How Building Healthy Routines Supports Psychological Stability
 Editor's note: This piece discusses mental health issues. If you have experienced suicidal thoughts or have lost someone to suicide and want to seek help, you can contact the Crisis Text Line by texting "START" to 741-741 or call the Suicide Prevention Lifeline at 800-273-8255.
Want to feel more stable in your day-to-day life?
Simple tasks can be monumental for those who live with mental illness and addiction. Rising out of bed. Eating a nutritious meal. Attending therapy.
Here's the good news:
Consistently doing something every day can turn all of that around. It's also one of the most under utilized tools.
Routine is particularly important for those suffering from a dual diagnosis. If you have two conditions occurring simultaneously your days can seem random and hectic. Routine is where you can regain some control. Dual diagnosis treatment that is effective works to restore some of the daily routines you need to stay grounded. That process for many begins with drug rehab services in Northern Virginia.
Let's jump in...
What you'll discover:
Why Routines Matter For Dual Diagnosis
The Building Blocks Of A Healthy Routine
How Structure Calms The Mind
Simple Steps To Get Started
Editor's note: This piece discusses mental health issues. If you have experienced suicidal thoughts or have lost someone to suicide and want to seek help, you can contact the Crisis Text Line by texting "START" to 741-741 or call the Suicide Prevention Lifeline at 800-273-8255.
Want to feel more stable in your day-to-day life?
Simple tasks can be monumental for those who live with mental illness and addiction. Rising out of bed. Eating a nutritious meal. Attending therapy.
Here's the good news:
Consistently doing something every day can turn all of that around. It's also one of the most under utilized tools.
Routine is particularly important for those suffering from a dual diagnosis. If you have two conditions occurring simultaneously your days can seem random and hectic. Routine is where you can regain some control. Dual diagnosis treatment that is effective works to restore some of the daily routines you need to stay grounded. That process for many begins with drug rehab services in Northern Virginia.
Let's jump in...
What you'll discover:
Why Routines Matter For Dual Diagnosis
The Building Blocks Of A Healthy Routine
How Structure Calms The Mind
Simple Steps To Get Started
Karolinska Institutet Evaluates Single Dose of Psilocybin for Depression
 Dr. Hampus Yngwe[/caption]
MedicalResearch.com Interview with:
Hampus Yngwe, MD, MSc
Centre for Psychiatry Research,
Department of Clinical Neuroscience,
Karolinska Institutet, and
Stockholm Health Care Services
Stockholm, Sweden
MedicalResearch.com: What is the background for this study?
Response: Depression is a common and disabling condition and current treatments do not work for all patients. Psilocybin has shown promise as a rapid-acting treatment, but more controlled studies are needed to clarify its effects, durability and safety.
Dr. Hampus Yngwe[/caption]
MedicalResearch.com Interview with:
Hampus Yngwe, MD, MSc
Centre for Psychiatry Research,
Department of Clinical Neuroscience,
Karolinska Institutet, and
Stockholm Health Care Services
Stockholm, Sweden
MedicalResearch.com: What is the background for this study?
Response: Depression is a common and disabling condition and current treatments do not work for all patients. Psilocybin has shown promise as a rapid-acting treatment, but more controlled studies are needed to clarify its effects, durability and safety.
How Residential Programs in Austin Help Teen Girls Reconnect With Parents
 Pexels[/caption]
Editor's note: This piece discusses mental health issues. If you have experienced suicidal thoughts or have lost someone to suicide and want to seek help, you can contact the Crisis Text Line by texting "START" to 741-741 or call the Suicide Prevention Lifeline at 800-273-8255.
Tension at home can leave parents and teen girls unsure how to move forward. In Austin, residential programs step in with structure, therapy, and clear expectations that guide both sides toward repair. These programs do more than address mental health or behavior — they help families reset how they relate to each other.
Residential programs in Austin may help teen girls reconnect with parents by creating a safe space for therapy, clear communication, and shared accountability that rebuilds trust over time. Staff guides teen girls through daily routines, individual therapy, and family sessions that focus on honest dialogue. As a result, parents gain tools to respond with calm and consistency instead of fear or anger.
Pexels[/caption]
Editor's note: This piece discusses mental health issues. If you have experienced suicidal thoughts or have lost someone to suicide and want to seek help, you can contact the Crisis Text Line by texting "START" to 741-741 or call the Suicide Prevention Lifeline at 800-273-8255.
Tension at home can leave parents and teen girls unsure how to move forward. In Austin, residential programs step in with structure, therapy, and clear expectations that guide both sides toward repair. These programs do more than address mental health or behavior — they help families reset how they relate to each other.
Residential programs in Austin may help teen girls reconnect with parents by creating a safe space for therapy, clear communication, and shared accountability that rebuilds trust over time. Staff guides teen girls through daily routines, individual therapy, and family sessions that focus on honest dialogue. As a result, parents gain tools to respond with calm and consistency instead of fear or anger.
