Author Interviews, Cancer Research, FDA, Vaccine Studies / 14.08.2019
FDA Identifies No New Safety Concerns Associated with Prostate Cancer Treatment Vaccine Sipuleucel-T
MedicalResearch.com Interview with:
[caption id="attachment_50871" align="alignleft" width="150"] Dr. Graca Dores (left) and Dr. Perez-Vilar (senior author)[/caption]
Dr. Graca Dores MD MPH
US Food and Drug Administration
Center for Biologics Evaluation and Research
Office of Biostatistics and Epidemiology
Division of Epidemiology
Silver Spring, Maryland
Oklahoma City, OK
MedicalResearch.com: What is the background for this study? Would you briefly explain what Sipuleucel-T is used for?
Response: Sipuleucel-T was the first therapeutic vaccine approved by the U.S. Food and Drug Administration (FDA) in 2010. It is indicated for the treatment of asymptomatic or minimally symptomatic, metastatic, castration-resistant prostate cancer (CRPC; prostate cancer that spreads while an individual is on hormone-blocking therapy). During the preparation of this product, the patient’s cells are collected (leukapheresis), sent for processing to generate a dose of patient-specific vaccine, and then administered intravenously back to the patient. This process is repeated approximately every two weeks for a total of three doses.
Except for the pre-marketing clinical trials that were reviewed during the sipuleucel-T approval process, post-marketing studies that have evaluated the safety profile of sipuleucel-T are scarce. Therefore, we used the FDA’s Adverse Event Reporting System (FAERS) database to summarize the adverse events reported to FDA by industry, medical professionals, and consumers. We also assessed whether sipuleucel-T and specific adverse events (product-event pairs) were reported more than expected compared to all other drug/biologic-adverse event pairs in the FAERS database.
Dr. Graca Dores (left) and Dr. Perez-Vilar (senior author)[/caption]
Dr. Graca Dores MD MPH
US Food and Drug Administration
Center for Biologics Evaluation and Research
Office of Biostatistics and Epidemiology
Division of Epidemiology
Silver Spring, Maryland
Oklahoma City, OK
MedicalResearch.com: What is the background for this study? Would you briefly explain what Sipuleucel-T is used for?
Response: Sipuleucel-T was the first therapeutic vaccine approved by the U.S. Food and Drug Administration (FDA) in 2010. It is indicated for the treatment of asymptomatic or minimally symptomatic, metastatic, castration-resistant prostate cancer (CRPC; prostate cancer that spreads while an individual is on hormone-blocking therapy). During the preparation of this product, the patient’s cells are collected (leukapheresis), sent for processing to generate a dose of patient-specific vaccine, and then administered intravenously back to the patient. This process is repeated approximately every two weeks for a total of three doses.
Except for the pre-marketing clinical trials that were reviewed during the sipuleucel-T approval process, post-marketing studies that have evaluated the safety profile of sipuleucel-T are scarce. Therefore, we used the FDA’s Adverse Event Reporting System (FAERS) database to summarize the adverse events reported to FDA by industry, medical professionals, and consumers. We also assessed whether sipuleucel-T and specific adverse events (product-event pairs) were reported more than expected compared to all other drug/biologic-adverse event pairs in the FAERS database.
 Dr. Graca Dores (left) and Dr. Perez-Vilar (senior author)[/caption]
Dr. Graca Dores MD MPH
US Food and Drug Administration
Center for Biologics Evaluation and Research
Office of Biostatistics and Epidemiology
Division of Epidemiology
Silver Spring, Maryland
Oklahoma City, OK
MedicalResearch.com: What is the background for this study? Would you briefly explain what Sipuleucel-T is used for?
Response: Sipuleucel-T was the first therapeutic vaccine approved by the U.S. Food and Drug Administration (FDA) in 2010. It is indicated for the treatment of asymptomatic or minimally symptomatic, metastatic, castration-resistant prostate cancer (CRPC; prostate cancer that spreads while an individual is on hormone-blocking therapy). During the preparation of this product, the patient’s cells are collected (leukapheresis), sent for processing to generate a dose of patient-specific vaccine, and then administered intravenously back to the patient. This process is repeated approximately every two weeks for a total of three doses.
Except for the pre-marketing clinical trials that were reviewed during the sipuleucel-T approval process, post-marketing studies that have evaluated the safety profile of sipuleucel-T are scarce. Therefore, we used the FDA’s Adverse Event Reporting System (FAERS) database to summarize the adverse events reported to FDA by industry, medical professionals, and consumers. We also assessed whether sipuleucel-T and specific adverse events (product-event pairs) were reported more than expected compared to all other drug/biologic-adverse event pairs in the FAERS database.
