Author Interviews, Endocrinology, Hormone Therapy, Testosterone / 09.10.2025
Exploring Male Hormone Restoration with Enclomiphene
Editor's note: Enclomiphene is an investigational drug that is not FDA approved. Enclomiphene must be taken under a health care provider's supervision. Enclomiphene may have significant side effects and should never be used by women, those with liver disease or other medical conditions. This blog and the links provided are for informational purposes only and is not specific medical advice. Products are not tested or warranted by MedicalResearch.com or Eminent Domains Inc.

Revisiting Testosterone Therapy: Is Enclomiphene the Future of Male Hormone Restoration?
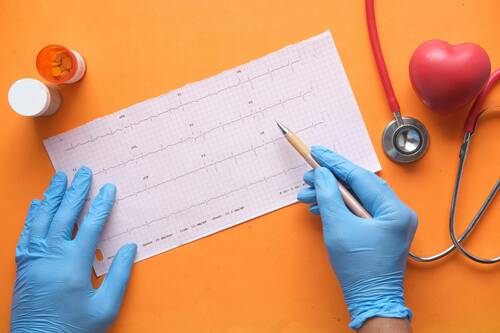
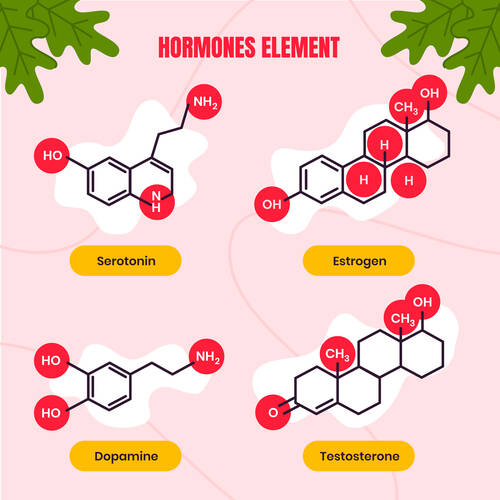
Testosterone therapy has long been a key treatment for male hypogonadism, a condition marked by low testosterone and related symptoms such as fatigue, reduced libido, and loss of muscle mass. Yet, traditional testosterone replacement therapy (TRT) is not without drawbacks. It can suppress natural hormone production, impair fertility, and carry cardiovascular risks. The emergence of Enclomiphene citrate, a selective estrogen receptor modulator (SERM), offers a promising alternative. Rather than replacing testosterone externally, it stimulates the body’s natural production. This shift toward physiological restoration may redefine the future of male hormone management.


























