Author Interviews, PT-Rehabilitation, Rheumatology / 18.04.2026
Compression Therapy for Knee Osteoarthritis: What the Evidence Shows
[caption id="attachment_73342" align="aligncenter" width="500"]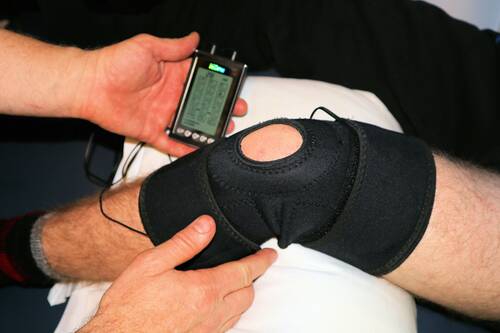 Photo by Terry Shultz P.T. on Unsplash[/caption]
Symptomatic knee osteoarthritis affects roughly 13.8 percent of adults over 40, making it one of the most common causes of chronic joint pain worldwide. As clinicians increasingly prioritize conservative management over early pharmacological intervention, non-pharmacological strategies have gained renewed attention. Among these, compression bracing has emerged as a subject of growing research interest, with recent meta-analyses suggesting measurable benefits for pain, stiffness, and physical function.
A body of evidence now supports the idea that compression knee support shown to improve joint proprioception through stimulation of cutaneous mechanoreceptors surrounding the joint capsule. This mechanism, first described in biomechanical research published in the Journal of Sports Science & Medicine (PubMed 15388537), offers a physiological rationale for what many patients report anecdotally: that wearing a compression sleeve makes the knee feel more stable during movement. For clinicians weighing treatment options, the question is no longer whether bracing has a role in osteoarthritis care, but which type of brace matches a given patient's needs.
Photo by Terry Shultz P.T. on Unsplash[/caption]
Symptomatic knee osteoarthritis affects roughly 13.8 percent of adults over 40, making it one of the most common causes of chronic joint pain worldwide. As clinicians increasingly prioritize conservative management over early pharmacological intervention, non-pharmacological strategies have gained renewed attention. Among these, compression bracing has emerged as a subject of growing research interest, with recent meta-analyses suggesting measurable benefits for pain, stiffness, and physical function.
A body of evidence now supports the idea that compression knee support shown to improve joint proprioception through stimulation of cutaneous mechanoreceptors surrounding the joint capsule. This mechanism, first described in biomechanical research published in the Journal of Sports Science & Medicine (PubMed 15388537), offers a physiological rationale for what many patients report anecdotally: that wearing a compression sleeve makes the knee feel more stable during movement. For clinicians weighing treatment options, the question is no longer whether bracing has a role in osteoarthritis care, but which type of brace matches a given patient's needs.
 Photo by Terry Shultz P.T. on Unsplash[/caption]
Symptomatic knee osteoarthritis affects roughly 13.8 percent of adults over 40, making it one of the most common causes of chronic joint pain worldwide. As clinicians increasingly prioritize conservative management over early pharmacological intervention, non-pharmacological strategies have gained renewed attention. Among these, compression bracing has emerged as a subject of growing research interest, with recent meta-analyses suggesting measurable benefits for pain, stiffness, and physical function.
A body of evidence now supports the idea that compression knee support shown to improve joint proprioception through stimulation of cutaneous mechanoreceptors surrounding the joint capsule. This mechanism, first described in biomechanical research published in the Journal of Sports Science & Medicine (PubMed 15388537), offers a physiological rationale for what many patients report anecdotally: that wearing a compression sleeve makes the knee feel more stable during movement. For clinicians weighing treatment options, the question is no longer whether bracing has a role in osteoarthritis care, but which type of brace matches a given patient's needs.
Photo by Terry Shultz P.T. on Unsplash[/caption]
Symptomatic knee osteoarthritis affects roughly 13.8 percent of adults over 40, making it one of the most common causes of chronic joint pain worldwide. As clinicians increasingly prioritize conservative management over early pharmacological intervention, non-pharmacological strategies have gained renewed attention. Among these, compression bracing has emerged as a subject of growing research interest, with recent meta-analyses suggesting measurable benefits for pain, stiffness, and physical function.
A body of evidence now supports the idea that compression knee support shown to improve joint proprioception through stimulation of cutaneous mechanoreceptors surrounding the joint capsule. This mechanism, first described in biomechanical research published in the Journal of Sports Science & Medicine (PubMed 15388537), offers a physiological rationale for what many patients report anecdotally: that wearing a compression sleeve makes the knee feel more stable during movement. For clinicians weighing treatment options, the question is no longer whether bracing has a role in osteoarthritis care, but which type of brace matches a given patient's needs.








 Dr. LaMoreaux[/caption]
Brian LaMoreaux, MD, MS
Internist and Rheumatologist
Executive Medical Director, Amgen
MedicalResearch.com: What is the background for this study? How does KRYSTEXXA® (pegloticase) work in gout?
Response: Many other diseases in gout have well-defined definitions of remission, but gout has lagged behind on this. With systemic consequences of gout becoming more apparent, the concept of treating gout to remission is increasing important to improving patient care and preserving patient health.
Dr. LaMoreaux[/caption]
Brian LaMoreaux, MD, MS
Internist and Rheumatologist
Executive Medical Director, Amgen
MedicalResearch.com: What is the background for this study? How does KRYSTEXXA® (pegloticase) work in gout?
Response: Many other diseases in gout have well-defined definitions of remission, but gout has lagged behind on this. With systemic consequences of gout becoming more apparent, the concept of treating gout to remission is increasing important to improving patient care and preserving patient health.



 Dr. Nowell[/caption]
W. Benjamin Nowell PhD
Director of Patient-Centered Research at Global Healthy Living Foundation
Columbia University in the City of New York
Dr. Nowell[/caption]
W. Benjamin Nowell PhD
Director of Patient-Centered Research at Global Healthy Living Foundation
Columbia University in the City of New York







 Dr. Connelly[/caption]
Stephen Connelly, PhD
Co-founder & Chief Scientific Officer
Dr. Connelly[/caption]
Stephen Connelly, PhD
Co-founder & Chief Scientific Officer

 Kelly Gavigan[/caption]
Kelly Gavigan, MPH
Manager, Research and Data Science
Kelly Gavigan[/caption]
Kelly Gavigan, MPH
Manager, Research and Data Science

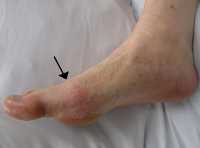
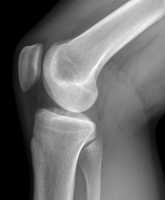


![MedicalResearch.com Interview with: Jeffrey D. Kent, M.D., FACG, FACP Executive Vice President, Medical Affairs and Outcomes Research Horizon MedicalResearch.com: What is the background for this study? What is the marker for reduced immunogenicity with Pegloticase? Response: Pegloticase is a recombinant, pegylated uricase that is used for treatment of chronic gout in patients who fail oral urate lowering therapy (uncontrolled gout) and has a demonstrated impact on the serum uric acid (sUA) level. As with other biologics, in some people the body’s immune system develops anti-drug antibodies and reduces the effectiveness of the biologic therapy. Recent case series and open-label trials have suggested that using an immunomodulator with pegloticase has the potential to increase the durability of response so patients can receive a full course of therapy. Researchers in the RECIPE trial sought to examine whether the co-administration of disease-modifying antirheumatic drugs (DMARDs), specifically mycophenolate mofetil, may mitigate this loss of efficacy and increase in response rates for people living with uncontrolled gout MedicalResearch.com: Are symptoms of gout improved as well as reduced infusion reactions? Response Results from this trial indicated that short-term concomitant use of mycophenolate mofetil with pegloticase was generally well tolerated. It was also associated with a statistically significant and clinically meaningful impact on the proportion of patients achieving and maintaining an sUA ≤6 mg/dL at 24 weeks. No infusion reactions were reported in the pegloticase/mycophenolate mofetil arm (0 or 22 patients) compared to 30 percent (3 of 10) of patients reporting infusion reactions in the pegloticase/placebo arm. It’s been well established that in patients receiving pegloticase with persistent urate lowering, they experience relatively rapid resolution of tophi indicating significant reductions in their urate burden. MedicalResearch.com: What are the main findings? Response: This is the first randomized controlled trial evaluating pegloticase co-prescribed with an immunomodulator compared to pegloticase with placebo. Data showed that 86.4 percent of patients (19 of 22) receiving co-therapy of pegloticase with mycophenolate mofetil achieved an sUA ≤ 6 mg/dL through Month 3, the primary study endpoint, compared to 40.0 percent of patients (4 of 10) receiving pegloticase monotherapy. After Month 3, all patients received pegloticase only and at Month 6 a sustained response was shown in 68.2 percent (15 of 22) of patients who had received pegloticase with mycophenolate mofetil versus 30.0 percent (3 of 10) of patients who received pegloticase and placebo. This data adds to the growing body of evidence on the concomitant use of pegloticase with an immunomodulator to ultimately help more patients receive a full course of therapy and improve outcomes and may help shift the treatment paradigm in uncontrolled gout. MedicalResearch.com: What should readers take away from your report? Response: While rheumatologists are familiar with and may use DMARDs for other autoimmune conditions to minimize the development of anti-drug antibodies and increase response to therapies, data shows that the use of an immunomodulating therapy in patients with uncontrolled gout can improve response rates. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: There is a consistent pattern demonstrating that the concomitant use of pegloticase and an immunomodulator can improve patient outcomes without introducing additional toxicities. As clinicians we understand the immense burden gout places on our patients. Future research should continue exploring options to maximize the benefit of effective treatments to improve patient outcomes. MedicalResearch.com: Is there anything else you would like to add? Response: Uncontrolled gout is a chronic, systemic inflammatory condition and we continue to see data linking it to many comorbid conditions. Horizon is evaluating the use of methotrexate to improve response rates for pegloticase. We are committed to exploring various immunotherapy co-treatment options to allow both patients and clinicians to address elevated sUA levels to minimize urate burden and avoid lasting damage to the body. RECIPE is an investigator-initiated trial led by Puja Khanna, M.D., M.P.H. and Kenneth Saag, M.D., M.Sc. Citation: Khanna P, Khanna D, Cutter G, Foster J, Melnick J, Jaafar S, Biggers S, Rahman A, Kuo H, Feese M, Saag K. Reducing Immunogenicity of Pegloticase (RECIPE) with Concomitant Use of Mycophenolate Mofetil in Patients with Refractory Gout—a Phase II Double Blind Randomized Controlled Trial [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/reducing-immunogenicity-of-pegloticase-recipe-with-concomitant-use-of-mycophenolate-mofetil-in-patients-with-refractory-gout-a-phase-ii-double-blind-randomized-controlled-trial/. Accessed November 12, 2020. [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/11/Dr-Jeffrey-Kent.jpg)