Finding Hope and Healing: Online Opioid Addiction Treatment in Kentucky
 Pexels[/caption]
Pexels[/caption]
Online Opioid Addiction Treatment in Kentucky: How Telehealth Is Changing Recovery
Kentucky families know all too well how much damage opioid addiction can cause. But today, hope is closer than ever. New digital tools mean you can start your recovery without leaving your house or missing work. If you're ready for a change, online opioid addiction treatment in Kentucky with Aegis Medical is designed to provide specialized, compassionate care that is easy to reach and built to help you succeed on your own terms.The Growing Crisis in Kentucky
Kentucky has been hit hard by the opioid epidemic. Recent data shows the state consistently has some of the highest overdose rates in the country. This isn't just a city problem or a rural problem — it's everywhere, fueled by job losses, the difficulty of finding doctors in small towns, and the high availability of both prescription pills and illegal street drugs. For most people, beating addiction isn't just about trying harder. It's a medical condition that needs a real medical plan — one that addresses physical dependency while also identifying the mental and social triggers. Traditional rehab centers are valuable, but they aren't always easy to reach. Whether it's the cost, the drive, or life getting in the way, those barriers are real. This is why online options are changing the picture for so many Kentuckians.Why Choose Online Treatment
Online programs, sometimes called telehealth, have become a lifeline for Kentuckians, especially in rural areas. More people are choosing this path for several reasons:- Easy access. You get expert medical care from home. No more driving an hour each way to a clinic.
- Total privacy. Some people worry about being seen at a local rehab center. Online treatment is completely private, which helps many people feel safe enough to start.
- Flexible timing. You can fit appointments around your job, your kids, and your life.
- Staying on track. Even after the hardest part of detox is over, online programs keep you connected to support so you don't feel alone in your recovery.
About Aegis Medical: Expert Care at Home
Aegis Medical combines high-quality medical science with the convenience of a smartphone app or video call. Their approach includes:- Expert doctors. Their team specializes in addiction medicine and understands how opioids affect the brain.
- Medication-Assisted Treatment (MAT). They use proven, FDA-approved medicines like buprenorphine to help manage withdrawal symptoms and cravings.
- Individualized plans. Your treatment plan is built around your health history and your goals.
- Counseling support. Therapy is included to help address the emotional side of addiction alongside the physical.
- Regular check-ins. Ongoing virtual visits to monitor progress and adjust care as needed.
How Medication-Assisted Treatment Helps
A major part of recovery at Aegis Medical is Medication-Assisted Treatment, widely considered the gold standard for opioid recovery. It combines medicine with talk therapy and works in three key ways:- Stopping cravings by reducing the brain signals that drive drug-seeking behavior.
- Ending withdrawal by preventing the physical sickness that makes quitting so difficult.
- Supporting brain recovery by helping normal neurological function resume after sustained opioid use.
What to Expect When You Sign Up
- The consult. A private video call to understand your medical history and needs.
- The strategy. A doctor builds a recovery plan tailored to your life.
- The medication. Prescriptions are managed and sent to your local pharmacy.
- Counseling. Virtual sessions to address the mental and emotional side of addiction.
- Ongoing support. Continuous check-ins to keep you feeling supported and safe.
- Family education. Optional sessions to help build a stronger support system at home.
Breaking Barriers Across the State
In Kentucky, travel distances and concerns about stigma often stop people from seeking help. Online treatment removes those barriers. You skip the long commutes and keep your recovery completely private. It's expert care that fits your schedule, not the other way around.Take Your First Step Today
You don't have to do this alone. If you're tired of the cycle of addiction, help is available. Exploring online opioid addiction treatment in Kentucky with Aegis Medical is a straightforward first step. Their team is ready to walk with you every step of the way.The Clinical Efficacy of Modern Substance Screening in Occupational Health
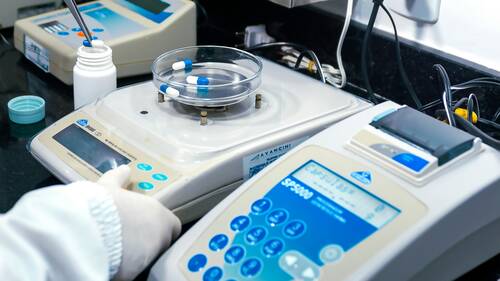 Photo by Pilan Filmes:[/caption]
Occupational health and safety protocols have evolved significantly over the past decade. Australian workplaces are increasingly adopting evidence-based strategies to mitigate risks and ensure employee wellbeing. A critical component of these modern safety management systems is the accurate identification and prevention of impairment on the job. Substance use remains a complex challenge for industries operating heavy machinery, transport sectors, and hazardous construction environments. Beyond the immediate risk of physical injury, the financial burden of workplace accidents strains healthcare systems and reduces overall productivity. To address these vulnerabilities, safety officers rely heavily on preliminary biological testing to make quick determinations following a workplace accident or a reasonable suspicion report. Utilising a urine drug test kit allows occupational health teams to quickly identify the presence of specific metabolites within established biological windows. This ensures that workplace policies are guided by scientific reality rather than assumption.
The accuracy of substance detection fundamentally relies on the biological processes of human metabolism and elimination. Different substances metabolise at drastically varying rates depending on factors such as an individual's hydration levels, body mass index, and the frequency of substance use. This physiological variance creates specific detection windows that clinical officers must understand to administer fair and effective evaluations.
Photo by Pilan Filmes:[/caption]
Occupational health and safety protocols have evolved significantly over the past decade. Australian workplaces are increasingly adopting evidence-based strategies to mitigate risks and ensure employee wellbeing. A critical component of these modern safety management systems is the accurate identification and prevention of impairment on the job. Substance use remains a complex challenge for industries operating heavy machinery, transport sectors, and hazardous construction environments. Beyond the immediate risk of physical injury, the financial burden of workplace accidents strains healthcare systems and reduces overall productivity. To address these vulnerabilities, safety officers rely heavily on preliminary biological testing to make quick determinations following a workplace accident or a reasonable suspicion report. Utilising a urine drug test kit allows occupational health teams to quickly identify the presence of specific metabolites within established biological windows. This ensures that workplace policies are guided by scientific reality rather than assumption.
