Author Interviews, Infections, Pediatrics, Vaccine Studies / 12.02.2026
IDSA Spokesperson Discusses Recent Outbreaks of Measles Infections
MedicalResearch.com Interview with:
[caption id="attachment_72376" align="alignleft" width="190"] Dr. Schaffner[/caption]
William Schaffner, MD
Professor of Preventive Medicine, Department of Health Policy
Professor of Medicine, Division of Infectious Diseases
Vanderbilt University Medical Center
Nashville, TN 37203
Dr. Schaffner discusses the recent increase in the incidence of measles infections.
MedicalResearch.com: What is the background for this study?
Response: The fundamental reason leading to the increase in measles cases in the US is that some parents are withholding their children from routine measles vaccination: Failure to vaccinate. As a result, there are neighborhoods, schools, and communities that now have vaccination rates substantially below the 92% to 95% needed to prevent outbreaks of infection. Measles is the most contagious virus we know, so it takes very high vaccination rates to prevent transmission and to avert outbreaks.
Vaccine hesitancy has many causes: Lack of knowledge of the severity of measles, concern over vaccine side-effects, low trust in public health, a desire to do things more “naturally” and it can also have political overtones, among others.
The measles vaccine is extraordinarily effective; the routine two-dose series confers 97% to 98% protection for life. The rare “breakthrough” infections that occur in vaccinated persons are generally milder, with fewer complications than in persons who are unvaccinated.
The US was certified as having eliminated measles in 2000 because of high vaccination rates across the country. Sadly, the US is likely to lose that designation because of sustained measles transmission, reverting us back to the bad old days. It is particularly sad for any of our children to have to endure measles and its consequences. All these cases could have been prevented by vaccination.
Dr. Schaffner[/caption]
William Schaffner, MD
Professor of Preventive Medicine, Department of Health Policy
Professor of Medicine, Division of Infectious Diseases
Vanderbilt University Medical Center
Nashville, TN 37203
Dr. Schaffner discusses the recent increase in the incidence of measles infections.
MedicalResearch.com: What is the background for this study?
Response: The fundamental reason leading to the increase in measles cases in the US is that some parents are withholding their children from routine measles vaccination: Failure to vaccinate. As a result, there are neighborhoods, schools, and communities that now have vaccination rates substantially below the 92% to 95% needed to prevent outbreaks of infection. Measles is the most contagious virus we know, so it takes very high vaccination rates to prevent transmission and to avert outbreaks.
Vaccine hesitancy has many causes: Lack of knowledge of the severity of measles, concern over vaccine side-effects, low trust in public health, a desire to do things more “naturally” and it can also have political overtones, among others.
The measles vaccine is extraordinarily effective; the routine two-dose series confers 97% to 98% protection for life. The rare “breakthrough” infections that occur in vaccinated persons are generally milder, with fewer complications than in persons who are unvaccinated.
The US was certified as having eliminated measles in 2000 because of high vaccination rates across the country. Sadly, the US is likely to lose that designation because of sustained measles transmission, reverting us back to the bad old days. It is particularly sad for any of our children to have to endure measles and its consequences. All these cases could have been prevented by vaccination.
 MedicalResearch.com: What roles do a decrease in US immunization rates and/or increased immigration from under-vaccinated area play in this increase?
Response: The substantial majority of unimmunized children in the US were born and raised in this country. They usually are members of middle- or upper-income families. The most frequent importers of measles into the US are our own unimmunized children who travel abroad, encounter measles virus and bring it back to their homes where the virus then spreads among the child’s schoolmates and playmates, creating an outbreak.
MedicalResearch.com: What roles do a decrease in US immunization rates and/or increased immigration from under-vaccinated area play in this increase?
Response: The substantial majority of unimmunized children in the US were born and raised in this country. They usually are members of middle- or upper-income families. The most frequent importers of measles into the US are our own unimmunized children who travel abroad, encounter measles virus and bring it back to their homes where the virus then spreads among the child’s schoolmates and playmates, creating an outbreak.
 Dr. Schaffner[/caption]
William Schaffner, MD
Professor of Preventive Medicine, Department of Health Policy
Professor of Medicine, Division of Infectious Diseases
Vanderbilt University Medical Center
Nashville, TN 37203
Dr. Schaffner discusses the recent increase in the incidence of measles infections.
MedicalResearch.com: What is the background for this study?
Response: The fundamental reason leading to the increase in measles cases in the US is that some parents are withholding their children from routine measles vaccination: Failure to vaccinate. As a result, there are neighborhoods, schools, and communities that now have vaccination rates substantially below the 92% to 95% needed to prevent outbreaks of infection. Measles is the most contagious virus we know, so it takes very high vaccination rates to prevent transmission and to avert outbreaks.
Vaccine hesitancy has many causes: Lack of knowledge of the severity of measles, concern over vaccine side-effects, low trust in public health, a desire to do things more “naturally” and it can also have political overtones, among others.
The measles vaccine is extraordinarily effective; the routine two-dose series confers 97% to 98% protection for life. The rare “breakthrough” infections that occur in vaccinated persons are generally milder, with fewer complications than in persons who are unvaccinated.
The US was certified as having eliminated measles in 2000 because of high vaccination rates across the country. Sadly, the US is likely to lose that designation because of sustained measles transmission, reverting us back to the bad old days. It is particularly sad for any of our children to have to endure measles and its consequences. All these cases could have been prevented by vaccination.
Dr. Schaffner[/caption]
William Schaffner, MD
Professor of Preventive Medicine, Department of Health Policy
Professor of Medicine, Division of Infectious Diseases
Vanderbilt University Medical Center
Nashville, TN 37203
Dr. Schaffner discusses the recent increase in the incidence of measles infections.
MedicalResearch.com: What is the background for this study?
Response: The fundamental reason leading to the increase in measles cases in the US is that some parents are withholding their children from routine measles vaccination: Failure to vaccinate. As a result, there are neighborhoods, schools, and communities that now have vaccination rates substantially below the 92% to 95% needed to prevent outbreaks of infection. Measles is the most contagious virus we know, so it takes very high vaccination rates to prevent transmission and to avert outbreaks.
Vaccine hesitancy has many causes: Lack of knowledge of the severity of measles, concern over vaccine side-effects, low trust in public health, a desire to do things more “naturally” and it can also have political overtones, among others.
The measles vaccine is extraordinarily effective; the routine two-dose series confers 97% to 98% protection for life. The rare “breakthrough” infections that occur in vaccinated persons are generally milder, with fewer complications than in persons who are unvaccinated.
The US was certified as having eliminated measles in 2000 because of high vaccination rates across the country. Sadly, the US is likely to lose that designation because of sustained measles transmission, reverting us back to the bad old days. It is particularly sad for any of our children to have to endure measles and its consequences. All these cases could have been prevented by vaccination.
 MedicalResearch.com: What roles do a decrease in US immunization rates and/or increased immigration from under-vaccinated area play in this increase?
Response: The substantial majority of unimmunized children in the US were born and raised in this country. They usually are members of middle- or upper-income families. The most frequent importers of measles into the US are our own unimmunized children who travel abroad, encounter measles virus and bring it back to their homes where the virus then spreads among the child’s schoolmates and playmates, creating an outbreak.
MedicalResearch.com: What roles do a decrease in US immunization rates and/or increased immigration from under-vaccinated area play in this increase?
Response: The substantial majority of unimmunized children in the US were born and raised in this country. They usually are members of middle- or upper-income families. The most frequent importers of measles into the US are our own unimmunized children who travel abroad, encounter measles virus and bring it back to their homes where the virus then spreads among the child’s schoolmates and playmates, creating an outbreak.


 Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"]
Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"]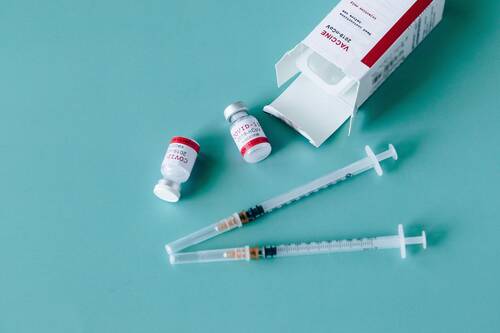






 Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.
Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.

 Dr. García Cenoz[/caption]
Manuel García Cenoz MD, PhD
Dr. García Cenoz[/caption]
Manuel García Cenoz MD, PhD

 Dr. Wall[/caption]
Dr Emma Wall
Senior Clinical Research Fellow, UCLH-Crick Legacy study
Consultant Infectious Diseases UCLH
MedicalResearch.com: What is the background for this study?
Response: Since April 2022, both the UK and US have changed their COVID-19 isolation and testing policies. The impact these changes in the guidance and vaccination on community-acquired COVID-19 caused by recent SARS-CoV-2 variants of concern (VOC) has not been fully tested, including infections with BA.2. We aimed to characterise both symptoms and viral loads over the course of COVID-19 infection in otherwise-healthy, vaccinated, non-hospitalised adults, to assess whether current guidance remains justified. All participants were included in the UCLH-Crick Legacy study, a prospective, observational cohort study of otherwise healthy adults who have been taking part in regular workplace testing for SARS-CoV-2 in London
We sent swabs by same-day courier every other day to all adults who reported a positive PCR or lateral flow test to the study team up to day 10 after the start of each infection. We confirmed which variant caused the infection by PCR and sequencing. All participants completed linked symptom diaries.
We compared symptoms and changes in the amount of virus detected in the nose and throat during infection between study participants reporting COVID-19 caused by VOCs Delta and Omicron BA.1 and BA.2. We then analysed how many of our participants would meet current UK/US isolation guidelines.
Dr. Wall[/caption]
Dr Emma Wall
Senior Clinical Research Fellow, UCLH-Crick Legacy study
Consultant Infectious Diseases UCLH
MedicalResearch.com: What is the background for this study?
Response: Since April 2022, both the UK and US have changed their COVID-19 isolation and testing policies. The impact these changes in the guidance and vaccination on community-acquired COVID-19 caused by recent SARS-CoV-2 variants of concern (VOC) has not been fully tested, including infections with BA.2. We aimed to characterise both symptoms and viral loads over the course of COVID-19 infection in otherwise-healthy, vaccinated, non-hospitalised adults, to assess whether current guidance remains justified. All participants were included in the UCLH-Crick Legacy study, a prospective, observational cohort study of otherwise healthy adults who have been taking part in regular workplace testing for SARS-CoV-2 in London
We sent swabs by same-day courier every other day to all adults who reported a positive PCR or lateral flow test to the study team up to day 10 after the start of each infection. We confirmed which variant caused the infection by PCR and sequencing. All participants completed linked symptom diaries.
We compared symptoms and changes in the amount of virus detected in the nose and throat during infection between study participants reporting COVID-19 caused by VOCs Delta and Omicron BA.1 and BA.2. We then analysed how many of our participants would meet current UK/US isolation guidelines.

