsan Hospital
College of Medicine, Dongguk University
Goyang-si, Gyeonggi-do, Korea
MedicalResearch.com: What is the background for this study?
Response: Hypertension remains one of the leading causes of cardiovascular morbidity and mortality worldwide. Major challenges in its initial treatment include therapeutic inertia, reliance on stepwise dose escalation of single agents, and reduced adherence due to dose-related adverse effects. These limitations often delay optimal blood pressure control.
To address these issues, the concept of low-dose combination therapy was proposed, based on the rationale that combining multiple agents at lower doses may enhance efficacy while minimizing side effects. Although several studies have supported this concept, systematic translational research and confirmatory clinical trials were needed before widespread clinical implementation.
The recently completed APOLLO-301 and APOLLO-302 trials were confirmatory, randomized, phase 3 studies designed to evaluate the efficacy and safety of a single-pill ultra-low-dose triple combination therapy, conducted in accordance with regulatory standards. This formulation combined three antihypertensive agents (amlodipine (1.67 mg), losartan (16.67 mg), and chlorthalidone (4.17 mg)) each at approximately one-third of its standard dose. The triple combination was directly compared with standard-dose monotherapy (amlodipine 5 mg or losartan 50 mg).
After 8 weeks of treatment, the ultra-low-dose triple combination achieved blood pressure reductions comparable to those of amlodipine 5 mg and significantly greater than those of losartan 50 mg, while maintaining good tolerability. These findings support the potential role of ultra-low-dose triple therapy as an effective initial treatment strategy for patients with mild-to-moderate hypertension.






 It is your lifestyle that determines your blood pressure levels. Your nutritional intake and the level of activity have a significant part as well.
It is your lifestyle that determines your blood pressure levels. Your nutritional intake and the level of activity have a significant part as well. 
 Esa M. Davis, M.D., M.P.H , F.A.A.F.P
Professor of Medicine and Family and Community Medicine
Associate Vice President of Community Health and
Senior Associate Dean of pPopulation Health and Community Medicine
University of Maryland School of Medicine
Dr. Davis joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study?
Response: Hypertensive disorders of pregnancy, including gestational hypertension, preeclampsia, and eclampsia, are among the leading causes of serious complications and death for pregnant people in the United States.
Pregnant women and pregnant people of all genders should have their blood pressure measured at each prenatal visit to help find and prevent serious health issues related to hypertensive disorders of pregnancy.
Esa M. Davis, M.D., M.P.H , F.A.A.F.P
Professor of Medicine and Family and Community Medicine
Associate Vice President of Community Health and
Senior Associate Dean of pPopulation Health and Community Medicine
University of Maryland School of Medicine
Dr. Davis joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study?
Response: Hypertensive disorders of pregnancy, including gestational hypertension, preeclampsia, and eclampsia, are among the leading causes of serious complications and death for pregnant people in the United States.
Pregnant women and pregnant people of all genders should have their blood pressure measured at each prenatal visit to help find and prevent serious health issues related to hypertensive disorders of pregnancy. 
 Dr. McLoughlin Brady[/caption]
Tammy M. Brady, MD, PhD (she/her/hers)
Vice Chair for Clinical Research, Dept of Pediatrics
Associate Director, Welch Center for Prevention, Epidemiology, and Clinical Research
Associate Professor of Pediatrics, Division of Pediatric Nephrology
Medical Director, Pediatric Hypertension Program
Johns Hopkins University
Baltimore, MD 21287
MedicalResearch.com: What is the background for this study? What are the main findings?
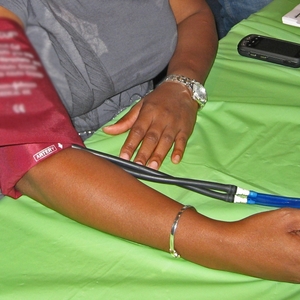
Response: Accurate BP measurement is key to identification and treatment of hypertension which serves ultimately to prevent cardiovascular disease. Our study describes substantial measurement error that can occur in a common office and home BP measurement scenario: use of a regular cuff size for all individuals regardless of arm size. Many office triage measurements occur without individualized cuff selection and most home BP devices come with one cuff size – and our study shows that using a regular cuff size for people who have larger arms – those who require a large adult cuff or an extra-large adult cuff – can lead to blood pressure readings that are almost 5 and 20 mmHg greater than their actual BP, respectively. Those require a small adult cuff can have BP readings that are almost 4 mmHg lower than their actual BP.
