Author Interviews, Melanoma, NYU/NYMC / 20.02.2026
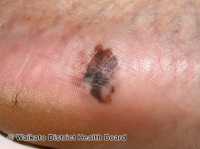
Melanoma: NYU Study Outlines Mechanisms Tumors Use to Sustain Blood Supply and Escape Immune Detection
[caption id="attachment_72519" align="alignleft" width="200"] Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.
Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.
 Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.
Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.





 Dr. Alexis[/caption]
Andrew F. Alexis, MD, MPH
Vice-Chair for Diversity and Inclusion
Department of Dermatology
Dermatologist
Center for Diverse Skin Complexions
Weill Cornell Medicine – NY
MedicalResearch.com: What are the main types of skin cancer? Is the incidence changing?
Response: The 3 main types of skin cancer are melanoma, squamous cell carcinoma (SCC) and basal cell carcinoma (BCC). Skin cancer is the most common cancer in the United States1 and 1 in 5 Americans will develop skin cancer in their lifetime. (2)
The overall incidence has changed as follows:
• Melanoma: Rates doubled over past 30 years from 1982 to 2011.3 It differs by age group.
o Adolescents and adults age 30 and younger: incidence rate is declining
o Older age groups (e.g. 80 and older): incidence rate is increasing
• Squamous Cell Cancer:
o Incidence increased 263% between 1976-1984 and 2000-20104
• Basal Cell Cancer:
o Incidence increased 145% between 1976-1984 and 2000-20104
Dr. Alexis[/caption]
Andrew F. Alexis, MD, MPH
Vice-Chair for Diversity and Inclusion
Department of Dermatology
Dermatologist
Center for Diverse Skin Complexions
Weill Cornell Medicine – NY
MedicalResearch.com: What are the main types of skin cancer? Is the incidence changing?
Response: The 3 main types of skin cancer are melanoma, squamous cell carcinoma (SCC) and basal cell carcinoma (BCC). Skin cancer is the most common cancer in the United States1 and 1 in 5 Americans will develop skin cancer in their lifetime. (2)
The overall incidence has changed as follows:
• Melanoma: Rates doubled over past 30 years from 1982 to 2011.3 It differs by age group.
o Adolescents and adults age 30 and younger: incidence rate is declining
o Older age groups (e.g. 80 and older): incidence rate is increasing
• Squamous Cell Cancer:
o Incidence increased 263% between 1976-1984 and 2000-20104
• Basal Cell Cancer:
o Incidence increased 145% between 1976-1984 and 2000-20104
 Dr. Stark[/caption]
Dr Mitchell Stark
Dr. Stark[/caption]
Dr Mitchell Stark
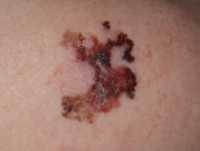
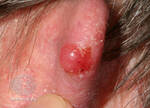 One example of a nodular melanoma without pigment.
One example of a nodular melanoma without pigment. 
 Dr. Ruiz[/caption]
John M. Ruiz, Ph.D
Associate Professor of Clinical Psychology
Department of Psychology
University of Arizona
Dr. Ruiz is the incoming editor-in-chief of the American Psychological Association (APA) journal, Health Psychology
Dr. Ruiz joined the U.S. Preventive Services Task Force in January 2022
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Skin cancer is the most common type of cancer in the United States, but it often does not cause serious complications or death. The Task Force’s recommendation on screening for skin cancer focuses on the effectiveness of visual skin exams for children and adults who do not have any symptoms. When reviewing the latest research, we found that there is currently not enough evidence to tell us whether or not screening people without signs or symptoms is beneficial. This is an I statement.
Dr. Ruiz[/caption]
John M. Ruiz, Ph.D
Associate Professor of Clinical Psychology
Department of Psychology
University of Arizona
Dr. Ruiz is the incoming editor-in-chief of the American Psychological Association (APA) journal, Health Psychology
Dr. Ruiz joined the U.S. Preventive Services Task Force in January 2022
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Skin cancer is the most common type of cancer in the United States, but it often does not cause serious complications or death. The Task Force’s recommendation on screening for skin cancer focuses on the effectiveness of visual skin exams for children and adults who do not have any symptoms. When reviewing the latest research, we found that there is currently not enough evidence to tell us whether or not screening people without signs or symptoms is beneficial. This is an I statement.
 Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
 Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.
Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.