 Dr. Otter[/caption]
Ashley Otter, PhD
Research scientist within Diagnostic Support
for the rare/imported pathogens laboratory (RIPL)
Public Health England (PHE)
MedicalResearch.com: What is the background for this study?
Response: The SIREN study is a national research project covering all four nations of the United Kingdom. Almost 45,000 healthcare workers from across the UK were enrolled midway through 2020, each providing monthly samples for antibody testing and fortnightly PCR testing. Using samples from participants from this project, we were able to take a snapshot of ~6,000 participants at different stages after they received their vaccination to see how different factors affect their antibody responses.
Dr. Otter[/caption]
Ashley Otter, PhD
Research scientist within Diagnostic Support
for the rare/imported pathogens laboratory (RIPL)
Public Health England (PHE)
MedicalResearch.com: What is the background for this study?
Response: The SIREN study is a national research project covering all four nations of the United Kingdom. Almost 45,000 healthcare workers from across the UK were enrolled midway through 2020, each providing monthly samples for antibody testing and fortnightly PCR testing. Using samples from participants from this project, we were able to take a snapshot of ~6,000 participants at different stages after they received their vaccination to see how different factors affect their antibody responses.

 Shuchi Anand, MD MS (she/her)
Assistant Professor in Medicine
Director, Center for Tubulointerstitial Kidney Disease
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A majority of people on dialysis who completed vaccination as of September 2021 have had a decline in antibody response to levels that would render them vulnerable to infection. Antibody response immediately after vaccination and circulating antibody response is strongly associated with risk for breakthrough after the initial vaccination series.
Shuchi Anand, MD MS (she/her)
Assistant Professor in Medicine
Director, Center for Tubulointerstitial Kidney Disease
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A majority of people on dialysis who completed vaccination as of September 2021 have had a decline in antibody response to levels that would render them vulnerable to infection. Antibody response immediately after vaccination and circulating antibody response is strongly associated with risk for breakthrough after the initial vaccination series.

 Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.
Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.
 Dr. Elwy[/caption]
Rani Elwy, PhD
Bridge Quality Enhancement Research Initiative Program, Center for Healthcare Organization and Implementation Research,
VA Bedford Healthcare System
Bedford, Massachusetts
Department of Psychiatry and Human Behavior, Alpert Medical School
Brown University, Providence, Rhode Island
MedicalResearch.com: What is the background for this study?
Response: The VA operates a very robust, embedded quality improvement and implementation science program, of which our team is involved. As the VA was one of the first US healthcare systems to rollout COVID-19 vaccination programs, we were asked to evaluate these efforts in real-time, to provide input to VA healthcare leaders on what was going well and what could be improved. This survey reported in JAMA Network Open is one of the quality improvement efforts we engaged in.
Dr. Elwy[/caption]
Rani Elwy, PhD
Bridge Quality Enhancement Research Initiative Program, Center for Healthcare Organization and Implementation Research,
VA Bedford Healthcare System
Bedford, Massachusetts
Department of Psychiatry and Human Behavior, Alpert Medical School
Brown University, Providence, Rhode Island
MedicalResearch.com: What is the background for this study?
Response: The VA operates a very robust, embedded quality improvement and implementation science program, of which our team is involved. As the VA was one of the first US healthcare systems to rollout COVID-19 vaccination programs, we were asked to evaluate these efforts in real-time, to provide input to VA healthcare leaders on what was going well and what could be improved. This survey reported in JAMA Network Open is one of the quality improvement efforts we engaged in.

 Dr. Frost[/caption]
Holly Frost, MD
Assistant Professor Pediatrics
University of Colorado Anschutz School of Medicine
[caption id="attachment_58185" align="alignleft" width="150"]
Dr. Frost[/caption]
Holly Frost, MD
Assistant Professor Pediatrics
University of Colorado Anschutz School of Medicine
[caption id="attachment_58185" align="alignleft" width="150"]
