Immunotherapy, Pharmaceutical Companies / 26.03.2026
The Evolving Landscape of Immunogenicity Risk Assessment in Biologic Drug Development
[caption id="attachment_72949" align="aligncenter" width="500"] Photo by Daniel Dan on Unsplash[/caption]
As biologic therapeutics continue to reshape modern medicine — from monoclonal antibodies to gene therapies and fusion proteins — one of the most consequential challenges facing drug developers remains largely invisible to the public: the immune response a patient’s own body may mount against a therapeutic protein. Immunogenicity, defined as the propensity of a biologic to trigger an unwanted immune response, can range from a clinically silent laboratory finding to a life-threatening hypersensitivity reaction or a complete loss of therapeutic efficacy. Understanding and mitigating this risk has become a cornerstone of the modern drug development paradigm.
Photo by Daniel Dan on Unsplash[/caption]
As biologic therapeutics continue to reshape modern medicine — from monoclonal antibodies to gene therapies and fusion proteins — one of the most consequential challenges facing drug developers remains largely invisible to the public: the immune response a patient’s own body may mount against a therapeutic protein. Immunogenicity, defined as the propensity of a biologic to trigger an unwanted immune response, can range from a clinically silent laboratory finding to a life-threatening hypersensitivity reaction or a complete loss of therapeutic efficacy. Understanding and mitigating this risk has become a cornerstone of the modern drug development paradigm.
 Photo by Daniel Dan on Unsplash[/caption]
As biologic therapeutics continue to reshape modern medicine — from monoclonal antibodies to gene therapies and fusion proteins — one of the most consequential challenges facing drug developers remains largely invisible to the public: the immune response a patient’s own body may mount against a therapeutic protein. Immunogenicity, defined as the propensity of a biologic to trigger an unwanted immune response, can range from a clinically silent laboratory finding to a life-threatening hypersensitivity reaction or a complete loss of therapeutic efficacy. Understanding and mitigating this risk has become a cornerstone of the modern drug development paradigm.
Photo by Daniel Dan on Unsplash[/caption]
As biologic therapeutics continue to reshape modern medicine — from monoclonal antibodies to gene therapies and fusion proteins — one of the most consequential challenges facing drug developers remains largely invisible to the public: the immune response a patient’s own body may mount against a therapeutic protein. Immunogenicity, defined as the propensity of a biologic to trigger an unwanted immune response, can range from a clinically silent laboratory finding to a life-threatening hypersensitivity reaction or a complete loss of therapeutic efficacy. Understanding and mitigating this risk has become a cornerstone of the modern drug development paradigm.










 Prof. Dubinsky[/caption]
Marla Dubinsky, M.D.
Professor of Pediatrics and Medicine
Co-director of the Susan and Leonard Feinstein IBD Clinical Center
Chief of the Division of Pediatric Gastroenterology and Nutrition
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? How does MIRIKIZUMAB differ from other medications for UC?
Response: This is a phase 2 study to assess the PK (pharamcokinetics), safety and efficacy of mirikizumab in pediatric ulcerative colitis (UC).
Prof. Dubinsky[/caption]
Marla Dubinsky, M.D.
Professor of Pediatrics and Medicine
Co-director of the Susan and Leonard Feinstein IBD Clinical Center
Chief of the Division of Pediatric Gastroenterology and Nutrition
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? How does MIRIKIZUMAB differ from other medications for UC?
Response: This is a phase 2 study to assess the PK (pharamcokinetics), safety and efficacy of mirikizumab in pediatric ulcerative colitis (UC).

 Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology




 Dr. Leonard[/caption]
Dr. Cathy Leonard PhD
Department of Infection and Immunity
Luxembourg Institute of Health
Luxembourg
MedicalResearch.com: What is the background for this study?
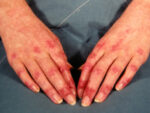
Response: Cat allergy is a rapidly increasing phenomenon characterized by hypersensitivity and an excessive immune response to certain allergens associated with cats, among which the major allergen Fel d 1, a protein typically found in their saliva, on their skin and fur. Cat allergy manifestations can range from mild forms like itchy nose or sneezing to the development of severe symptoms such as rhinitis and asthma, with potentially fatal outcomes.
Only Allergen‐specific immunotherapy (AIT )can ensure an effective and longer lasting treatment in the more advanced cases. AIT typically consists in the subcutaneous injection of gradually increasing doses of the allergen of interest, until a critical quantity is reached that induces long-term immune tolerance. Nevertheless, there is still the need to improve cat AIT in terms of efficacy and safety. We hypothesized that immune tolerance to the allergen could be boosted by improving the adjuvanticity of AIT solutions, thereby optimizing the production of antibodies against Fel d 1, while minimizing inflammation.
Dr. Leonard[/caption]
Dr. Cathy Leonard PhD
Department of Infection and Immunity
Luxembourg Institute of Health
Luxembourg
MedicalResearch.com: What is the background for this study?
Response: Cat allergy is a rapidly increasing phenomenon characterized by hypersensitivity and an excessive immune response to certain allergens associated with cats, among which the major allergen Fel d 1, a protein typically found in their saliva, on their skin and fur. Cat allergy manifestations can range from mild forms like itchy nose or sneezing to the development of severe symptoms such as rhinitis and asthma, with potentially fatal outcomes.
Only Allergen‐specific immunotherapy (AIT )can ensure an effective and longer lasting treatment in the more advanced cases. AIT typically consists in the subcutaneous injection of gradually increasing doses of the allergen of interest, until a critical quantity is reached that induces long-term immune tolerance. Nevertheless, there is still the need to improve cat AIT in terms of efficacy and safety. We hypothesized that immune tolerance to the allergen could be boosted by improving the adjuvanticity of AIT solutions, thereby optimizing the production of antibodies against Fel d 1, while minimizing inflammation. 