Dr. Graca Dores (left) and Dr. Perez-Vilar (senior author)[/caption]
Dr. Graca Dores MD MPH
US Food and Drug Administration
Center for Biologics Evaluation and Research
Office of Biostatistics and Epidemiology
Division of Epidemiology
Silver Spring, Maryland
Oklahoma City, OK
MedicalResearch.com: What is the background for this study? Would you briefly explain what Sipuleucel-T is used for?
Response: Sipuleucel-T was the first therapeutic vaccine approved by the U.S. Food and Drug Administration (FDA) in 2010. It is indicated for the treatment of asymptomatic or minimally symptomatic, metastatic, castration-resistant prostate cancer (CRPC; prostate cancer that spreads while an individual is on hormone-blocking therapy). During the preparation of this product, the patient’s cells are collected (leukapheresis), sent for processing to generate a dose of patient-specific vaccine, and then administered intravenously back to the patient. This process is repeated approximately every two weeks for a total of three doses.
Except for the pre-marketing clinical trials that were reviewed during the sipuleucel-T approval process, post-marketing studies that have evaluated the safety profile of sipuleucel-T are scarce. Therefore, we used the FDA’s Adverse Event Reporting System (FAERS) database to summarize the adverse events reported to FDA by industry, medical professionals, and consumers. We also assessed whether sipuleucel-T and specific adverse events (product-event pairs) were reported more than expected compared to all other drug/biologic-adverse event pairs in the FAERS database.

 Prof. Satchi-Fainaro[/caption]
Prof. Ronit Satchi-Fainaro, PhD
Head, Cancer Research and Nanomedicine Laboratory
Department of Physiology and Pharmacology,
Sackler Faculty of Medicine,
Tel Aviv University,
Tel-Aviv 69978, Israel
[caption id="attachment_50670" align="alignleft" width="116"]
Prof. Satchi-Fainaro[/caption]
Prof. Ronit Satchi-Fainaro, PhD
Head, Cancer Research and Nanomedicine Laboratory
Department of Physiology and Pharmacology,
Sackler Faculty of Medicine,
Tel Aviv University,
Tel-Aviv 69978, Israel
[caption id="attachment_50670" align="alignleft" width="116"] Prof. Florindo[/caption]
Prof. Helena Florindo, PhD
Head, BioNanoSciences – iMed.ULisboa
Faculty of Pharmacy,
University of Lisbon
Lisbon, Portugal
MedicalResearch.com: What are the main findings?
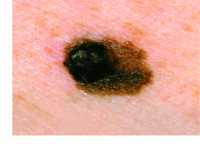
Response: The war against cancer in general, and melanoma in particular, has advanced over the years through a variety of treatment modalities, such as surgery, chemotherapy, radiation therapy and immunotherapy. The immune checkpoint inhibitors brought a breakthrough solution for advanced melanoma patients, but only a low percentage of those respond to this therapy, developing resistance and being affected by severe side effects. Despite the success of several vaccines against viral diseases, this success has not been materialized yet against cancer.
This study led by my lab at Tel Aviv University, and Helena Florindo’s lab at the University of Lisbon, describes the development of an effective nano-vaccine against melanoma, that also sensitizes the immune system to immunotherapies.
This nano-vaccine prevented melanoma, and also led to remarkable tumor inhibition and prolonged survival in mice already affected by this disease.
Prof. Florindo[/caption]
Prof. Helena Florindo, PhD
Head, BioNanoSciences – iMed.ULisboa
Faculty of Pharmacy,
University of Lisbon
Lisbon, Portugal
MedicalResearch.com: What are the main findings?
Response: The war against cancer in general, and melanoma in particular, has advanced over the years through a variety of treatment modalities, such as surgery, chemotherapy, radiation therapy and immunotherapy. The immune checkpoint inhibitors brought a breakthrough solution for advanced melanoma patients, but only a low percentage of those respond to this therapy, developing resistance and being affected by severe side effects. Despite the success of several vaccines against viral diseases, this success has not been materialized yet against cancer.
This study led by my lab at Tel Aviv University, and Helena Florindo’s lab at the University of Lisbon, describes the development of an effective nano-vaccine against melanoma, that also sensitizes the immune system to immunotherapies.
This nano-vaccine prevented melanoma, and also led to remarkable tumor inhibition and prolonged survival in mice already affected by this disease. 
 Dr. Nandi[/caption]
Arindam Nandi PhD
Center for Disease Dynamics, Economics & Policy
MedicalResearch.com: What is the background for this study?
