Author Interviews, Melanoma, Psychological Science / 05.03.2020
Stress and Delayed Detection Contribute to Increased Melanoma Mortality with Loss of Partner
MedicalResearch.com Interview with:
[caption id="attachment_53405" align="alignleft" width="160"] Dr. Langan[/caption]
Dr. Sinead Langan. FRCP MSc PhD
Professor of Clinical Epidemiology
Wellcome Senior Clinical Fellow
Faculty of Epidemiology and Population Health,
London School of Hygiene and Tropical Medicine
London, U.K.
MedicalResearch.com: What is the background for this study?
Response: Psychological stress is commonly cited as a risk factor for melanoma, but clinical evidence is limited. We wanted to test the hypothesis that acute severe stress increases the risk of melanoma and melanoma progression.
Dr. Langan[/caption]
Dr. Sinead Langan. FRCP MSc PhD
Professor of Clinical Epidemiology
Wellcome Senior Clinical Fellow
Faculty of Epidemiology and Population Health,
London School of Hygiene and Tropical Medicine
London, U.K.
MedicalResearch.com: What is the background for this study?
Response: Psychological stress is commonly cited as a risk factor for melanoma, but clinical evidence is limited. We wanted to test the hypothesis that acute severe stress increases the risk of melanoma and melanoma progression.
 Dr. Langan[/caption]
Dr. Sinead Langan. FRCP MSc PhD
Professor of Clinical Epidemiology
Wellcome Senior Clinical Fellow
Faculty of Epidemiology and Population Health,
London School of Hygiene and Tropical Medicine
London, U.K.
MedicalResearch.com: What is the background for this study?
Response: Psychological stress is commonly cited as a risk factor for melanoma, but clinical evidence is limited. We wanted to test the hypothesis that acute severe stress increases the risk of melanoma and melanoma progression.
Dr. Langan[/caption]
Dr. Sinead Langan. FRCP MSc PhD
Professor of Clinical Epidemiology
Wellcome Senior Clinical Fellow
Faculty of Epidemiology and Population Health,
London School of Hygiene and Tropical Medicine
London, U.K.
MedicalResearch.com: What is the background for this study?
Response: Psychological stress is commonly cited as a risk factor for melanoma, but clinical evidence is limited. We wanted to test the hypothesis that acute severe stress increases the risk of melanoma and melanoma progression.






 Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
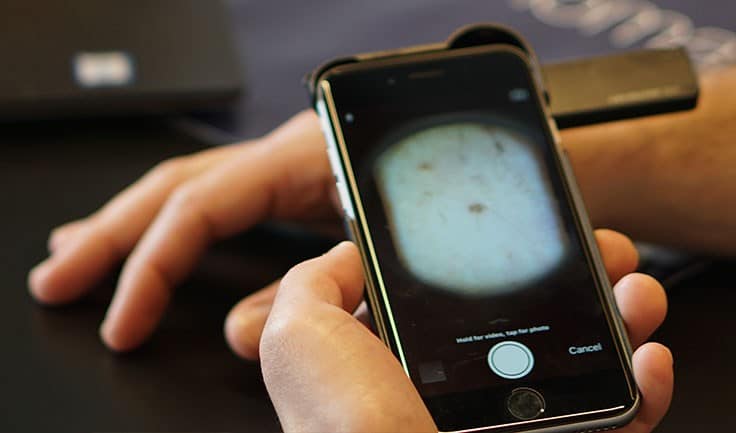
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.
Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.
 Dr. Qing Chen[/caption]
Qing Chen, M.D., Ph.D.
Assistant Professor, Immunology, Microenvironment & Metastasis Program
Scientific Director, Imaging Facility
The Wistar Institute
MedicalResearch.com: What is the background for this study?
Response: We are focusing on how a specific type of brain cells, astrocytes, helps the cancer cells from melanoma and breast cancer to form metastatic lesions.
Dr. Qing Chen[/caption]
Qing Chen, M.D., Ph.D.
Assistant Professor, Immunology, Microenvironment & Metastasis Program
Scientific Director, Imaging Facility
The Wistar Institute
MedicalResearch.com: What is the background for this study?
Response: We are focusing on how a specific type of brain cells, astrocytes, helps the cancer cells from melanoma and breast cancer to form metastatic lesions.




