MedicalResearch.com Interview with:
[caption id="attachment_60038" align="alignleft" width="200"]

Dr. Schutz[/caption]
Michael R.
Schutz,
Ph.D.
Professor of Music Cognition/Percussion at McMaster University
Founding director of the
MAPLE Lab and
Core member of the McMaster Institute for Music and the Mind.
Prof. Schutz is also a professional musician and directs McMaster’s percussion ensemble.
MedicalResearch.com: What is the background for this study?
Response: Hospitals around the world are filled with devices generating a
constant stream of tones conveying information to medical staff.
overburdened healthcare professionals, and contributes to burnout in
medical staff. The Emergency Care Research Institute (ECRI) regularly
includes problems with auditory alarms in their list of "Top 10 Health
Technology Hazards" and they are so problematic an FDA survey
implicated them in hundreds of patient deaths.
While there is currently a lot of interest in how to improve alarm
management protocols, this study is different in that it looks at
improving the quality of the alarm sounds themselves. For historical
reasons many default to simplistic "beeps" which are generally
annoying. While annoying is useful for critical alarms requiring
immediate action, the vast majority of these messages are merely
intended to update medical staff of changes (i.e. blood pressure is
rising) or indicate other situations that do not require immediate
action. Unfortunately, many machines use the same simplistic and
annoying "beeps" regardless of whether the messages are urgent or
non-urgent. This constant flood of annoying beeps negatively affects
both patients (extending recovery time due to interrupted rest) and
staff (who can develop "alarm fatigue" from the constant cacophony).

















 The ResMed AirSense™ 10 AutoSet™ Tri-Pack is an essential package designed for individuals with sleep apnea who require consistent and effective therapy. This article delves into the key features benefits and frequently asked questions surrounding the ResMed AirSense™ 10 AutoSet™ Tri-Pack offering a guide to help you understand its significance in sleep apnea treatment.
What is the ResMed AirSense™ 10 AutoSet™ Tri-Pack?
The
The ResMed AirSense™ 10 AutoSet™ Tri-Pack is an essential package designed for individuals with sleep apnea who require consistent and effective therapy. This article delves into the key features benefits and frequently asked questions surrounding the ResMed AirSense™ 10 AutoSet™ Tri-Pack offering a guide to help you understand its significance in sleep apnea treatment.
What is the ResMed AirSense™ 10 AutoSet™ Tri-Pack?
The 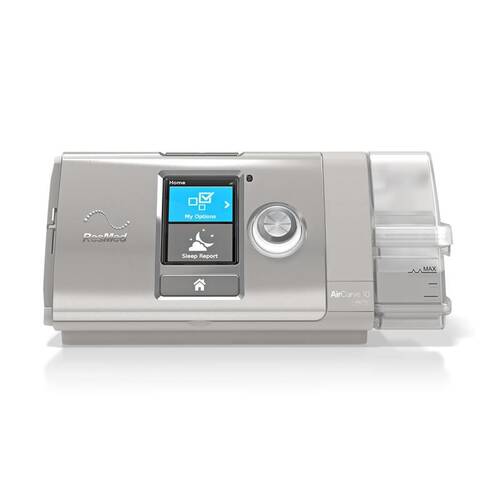





 Dr. Oliva[/caption]
Azahara Oliva PhD
Assistant Professor
Department of Neurobiology and Behavior
Cornell University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background is that we knew for a while now that neurons work hard to consolidate into memories each experience that we have during the day. But at the same time, it is known that sleep restore activity of our body and physiology. How was that possible? How can the neurons in our brain "work hard" during the time that we are supposed to be restoring our vitals? We found that in between their hard work, during sleep, our neurons take "breaks of activity" so our brain can build memories with precision.
Dr. Oliva[/caption]
Azahara Oliva PhD
Assistant Professor
Department of Neurobiology and Behavior
Cornell University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background is that we knew for a while now that neurons work hard to consolidate into memories each experience that we have during the day. But at the same time, it is known that sleep restore activity of our body and physiology. How was that possible? How can the neurons in our brain "work hard" during the time that we are supposed to be restoring our vitals? We found that in between their hard work, during sleep, our neurons take "breaks of activity" so our brain can build memories with precision.

 Dr. Avinesh Bhar[/caption]
Dr. Avinesh Bhar[/caption]