The accuracy of substance detection fundamentally relies on the biological processes of human metabolism and elimination. Different substances metabolise at drastically varying rates depending on factors such as an individual's hydration levels, body mass index, and the frequency of substance use. This physiological variance creates specific detection windows that clinical officers must understand to administer fair and effective evaluations.
Adolescents View Cannabis as Less Harmful Than Alcohol and Tobacco — New California Survey Data
Please note: Cannabis laws and regulations vary by state and locality. Cannabis use may have significant health risks, particularly for adolescents, pregnant individuals, and those with a history of mental health conditions. Cannabis has not been approved by the FDA for most uses and may interact with medications. Do not use cannabis as a substitute for medical treatment. The information in this post is for educational purposes only and does not constitute medical or legal advice. Always consult your physician or qualified healthcare provider before making decisions about cannabis use. Do not use cannabis products if pregnant, nursing or may become pregnant. Children should never be exposed to cannabis products.
MedicalResearch.com Interview with: [caption id="attachment_73658" align="alignleft" width="130"] Prof. Shu-Hong Zhu[/caption]
Shu-Hong Zhu, Ph.D.
Professor of Family Medicine and Public Health and
Director of the Center for Research and Intervention in Tobacco Control (CRITC)
University of California, San Diego
MedicalResearch.com: What is the background for this study?
Response: Cannabis use in the U.S. has steadily increased over recent decades. As use rates increased, perceptions that cannabis use is harmful have trended in the opposite direction.
Declining harm perceptions in the broader population are concerning in part because of their influence on adolescents. Regular cannabis use during adolescents can negatively impact overall functioning, cognition, and educational achievement. It can lead to depression, psychosis, and suicidality. If young people don’t perceive cannabis as harmful, they are more likely to use it and suffer these effects.
The purpose of this study was to investigate the extent to which adolescents view the everyday and occasional use of cannabis as harmful, and to compare their perceptions of cannabis to their perceptions of alcohol, cigarettes, and nicotine vapes. It used data from over 160,000 students who took the 2019−2020 California Student Tobacco Survey and over 16,000 who took the 2024 California Youth Tobacco Survey.
Prof. Shu-Hong Zhu[/caption]
Shu-Hong Zhu, Ph.D.
Professor of Family Medicine and Public Health and
Director of the Center for Research and Intervention in Tobacco Control (CRITC)
University of California, San Diego
MedicalResearch.com: What is the background for this study?
Response: Cannabis use in the U.S. has steadily increased over recent decades. As use rates increased, perceptions that cannabis use is harmful have trended in the opposite direction.
Declining harm perceptions in the broader population are concerning in part because of their influence on adolescents. Regular cannabis use during adolescents can negatively impact overall functioning, cognition, and educational achievement. It can lead to depression, psychosis, and suicidality. If young people don’t perceive cannabis as harmful, they are more likely to use it and suffer these effects.
The purpose of this study was to investigate the extent to which adolescents view the everyday and occasional use of cannabis as harmful, and to compare their perceptions of cannabis to their perceptions of alcohol, cigarettes, and nicotine vapes. It used data from over 160,000 students who took the 2019−2020 California Student Tobacco Survey and over 16,000 who took the 2024 California Youth Tobacco Survey.
From promoting relaxation to improving sleep quality, cannabis is increasingly explored as a natural option for managing stress and anxiety...
Clinical Advancements in Cannabidiol Therapeutics and the Shift Toward Specialised Care Models
 Pexels[/caption]
Pexels[/caption]
Please note: Cannabis and cannabidiol (CBD) products are generally not FDA tested or approved for all conditions referenced in this article. Cannabis and CBD products can interfere with medications including blood pressure medications and anticoagulants. Do not use cannabis products if pregnant, nursing or planning to become pregnant. Do not delay seeking medical attention for medical concerns by using cannabis or CBD products without medical advice. Cannabis products should not be used while driving or operating machinery. Statements and product contents have not been independently confirmed by MedicalResearch.com or Eminent Domains Inc. Please discuss any and all cannabis or CBD use with your health care provider before beginning any such regimen.
The landscape of chronic condition management has undergone a significant transformation over the past decade. For years, the medical community relied heavily on isolated symptom treatments and traditional pharmacological interventions to manage complex ailments. Patients suffering from long-term conditions like neuropathy, chronic inflammation, or severe anxiety frequently found themselves cycling through various medications with limited success and significant side effects. These recurring challenges have prompted healthcare professionals to rethink standard protocols. The latest clinical evidence supports a multidimensional approach to chronic pain that incorporates alternative and complementary therapies, reflecting a broader shift away from conventional, single-track treatments. As recent insights into pain management demonstrate, invasive procedures and heavy medications are no longer the default first-line defense. Instead, clinicians are increasingly advocating for whole-person care that values patient lifestyle strategies, psychological support, and alternative therapeutics. Among these emerging alternatives, cannabidiol has garnered substantial attention from the global medical and academic communities as a viable option for those who have exhausted standard therapies.If you or someone you know is struggling or in crisis, help is available.
Call or text 988 or chat at 988lifeline.org. To learn how to get support for mental health, drug or alcohol conditions, visit FindSupport.gov. If you are ready to locate a treatment facility or provider, visit FindTreatment.gov or call 800-662-HELP (4357).
U.S. veterans or service members in crisis can call 988 then press "1" for the Veterans Crisis Line, text 838255, or chat online.
The Suicide & Crisis Lifeline has a Spanish language line at 1-888-628-9454 (toll-free).
 Unsplash image[/caption]
Addiction recovery is often misunderstood as a matter of willpower. If someone wants to stop badly enough, they will. If they don't, they won't. But that perspective leaves out something critical. Addiction is not just behavioral. It's biological, psychological, and deeply influenced by environment.
Over the past few decades, research has shifted how professionals understand and treat addiction. Instead of viewing it as a failure of discipline, it's now approached as a complex condition that affects brain function, emotional regulation, and decision-making processes. That shift has led to more effective, science-backed treatment methods that focus on long-term outcomes rather than short-term fixes.
Unsplash image[/caption]
Addiction recovery is often misunderstood as a matter of willpower. If someone wants to stop badly enough, they will. If they don't, they won't. But that perspective leaves out something critical. Addiction is not just behavioral. It's biological, psychological, and deeply influenced by environment.
Over the past few decades, research has shifted how professionals understand and treat addiction. Instead of viewing it as a failure of discipline, it's now approached as a complex condition that affects brain function, emotional regulation, and decision-making processes. That shift has led to more effective, science-backed treatment methods that focus on long-term outcomes rather than short-term fixes.
If you or someone you know is struggling or in crisis, help is available.
Call or text 988 or chat at 988lifeline.org. To learn how to get support for mental health, drug or alcohol conditions, visit FindSupport.gov. If you are ready to locate a treatment facility or provider, visit FindTreatment.gov or call 800-662-HELP (4357).
U.S. veterans or service members in crisis can call 988 then press "1" for the Veterans Crisis Line, text 838255, or chat online.
The Suicide & Crisis Lifeline has a Spanish language line at 1-888-628-9454 (toll-free).
 Pexels[/caption]
The first day back at work after treatment isn't usually how movies show it. There's no triumphant montage. Mostly there's an inbox that's been ignored for thirty days, a few co-workers whose eyes you can't quite read, and a quiet anxiety about whether anyone is going to ask the questions you don't have rehearsed answers for.
The transition back to work is one of the highest-risk stretches in early recovery. Done well, it builds the structure that long-term sobriety depends on. Done poorly, it can unravel everything treatment just put together. Here's how to think about it before you walk back through the door.
Pexels[/caption]
The first day back at work after treatment isn't usually how movies show it. There's no triumphant montage. Mostly there's an inbox that's been ignored for thirty days, a few co-workers whose eyes you can't quite read, and a quiet anxiety about whether anyone is going to ask the questions you don't have rehearsed answers for.
The transition back to work is one of the highest-risk stretches in early recovery. Done well, it builds the structure that long-term sobriety depends on. Done poorly, it can unravel everything treatment just put together. Here's how to think about it before you walk back through the door.
The Question to Answer First: Are You Actually Ready?
Discharge from a treatment program isn't the same as readiness for work. They're related, but not identical. A useful self-check before scheduling your return:- Have you and your clinical team explicitly agreed on a return-to-work date?
- Do you have a written plan for handling cravings during the workday?
- Do you know how you'll manage the first work event involving alcohol?
- Have you identified at least one person you can contact during the day if things go sideways?
Declines and pronounced state-level disparities in tetrahydrocannabinol (THC) prescribing to Medicare patients
 Dr. Edward Liu[/caption]
MedicalResearch.com Interview with:
Edward Liu, MD
Geisinger College of Health Sciences
Scranton, PA 18509
Medicalresearch.com: What is the background for this study?
Response: Prescription drugs have high levels of uniformity that plant-based products cannot achieve. Given the liberalization of state-laws regarding medical marijuana1 over the past three-decades and increasing evidence of evidence of cannabis for conditions like chronic pain,2 we were interested in the use of the prescription formulation of delta(Δ)9-tetrahydrocannabinol (THC). A prior pharmacoepidemiology report found that prescription THC (dronabinol) to Medicaid patients decreased from 2016 to 2020. There were also pronounced state-level disparities in prescribing with a 130-fold difference when correcting for population between the highest and lowest states.
There was no research on this topic among Medicare patients. To address this gap, we obtained prescription numbers nationally and at a state level from 2014 to 2019 for Medicare Part D patients.
Dr. Edward Liu[/caption]
MedicalResearch.com Interview with:
Edward Liu, MD
Geisinger College of Health Sciences
Scranton, PA 18509
Medicalresearch.com: What is the background for this study?
Response: Prescription drugs have high levels of uniformity that plant-based products cannot achieve. Given the liberalization of state-laws regarding medical marijuana1 over the past three-decades and increasing evidence of evidence of cannabis for conditions like chronic pain,2 we were interested in the use of the prescription formulation of delta(Δ)9-tetrahydrocannabinol (THC). A prior pharmacoepidemiology report found that prescription THC (dronabinol) to Medicaid patients decreased from 2016 to 2020. There were also pronounced state-level disparities in prescribing with a 130-fold difference when correcting for population between the highest and lowest states.
There was no research on this topic among Medicare patients. To address this gap, we obtained prescription numbers nationally and at a state level from 2014 to 2019 for Medicare Part D patients.
The Pharmacokinetics of the Last Mile: Protecting Cannabinoid Integrity in 2026
 Source: IMAGE[/caption]
Source: IMAGE[/caption]
Editor's note: Cannabis and THCA/Hemp CBD products should have an active ingredient list on the container and a Certificate of Analysis (COA). Discuss your use of THC, cannabis, or CBD products with your health care provider. Dosing of cannabis products is variable, especially since they are not FDA regulated. Cannabis/CBD may interfere with other medications and should not be used in individuals with certain health conditions, including liver issues. CBD skin care products can be absorbed through the skin and have similar effects. Do not use cannabis products including edibles, drinks, and CBD if you are pregnant, nursing, or may become pregnant. Do not use cannabis products if driving or operating difficult or dangerous machinery. Children should not be exposed to cannabis or CBD products.