 Dr. GALBIATI[/caption]
Francesca Galbiati, MD
Clinical/Research fellow in Endocrinology
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study?
Response: Arginine-vasopressin (AVP) is a neurohormone well known for its role in water balance regulation. It promotes renal water absorption in the kidney, to maintain normal sodium levels in the blood via a tightly controlled osmotic regulation. Besides AVP classical role, data have shown that AVP effects extend beyond water balance regulation. Animal studies have shown that AVP has metabolic effects, including reducing food intake, inducing lipolysis, and promoting muscle regeneration in male mice.
Furthermore, AVP is regulated differently in males and females, and affects cognition differently across sexes, a phenomenon called sexual dimorphism. However, it is unknown whether its dimorphism translates to metabolism. Also, findings on AVP metabolic role are inconsistent, possibly due to the opposing effects of AVP at different receptor subtypes, which regulation is still largely unknown. We performed this study to better investigate AVP metabolic role, and explore sex differences. We hypothesized that AVP would be positively associated with BMI, adiposity, and lean mass (acting as a signal of energy availability). We also predicted that relationships between AVP and body composition measures would differ by sex. We used the AVP area under the curve around a standardized meal to better capture repeated measures in response to food intake (that directly impacts energy availability). This also allowed to avoid the possible risk of fluctuating AVP levels due to possible pulsatile secretion.
Dr. GALBIATI[/caption]
Francesca Galbiati, MD
Clinical/Research fellow in Endocrinology
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study?
Response: Arginine-vasopressin (AVP) is a neurohormone well known for its role in water balance regulation. It promotes renal water absorption in the kidney, to maintain normal sodium levels in the blood via a tightly controlled osmotic regulation. Besides AVP classical role, data have shown that AVP effects extend beyond water balance regulation. Animal studies have shown that AVP has metabolic effects, including reducing food intake, inducing lipolysis, and promoting muscle regeneration in male mice.
Furthermore, AVP is regulated differently in males and females, and affects cognition differently across sexes, a phenomenon called sexual dimorphism. However, it is unknown whether its dimorphism translates to metabolism. Also, findings on AVP metabolic role are inconsistent, possibly due to the opposing effects of AVP at different receptor subtypes, which regulation is still largely unknown. We performed this study to better investigate AVP metabolic role, and explore sex differences. We hypothesized that AVP would be positively associated with BMI, adiposity, and lean mass (acting as a signal of energy availability). We also predicted that relationships between AVP and body composition measures would differ by sex. We used the AVP area under the curve around a standardized meal to better capture repeated measures in response to food intake (that directly impacts energy availability). This also allowed to avoid the possible risk of fluctuating AVP levels due to possible pulsatile secretion.

 Dr. Goodrich[/caption]
Jesse Goodrich PhD
Assistant Professor
Department of Population and Public Health Sciences
Keck School of Medicine
University of Southern California
MedicalResearch.com: What is the background for this study?
Response: Per- and poly-fluoroalkyl substances (PFAS) are a group of persistent chemicals that are known to interfere with hormones and metabolism. In our previous research, we have found that PFAS exposure is associated several specific diseases, especially in children and adolescents. These include obesity, type 2 diabetes, liver disease, and even liver cancer. However, we are still only just starting to fully understand all of the health effects of the many different PFAS in existence. Previous studies have focused primarily on one or two main PFAS. However, there are over 9,000 known PFAS, and people are exposed not just to a single PFAS but to mixtures of many PFAS. Importantly, the combination of these chemical exposures may affect us differently than single exposures alone.
To address this challenge, we used an innovative approach to study design to examine how exposure to PFAS impacts biological processes which may underly the development of many different diseases in adolescents and young adults. To do this, we first measured thousands of naturally occurring chemicals, known as metabolites, in people's blood. Then, using a new biostatistical method developed by our team, we identified how exposure to a mixture of several PFAS impacted each individual chemical. Finally, we used this information to determine which biological processes are changed by PFAS exposure.
Dr. Goodrich[/caption]
Jesse Goodrich PhD
Assistant Professor
Department of Population and Public Health Sciences
Keck School of Medicine
University of Southern California
MedicalResearch.com: What is the background for this study?
Response: Per- and poly-fluoroalkyl substances (PFAS) are a group of persistent chemicals that are known to interfere with hormones and metabolism. In our previous research, we have found that PFAS exposure is associated several specific diseases, especially in children and adolescents. These include obesity, type 2 diabetes, liver disease, and even liver cancer. However, we are still only just starting to fully understand all of the health effects of the many different PFAS in existence. Previous studies have focused primarily on one or two main PFAS. However, there are over 9,000 known PFAS, and people are exposed not just to a single PFAS but to mixtures of many PFAS. Importantly, the combination of these chemical exposures may affect us differently than single exposures alone.
To address this challenge, we used an innovative approach to study design to examine how exposure to PFAS impacts biological processes which may underly the development of many different diseases in adolescents and young adults. To do this, we first measured thousands of naturally occurring chemicals, known as metabolites, in people's blood. Then, using a new biostatistical method developed by our team, we identified how exposure to a mixture of several PFAS impacted each individual chemical. Finally, we used this information to determine which biological processes are changed by PFAS exposure.