Dr. McLoughlin Brady[/caption]
Tammy M. Brady, MD, PhD (she/her/hers)
Vice Chair for Clinical Research, Dept of Pediatrics
Associate Director, Welch Center for Prevention, Epidemiology, and Clinical Research
Associate Professor of Pediatrics, Division of Pediatric Nephrology
Medical Director, Pediatric Hypertension Program
Johns Hopkins University
Baltimore, MD 21287
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Accurate BP measurement is key to identification and treatment of hypertension which serves ultimately to prevent cardiovascular disease. Our study describes substantial measurement error that can occur in a common office and home BP measurement scenario: use of a regular cuff size for all individuals regardless of arm size. Many office triage measurements occur without individualized cuff selection and most home BP devices come with one cuff size – and our study shows that using a regular cuff size for people who have larger arms – those who require a large adult cuff or an extra-large adult cuff – can lead to blood pressure readings that are almost 5 and 20 mmHg greater than their actual BP, respectively. Those require a small adult cuff can have BP readings that are almost 4 mmHg lower than their actual BP.

 Dr. Sundström[/caption]
Johan Sundström, MD, PhD
Professor of Epidemiology at Uppsala University
Professorial Fellow at The George Institute for Global Health
Cardiologist at Uppsala University Hospital
MedicalResearch.com: What is the background for this study?
Response: High blood pressure, hypertension, is a growing global health challenge. Over the last 30 years, the number of people with hypertension has doubled, and it is estimated that around a third of adults aged 30-79 have the condition - a total of 1.28 billion people worldwide. Untreated hypertension can lead to kidney disease, heart disease, and stroke, accounting for 11.3 million deaths in 2021 alone. A small minority get their blood pressure under control with drug therapy, and some studies indicate that as little as half are taking their blood pressure medications as intended. Is this because the drugs' effectiveness and side effects differ between different individuals? If so, there would be a substantial risk that patients will not get their optimal medication on the first try, with poor blood pressure lowering and unnecessary side effects as a result.
In a new clinical trial in Sweden, it was studied whether there is an optimal blood pressure medication for each person, and thus a potential for personalized blood pressure treatment. In the study, 280 people with high blood pressure tried out four different blood pressure drugs on several different occasions over a total of one year.
Dr. Sundström[/caption]
Johan Sundström, MD, PhD
Professor of Epidemiology at Uppsala University
Professorial Fellow at The George Institute for Global Health
Cardiologist at Uppsala University Hospital
MedicalResearch.com: What is the background for this study?
Response: High blood pressure, hypertension, is a growing global health challenge. Over the last 30 years, the number of people with hypertension has doubled, and it is estimated that around a third of adults aged 30-79 have the condition - a total of 1.28 billion people worldwide. Untreated hypertension can lead to kidney disease, heart disease, and stroke, accounting for 11.3 million deaths in 2021 alone. A small minority get their blood pressure under control with drug therapy, and some studies indicate that as little as half are taking their blood pressure medications as intended. Is this because the drugs' effectiveness and side effects differ between different individuals? If so, there would be a substantial risk that patients will not get their optimal medication on the first try, with poor blood pressure lowering and unnecessary side effects as a result.
In a new clinical trial in Sweden, it was studied whether there is an optimal blood pressure medication for each person, and thus a potential for personalized blood pressure treatment. In the study, 280 people with high blood pressure tried out four different blood pressure drugs on several different occasions over a total of one year.

 Prof. Rahimi[/caption]
Kazem Rahimi FRCP, DM, MSc, FESC
Professor of Cardiovascular Medicine and Population Health
University of Oxford
Consultant cardiologist
Oxford University Hospitals NHS Trust
MedicalResearch.com: What is the background for this study?
