Author Interviews, Gout, Rheumatology / 15.06.2020
Trends in Immunomodulation Co-Therapy with Pegloticase for Uncontrolled Gout
MedicalResearch.com Interview with:
[caption id="attachment_54552" align="alignleft" width="200"] Dr. LaMoreaux[/caption]
Brian LaMoreaux, M.D., M.S.
Medical Director, Medical Affairs
Horizon Therapeutics
MedicalResearch.com: What is the background for this study?
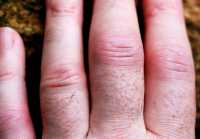
Response: Pegloticase is a PEGylated biologic therapy for patients with uncontrolled gout who have not improved on or could not tolerate conventional urate-lowering therapies. All biologics have the ability to engender anti-drug antibodies (ADAs) and it is known that some patients given pegloticase develop ADAs that cause them to stop treatment prior to receiving a complete course of therapy.
In other rheumatic autoimmune diseases, DMARDs such as methotrexate or azathioprine are used as standard of care to prevent the development of ADAs to biologics. These DMARDs often allow patients to remain on biologic therapies longer and receive the full therapeutic benefits while minimizing adverse events. While pegloticase has been used traditionally as monotherapy, recent case series have demonstrated the therapeutic benefit of immunomodulator co-administration, allowing more patients to receive a full course of pegloticase therapy. Little has been published on how widespread this practice is and whether it has changed over time.
Dr. LaMoreaux[/caption]
Brian LaMoreaux, M.D., M.S.
Medical Director, Medical Affairs
Horizon Therapeutics
MedicalResearch.com: What is the background for this study?
Response: Pegloticase is a PEGylated biologic therapy for patients with uncontrolled gout who have not improved on or could not tolerate conventional urate-lowering therapies. All biologics have the ability to engender anti-drug antibodies (ADAs) and it is known that some patients given pegloticase develop ADAs that cause them to stop treatment prior to receiving a complete course of therapy.
In other rheumatic autoimmune diseases, DMARDs such as methotrexate or azathioprine are used as standard of care to prevent the development of ADAs to biologics. These DMARDs often allow patients to remain on biologic therapies longer and receive the full therapeutic benefits while minimizing adverse events. While pegloticase has been used traditionally as monotherapy, recent case series have demonstrated the therapeutic benefit of immunomodulator co-administration, allowing more patients to receive a full course of pegloticase therapy. Little has been published on how widespread this practice is and whether it has changed over time.
 Dr. LaMoreaux[/caption]
Brian LaMoreaux, M.D., M.S.
Medical Director, Medical Affairs
Horizon Therapeutics
MedicalResearch.com: What is the background for this study?
Response: Pegloticase is a PEGylated biologic therapy for patients with uncontrolled gout who have not improved on or could not tolerate conventional urate-lowering therapies. All biologics have the ability to engender anti-drug antibodies (ADAs) and it is known that some patients given pegloticase develop ADAs that cause them to stop treatment prior to receiving a complete course of therapy.
In other rheumatic autoimmune diseases, DMARDs such as methotrexate or azathioprine are used as standard of care to prevent the development of ADAs to biologics. These DMARDs often allow patients to remain on biologic therapies longer and receive the full therapeutic benefits while minimizing adverse events. While pegloticase has been used traditionally as monotherapy, recent case series have demonstrated the therapeutic benefit of immunomodulator co-administration, allowing more patients to receive a full course of pegloticase therapy. Little has been published on how widespread this practice is and whether it has changed over time.
Dr. LaMoreaux[/caption]
Brian LaMoreaux, M.D., M.S.
Medical Director, Medical Affairs
Horizon Therapeutics
MedicalResearch.com: What is the background for this study?
Response: Pegloticase is a PEGylated biologic therapy for patients with uncontrolled gout who have not improved on or could not tolerate conventional urate-lowering therapies. All biologics have the ability to engender anti-drug antibodies (ADAs) and it is known that some patients given pegloticase develop ADAs that cause them to stop treatment prior to receiving a complete course of therapy.
In other rheumatic autoimmune diseases, DMARDs such as methotrexate or azathioprine are used as standard of care to prevent the development of ADAs to biologics. These DMARDs often allow patients to remain on biologic therapies longer and receive the full therapeutic benefits while minimizing adverse events. While pegloticase has been used traditionally as monotherapy, recent case series have demonstrated the therapeutic benefit of immunomodulator co-administration, allowing more patients to receive a full course of pegloticase therapy. Little has been published on how widespread this practice is and whether it has changed over time.




 Prof. Dagna[/caption]
Prof. Lorenzo Dagna MD FACP
Ospedale San Raffaele and
Vita-Salute San Raffaele University
Milan, Italy
MedicalResearch.com: What is the background for this study?