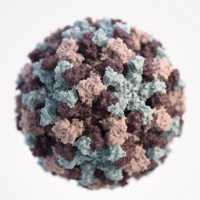
Response: The motivation for this study comes from a small but growing body of evidence on the potential long-term benefits of vaccines. The recent resurgence of measles outbreaks in several countries which had previously eliminated the virus makes our study additionally relevant. There have been over 1,000 measles cases reported across 28 states in the US so far in 2019, which is the largest number of cases the country has seen in almost 3 decades. Similarly high number of cases have been reported in several European countries in recent years. This study reiterates the importance of vaccination and proves the long-term benefits of the measles vaccine in low- and middle-income countries, which account for a large proportion of global measles cases.
Dr. Nandi[/caption]
Arindam Nandi PhD
Center for Disease Dynamics, Economics & Policy
MedicalResearch.com: What is the background for this study?
Response: The motivation for this study comes from a small but growing body of evidence on the potential long-term benefits of vaccines. The recent resurgence of measles outbreaks in several countries which had previously eliminated the virus makes our study additionally relevant. There have been over 1,000 measles cases reported across 28 states in the US so far in 2019, which is the largest number of cases the country has seen in almost 3 decades. Similarly high number of cases have been reported in several European countries in recent years. This study reiterates the importance of vaccination and proves the long-term benefits of the measles vaccine in low- and middle-income countries, which account for a large proportion of global measles cases.
















 Kathryn M. Edwards, M.D.
Sarah H. Sell and Cornelius Vanderbilt Chair in Pediatrics
Professor of Pediatrics
Vanderbilt University School of Medicine
Dr. Edwards discusses the statement from the Infectious Diseases Society of America (IDSA) regarding the Centers for Disease Control and Prevention’s new data on child vaccine rates across the United States.
MedicalResearch.com: What is the background for this study? What are the main findings?
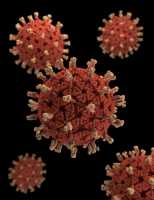
Response: To monitor the uptake of vaccines the CDC conducts a National Immunization Survey each year. This survey is conducted by random-digit dialing (cell phones or landlines) of parents and guardians of children 19-35 months of age. The interviewers ask the families who provides the vaccines for their children and if these providers can be contacted to inquire about the immunizations received. The overall response rate to the telephone survey was 26% and immunization records were provided on 54% of the children where permission was granted. Overall 15, 333 children had their immunization records reviewed.
When comparing immunization rates for 2017 and 2016, the last two years of the study, several new findings were discovered.
First the overall coverage rate for 3 doses of polio vaccine, one dose of MMR, 3 doses of Hepatitis b, and 1 dose of chickenpox vaccine was 90%, a high rate of coverage. Children were less likely to be up to date on the hepatitis A vaccine (70%) and rotavirus vaccine (73%). Coverage was lower for children living in rural areas when compared with urban areas and children living in rural areas had higher percentages of no vaccine receipt at all (1.9%) compared with those living in urban areas (1%).
There were more uninsured children in 2017 at 2.8% and these children had lower immunization rates. In fact 7.1% of the children with no insurance were totally unimmunized when compared with 0.8% unimmunized in those with private insurance. Vaccine coverage varies by state and by vaccine.
Kathryn M. Edwards, M.D.
Sarah H. Sell and Cornelius Vanderbilt Chair in Pediatrics
Professor of Pediatrics
Vanderbilt University School of Medicine
Dr. Edwards discusses the statement from the Infectious Diseases Society of America (IDSA) regarding the Centers for Disease Control and Prevention’s new data on child vaccine rates across the United States.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To monitor the uptake of vaccines the CDC conducts a National Immunization Survey each year. This survey is conducted by random-digit dialing (cell phones or landlines) of parents and guardians of children 19-35 months of age. The interviewers ask the families who provides the vaccines for their children and if these providers can be contacted to inquire about the immunizations received. The overall response rate to the telephone survey was 26% and immunization records were provided on 54% of the children where permission was granted. Overall 15, 333 children had their immunization records reviewed.
When comparing immunization rates for 2017 and 2016, the last two years of the study, several new findings were discovered.
First the overall coverage rate for 3 doses of polio vaccine, one dose of MMR, 3 doses of Hepatitis b, and 1 dose of chickenpox vaccine was 90%, a high rate of coverage. Children were less likely to be up to date on the hepatitis A vaccine (70%) and rotavirus vaccine (73%). Coverage was lower for children living in rural areas when compared with urban areas and children living in rural areas had higher percentages of no vaccine receipt at all (1.9%) compared with those living in urban areas (1%).
There were more uninsured children in 2017 at 2.8% and these children had lower immunization rates. In fact 7.1% of the children with no insurance were totally unimmunized when compared with 0.8% unimmunized in those with private insurance. Vaccine coverage varies by state and by vaccine.