 Ruth Fernandez-Ruiz, MD
Post-Doctoral Fellow
Department of Rheumatology
NYU Langone Heath
MedicalResearch.com: What is the background for this study?
Response: Patients with systemic lupus erythematosus (SLE) represent a unique population in considering risk for COVID-19 with biologic, genetic, demographic, clinical and treatment issues at play. By the nature of their chronic inflammatory autoimmune condition, the presence of comorbidities, and regular use of immunosuppressants, these individuals would traditionally be considered at high risk of contracting SARS-CoV-2 and possibly having worse outcomes from the viral infection.
However, it might be speculated that inherently elevated type I Interferon, characteristic of the majority of patients with SLE, confers a protective effect as a first line anti-viral defense. Additionally, hydroxychloroquine, which was suggested as a potential therapeutic agent for COVID-19 early on, is used in most patients with SLE. Accordingly, we initiated this study to provide critical data needed to address the frequency and severity of COVID-19 in patients with SLE.
Ruth Fernandez-Ruiz, MD
Post-Doctoral Fellow
Department of Rheumatology
NYU Langone Heath
MedicalResearch.com: What is the background for this study?
Response: Patients with systemic lupus erythematosus (SLE) represent a unique population in considering risk for COVID-19 with biologic, genetic, demographic, clinical and treatment issues at play. By the nature of their chronic inflammatory autoimmune condition, the presence of comorbidities, and regular use of immunosuppressants, these individuals would traditionally be considered at high risk of contracting SARS-CoV-2 and possibly having worse outcomes from the viral infection.
However, it might be speculated that inherently elevated type I Interferon, characteristic of the majority of patients with SLE, confers a protective effect as a first line anti-viral defense. Additionally, hydroxychloroquine, which was suggested as a potential therapeutic agent for COVID-19 early on, is used in most patients with SLE. Accordingly, we initiated this study to provide critical data needed to address the frequency and severity of COVID-19 in patients with SLE.


 Dr. LaMoreaux[/caption]
Brian LaMoreaux, M.D., M.S.
Medical Director, Medical Affairs
Horizon Therapeutics
MedicalResearch.com: What is the background for this study?
Response: Hyperuricemia is associated with non-alcoholic fatty liver disease (NAFLD) but the relationship to fibrosis remains uncertain. Moreover, it is not known whether lowering serum urate will affect the course of NAFLD.
Dr. LaMoreaux[/caption]
Brian LaMoreaux, M.D., M.S.
Medical Director, Medical Affairs
Horizon Therapeutics
MedicalResearch.com: What is the background for this study?
Response: Hyperuricemia is associated with non-alcoholic fatty liver disease (NAFLD) but the relationship to fibrosis remains uncertain. Moreover, it is not known whether lowering serum urate will affect the course of NAFLD.