 Dr. Parekh[/caption]
Ankit Parekh, PhD
Director of the Sleep And Circadian Analysis (SCAN) Group
Assistant Professor of Medicine
(Pulmonary, Critical Care and Sleep Medicine)
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Sleep apnea is associated with incident cardiovascular disease, and is a common chronic condition affecting over a billion people worldwide. In diagnosing and treating sleep apnea, it is imperative to establish the type of sleep apnea—whether it is obstructive or central sleep apnea. The differential contribution of central vs. obstructive sleep apnea toward incidental cardiovascular disease in those with significant sleep apnea has not been well studied.
Our group has developed an automated algorithm that deduces on a breath-by-breath level whether reductions in airflow are predominantly due to obstructive or central phenomena. Our algorithm uses several features that are known to be key in distinguishing the type of events and derives a probability of obstruction across each “small” (reduced amplitude) breath. The breath-by-breath probability is then used to determine whether a patient’s burden of sleep apnea is predominantly obstructive or central.
In this work, we analyzed sleep study data from The Osteoporotic Fractures in Men (MrOS) cohort (N=2793) consisting of elderly men, across two visits separated on average by 6.5 years, and derived the probability of obstruction on a breath-by-breath level. The median probability of obstruction for each subject was computed and analyzed against outcomes of cardiovascular disease. We also assessed the stability of the metric in those without any prevalent cardiovascular disease. We find that median probability of obstruction was stable across the two visits, and those with any incident cardiovascular disease had a lower median probability of obstruction: patients with incident cardiovascular outcomes had a significant burden of sleep apnea that was predominantly “central” in nature.
Dr. Parekh[/caption]
Ankit Parekh, PhD
Director of the Sleep And Circadian Analysis (SCAN) Group
Assistant Professor of Medicine
(Pulmonary, Critical Care and Sleep Medicine)
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Sleep apnea is associated with incident cardiovascular disease, and is a common chronic condition affecting over a billion people worldwide. In diagnosing and treating sleep apnea, it is imperative to establish the type of sleep apnea—whether it is obstructive or central sleep apnea. The differential contribution of central vs. obstructive sleep apnea toward incidental cardiovascular disease in those with significant sleep apnea has not been well studied.
Our group has developed an automated algorithm that deduces on a breath-by-breath level whether reductions in airflow are predominantly due to obstructive or central phenomena. Our algorithm uses several features that are known to be key in distinguishing the type of events and derives a probability of obstruction across each “small” (reduced amplitude) breath. The breath-by-breath probability is then used to determine whether a patient’s burden of sleep apnea is predominantly obstructive or central.
In this work, we analyzed sleep study data from The Osteoporotic Fractures in Men (MrOS) cohort (N=2793) consisting of elderly men, across two visits separated on average by 6.5 years, and derived the probability of obstruction on a breath-by-breath level. The median probability of obstruction for each subject was computed and analyzed against outcomes of cardiovascular disease. We also assessed the stability of the metric in those without any prevalent cardiovascular disease. We find that median probability of obstruction was stable across the two visits, and those with any incident cardiovascular disease had a lower median probability of obstruction: patients with incident cardiovascular outcomes had a significant burden of sleep apnea that was predominantly “central” in nature.


 Dr. Traverso[/caption]
Giovanni Traverso MD PhD
Karl Van Tassel (1925) Career Development Professor
Department of Mechanical Engineering
Koch Institute of Integrative Cancer Research
Division of Gastroenterology
Brigham and Women’s Hospital
Harvard Medical School, Boston, MA, USA
MedicalResearch.com: What is the background for this study?
Response: I think its always important to acknowledge that this is a big team effort. We have the teams from MIT, Celero Systems, West Virgnia University (WVU) and Brigham and Women’s Hospital (BWH) all working together on this. For this study, Celero prototyped the devices that we tested in pre-clinical (Swine) models and in a first-in-human study with the team at WVU.
Our lab focuses on the development of ingestible devices for drug delivery and sensing and these have informed the development of these efforts as you can see.
Dr. Traverso[/caption]
Giovanni Traverso MD PhD
Karl Van Tassel (1925) Career Development Professor
Department of Mechanical Engineering
Koch Institute of Integrative Cancer Research
Division of Gastroenterology
Brigham and Women’s Hospital
Harvard Medical School, Boston, MA, USA
MedicalResearch.com: What is the background for this study?
Response: I think its always important to acknowledge that this is a big team effort. We have the teams from MIT, Celero Systems, West Virgnia University (WVU) and Brigham and Women’s Hospital (BWH) all working together on this. For this study, Celero prototyped the devices that we tested in pre-clinical (Swine) models and in a first-in-human study with the team at WVU.
Our lab focuses on the development of ingestible devices for drug delivery and sensing and these have informed the development of these efforts as you can see.


 Valentina Paz[/caption]
Valentina Paz, M.Sc
Valentina Paz[/caption]
Valentina Paz, M.Sc 
 Joanna Gorgol[/caption]
Joanna Gorgol
PhD Student
University of Warsaw
MedicalResearch.com: What is the background for this study?
Response: People differ in the time when they prefer to wake up and fall asleep: some people prefer going to bed and waking up early, while others prefer later hours. Most of the population is somewhere between them. Research indicates that being a morning person is related to reporting higher satisfaction with life and conscientiousness. Studies also show the associations between being religious and having higher life satisfaction and conscientiousness. It seems that religiosity might mediate the relationship between morningness and higher life satisfaction. To better understand these associations we conducted two questionnaire-based studies of Polish adults, one with 500 participants and the other with 728 participants. All participants completed questionnaires measuring their chronotype, satisfaction with life, personality traits, and religiosity
Joanna Gorgol[/caption]
Joanna Gorgol
PhD Student
University of Warsaw
MedicalResearch.com: What is the background for this study?
Response: People differ in the time when they prefer to wake up and fall asleep: some people prefer going to bed and waking up early, while others prefer later hours. Most of the population is somewhere between them. Research indicates that being a morning person is related to reporting higher satisfaction with life and conscientiousness. Studies also show the associations between being religious and having higher life satisfaction and conscientiousness. It seems that religiosity might mediate the relationship between morningness and higher life satisfaction. To better understand these associations we conducted two questionnaire-based studies of Polish adults, one with 500 participants and the other with 728 participants. All participants completed questionnaires measuring their chronotype, satisfaction with life, personality traits, and religiosity

 Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD
Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD