[caption id="attachment_64143" align="aligncenter" width="500"]
 Source
Source[/caption]
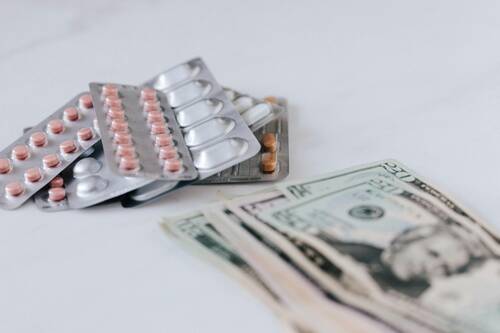
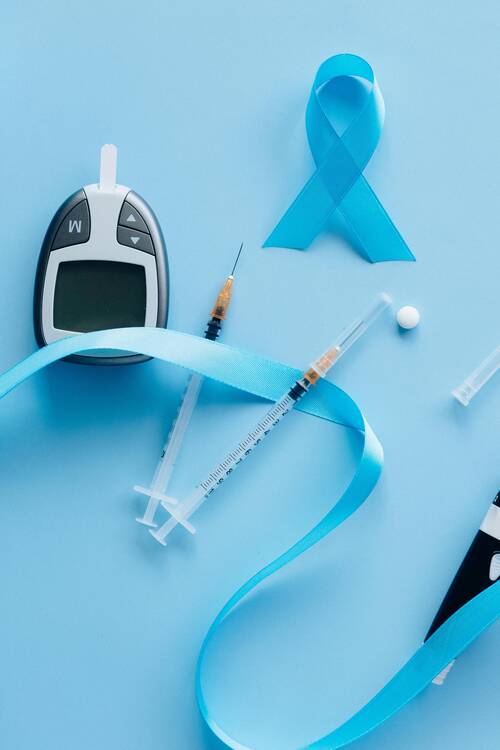
Access to affordable insulin remains a challenge for millions of people living with diabetes around the world, particularly in middle-income countries. To bridge this gap, platforms are emerging that connect patients with high-quality insulin at reduced prices. For individuals struggling to afford their life-saving medication, these services offer a convenient and affordable solution, making a significant impact on global health.
The Global Insulin Crisis
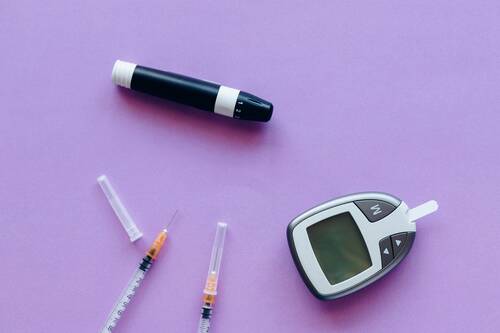
Diabetes affects millions worldwide, and the demand for insulin continues to rise. Major insulin manufacturers, including Novo Nordisk, Eli Lilly, and Sanofi, dominate the global market, producing essential medications for managing blood sugar levels. However, in many parts of the world, including countries like India, Mexico, and the Philippines, insulin prices remain prohibitively high. This leaves a substantial portion of the population without access to the medication they need to live healthy lives.
Data shows that insulin prices are often out of reach for people in middle-income countries. The situation is particularly dire in regions like Kenya, Malaysia, and Vietnam, where the cost of insulin may equal a month's salary. With nearly three major companies controlling the insulin market, competition is limited, and prices remain high. As a result, many patients with type 1 and type 2 diabetes face inconsistent access to insulin, which can put their health at significant risk.
 Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.
Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.