 Response: LENVIMA (lenvatinib), discovered and developed by Eisai, is an orally available multiple receptor tyrosine kinase inhibitor that inhibits the kinase activities of vascular endothelial growth factor (VEGF) receptors VEGFR1 (FLT1), VEGFR2 (KDR), and VEGFR3 (FLT4). LENVIMA inhibits other kinases that have been implicated in pathogenic angiogenesis, tumor growth, and cancer progression in addition to their normal cellular functions, including fibroblast growth factor (FGF) receptors FGFR1-4, the platelet derived growth factor receptor alpha (PDGFRα), KIT, and RET.
LENVIMA is approved in combination with everolimus for the treatment of patients with advanced renal cell carcinoma (RCC) following one prior anti-angiogenic therapy. The approved starting dose for LENVIMA is 18 mg daily. The objective of Study 218, a randomized, open-label, Phase 2 trial, was to assess whether the lower starting dose of LENVIMA (14 mg daily) in combination with everolimus (5 mg daily) would provide similar efficacy with an improved safety profile compared to the FDA-approved starting dose of LENVIMA (18 mg daily) plus everolimus (5 mg daily) in patients with advanced renal cell carcinoma (RCC) following prior treatment with an antiangiogenic therapy.
In the US, LENVIMA is also indicated for:
Response: LENVIMA (lenvatinib), discovered and developed by Eisai, is an orally available multiple receptor tyrosine kinase inhibitor that inhibits the kinase activities of vascular endothelial growth factor (VEGF) receptors VEGFR1 (FLT1), VEGFR2 (KDR), and VEGFR3 (FLT4). LENVIMA inhibits other kinases that have been implicated in pathogenic angiogenesis, tumor growth, and cancer progression in addition to their normal cellular functions, including fibroblast growth factor (FGF) receptors FGFR1-4, the platelet derived growth factor receptor alpha (PDGFRα), KIT, and RET.
LENVIMA is approved in combination with everolimus for the treatment of patients with advanced renal cell carcinoma (RCC) following one prior anti-angiogenic therapy. The approved starting dose for LENVIMA is 18 mg daily. The objective of Study 218, a randomized, open-label, Phase 2 trial, was to assess whether the lower starting dose of LENVIMA (14 mg daily) in combination with everolimus (5 mg daily) would provide similar efficacy with an improved safety profile compared to the FDA-approved starting dose of LENVIMA (18 mg daily) plus everolimus (5 mg daily) in patients with advanced renal cell carcinoma (RCC) following prior treatment with an antiangiogenic therapy.
In the US, LENVIMA is also indicated for:
 Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.
Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.






 Dr. Shaker[/caption]
Marcus S. Shaker, MD
Associate Professor of Pediatrics
Associate Professor of Community and Family Medicine
Dartmouth-Hitchcock Medical Center
MedicalResearch.com: What is the background for this study?
Response: There are two peanut allergy treatments that are being evaluated for potential FDA approval—an orally administered treatment and an epicutaneous (skin based) treatment. Both have tremendous potential benefit. The focus of our study was to explore the range of health and economic benefits in terms of establishing pathways for how each therapy could be cost effective.
We want to be clear that our purpose was not to suggest one therapy is or is not cost effective at present. That would be a ridiculous statement to make regarding two treatments that not only lack FDA approval, but do not have established pricing. Rather, we used preliminary inputs that are presently available to create as robust a model as we could to better determine the individual paths that would make them more or less cost-effective.
Dr. Shaker[/caption]
Marcus S. Shaker, MD
Associate Professor of Pediatrics
Associate Professor of Community and Family Medicine
Dartmouth-Hitchcock Medical Center
MedicalResearch.com: What is the background for this study?
Response: There are two peanut allergy treatments that are being evaluated for potential FDA approval—an orally administered treatment and an epicutaneous (skin based) treatment. Both have tremendous potential benefit. The focus of our study was to explore the range of health and economic benefits in terms of establishing pathways for how each therapy could be cost effective.
We want to be clear that our purpose was not to suggest one therapy is or is not cost effective at present. That would be a ridiculous statement to make regarding two treatments that not only lack FDA approval, but do not have established pricing. Rather, we used preliminary inputs that are presently available to create as robust a model as we could to better determine the individual paths that would make them more or less cost-effective.