MedicalResearch.com Interview with:
[caption id="attachment_53245" align="alignleft" width="143"]

Dr. Tymianski[/caption]
Michael Tymianski, CM, MD, PhD, FRCSC, FAHA
Head, Division of Neurosurgery, University Health Network
Medical Director, Neurovascular Therapeutics Program, University Health Network
Professor, Departments of Surgery and Physiology, University of Toronto
Senior Scientist, Toronto Western Hospital Research Institute
Director, Neuroprotection Laboratory, Toronto Western Hospital
President and CEO, NoNO Inc
MedicalResearch.com: What is the background for this study? How is alteplase related to and affect nerinetide?
Response: Cerebral neuroprotection for acute ischemic stroke (AIS) is defined as a therapy aimed at enhancing the brain’s resilience to ischemia to improve the clinical outcome of affected individuals. Although traditionally aimed at the salvage of neurons, this term may be equally applicable to all the cellular constituents of the brain, including cells of cerebral blood vessels, neurons, and glia. Pharmacological neuroprotection (hereafter referred to as neuroprotection) would be achieved by drugs targeting one or more critical components of the ischemic cascade that lead to ischemic damage. The feasibility of neuroprotection has a strong basis in animal experiments, but research for several decades has failed to translate neuroprotective treatments from animals to humans. The disappointing results of all controlled clinical neuroprotection trials for AIS have cast doubts as to whether neuroprotection in humans is biologically possible and, given the complexities of human stroke syndromes, whether it is a clinically practicable therapy for patients experiencing AIS in the community.
In the case of neuroprotection trials for acute ischemic stroke, all to date have failed to demonstrate a clinical benefit of the study agent. Our review of studies since the year 2000 shows that many were not conducted in accordance with the animal studies that supported efficacy. They enrolled a heterogeneous subject population with varying (small and large) vessel occlusions and without knowledge of the degree of completed infarctions. Most had not implemented a strategy to ensure that the treatment effect size was maximized, and all in-hospital trials enrolled in treatment windows that exceeded 4 hours, at which an important proportion of enrolled subjects cannot respond to treatment because they no longer have salvageable brain.
The ESCAPE-NA1 addressed past deficiencies of AIS trials. It was based on a sound scientific foundation including extensive animal studies, and capitalized on the designs that led to success in AIS trials of endovascular thrombectomy. ESCAPE-NA1 enrolled patients proven by these past trials to have salvageable brain at the time that the treatment was given, and tested the drug in an ischemia-reperfusion scenario in which it was anticipated to be most effective. The enrollment was over 12 hours, but only including patients who had medical imaging suggestive that they still had salvageable brain.
Alteplase is an agent that activates the protease plasmin in the bloodstream. Plasmin cleaves peptides at certain spots within their structure, and it is a known biological fact that plasmin is able to cleave nerinetide. What was not known at the time of the trial was the degree to which this would reduce nerinetide plasma leves in humans, and the impact that this would have on the therapeutic effects of nerinetide. This is why we conducted a very large trial in which the participants’ enrollment was stratified according to whether or not they received alteplase. This ensured that there was good balance within each stratum, thereby enabling us to make more robust conclusions.







 Dr. Palatini[/caption]
Paolo Palatini, M.D.
Professor of Internal Medicine
University of Padova
Padova, Italy
MedicalResearch.com: What is the background for this study?
Response: Up to now doctors measured blood pressure (BP) on standing only in elderly people on pharmacological treatment with the purpose of detecting orthostatic hypotension. In young-to-middle-age people BP is currently measured only in the lying or the sitting posture.
Our starting point was that young borderline hypertensive people have an increased sympathetic activity and thus they might be hyperreactive to physical stimuli such as assuming the orthostatic posture which may be deleterious in the long run. This hypothesis was tested in the HARVEST, a study initiated in Italy in 1990, in which over 1200 young patients screened for stage 1 hypertension were enrolled.
Dr. Palatini[/caption]
Paolo Palatini, M.D.
Professor of Internal Medicine
University of Padova
Padova, Italy
MedicalResearch.com: What is the background for this study?
Response: Up to now doctors measured blood pressure (BP) on standing only in elderly people on pharmacological treatment with the purpose of detecting orthostatic hypotension. In young-to-middle-age people BP is currently measured only in the lying or the sitting posture.
Our starting point was that young borderline hypertensive people have an increased sympathetic activity and thus they might be hyperreactive to physical stimuli such as assuming the orthostatic posture which may be deleterious in the long run. This hypothesis was tested in the HARVEST, a study initiated in Italy in 1990, in which over 1200 young patients screened for stage 1 hypertension were enrolled.

