Endocrinology, Sexual Health / 30.04.2025
How Long Do the Results of a P-Shot Last, and What Should You Expect?
[caption id="attachment_68237" align="aligncenter" width="232"] Photo by Italo Melo[/caption]
The P-Shot, a revolutionary treatment for erectile dysfunction, has garnered significant attention for its non-invasive approach, using platelet-rich plasma (PRP) to enhance sexual performance. Results from the P-Shot can last anywhere from one to two years, providing long-lasting improvements for many individuals. The treatment's time frame for noticeable effects varies, with some people observing changes within a few weeks and others needing several months.
For those considering this treatment, it's important to understand the benefits and limitations. Individual outcomes can largely depend on the person’s unique circumstances and health. These factors can influence not only the effectiveness of the procedure but also the expectations around it. Reviewing p-shot before and after results from real patients can provide valuable insight into the range of outcomes—some notice enhanced performance or sensitivity, while others see subtler changes. It’s also worth noting that psychological factors, underlying health conditions, and adherence to post-treatment care play a significant role. Consulting with a specialist can help clarify what’s realistic for your specific situation.
Individuals exploring this option should approach it as part of a holistic approach to sexual wellness, considering ongoing lifestyle choices and health management to maximize benefits. By setting realistic expectations and maintaining open communication with healthcare providers, users can optimize their experience with the P-Shot, ensuring it aligns with their personal goals for sexual health improvement.
Photo by Italo Melo[/caption]
The P-Shot, a revolutionary treatment for erectile dysfunction, has garnered significant attention for its non-invasive approach, using platelet-rich plasma (PRP) to enhance sexual performance. Results from the P-Shot can last anywhere from one to two years, providing long-lasting improvements for many individuals. The treatment's time frame for noticeable effects varies, with some people observing changes within a few weeks and others needing several months.
For those considering this treatment, it's important to understand the benefits and limitations. Individual outcomes can largely depend on the person’s unique circumstances and health. These factors can influence not only the effectiveness of the procedure but also the expectations around it. Reviewing p-shot before and after results from real patients can provide valuable insight into the range of outcomes—some notice enhanced performance or sensitivity, while others see subtler changes. It’s also worth noting that psychological factors, underlying health conditions, and adherence to post-treatment care play a significant role. Consulting with a specialist can help clarify what’s realistic for your specific situation.
Individuals exploring this option should approach it as part of a holistic approach to sexual wellness, considering ongoing lifestyle choices and health management to maximize benefits. By setting realistic expectations and maintaining open communication with healthcare providers, users can optimize their experience with the P-Shot, ensuring it aligns with their personal goals for sexual health improvement.
 Photo by Italo Melo[/caption]
The P-Shot, a revolutionary treatment for erectile dysfunction, has garnered significant attention for its non-invasive approach, using platelet-rich plasma (PRP) to enhance sexual performance. Results from the P-Shot can last anywhere from one to two years, providing long-lasting improvements for many individuals. The treatment's time frame for noticeable effects varies, with some people observing changes within a few weeks and others needing several months.
For those considering this treatment, it's important to understand the benefits and limitations. Individual outcomes can largely depend on the person’s unique circumstances and health. These factors can influence not only the effectiveness of the procedure but also the expectations around it. Reviewing p-shot before and after results from real patients can provide valuable insight into the range of outcomes—some notice enhanced performance or sensitivity, while others see subtler changes. It’s also worth noting that psychological factors, underlying health conditions, and adherence to post-treatment care play a significant role. Consulting with a specialist can help clarify what’s realistic for your specific situation.
Individuals exploring this option should approach it as part of a holistic approach to sexual wellness, considering ongoing lifestyle choices and health management to maximize benefits. By setting realistic expectations and maintaining open communication with healthcare providers, users can optimize their experience with the P-Shot, ensuring it aligns with their personal goals for sexual health improvement.
Photo by Italo Melo[/caption]
The P-Shot, a revolutionary treatment for erectile dysfunction, has garnered significant attention for its non-invasive approach, using platelet-rich plasma (PRP) to enhance sexual performance. Results from the P-Shot can last anywhere from one to two years, providing long-lasting improvements for many individuals. The treatment's time frame for noticeable effects varies, with some people observing changes within a few weeks and others needing several months.
For those considering this treatment, it's important to understand the benefits and limitations. Individual outcomes can largely depend on the person’s unique circumstances and health. These factors can influence not only the effectiveness of the procedure but also the expectations around it. Reviewing p-shot before and after results from real patients can provide valuable insight into the range of outcomes—some notice enhanced performance or sensitivity, while others see subtler changes. It’s also worth noting that psychological factors, underlying health conditions, and adherence to post-treatment care play a significant role. Consulting with a specialist can help clarify what’s realistic for your specific situation.
Individuals exploring this option should approach it as part of a holistic approach to sexual wellness, considering ongoing lifestyle choices and health management to maximize benefits. By setting realistic expectations and maintaining open communication with healthcare providers, users can optimize their experience with the P-Shot, ensuring it aligns with their personal goals for sexual health improvement.
Key Takeaways
- P-Shot results last one to two years.
- Noticeable effects vary per individual.
- Non-invasive option enhances sexual health.













 Dr. Ottesen Kennair[/caption]
Leif Edward Ottesen Kennair, Phd
Professor, Department of Psychology
Norwegian University of Science and Technology
Trondheim, Norway
MedicalResearch.com: What is the background for this study?
Response: We have two important lines of research running parallel: 1) research into casual sex research. Over several papers inspired by previous evolutionary studies on casual sex we map the proximate mechanisms involved in regret. However, the adaptive function of regret: more adaptive future choices, was not addressed. This is something that most people and most regret researchers just take for granted. Bendixen et al 2017, Kennair et al 2016, 2018. 2) Research into how worry and rumination is not adaptive and how changing metacognitions about these mental processes are helpful here and now, and how discontinuing these processes is an efficient treatment of GAD and MDD. Kennair et al 2017. Solem et al 2019.
We found that it was important to question whether regret indeed was adaptive and affected more adaptive future short-term sexual choices. However, this demands a longitudinal design and such data are not easy to collect.
Dr. Ottesen Kennair[/caption]
Leif Edward Ottesen Kennair, Phd
Professor, Department of Psychology
Norwegian University of Science and Technology
Trondheim, Norway
MedicalResearch.com: What is the background for this study?
Response: We have two important lines of research running parallel: 1) research into casual sex research. Over several papers inspired by previous evolutionary studies on casual sex we map the proximate mechanisms involved in regret. However, the adaptive function of regret: more adaptive future choices, was not addressed. This is something that most people and most regret researchers just take for granted. Bendixen et al 2017, Kennair et al 2016, 2018. 2) Research into how worry and rumination is not adaptive and how changing metacognitions about these mental processes are helpful here and now, and how discontinuing these processes is an efficient treatment of GAD and MDD. Kennair et al 2017. Solem et al 2019.
We found that it was important to question whether regret indeed was adaptive and affected more adaptive future short-term sexual choices. However, this demands a longitudinal design and such data are not easy to collect.

 Dr. Kaufman[/caption]
Gregory Kaufman, M.D.
Senior Vice President
Global Clinical and Medical Affairs
Specialty at Lupin
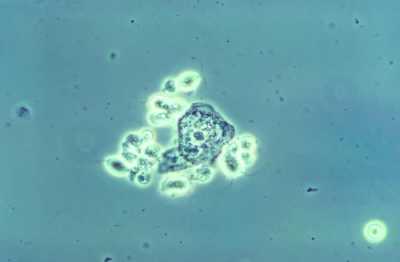
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by trichomoniasis? How common is this infection?
Response: The Phase 3 trial evaluated the effectiveness and safety of a single oral dose of Solosec® (secnidazole) 2g oral granules for the treatment of trichomoniasis in adult women. Top-line results were positive and showed that Solosec was generally well-tolerated.
Trichomoniasis is the most common non-viral sexually transmitted infection (STI) in the U.S., and is caused by a protozoan parasite called Trichomonas vaginalis.
Dr. Kaufman[/caption]
Gregory Kaufman, M.D.
Senior Vice President
Global Clinical and Medical Affairs
Specialty at Lupin
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by trichomoniasis? How common is this infection?
Response: The Phase 3 trial evaluated the effectiveness and safety of a single oral dose of Solosec® (secnidazole) 2g oral granules for the treatment of trichomoniasis in adult women. Top-line results were positive and showed that Solosec was generally well-tolerated.
Trichomoniasis is the most common non-viral sexually transmitted infection (STI) in the U.S., and is caused by a protozoan parasite called Trichomonas vaginalis.










 Dr. Lischke[/caption]
Dr. Alexander Lischke, Dipl.-Psych.
Universität Greifswald
Institut für Psychologie
Physiologische und Klinische Psychologie/Psychotherapie
University of Greifswald, Germany
MedicalResearch.com: What is the background for this study?
Response: We know for a long time that cyclic variations in womens' estrogen and progesterone levels affect their emotion recognition abilities by modulating neural activity in brain regions implicated in emotion processing. We also know that oral contraceptives suppress cyclic variations in womens' estrogen and progesterone levels. We, thus, assumed that oral contraceptives would affect womens' emotion recognition abilities due to the aforementioned suppression of cylic variations in estrogen and progesterone levels that modulate neural activity in brain regions during emotion processing. To test this assumption, at least with respect to the behavioral effects of oral contraceptive use on emotion recognition, we performed the current study.
We recruited regular cylcling women with and without oral contraceptive use for our study. None of the women were in psychotherapeutical or psychopharmacological treatment at the time of the study. During the study, women performed a emotion recognition task that required the recognition of complex emotional expressions like, for example, pride or contempt.
Dr. Lischke[/caption]
Dr. Alexander Lischke, Dipl.-Psych.
Universität Greifswald
Institut für Psychologie
Physiologische und Klinische Psychologie/Psychotherapie
University of Greifswald, Germany
MedicalResearch.com: What is the background for this study?
Response: We know for a long time that cyclic variations in womens' estrogen and progesterone levels affect their emotion recognition abilities by modulating neural activity in brain regions implicated in emotion processing. We also know that oral contraceptives suppress cyclic variations in womens' estrogen and progesterone levels. We, thus, assumed that oral contraceptives would affect womens' emotion recognition abilities due to the aforementioned suppression of cylic variations in estrogen and progesterone levels that modulate neural activity in brain regions during emotion processing. To test this assumption, at least with respect to the behavioral effects of oral contraceptive use on emotion recognition, we performed the current study.
We recruited regular cylcling women with and without oral contraceptive use for our study. None of the women were in psychotherapeutical or psychopharmacological treatment at the time of the study. During the study, women performed a emotion recognition task that required the recognition of complex emotional expressions like, for example, pride or contempt.