Author Interviews, Education, Health Care Workers, Menopause, University of Pittsburgh / 07.08.2025
What to Know Before Starting a Career in Health
[caption id="attachment_70198" align="aligncenter" width="500"] Source[/caption]
Ever watched a nurse steady a patient’s arm during an injection, answer a family’s questions, juggle documentation, and still keep calm—then thought, I could do that? It’s a common spark. Health careers are high-impact, in demand, and offer the kind of work that feels meaningful. But behind the scrubs and steady hands is a world that asks more than most people expect. In this blog, we will share what you need to know before stepping into a health career.
Start With the Structure, Not the Aesthetic
Everyone sees the outside first—neatly pressed uniforms, digital charts, exam gloves, badges swinging from lanyards. What’s less obvious is the scaffolding beneath. Health work is layered. Each role connects to others, and each tier carries specific responsibilities, training, and legal scope. If you're picturing your future in health, the first thing to understand is where you want to start, how far you want to go, and what that pathway actually involves.
Titles aren’t interchangeable. The difference between a nurse who administers medication and one who diagnoses conditions is more than experience—it’s formal licensing, state-defined boundaries, and years of education. This is where questions like LPN vs nurse practitioner become more than trivia. A Licensed Practical Nurse supports care under the supervision of RNs or physicians, usually after completing a year-long program. A Nurse Practitioner, on the other hand, holds a graduate degree, can assess and diagnose independently in many states, and often carries a caseload similar to a primary care provider.
Understanding the distinctions early can save years of missteps. Every job in the system matters, but they’re built on different skill sets. If you want flexibility, long-term growth, or eventual autonomy, you need to plan for that at the start—not halfway through your training. This doesn’t mean locking in a decision forever. It means knowing what each credential unlocks, so you can move with purpose, not guesswork.
Source[/caption]
Ever watched a nurse steady a patient’s arm during an injection, answer a family’s questions, juggle documentation, and still keep calm—then thought, I could do that? It’s a common spark. Health careers are high-impact, in demand, and offer the kind of work that feels meaningful. But behind the scrubs and steady hands is a world that asks more than most people expect. In this blog, we will share what you need to know before stepping into a health career.
Start With the Structure, Not the Aesthetic
Everyone sees the outside first—neatly pressed uniforms, digital charts, exam gloves, badges swinging from lanyards. What’s less obvious is the scaffolding beneath. Health work is layered. Each role connects to others, and each tier carries specific responsibilities, training, and legal scope. If you're picturing your future in health, the first thing to understand is where you want to start, how far you want to go, and what that pathway actually involves.
Titles aren’t interchangeable. The difference between a nurse who administers medication and one who diagnoses conditions is more than experience—it’s formal licensing, state-defined boundaries, and years of education. This is where questions like LPN vs nurse practitioner become more than trivia. A Licensed Practical Nurse supports care under the supervision of RNs or physicians, usually after completing a year-long program. A Nurse Practitioner, on the other hand, holds a graduate degree, can assess and diagnose independently in many states, and often carries a caseload similar to a primary care provider.
Understanding the distinctions early can save years of missteps. Every job in the system matters, but they’re built on different skill sets. If you want flexibility, long-term growth, or eventual autonomy, you need to plan for that at the start—not halfway through your training. This doesn’t mean locking in a decision forever. It means knowing what each credential unlocks, so you can move with purpose, not guesswork.
 Source[/caption]
Ever watched a nurse steady a patient’s arm during an injection, answer a family’s questions, juggle documentation, and still keep calm—then thought, I could do that? It’s a common spark. Health careers are high-impact, in demand, and offer the kind of work that feels meaningful. But behind the scrubs and steady hands is a world that asks more than most people expect. In this blog, we will share what you need to know before stepping into a health career.
Start With the Structure, Not the Aesthetic
Everyone sees the outside first—neatly pressed uniforms, digital charts, exam gloves, badges swinging from lanyards. What’s less obvious is the scaffolding beneath. Health work is layered. Each role connects to others, and each tier carries specific responsibilities, training, and legal scope. If you're picturing your future in health, the first thing to understand is where you want to start, how far you want to go, and what that pathway actually involves.
Titles aren’t interchangeable. The difference between a nurse who administers medication and one who diagnoses conditions is more than experience—it’s formal licensing, state-defined boundaries, and years of education. This is where questions like LPN vs nurse practitioner become more than trivia. A Licensed Practical Nurse supports care under the supervision of RNs or physicians, usually after completing a year-long program. A Nurse Practitioner, on the other hand, holds a graduate degree, can assess and diagnose independently in many states, and often carries a caseload similar to a primary care provider.
Understanding the distinctions early can save years of missteps. Every job in the system matters, but they’re built on different skill sets. If you want flexibility, long-term growth, or eventual autonomy, you need to plan for that at the start—not halfway through your training. This doesn’t mean locking in a decision forever. It means knowing what each credential unlocks, so you can move with purpose, not guesswork.
Source[/caption]
Ever watched a nurse steady a patient’s arm during an injection, answer a family’s questions, juggle documentation, and still keep calm—then thought, I could do that? It’s a common spark. Health careers are high-impact, in demand, and offer the kind of work that feels meaningful. But behind the scrubs and steady hands is a world that asks more than most people expect. In this blog, we will share what you need to know before stepping into a health career.
Start With the Structure, Not the Aesthetic
Everyone sees the outside first—neatly pressed uniforms, digital charts, exam gloves, badges swinging from lanyards. What’s less obvious is the scaffolding beneath. Health work is layered. Each role connects to others, and each tier carries specific responsibilities, training, and legal scope. If you're picturing your future in health, the first thing to understand is where you want to start, how far you want to go, and what that pathway actually involves.
Titles aren’t interchangeable. The difference between a nurse who administers medication and one who diagnoses conditions is more than experience—it’s formal licensing, state-defined boundaries, and years of education. This is where questions like LPN vs nurse practitioner become more than trivia. A Licensed Practical Nurse supports care under the supervision of RNs or physicians, usually after completing a year-long program. A Nurse Practitioner, on the other hand, holds a graduate degree, can assess and diagnose independently in many states, and often carries a caseload similar to a primary care provider.
Understanding the distinctions early can save years of missteps. Every job in the system matters, but they’re built on different skill sets. If you want flexibility, long-term growth, or eventual autonomy, you need to plan for that at the start—not halfway through your training. This doesn’t mean locking in a decision forever. It means knowing what each credential unlocks, so you can move with purpose, not guesswork.







 Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
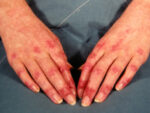
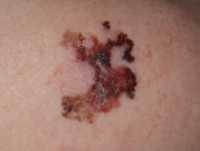
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.
Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.

 Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
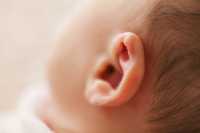
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.
Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.

 Dr. El Khoudary[/caption]
Samar El Khoudary, PhD, MPH, BPharm, FAHA
Associate Professor of Epidemiology
University of Pittsburgh Graduate School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Research increasingly shows that it isn’t so important how much fat a woman is carrying, which doctors typically measure using weight and BMI, as it is where she is carrying that fat. To investigate this, we looked at 25 years of data on 362 women from Pittsburgh and Chicago who participated in the
Dr. El Khoudary[/caption]
Samar El Khoudary, PhD, MPH, BPharm, FAHA
Associate Professor of Epidemiology
University of Pittsburgh Graduate School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Research increasingly shows that it isn’t so important how much fat a woman is carrying, which doctors typically measure using weight and BMI, as it is where she is carrying that fat. To investigate this, we looked at 25 years of data on 362 women from Pittsburgh and Chicago who participated in the 














 Dr. Schneider[/caption]
Dr. Michael Schneider DC, PhD
Associate Professor
School of Health and Rehabilitation Sciences
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
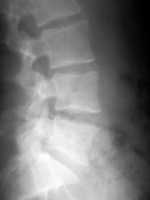
Response: Lumbar spinal stenosis (LSS) is one of the fastest growing problems in the country due to its aging population. One third of Medicare users have the condition, and it is the number one reason for spine surgery in this population. Existing research evaluates the benefits of nonsurgical treatment options compared to surgery, but there was no existing research that compared the available nonsurgical options to each other to determine the best course of treatment for each patient.
We studied three nonsurgical treatments for LSS: medical management with medications and/or epidural injections, individualized care with a physical therapist or chiropractor, and group exercise. We assessed each of these treatment methods with a questionnaire, a walking distance test, and a physical activity monitor.
Dr. Schneider[/caption]
Dr. Michael Schneider DC, PhD
Associate Professor
School of Health and Rehabilitation Sciences
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: Lumbar spinal stenosis (LSS) is one of the fastest growing problems in the country due to its aging population. One third of Medicare users have the condition, and it is the number one reason for spine surgery in this population. Existing research evaluates the benefits of nonsurgical treatment options compared to surgery, but there was no existing research that compared the available nonsurgical options to each other to determine the best course of treatment for each patient.
We studied three nonsurgical treatments for LSS: medical management with medications and/or epidural injections, individualized care with a physical therapist or chiropractor, and group exercise. We assessed each of these treatment methods with a questionnaire, a walking distance test, and a physical activity monitor.