Editor's note: This piece discusses mental health issues. If you have experienced suicidal thoughts or have lost someone to suicide and want to seek help, you can contact the Crisis Text Line by texting "START" to 741-741 or call the Suicide Prevention Lifeline at 800-273-8255.
The world of mental healthcare has always been influenced by the world that people live in. As the world that people live in changes, the symptoms change too. A generation ago, there were many discussions in the world of psychiatry that focused on workplace stress, family problems, grief, addiction, and mood disorders that were quite familiar to most practitioners. Of course, these are still important issues, although the world that they occur in is quite different. Today, people are carrying around social pressure, information overload, algorithmic pressure, financial obsession, and always being available. The result is a new kind of emotional strain that often builds quietly before anyone names it.
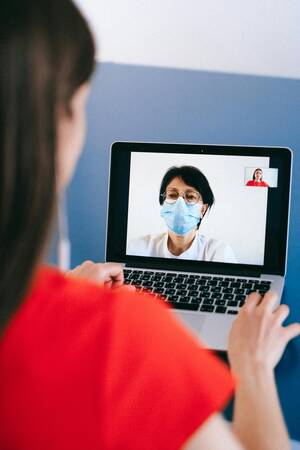
That is one reason more clinics and community systems are paying attention to telehealth psychiatry as a practical way to connect patients with specialists when local access is thin, schedules are crowded, or a person simply feels more able to open up through a screen. In many settings, this model has become especially relevant for people dealing with newer patterns of distress tied to technology itself, from compulsive market checking and online isolation to the strange emotional fallout of spending too much time in synthetic digital environments.
















 Dr. Avinesh Bhar[/caption]
Dr. Avinesh Bhar[/caption]






 Dr. Crowley[/caption]
Matthew J. Crowley, MD
Core Investigator, Durham Center of Innovation to Accelerate Discovery and Practice Transformation (ADAPT)
Affiliated Investigator, VA Office of Rural Health
Staff Physician, Endocrinology Section, Durham VA Health Care System
[caption id="attachment_54583" align="alignleft" width="144"]
Dr. Crowley[/caption]
Matthew J. Crowley, MD
Core Investigator, Durham Center of Innovation to Accelerate Discovery and Practice Transformation (ADAPT)
Affiliated Investigator, VA Office of Rural Health
Staff Physician, Endocrinology Section, Durham VA Health Care System
[caption id="attachment_54583" align="alignleft" width="144"]





 Dr. Mima Becevic[/caption]
Mirna Becevic, PhD, MHA
Assistant Research Professor
University of Missouri - Department of Dermatology
Missouri Telehealth Network
MedicalResearch.com: What is the background for this study?
Response: Psychiatry is, by far, the biggest utilizer of telemedicine services on the Missouri Telehealth Network (MTN). MTN supports an average of 4000 tele-psychiatry appointments every month, and 10% of those are provided by the University of Missouri Department of Psychiatry. Since we are all aware of the ever-increasing demand for child and adolescent psychiatry, but also the stigma that goes along with it, we wanted to examine more closely the actual usage of those services at the University of Missouri.
Dr. Mima Becevic[/caption]
Mirna Becevic, PhD, MHA
Assistant Research Professor
University of Missouri - Department of Dermatology
Missouri Telehealth Network
MedicalResearch.com: What is the background for this study?
Response: Psychiatry is, by far, the biggest utilizer of telemedicine services on the Missouri Telehealth Network (MTN). MTN supports an average of 4000 tele-psychiatry appointments every month, and 10% of those are provided by the University of Missouri Department of Psychiatry. Since we are all aware of the ever-increasing demand for child and adolescent psychiatry, but also the stigma that goes along with it, we wanted to examine more closely the actual usage of those services at the University of Missouri.