 MedicalResearch.com Interview with:
Eleonora Leucci, Ph.D Assistant Professor
Laboratory for RNA Cancer Biology
Department of Oncology
KU Leuven
MedicalResearch.com: What is the background for this study?
Response: Back in 2016, while I was characterising the RNA SAMMSON as essential for mitochondrial translation in melanoma, I noticed that its inhibition was causing cell death across a large spectrum of melanoma cell lines and models, irrespectively of their genetic background and cell state. At that time I still did not know why the effect was so pronounced on melanoma cells, but I knew that antibiotics of the tetracycline family could also block mitochondrial translation and I thought about repurposing them to treat melanoma.
MedicalResearch.com Interview with:
Eleonora Leucci, Ph.D Assistant Professor
Laboratory for RNA Cancer Biology
Department of Oncology
KU Leuven
MedicalResearch.com: What is the background for this study?
Response: Back in 2016, while I was characterising the RNA SAMMSON as essential for mitochondrial translation in melanoma, I noticed that its inhibition was causing cell death across a large spectrum of melanoma cell lines and models, irrespectively of their genetic background and cell state. At that time I still did not know why the effect was so pronounced on melanoma cells, but I knew that antibiotics of the tetracycline family could also block mitochondrial translation and I thought about repurposing them to treat melanoma.
 Professor Marie-Aleth Richard
EADV Communications Committee Chair
Professor, University Hospital of La Timone
Marseille, France
MedicalResearch.com: What is the background for this Roundtable event? Would you describe the mission of the European Commission’s Beating Cancer Plan?
Response: Europe’s Beating Cancer Plan is the first, comprehensive EU strategy on cancer, aimed at tackling the disease through all key stages: prevention; early detection; diagnosis and treatment; and quality of life of cancer patients and survivors. The Plan also aims to create opportunities to improve cancer care through research and innovative projects, such as artificial intelligence, and to promote equal access to knowledge and treatments in cancer care across Europe.
The EADV seeks to create a bridge between the EU health policy agenda and scientific research, by engaging with policymakers, patient organisations and other stakeholders to support a patient centric-approach; tackling melanoma and non-melanoma skin cancers (NMSC) at all stages of the pathway, from prevention to follow-up care.
Through our Roundtable event, the EADV brought together these key stakeholders to evaluate the effectiveness of the EBCP on preventing both melanoma and NMSC, as well as identify joint recommendations that step-up measures towards this goal.
Professor Marie-Aleth Richard
EADV Communications Committee Chair
Professor, University Hospital of La Timone
Marseille, France
MedicalResearch.com: What is the background for this Roundtable event? Would you describe the mission of the European Commission’s Beating Cancer Plan?
Response: Europe’s Beating Cancer Plan is the first, comprehensive EU strategy on cancer, aimed at tackling the disease through all key stages: prevention; early detection; diagnosis and treatment; and quality of life of cancer patients and survivors. The Plan also aims to create opportunities to improve cancer care through research and innovative projects, such as artificial intelligence, and to promote equal access to knowledge and treatments in cancer care across Europe.
The EADV seeks to create a bridge between the EU health policy agenda and scientific research, by engaging with policymakers, patient organisations and other stakeholders to support a patient centric-approach; tackling melanoma and non-melanoma skin cancers (NMSC) at all stages of the pathway, from prevention to follow-up care.
Through our Roundtable event, the EADV brought together these key stakeholders to evaluate the effectiveness of the EBCP on preventing both melanoma and NMSC, as well as identify joint recommendations that step-up measures towards this goal.

 Anne Cust[/caption]
Anne Cust | PhD, Professor of Cancer Epidemiology
The University of Sydney
Faculty of Medicine and Health
Sydney School of Public Health
MedicalResearch.com: What is the background for this study? Are the screeners specially trained, use full body photographs, dermoscopy etc?
Response: The Melanoma High-risk Clinic Study was developed to optimise the early detection of new melanomas in people at high risk of developing melanoma. A previous single-centre study observed fewer excisions and healthcare costs, thinner melanomas and better quality of life when surveillance of high risk patients was conducted in a melanoma dermatology clinic with a structured surveillance protocol involving 6-monthly full body examinations aided by total body photography (TBP) and sequential digital dermoscopy imaging (SDDI). The initial pilot study was performed in a single tertiary referral specialist centre using trained dermatologists who routinely used the diagnostic interventions.
Our objective was to examine longer-term sustainability and expansion of the program to multiple practices including a primary care skin cancer clinic setting. The hypothesis was that the outcomes would be similar if using the same protocol and diagnostic tools. The participating doctors were trained to follow the protocol, which included instruction on how to respond and interpret changing lesions, but not in use of dermoscopy or skin examinations, which were routinely and consistently used in all clinics prior to the study commencing. There were 593 participants assessed as very high risk of melanoma who participated in the Melanoma High-risk Clinic Study from 2012-2018. Nearly all of the participants had had a previous melanoma and had additional melanoma risk factors. 57% were male and the median age at study entry was 58 years.
Anne Cust[/caption]
Anne Cust | PhD, Professor of Cancer Epidemiology
The University of Sydney
Faculty of Medicine and Health
Sydney School of Public Health
MedicalResearch.com: What is the background for this study? Are the screeners specially trained, use full body photographs, dermoscopy etc?
Response: The Melanoma High-risk Clinic Study was developed to optimise the early detection of new melanomas in people at high risk of developing melanoma. A previous single-centre study observed fewer excisions and healthcare costs, thinner melanomas and better quality of life when surveillance of high risk patients was conducted in a melanoma dermatology clinic with a structured surveillance protocol involving 6-monthly full body examinations aided by total body photography (TBP) and sequential digital dermoscopy imaging (SDDI). The initial pilot study was performed in a single tertiary referral specialist centre using trained dermatologists who routinely used the diagnostic interventions.
Our objective was to examine longer-term sustainability and expansion of the program to multiple practices including a primary care skin cancer clinic setting. The hypothesis was that the outcomes would be similar if using the same protocol and diagnostic tools. The participating doctors were trained to follow the protocol, which included instruction on how to respond and interpret changing lesions, but not in use of dermoscopy or skin examinations, which were routinely and consistently used in all clinics prior to the study commencing. There were 593 participants assessed as very high risk of melanoma who participated in the Melanoma High-risk Clinic Study from 2012-2018. Nearly all of the participants had had a previous melanoma and had additional melanoma risk factors. 57% were male and the median age at study entry was 58 years.








 Dr. Brooks[/caption]
Dr. Kelly Brooks PhD
Research Officer
QIMR Berghofer Medical Research Institute
MedicalResearch.com: What is the background for this study?
[caption id="attachment_54258" align="alignleft" width="200"]
Dr. Brooks[/caption]
Dr. Kelly Brooks PhD
Research Officer
QIMR Berghofer Medical Research Institute
MedicalResearch.com: What is the background for this study?
[caption id="attachment_54258" align="alignleft" width="200"]