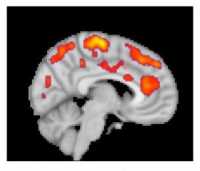
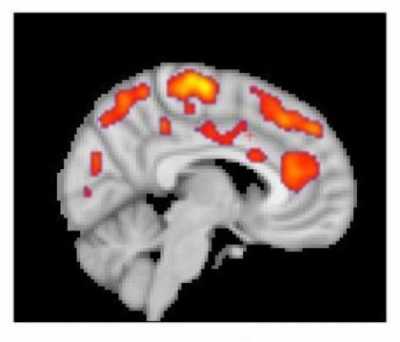
Response: Upon encountering pathogens, our immune system produces pro-inflammatory mediators, called cytokines. Cytokines activate cells from the immune system. In most people, production of cytokines is an appropriate and protective response to infection. However, some individuals develop excessive and detrimental inflammatory responses, which are even more harmful than the pathogen itself to the host organism.
We hypothesized that some patients with COVID-19 might develop excessive and detrimental inflammation, and that treatment with anti-inflammatory agents might be beneficial in this population.
Anakinra is an inhibitor of the pro-inflammatory molecule interleukin 1 (IL-1). It was originally marketed for the treatment of rheumatoid arthritis, but is now mostly used to treat a variety of pediatric inflammatory diseases.
Prof. Dagna[/caption]
Prof. Lorenzo Dagna MD FACP
Ospedale San Raffaele and
Vita-Salute San Raffaele University
Milan, Italy
MedicalResearch.com: What is the background for this study?
Response: Upon encountering pathogens, our immune system produces pro-inflammatory mediators, called cytokines. Cytokines activate cells from the immune system. In most people, production of cytokines is an appropriate and protective response to infection. However, some individuals develop excessive and detrimental inflammatory responses, which are even more harmful than the pathogen itself to the host organism.
We hypothesized that some patients with COVID-19 might develop excessive and detrimental inflammation, and that treatment with anti-inflammatory agents might be beneficial in this population.
Anakinra is an inhibitor of the pro-inflammatory molecule interleukin 1 (IL-1). It was originally marketed for the treatment of rheumatoid arthritis, but is now mostly used to treat a variety of pediatric inflammatory diseases.
 Dr. Ritch[/caption]
Robert Ritch, MD, FACS, FARVO
Shelley and Steven Einhorn Distinguished Chair
Professor of Ophthalmology, Surgeon Director Emeritus
Chief, Glaucoma Services Emeritus
The New York Eye and Ear Infirmary of Mount Sinai
New York, NY 10003
Founder, Medical Director and
Chairman, Scientific Advisory Board
The Glaucoma Foundation
MedicalResearch.com: What is the background for this study?
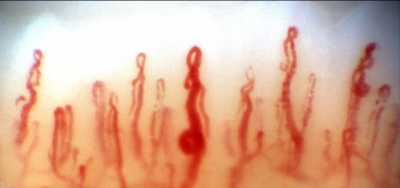
Response: Nailfold capillaroscopy (NFC), long used in rheumatology is a new approach to investigation of glaucoma.
Posterior to the nailbed and just anterior to the proximal nailfold is the cuticle, which has no structural elements visible to the naked eye. NFC is a non-invasive imaging modality that provides a highly magnified view of the capillaries at the nailfold of digits. It has also been used in ophthalmology to show morphological changes at the nailfold capillaries of POAG and XFG/XFS patients, helping to confirm the systemic nature of these diseases.
[caption id="attachment_52469" align="alignleft" width="400"]
Dr. Ritch[/caption]
Robert Ritch, MD, FACS, FARVO
Shelley and Steven Einhorn Distinguished Chair
Professor of Ophthalmology, Surgeon Director Emeritus
Chief, Glaucoma Services Emeritus
The New York Eye and Ear Infirmary of Mount Sinai
New York, NY 10003
Founder, Medical Director and
Chairman, Scientific Advisory Board
The Glaucoma Foundation
MedicalResearch.com: What is the background for this study?
Response: Nailfold capillaroscopy (NFC), long used in rheumatology is a new approach to investigation of glaucoma.
Posterior to the nailbed and just anterior to the proximal nailfold is the cuticle, which has no structural elements visible to the naked eye. NFC is a non-invasive imaging modality that provides a highly magnified view of the capillaries at the nailfold of digits. It has also been used in ophthalmology to show morphological changes at the nailfold capillaries of POAG and XFG/XFS patients, helping to confirm the systemic nature of these diseases.
[caption id="attachment_52469" align="alignleft" width="400"]