Response: The prevalence of hypertension has been rising worldwide. To mitigate the burden, identifying the modifiable environmental risk factors of hypertension and developing preventive interventions constitute important public health priorities. Despite the biological plausibility of the link between road traffic noise and the risk of hypertension, the quality of relevant evidence has been low, and the role of air pollution has been uncertain.
Prof. Rahimi[/caption]
Kazem Rahimi FRCP, DM, MSc, FESC
Professor of Cardiovascular Medicine and Population Health
University of Oxford
Consultant cardiologist
Oxford University Hospitals NHS Trust
MedicalResearch.com: What is the background for this study?
Response: The prevalence of hypertension has been rising worldwide. To mitigate the burden, identifying the modifiable environmental risk factors of hypertension and developing preventive interventions constitute important public health priorities. Despite the biological plausibility of the link between road traffic noise and the risk of hypertension, the quality of relevant evidence has been low, and the role of air pollution has been uncertain.

 Prof. McManus[/caption]
Richard McManus MA PhD MBBS FRCGP FRCP
Professor of Primary Care
Dr. McManus chairs the Blood Pressure Monitoring Working Party
of the British Hypertension Society
Nuffield Department of Primary Care Health Sciences
MedicalResearch.com: What is the background for this study?
Response: About one in ten people who are pregnant develop high blood pressure and almost half of these go onto to have pre-eclampsia. Many pregnant women and individuals are already measuring their own blood pressure – well over half of those with high blood pressure in a recent large survey in the UK but until recently there were no data to support this.
Prof. McManus[/caption]
Richard McManus MA PhD MBBS FRCGP FRCP
Professor of Primary Care
Dr. McManus chairs the Blood Pressure Monitoring Working Party
of the British Hypertension Society
Nuffield Department of Primary Care Health Sciences
MedicalResearch.com: What is the background for this study?
Response: About one in ten people who are pregnant develop high blood pressure and almost half of these go onto to have pre-eclampsia. Many pregnant women and individuals are already measuring their own blood pressure – well over half of those with high blood pressure in a recent large survey in the UK but until recently there were no data to support this.

 Dr. Palatini[/caption]
Paolo Palatini, M.D.
Professor of Internal Medicine
University of Padova
Padova, Italy
MedicalResearch.com: What is the background for this study?
Response: Up to now doctors measured blood pressure (BP) on standing only in elderly people on pharmacological treatment with the purpose of detecting orthostatic hypotension. In young-to-middle-age people BP is currently measured only in the lying or the sitting posture.
Our starting point was that young borderline hypertensive people have an increased sympathetic activity and thus they might be hyperreactive to physical stimuli such as assuming the orthostatic posture which may be deleterious in the long run. This hypothesis was tested in the HARVEST, a study initiated in Italy in 1990, in which over 1200 young patients screened for stage 1 hypertension were enrolled.
Dr. Palatini[/caption]
Paolo Palatini, M.D.
Professor of Internal Medicine
University of Padova
Padova, Italy
MedicalResearch.com: What is the background for this study?
Response: Up to now doctors measured blood pressure (BP) on standing only in elderly people on pharmacological treatment with the purpose of detecting orthostatic hypotension. In young-to-middle-age people BP is currently measured only in the lying or the sitting posture.
Our starting point was that young borderline hypertensive people have an increased sympathetic activity and thus they might be hyperreactive to physical stimuli such as assuming the orthostatic posture which may be deleterious in the long run. This hypothesis was tested in the HARVEST, a study initiated in Italy in 1990, in which over 1200 young patients screened for stage 1 hypertension were enrolled.

 Dr. Launer[/caption]
Lenore J. Launer, Ph.D.
Chief, Laboratory of Epidemiology and Population Sciences
Intramural Research Program, National Institute on Aging.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Identifying early risk factors and early changes in the brain will have a major impact on future clinical and public health priorities related to the looming epidemic of dementia. Several studies based on older populations suggest mid-life is an important period to start prevention measures. To date control of blood pressure levels has been the most robust and promising candidate to target for prevention of future cognitive impairment. Although several studies have looked at levels of blood pressure and risk for cognitive impairment, it was not known whether trajectories from young adulthood to middle age studies provided additional information about risk. To investigate possible biomarkers of future risk, we chose to examine the association of the mean arterial blood pressure trajectories to indicators of pathology seen on MRI and that are associated with cognition.
We highlight the results of the mean arterial blood pressure (MAP) measure, which is an integrated measure of systolic and diastolic blood pressure.
Dr. Launer[/caption]
Lenore J. Launer, Ph.D.
Chief, Laboratory of Epidemiology and Population Sciences
Intramural Research Program, National Institute on Aging.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Identifying early risk factors and early changes in the brain will have a major impact on future clinical and public health priorities related to the looming epidemic of dementia. Several studies based on older populations suggest mid-life is an important period to start prevention measures. To date control of blood pressure levels has been the most robust and promising candidate to target for prevention of future cognitive impairment. Although several studies have looked at levels of blood pressure and risk for cognitive impairment, it was not known whether trajectories from young adulthood to middle age studies provided additional information about risk. To investigate possible biomarkers of future risk, we chose to examine the association of the mean arterial blood pressure trajectories to indicators of pathology seen on MRI and that are associated with cognition.
We highlight the results of the mean arterial blood pressure (MAP) measure, which is an integrated measure of systolic and diastolic blood pressure.
 Dr. LaMonte[/caption]
Michael J. LaMonte, PhD, MPH
Research Professor (epidemiology)
Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
Women’s Health Initiative Northeast Regional Center
University at Buffalo – SUNY
Buffalo, NY 14214
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. LaMonte: The rationale for this study was based on existing study results showing
Dr. LaMonte[/caption]
Michael J. LaMonte, PhD, MPH
Research Professor (epidemiology)
Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
Women’s Health Initiative Northeast Regional Center
University at Buffalo – SUNY
Buffalo, NY 14214
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. LaMonte: The rationale for this study was based on existing study results showing
 Dr. van Dalen[/caption]
Jan Willem van Dalen, PhD
Department of Neurology
Donders Institute for Brain, Behaviour and Cognition
Radboud University Medical Centre Nijmegen
Department of Neurology
The Netherlands3Department of Public and Occupational Health
Amsterdam UMC, University of Amsterdam, Amsterdam
MedicalResearch.com: What is the background for this study?
Response: Although high systolic blood pressure in midlife has consistently been reported as a condition that increases the risk of developing dementia in old age, reports regarding this relationship in older people have been inconsistent. One potential reason for this, is that the relationship between systolic blood pressure and dementia in later life may be U-shaped, meaning that both individuals with low and with high systolic blood pressure are at increased incident dementia risk.
This study combined data from several longitudinal cohort studies specifically designed to study incident dementia in older people, to investigate whether these U-shaped relationships exist, and in which age ranges they appear. We included more than 16,500 people aged 60 and older, with over 2,700 incident dementia cases.
Also, we aimed to investigate whether these observational associations might be caused by confounding, differences in mortality, or result from opposite relationships between certain subgroups of individuals.
Dr. van Dalen[/caption]
Jan Willem van Dalen, PhD
Department of Neurology
Donders Institute for Brain, Behaviour and Cognition
Radboud University Medical Centre Nijmegen
Department of Neurology
The Netherlands3Department of Public and Occupational Health
Amsterdam UMC, University of Amsterdam, Amsterdam
MedicalResearch.com: What is the background for this study?
Response: Although high systolic blood pressure in midlife has consistently been reported as a condition that increases the risk of developing dementia in old age, reports regarding this relationship in older people have been inconsistent. One potential reason for this, is that the relationship between systolic blood pressure and dementia in later life may be U-shaped, meaning that both individuals with low and with high systolic blood pressure are at increased incident dementia risk.
This study combined data from several longitudinal cohort studies specifically designed to study incident dementia in older people, to investigate whether these U-shaped relationships exist, and in which age ranges they appear. We included more than 16,500 people aged 60 and older, with over 2,700 incident dementia cases.
Also, we aimed to investigate whether these observational associations might be caused by confounding, differences in mortality, or result from opposite relationships between certain subgroups of individuals.


 Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.
Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.
 Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).
Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).
 Dr. Lopez[/caption]
Maria Luisa S. Sequeira Lopez, MD, FAHA
Harrison Distinguished Professor in Pediatrics and Biology
University of Virginia
Charlottesville, VA 22908
MedicalResearch.com: What is the background for this study?
Response: The renin-angiotensin system (RAS) is crucial in the regulation of the blood pressure (BP). Synthesis and secretion of renin is the key regulated event in the operation of the RAS.
One of the main mechanisms that control renin synthesis and release is the baroreceptor mechanism whereby a decrease in blood pressure results in increased release of renin by juxtaglomerular (JG) cells.
In spite of its enormous importance, the nature and location of the renal baroreceptor was still unknown. This was due in great part to the lack of appropriate in vitro and in vivo models to confidently allow tracking of the fate and isolation of renin cells, and the lack of tools to study the chromatin in scarce cells.
Dr. Lopez[/caption]
Maria Luisa S. Sequeira Lopez, MD, FAHA
Harrison Distinguished Professor in Pediatrics and Biology
University of Virginia
Charlottesville, VA 22908
MedicalResearch.com: What is the background for this study?
Response: The renin-angiotensin system (RAS) is crucial in the regulation of the blood pressure (BP). Synthesis and secretion of renin is the key regulated event in the operation of the RAS.
One of the main mechanisms that control renin synthesis and release is the baroreceptor mechanism whereby a decrease in blood pressure results in increased release of renin by juxtaglomerular (JG) cells.
In spite of its enormous importance, the nature and location of the renal baroreceptor was still unknown. This was due in great part to the lack of appropriate in vitro and in vivo models to confidently allow tracking of the fate and isolation of renin cells, and the lack of tools to study the chromatin in scarce cells.
 Dr. Nation[/caption]
Daniel A. Nation, Ph.D.,
Associate Professor of Psychological Science
Institute for Memory Impairments and Neurological Disorders
University of California, Irvin
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a risk factor for cognitive decline and dementia, and treatment of hypertension has been linked to decreased risk for cognitive impairment.
Prior studies have attempted to identify which specific type of antihypertensive treatment conveys the most benefit for cognition, but findings have been mixed regarding this question. We hypothesized that antihypertensive drugs acting on the brain angiotensin system may convey the greatest benefit since they affect the brain angiotensin system that has been implicated in memory function.
Dr. Nation[/caption]
Daniel A. Nation, Ph.D.,
Associate Professor of Psychological Science
Institute for Memory Impairments and Neurological Disorders
University of California, Irvin
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a risk factor for cognitive decline and dementia, and treatment of hypertension has been linked to decreased risk for cognitive impairment.
Prior studies have attempted to identify which specific type of antihypertensive treatment conveys the most benefit for cognition, but findings have been mixed regarding this question. We hypothesized that antihypertensive drugs acting on the brain angiotensin system may convey the greatest benefit since they affect the brain angiotensin system that has been implicated in memory function.
 Dr. Wong[/caption]
John B. Wong, M.D.
Chief Scientific Officer
Vice chair for Clinical Affairs
Chief of the Division of Clinical Decision Making and
Primary care Clinician
Department of Medicine at Tufts Medical Center
MedicalResearch.com: What is the background for this study?
Response: Hypertension affects nearly half of all adults in the United States and is a major risk factor for many serious health conditions. Fortunately, by screening all adults for hypertension, clinicians can improve their patient’s health. The Task Force continues to recommend screening all adults for hypertension so that they can get the care they need to help prevent health conditions such as heart attack, stroke, and kidney failure.
Dr. Wong[/caption]
John B. Wong, M.D.
Chief Scientific Officer
Vice chair for Clinical Affairs
Chief of the Division of Clinical Decision Making and
Primary care Clinician
Department of Medicine at Tufts Medical Center
MedicalResearch.com: What is the background for this study?
Response: Hypertension affects nearly half of all adults in the United States and is a major risk factor for many serious health conditions. Fortunately, by screening all adults for hypertension, clinicians can improve their patient’s health. The Task Force continues to recommend screening all adults for hypertension so that they can get the care they need to help prevent health conditions such as heart attack, stroke, and kidney failure.