Whereas logistics professionals are more likely to concentrate on the purity and quality of laboratory extractions or cultivations, one of the most unstable parts of the medicinal substance's route to delivery — the final mile — may sometimes be neglected. The cannabis industry has turned to a pharmaceutical approach in 2026 to safeguard the chemical composition of the plant from exposure to damaging effects before reaching the end user.The Science of Thermal Degradation and Molecular Shifts
The main challenge is the heat issue, which is considered the major cause of irregularity among chemicals. Research results from the beginning of 2026 indicate that different temperatures during transportation can affect the composition of cannabis within three hours by 15%.How Harp Rehab’s Patient-Focused Approach Supports Lasting Recovery
 Photo by Lance Reis on Unsplash[/caption]
Photo by Lance Reis on Unsplash[/caption]
If you or someone you know is struggling or in crisis, help is available.
Call or text 988 or chat at 988lifeline.org. To learn how to get support for mental health, drug or alcohol conditions, visit FindSupport.gov. If you are ready to locate a treatment facility or provider, visit FindTreatment.gov or call 800-662-HELP (4357).
U.S. veterans or service members in crisis can call 988 then press "1" for the Veterans Crisis Line, text 838255, or chat online.
The Suicide & Crisis Lifeline has a Spanish language line at 1-888-628-9454 (toll-free).
 Unsplash image[/caption]
Unsplash image[/caption]
Editor's note: Cannabis and THCA/Hemp CBD products should have an active ingredient list on the container and a Certificate of Analysis (COA). Discuss your use of THC, cannabis, or CBD products with your health care provider. Dosing of cannabis products is variable, especially since they are not FDA regulated. Cannabis/CBD may interfere with other medications and should not be used in individuals with certain health conditions, including liver issues. CBD skin care products can be absorbed through the skin and have similar effects. Do not use cannabis products including edibles, drinks, and CBD if you are pregnant, nursing, or may become pregnant. Do not use cannabis products if driving or operating difficult or dangerous machinery. Children should not be exposed to cannabis or CBD products.
Cannabis research has always straddled a gray area. Popular takes are sometimes upended following a "groundbreaking" study. And yet, what we do know about its effects on the brain barely scratches the surface. Coincidentally, scientists are venturing into neurological territory and expanding their focus on brain function and connectivity. Harvard Medical School, for one, is pioneering studies utilizing neuroimaging techniques like functional MRI to determine how cannabis affects the mind.Researchers Found Why CBD Affects Anxiety Differently in Each Person
 SOURCE: IMAGE[/caption]
SOURCE: IMAGE[/caption]
Editor's note: Cannabis and THCA/Hemp CBD products should have an active ingredient list on the container and a Certificate of Analysis (COA). Discuss your use of THC, cannabis, or CBD products with your health care provider. Dosing of cannabis products is variable, especially since they are not FDA regulated. Cannabis/CBD may interfere with other medications and should not be used in individuals with certain health conditions, including liver issues. CBD skin care products can be absorbed through the skin and have similar effects. Do not use cannabis products including edibles, drinks, and CBD if you are pregnant, nursing, or may become pregnant. Do not use cannabis products if driving or operating difficult or dangerous machinery. Children should not be exposed to cannabis or CBD products.
A question that comes up constantly in cannabis research is one that patients have been asking for years: why does CBD ease anxiety in one person and make another feel worse? For a long time, the honest answer was that nobody fully knew. A landmark study out of McGill University changedthat, and the findings reveal something that most consumer guides on CBD have never properly explained.
The answer is not about product quality, dosage form, or brand. It comes down to how cannabis interacts with serotonin — and specifically why that interaction is not the same at every dose.How Healthcare Leaders Evaluate Rehab Programs That Actually Support Long Term Recovery Outcomes
 Unsplash image[/caption]
Unsplash image[/caption]
If you or someone you know is struggling or in crisis, help is available.
Call or text 988 or chat at 988lifeline.org. To learn how to get support for mental health, drug or alcohol conditions, visit FindSupport.gov. If you are ready to locate a treatment facility or provider, visit FindTreatment.gov or call 800-662-HELP (4357).
U.S. veterans or service members in crisis can call 988 then press "1" for the Veterans Crisis Line, text 838255, or chat online.
The Suicide & Crisis Lifeline has a Spanish language line at 1-888-628-9454 (toll-free).
Fentanyl addiction and overdose: addressing opioid use disorder through modern addiction treatment programs
 Fentanyl addiction and overdose rates are mounting public health challenges linked to opioid use disorder across the United States. Effective treatment programs for recovery are essential to address these concerns, especially as access to both in-person and virtual options improves. Renew Health Addiction Recovery Services delivers evidence-based care and supports individuals seeking help for substance abuse addiction throughout New Mexico.
Fentanyl is a potent synthetic opioid responsible for rising overdose deaths and severe complications among people with substance use disorder. Reaching effective recovery remains difficult for many due to barriers such as stigma, provider shortages, and the geographic spread of rural populations. Organizations like Renew Health Addiction Recovery Services are working to overcome these obstacles by offering accessible, evidence-based addiction care through various treatment options. Renew Health Addiction Recovery Services is a leading drug and alcohol addiction treatment center in New Mexico, providing in-person and online outpatient rehab, plus local clinics in Roswell, Alamogordo, and Clovis. Their programs address opioid, alcohol, methamphetamine, and cocaine addiction, offering medical detoxification, medication-assisted treatment (MAT), mental health services, and ongoing recovery support.
Fentanyl addiction and overdose rates are mounting public health challenges linked to opioid use disorder across the United States. Effective treatment programs for recovery are essential to address these concerns, especially as access to both in-person and virtual options improves. Renew Health Addiction Recovery Services delivers evidence-based care and supports individuals seeking help for substance abuse addiction throughout New Mexico.
Fentanyl is a potent synthetic opioid responsible for rising overdose deaths and severe complications among people with substance use disorder. Reaching effective recovery remains difficult for many due to barriers such as stigma, provider shortages, and the geographic spread of rural populations. Organizations like Renew Health Addiction Recovery Services are working to overcome these obstacles by offering accessible, evidence-based addiction care through various treatment options. Renew Health Addiction Recovery Services is a leading drug and alcohol addiction treatment center in New Mexico, providing in-person and online outpatient rehab, plus local clinics in Roswell, Alamogordo, and Clovis. Their programs address opioid, alcohol, methamphetamine, and cocaine addiction, offering medical detoxification, medication-assisted treatment (MAT), mental health services, and ongoing recovery support.
Johns Hopkins Study Finds Cannabis Use May Pose Greater Mental Health Risks in Adolescents than Adults
Our findings suggest that cannabis prevention efforts should prioritize youth and adolescents, education campaigns should emphasize age-related risks, and policy...
The Intersection of Mental Health andLong-Term Recovery Sustainability
 Image Source[/caption]
Image Source[/caption]
The Case for Neuro-Restorative Continuity in SUD Treatment
 p[/caption]
In the contemporary landscape of addiction medicine, the primary clinical challenge has shifted. While the management of acute withdrawal—once a high-risk hurdle—has become a relatively standardized pharmacological procedure, the true "research frontier" lies in the post-stabilization window. This is the critical period where neuroplasticity can either facilitate a return to homeostasis or solidify the neural pathways of relapse.
The persistently high rates of recidivism in Substance Use Disorder (SUD) are frequently a byproduct of what researchers call "fragmented care." This occurs when a patient is medically detoxified in an isolated setting and then prematurely transitioned into a low-intensity environment before the brain’s reward circuitry has had the necessary time to recalibrate. This is why the conversation among clinical researchers is shifting toward the Integrated Longitudinal Model. In this context, a premier San Diego rehabilitation center serves as more than just a residential facility; it functions as a controlled, enriched environment for the phased restoration of the prefrontal cortex.
p[/caption]
In the contemporary landscape of addiction medicine, the primary clinical challenge has shifted. While the management of acute withdrawal—once a high-risk hurdle—has become a relatively standardized pharmacological procedure, the true "research frontier" lies in the post-stabilization window. This is the critical period where neuroplasticity can either facilitate a return to homeostasis or solidify the neural pathways of relapse.
The persistently high rates of recidivism in Substance Use Disorder (SUD) are frequently a byproduct of what researchers call "fragmented care." This occurs when a patient is medically detoxified in an isolated setting and then prematurely transitioned into a low-intensity environment before the brain’s reward circuitry has had the necessary time to recalibrate. This is why the conversation among clinical researchers is shifting toward the Integrated Longitudinal Model. In this context, a premier San Diego rehabilitation center serves as more than just a residential facility; it functions as a controlled, enriched environment for the phased restoration of the prefrontal cortex.
Why Funding Stability Is a Constant Concern in Behavioral Health and Addiction Care
Behavioral healthcare has long faced tight margins, uneven reimbursement, and heavy reliance on grant funding for prevention, early intervention, recovery...
The Behavioral Health Workforce Shortage Is Still Shaping Addiction and Mental Health Care
 Freepix[/caption]
Freepix[/caption]
Why staffing remains one of the field’s biggest challenges
The behavioral health workforce shortage is not a background issue. It is one of the defining pressures on the mental health and addiction treatment system. HRSA’s State of the Behavioral Health Workforce, 2025 brief states that the field is projected to face substantial shortages across addiction counselors, mental health counselors, psychologists, psychiatrists, and social workers, and notes that 40% of the U.S. population lives in a Mental Health Professional Shortage Area. That kind of shortage has implications far beyond staffing levels. It affects access, wait times, burnout, care continuity, and the ability of organizations to respond to rising demand. Freepix[/caption]
Recovery from addiction is a deeply personal journey, often filled with both breakthroughs and challenges. While completing a detox program or residential treatment is a major milestone, the transition back into everyday life can be one of the most vulnerable stages of recovery. This is where sober living homes play a crucial role. These supportive environments provide individuals with the structure, accountability, and community they need to maintain sobriety and build a stable, fulfilling life.
Freepix[/caption]
Recovery from addiction is a deeply personal journey, often filled with both breakthroughs and challenges. While completing a detox program or residential treatment is a major milestone, the transition back into everyday life can be one of the most vulnerable stages of recovery. This is where sober living homes play a crucial role. These supportive environments provide individuals with the structure, accountability, and community they need to maintain sobriety and build a stable, fulfilling life.
What Are Sober Living Homes?
Sober living homes are residential environments designed for individuals who are committed to recovery from substance use disorders. Unlike inpatient treatment centers, these homes offer more independence while still maintaining guidelines that promote sobriety. Residents are typically required to follow house rules, such as remaining drug- and alcohol-free, attending recovery meetings, contributing to household responsibilities, and sometimes participating in regular drug testing. These homes act as a bridge between intensive treatment and fully independent living, allowing individuals to gradually reintegrate into society while still receiving support.Codependency Treatment Centers: How Specialized Support Can Help Break Unhealthy Relationship Patterns
 Freepix image[/caption]
Freepix image[/caption]
Why codependency is an important issue in mental health and recovery
Codependency is often discussed in the context of relationships affected by addiction, but it can also show up in many other settings. It may involve unhealthy emotional reliance, difficulty setting boundaries, people-pleasing, fear of abandonment, or a pattern of prioritizing someone else’s needs at the expense of personal well-being. Over time, these patterns can affect mental health, self-worth, family relationships, and the ability to function in a healthy and balanced way. That is why codependency treatment centers can be an important resource. For some individuals, codependency is not just a relationship issue. It is a deeper pattern that shapes decision-making, emotional stability, and the way connection is experienced. Treatment can help people understand those patterns and begin building healthier ways of relating to others and to themselves. For those beginning to explore support, learning more about codependency treatment centers can be a helpful first step. Meagan Robichaud, Ph.D.[/caption]
Meagan Robichaud, PhD, MPH
Post-Doctoral Associate
Center for Rapid Surveillance of Tobacco
Rutgers Institute for Nicotine & Tobacco Studies
MedicalResearch.com: What is delta-8 THC?
Response: To understand delta-8 THC, it’s first important to understand the primary components of cannabis: THC (tetrahydrocannabinol) and CBD (cannabidiol). THC—typically referring to delta-9 THC—is the primary intoxicating substance in cannabis—it’s what makes consumers feel “high.” CBD is also abundant in cannabis but is non-intoxicating.
Delta-8 THC is an isomer of delta-9 THC—meaning it has the same chemical formula as delta-9 THC but with a slightly different arrangement of atoms. While early research suggest that delta-8 THC is less potent than delta-9 THC, delta-8 THC is still an intoxicating substance. Delta-8 THC naturally exists in very small amounts in cannabis plants but can be synthesized from CBD.
Meagan Robichaud, Ph.D.[/caption]
Meagan Robichaud, PhD, MPH
Post-Doctoral Associate
Center for Rapid Surveillance of Tobacco
Rutgers Institute for Nicotine & Tobacco Studies
MedicalResearch.com: What is delta-8 THC?
Response: To understand delta-8 THC, it’s first important to understand the primary components of cannabis: THC (tetrahydrocannabinol) and CBD (cannabidiol). THC—typically referring to delta-9 THC—is the primary intoxicating substance in cannabis—it’s what makes consumers feel “high.” CBD is also abundant in cannabis but is non-intoxicating.
Delta-8 THC is an isomer of delta-9 THC—meaning it has the same chemical formula as delta-9 THC but with a slightly different arrangement of atoms. While early research suggest that delta-8 THC is less potent than delta-9 THC, delta-8 THC is still an intoxicating substance. Delta-8 THC naturally exists in very small amounts in cannabis plants but can be synthesized from CBD.Altitude Recovery For Rehab Near Ventura And North LA That Accepts Insurance

 Searching for addiction treatment in Southern California can quickly become overwhelming. Families often begin with one practical question before anything else. Is there a high quality rehab near Ventura or Thousand Oaks that actually accepts insurance and helps navigate the process. The answer increasingly leads people toward Camarillo, where Altitude Recovery has built a reputation for offering residential care that balances clinical structure with real world accessibility.
The conversation around treatment has shifted over the past decade. People want privacy, evidence based therapy, and a program that feels supportive rather than institutional. At the same time, insurance coverage matters. Treatment becomes far more attainable when a center actively works with insurance carriers and helps families understand their options. Altitude Recovery sits at the intersection of those needs, offering a residential program near Ventura County that combines professional treatment with insurance guidance.
Searching for addiction treatment in Southern California can quickly become overwhelming. Families often begin with one practical question before anything else. Is there a high quality rehab near Ventura or Thousand Oaks that actually accepts insurance and helps navigate the process. The answer increasingly leads people toward Camarillo, where Altitude Recovery has built a reputation for offering residential care that balances clinical structure with real world accessibility.
The conversation around treatment has shifted over the past decade. People want privacy, evidence based therapy, and a program that feels supportive rather than institutional. At the same time, insurance coverage matters. Treatment becomes far more attainable when a center actively works with insurance carriers and helps families understand their options. Altitude Recovery sits at the intersection of those needs, offering a residential program near Ventura County that combines professional treatment with insurance guidance.
WSU Study: Avoid Cannabis When Relying on Memory is Important
 Dr. Cutttler, Ph.D.[/caption]
Carrie Cuttler, Ph.D.
The Health & Cognition (THC) Lab
Associate Professor
Director, Experimental Psychology Doctoral Program
Co-Director, Cannabis Research Center (CRC)
Department of Psychology
Washington State University
MedicalResearch.com: What is the background for this study?
Response: One of the most well-documented effects of acute cannabis intoxication is impairment in memory. However, memory is not a single process. It is a complex system made up of multiple distinct subsystems that rely on different neural mechanisms and support different types of remembering.
Most prior research examining the acute effects of cannabis in humans has focused on a relatively narrow set of memory tests—primarily verbal memory tasks, which involve recalling lists of words, and working memory tasks, which require temporarily holding and manipulating information in consciousness.