 Dr. LaMonte[/caption]
Michael J. LaMonte, PhD, MPH
Research Professor (epidemiology)
Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
Women’s Health Initiative Northeast Regional Center
University at Buffalo – SUNY
Buffalo, NY 14214
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. LaMonte: The rationale for this study was based on existing study results showing
Dr. LaMonte[/caption]
Michael J. LaMonte, PhD, MPH
Research Professor (epidemiology)
Department of Epidemiology and Environmental Health
School of Public Health and Health Professions
Women’s Health Initiative Northeast Regional Center
University at Buffalo – SUNY
Buffalo, NY 14214
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. LaMonte: The rationale for this study was based on existing study results showing

 Dr. Lopez[/caption]
Maria Luisa S. Sequeira Lopez, MD, FAHA
Harrison Distinguished Professor in Pediatrics and Biology
University of Virginia
Charlottesville, VA 22908
MedicalResearch.com: What is the background for this study?
Response: The renin-angiotensin system (RAS) is crucial in the regulation of the blood pressure (BP). Synthesis and secretion of renin is the key regulated event in the operation of the RAS.
One of the main mechanisms that control renin synthesis and release is the baroreceptor mechanism whereby a decrease in blood pressure results in increased release of renin by juxtaglomerular (JG) cells.
In spite of its enormous importance, the nature and location of the renal baroreceptor was still unknown. This was due in great part to the lack of appropriate in vitro and in vivo models to confidently allow tracking of the fate and isolation of renin cells, and the lack of tools to study the chromatin in scarce cells.
Dr. Lopez[/caption]
Maria Luisa S. Sequeira Lopez, MD, FAHA
Harrison Distinguished Professor in Pediatrics and Biology
University of Virginia
Charlottesville, VA 22908
MedicalResearch.com: What is the background for this study?
Response: The renin-angiotensin system (RAS) is crucial in the regulation of the blood pressure (BP). Synthesis and secretion of renin is the key regulated event in the operation of the RAS.
One of the main mechanisms that control renin synthesis and release is the baroreceptor mechanism whereby a decrease in blood pressure results in increased release of renin by juxtaglomerular (JG) cells.
In spite of its enormous importance, the nature and location of the renal baroreceptor was still unknown. This was due in great part to the lack of appropriate in vitro and in vivo models to confidently allow tracking of the fate and isolation of renin cells, and the lack of tools to study the chromatin in scarce cells.

 Dr. Nation[/caption]
Daniel A. Nation, Ph.D.,
Associate Professor of Psychological Science
Institute for Memory Impairments and Neurological Disorders
University of California, Irvin
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a risk factor for cognitive decline and dementia, and treatment of hypertension has been linked to decreased risk for cognitive impairment.
Prior studies have attempted to identify which specific type of antihypertensive treatment conveys the most benefit for cognition, but findings have been mixed regarding this question. We hypothesized that antihypertensive drugs acting on the brain angiotensin system may convey the greatest benefit since they affect the brain angiotensin system that has been implicated in memory function.
Dr. Nation[/caption]
Daniel A. Nation, Ph.D.,
Associate Professor of Psychological Science
Institute for Memory Impairments and Neurological Disorders
University of California, Irvin
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a risk factor for cognitive decline and dementia, and treatment of hypertension has been linked to decreased risk for cognitive impairment.
Prior studies have attempted to identify which specific type of antihypertensive treatment conveys the most benefit for cognition, but findings have been mixed regarding this question. We hypothesized that antihypertensive drugs acting on the brain angiotensin system may convey the greatest benefit since they affect the brain angiotensin system that has been implicated in memory function.

 Prof. D'Aiuto[/caption]
Francesco D’Aiuto
Professor/Hon Consultant
Head of Periodontology Unit
UCL Eastman Dental Institute
MedicalResearch.com: What is the background for this study?
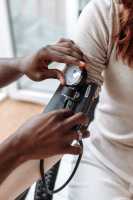
Response: This study was set out to further our understanding of the link between gum disease and high blood pressure. Recent evidence suggested that individuals with gum disease had a 20-70% increased risk of hypertension and systemic inflammation seemed to be a driver in mediating this association. Further research on the matter was needed. We recruited two relatively large groups of otherwise healthy participants (without a confirmed diagnosis of hypertension) who had gum disease one and healthy gums the other.
We found that diagnosis of periodontitis (gum disease) was consistently linked to higher systolic blood pressure independent of other cardiovascular risk factors.
Prof. D'Aiuto[/caption]
Francesco D’Aiuto
Professor/Hon Consultant
Head of Periodontology Unit
UCL Eastman Dental Institute
MedicalResearch.com: What is the background for this study?
Response: This study was set out to further our understanding of the link between gum disease and high blood pressure. Recent evidence suggested that individuals with gum disease had a 20-70% increased risk of hypertension and systemic inflammation seemed to be a driver in mediating this association. Further research on the matter was needed. We recruited two relatively large groups of otherwise healthy participants (without a confirmed diagnosis of hypertension) who had gum disease one and healthy gums the other.
We found that diagnosis of periodontitis (gum disease) was consistently linked to higher systolic blood pressure independent of other cardiovascular risk factors.
 Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
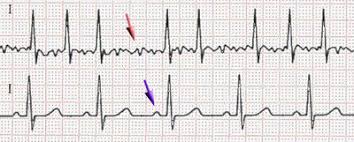
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.