 Prof. D'Aiuto[/caption]
Francesco D’Aiuto
Professor/Hon Consultant
Head of Periodontology Unit
UCL Eastman Dental Institute
MedicalResearch.com: What is the background for this study?
Response: This study was set out to further our understanding of the link between gum disease and high blood pressure. Recent evidence suggested that individuals with gum disease had a 20-70% increased risk of hypertension and systemic inflammation seemed to be a driver in mediating this association. Further research on the matter was needed. We recruited two relatively large groups of otherwise healthy participants (without a confirmed diagnosis of hypertension) who had gum disease one and healthy gums the other.
We found that diagnosis of periodontitis (gum disease) was consistently linked to higher systolic blood pressure independent of other cardiovascular risk factors.
Prof. D'Aiuto[/caption]
Francesco D’Aiuto
Professor/Hon Consultant
Head of Periodontology Unit
UCL Eastman Dental Institute
MedicalResearch.com: What is the background for this study?
Response: This study was set out to further our understanding of the link between gum disease and high blood pressure. Recent evidence suggested that individuals with gum disease had a 20-70% increased risk of hypertension and systemic inflammation seemed to be a driver in mediating this association. Further research on the matter was needed. We recruited two relatively large groups of otherwise healthy participants (without a confirmed diagnosis of hypertension) who had gum disease one and healthy gums the other.
We found that diagnosis of periodontitis (gum disease) was consistently linked to higher systolic blood pressure independent of other cardiovascular risk factors.
 Kathryn Foti, PhD, MPH
Postdoctoral fellow
Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: The Kidney Disease: Improving Global Outcomes (KDIGO) 2021 Clinical Practice Guideline for the Management of Blood Pressure (BP) in Chronic Kidney Disease (CKD) provides recommendations for the management of BP in individuals with nondialysis CKD, incorporating new evidence since the publication of its previous guideline in 2012.
The 2021 KDIGO guideline recommends a target systolic BP <120 mmHg based on standardized office BP measurement. This BP goal is largely informed by the findings of the SPRINT trial which found targeting SBP <120 mmHg compared with <140 mmHg reduced the risk of cardiovascular disease by 25% and all-cause mortality by 27%. The benefits were similar for participants with and without CKD.
In our study, we sought to examine the potential implications of the 2021 KDIGO guideline for BP lowering among US adults with CKD compared to the 2012 KDIGO guideline (target BP ≤130/80 mmHg in adults with albuminuria or ≤140/90 mmHg or under without albuminuria) and the 2017 American College of Cardiology/American Heart Association (target BP <130/80 mmHg) guideline. Additionally, we determined implications of the 2021 KDIGO guideline for angiotensin converting enzyme inhibitor (ACEi) or angiotensin II-receptor blocker (ARB) use for those with albuminuria (recommended at systolic BP ≥120 mmHg) compared to the 2012 KDIGO guideline (recommended at BP >130/80 mmHg).
Kathryn Foti, PhD, MPH
Postdoctoral fellow
Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: The Kidney Disease: Improving Global Outcomes (KDIGO) 2021 Clinical Practice Guideline for the Management of Blood Pressure (BP) in Chronic Kidney Disease (CKD) provides recommendations for the management of BP in individuals with nondialysis CKD, incorporating new evidence since the publication of its previous guideline in 2012.
The 2021 KDIGO guideline recommends a target systolic BP <120 mmHg based on standardized office BP measurement. This BP goal is largely informed by the findings of the SPRINT trial which found targeting SBP <120 mmHg compared with <140 mmHg reduced the risk of cardiovascular disease by 25% and all-cause mortality by 27%. The benefits were similar for participants with and without CKD.