Far fewer studies have examined how cannabis affects other types of memory that are more relevant to everyday life. These include temporal order memory (remembering the order in which events occurred), prospective memory (remembering to perform tasks in the future), source memory (remembering where information came from), false memory (recalling information that was never presented), and episodic content memory (recalling personally experienced events).
To address this gap, we conducted a randomized, double-blind, placebo-controlled study examining the acute effects of cannabis across multiple memory domains. In total, 120 participants were randomly assigned to vaporize either a placebo, a moderate dose of cannabis (20 mg THC), or a high dose of cannabis (40 mg THC).
Dr. Cutttler, Ph.D.[/caption]
Carrie Cuttler, Ph.D.
The Health & Cognition (THC) Lab
Associate Professor
Director, Experimental Psychology Doctoral Program
Co-Director, Cannabis Research Center (CRC)
Department of Psychology
Washington State University
MedicalResearch.com: What is the background for this study?
Response: One of the most well-documented effects of acute cannabis intoxication is impairment in memory. However, memory is not a single process. It is a complex system made up of multiple distinct subsystems that rely on different neural mechanisms and support different types of remembering.
Most prior research examining the acute effects of cannabis in humans has focused on a relatively narrow set of memory tests—primarily verbal memory tasks, which involve recalling lists of words, and working memory tasks, which require temporarily holding and manipulating information in consciousness.
Far fewer studies have examined how cannabis affects other types of memory that are more relevant to everyday life. These include temporal order memory (remembering the order in which events occurred), prospective memory (remembering to perform tasks in the future), source memory (remembering where information came from), false memory (recalling information that was never presented), and episodic content memory (recalling personally experienced events).
To address this gap, we conducted a randomized, double-blind, placebo-controlled study examining the acute effects of cannabis across multiple memory domains. In total, 120 participants were randomly assigned to vaporize either a placebo, a moderate dose of cannabis (20 mg THC), or a high dose of cannabis (40 mg THC).
How People Rebuild Their Lives After Difficult Periods
 Freepix[/caption]
Life can sometimes throw challenges that feel insurmountable. Whether it is the loss of a loved one, a period of severe illness, a financial setback, or struggles with addiction, these difficult times can leave people feeling lost, overwhelmed, and uncertain about the future. However, many individuals find ways to rebuild their lives, often emerging stronger and more resilient than before. Understanding the steps people take to recover and grow can offer hope and guidance to those navigating their own hardships.
Acknowledging the Pain
The first step in rebuilding life after a difficult period is acknowledging the pain. Denying or minimizing struggles can prolong the healing process. By confronting emotions head-on, people begin to understand the impact of their experiences and take ownership of their healing journey. This can involve seeking support from friends, family, or professional counsellors who can offer a safe space to express feelings without judgment. Journaling, art, or other forms of creative expression can also provide an outlet for processing complex emotions.
Freepix[/caption]
Life can sometimes throw challenges that feel insurmountable. Whether it is the loss of a loved one, a period of severe illness, a financial setback, or struggles with addiction, these difficult times can leave people feeling lost, overwhelmed, and uncertain about the future. However, many individuals find ways to rebuild their lives, often emerging stronger and more resilient than before. Understanding the steps people take to recover and grow can offer hope and guidance to those navigating their own hardships.
Acknowledging the Pain
The first step in rebuilding life after a difficult period is acknowledging the pain. Denying or minimizing struggles can prolong the healing process. By confronting emotions head-on, people begin to understand the impact of their experiences and take ownership of their healing journey. This can involve seeking support from friends, family, or professional counsellors who can offer a safe space to express feelings without judgment. Journaling, art, or other forms of creative expression can also provide an outlet for processing complex emotions.
 Freepix[/caption]
Recovering from addiction is a journey that challenges every part of a person’s life, physically, emotionally, and socially. While determination and personal effort are crucial, no one needs to face this journey alone. Support systems play a vital role in helping individuals overcome addiction, offering guidance, encouragement, and stability during what can be an overwhelming process.
Emotional Support: The Backbone of Recovery
One of the most significant aspects of a support system is emotional encouragement. Friends, family, or peers who understand the struggles of addiction can offer empathy, reassurance, and hope. Knowing that someone believes in your ability to overcome addiction can reduce feelings of isolation and despair. Emotional support helps individuals navigate the inevitable setbacks of recovery with resilience rather than discouragement.
Peer support groups, such as 12-step programs, also play a vital role. Being surrounded by others who have faced similar challenges fosters a sense of belonging. Sharing experiences, struggles, and victories with peers reinforces that recovery is attainable and provides practical strategies to overcome common obstacles.
Freepix[/caption]
Recovering from addiction is a journey that challenges every part of a person’s life, physically, emotionally, and socially. While determination and personal effort are crucial, no one needs to face this journey alone. Support systems play a vital role in helping individuals overcome addiction, offering guidance, encouragement, and stability during what can be an overwhelming process.
Emotional Support: The Backbone of Recovery
One of the most significant aspects of a support system is emotional encouragement. Friends, family, or peers who understand the struggles of addiction can offer empathy, reassurance, and hope. Knowing that someone believes in your ability to overcome addiction can reduce feelings of isolation and despair. Emotional support helps individuals navigate the inevitable setbacks of recovery with resilience rather than discouragement.
Peer support groups, such as 12-step programs, also play a vital role. Being surrounded by others who have faced similar challenges fosters a sense of belonging. Sharing experiences, struggles, and victories with peers reinforces that recovery is attainable and provides practical strategies to overcome common obstacles.