 Prof. Satchi-Fainaro[/caption]
Prof. Ronit Satchi-Fainaro, PhD
Head, Cancer Research and Nanomedicine Laboratory
Department of Physiology and Pharmacology,
Sackler Faculty of Medicine,
Tel Aviv University,
Tel-Aviv 69978, Israel
[caption id="attachment_50670" align="alignleft" width="116"]
Prof. Satchi-Fainaro[/caption]
Prof. Ronit Satchi-Fainaro, PhD
Head, Cancer Research and Nanomedicine Laboratory
Department of Physiology and Pharmacology,
Sackler Faculty of Medicine,
Tel Aviv University,
Tel-Aviv 69978, Israel
[caption id="attachment_50670" align="alignleft" width="116"] Prof. Florindo[/caption]
Prof. Helena Florindo, PhD
Head, BioNanoSciences – iMed.ULisboa
Faculty of Pharmacy,
University of Lisbon
Lisbon, Portugal
MedicalResearch.com: What are the main findings?
Response: The war against cancer in general, and melanoma in particular, has advanced over the years through a variety of treatment modalities, such as surgery, chemotherapy, radiation therapy and immunotherapy. The immune checkpoint inhibitors brought a breakthrough solution for advanced melanoma patients, but only a low percentage of those respond to this therapy, developing resistance and being affected by severe side effects. Despite the success of several vaccines against viral diseases, this success has not been materialized yet against cancer.
This study led by my lab at Tel Aviv University, and Helena Florindo’s lab at the University of Lisbon, describes the development of an effective nano-vaccine against melanoma, that also sensitizes the immune system to immunotherapies.
This nano-vaccine prevented melanoma, and also led to remarkable tumor inhibition and prolonged survival in mice already affected by this disease.
Prof. Florindo[/caption]
Prof. Helena Florindo, PhD
Head, BioNanoSciences – iMed.ULisboa
Faculty of Pharmacy,
University of Lisbon
Lisbon, Portugal
MedicalResearch.com: What are the main findings?
Response: The war against cancer in general, and melanoma in particular, has advanced over the years through a variety of treatment modalities, such as surgery, chemotherapy, radiation therapy and immunotherapy. The immune checkpoint inhibitors brought a breakthrough solution for advanced melanoma patients, but only a low percentage of those respond to this therapy, developing resistance and being affected by severe side effects. Despite the success of several vaccines against viral diseases, this success has not been materialized yet against cancer.
This study led by my lab at Tel Aviv University, and Helena Florindo’s lab at the University of Lisbon, describes the development of an effective nano-vaccine against melanoma, that also sensitizes the immune system to immunotherapies.
This nano-vaccine prevented melanoma, and also led to remarkable tumor inhibition and prolonged survival in mice already affected by this disease. 


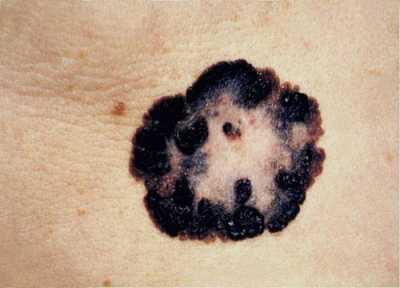
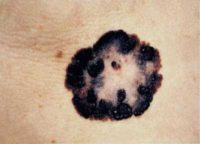
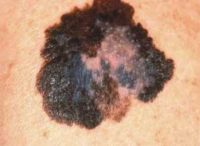
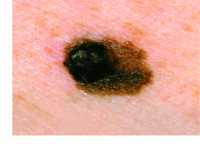
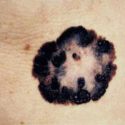 Example of one type of melanoma[/caption]
Dr. Catherine M. Olsen
Associate Professor
Cancer Control Group
QIMR Berghofer Medical Research Institute
MedicalResearch.com: What is the background for this study?
Response: Melanoma incidence and mortality rates are increasing globally. Public health campaigns aiming to reduce sun exposure and use of sunbed have been implemented in many parts of the world, but there is significant variability in terms of the history and reach of these campaigns across countries. We examined melanoma incidence rates in eight different countries with different patterns of sun exposure and varying approaches to melanoma control.
Example of one type of melanoma[/caption]
Dr. Catherine M. Olsen
Associate Professor
Cancer Control Group
QIMR Berghofer Medical Research Institute
MedicalResearch.com: What is the background for this study?
Response: Melanoma incidence and mortality rates are increasing globally. Public health campaigns aiming to reduce sun exposure and use of sunbed have been implemented in many parts of the world, but there is significant variability in terms of the history and reach of these campaigns across countries. We examined melanoma incidence rates in eight different countries with different patterns of sun exposure and varying approaches to melanoma control.