In our study, we sought to examine the potential implications of the 2021 KDIGO guideline for BP lowering among US adults with CKD compared to the 2012 KDIGO guideline (target BP ≤130/80 mmHg in adults with albuminuria or ≤140/90 mmHg or under without albuminuria) and the 2017 American College of Cardiology/American Heart Association (target BP <130/80 mmHg) guideline. Additionally, we determined implications of the 2021 KDIGO guideline for angiotensin converting enzyme inhibitor (ACEi) or angiotensin II-receptor blocker (ARB) use for those with albuminuria (recommended at systolic BP ≥120 mmHg) compared to the 2012 KDIGO guideline (recommended at BP >130/80 mmHg).  Dr. Taub[/caption]
Pam R. Taub, MD, FACC, FASPC
Director of Step Family Foundation Cardiovascular Rehabilitation and Wellness Center
Associate Professor of Medicine
UC San Diego Health System
Division of Cardiovascular Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by postural orthostatic tachycardia syndrome? Is it more common in patients who have incompletely recovered from a COVID-19 infection?
Response: Postural Orthostatic Tachycardia Syndrome (POTS) is a, complex multisystem clinical syndrome Patients experience a wide spectrum of symptoms of varying severity, which are often debilitating. Upon assuming an upright standing position from being supine, patients experience an increase in heart rate by 30 beats per minute (bpm) from supine position, This is often accompanied by lightheadedness, palpitations, dyspnea, mental clouding (“brain fog”), headaches.
POTS can occur after infections as it thought to be triggered by the immune system . The hypothesis is that when the body is fighting an infection some of the antibodies it produces can attack our regulatory systems that control heart rate and blood pressure.
We are seeing an increase in POTS cases occurring after COVID-19 infection. These patient are referred to as the “long haulers”
These long haulers have elevated heart rate, fatigue, brain fog and shortness of breath with activity consistent with POTS.
We are seeing that COVID-19 is another infection that can lead to POTS.
Some articles on this
Dr. Taub[/caption]
Pam R. Taub, MD, FACC, FASPC
Director of Step Family Foundation Cardiovascular Rehabilitation and Wellness Center
Associate Professor of Medicine
UC San Diego Health System
Division of Cardiovascular Medicine
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by postural orthostatic tachycardia syndrome? Is it more common in patients who have incompletely recovered from a COVID-19 infection?
Response: Postural Orthostatic Tachycardia Syndrome (POTS) is a, complex multisystem clinical syndrome Patients experience a wide spectrum of symptoms of varying severity, which are often debilitating. Upon assuming an upright standing position from being supine, patients experience an increase in heart rate by 30 beats per minute (bpm) from supine position, This is often accompanied by lightheadedness, palpitations, dyspnea, mental clouding (“brain fog”), headaches.
POTS can occur after infections as it thought to be triggered by the immune system . The hypothesis is that when the body is fighting an infection some of the antibodies it produces can attack our regulatory systems that control heart rate and blood pressure.
We are seeing an increase in POTS cases occurring after COVID-19 infection. These patient are referred to as the “long haulers”
These long haulers have elevated heart rate, fatigue, brain fog and shortness of breath with activity consistent with POTS.
We are seeing that COVID-19 is another infection that can lead to POTS.
Some articles on this
 Response: The background for the study is the steady rise of cannabis use as a therapeutic in Israel and in many countries around the world. This largest increasing population of patients treated with medical cannabis is the older adults. However, very little data was published about cannabis treatment in older adults, and specifically about the cardiovascular and metabolic implications. T
he main finding of the study is that cannabis treatment for 3 months was associated with a reduction in both systolic and diastolic blood pressure values, as measured by consequent 24-hours ABPM tests. In addition, no significant changes were found in blood lipids profile, hemoglobin A1C, fasting insulin, C-reactive protein, kidney function tests, electrolytes, anthropometric measurements, and ECG parameters.
Response: The background for the study is the steady rise of cannabis use as a therapeutic in Israel and in many countries around the world. This largest increasing population of patients treated with medical cannabis is the older adults. However, very little data was published about cannabis treatment in older adults, and specifically about the cardiovascular and metabolic implications. T
he main finding of the study is that cannabis treatment for 3 months was associated with a reduction in both systolic and diastolic blood pressure values, as measured by consequent 24-hours ABPM tests. In addition, no significant changes were found in blood lipids profile, hemoglobin A1C, fasting insulin, C-reactive protein, kidney function tests, electrolytes, anthropometric measurements, and ECG parameters.