[caption id="attachment_70070" align="aligncenter" width="500"]
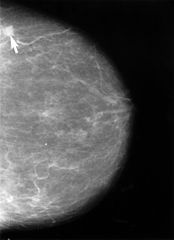
 Photo by Towfiqu barbhuiya
Photo by Towfiqu barbhuiya[/caption]
When it comes to clinical trials, the accuracy and reliability of data are paramount. Among the many types of data collected, imaging data plays a crucial role, particularly in fields such as oncology, cardiology, and neurology. However, managing and interpreting this data can be complex, and errors or inconsistencies can significantly impact trial outcomes. This is where expert image review and analysis come into play, offering a pathway to enhanced accuracy, consistency, and ultimately, improved trial outcomes.
The Role of Imaging in Clinical Trials
Imaging techniques such as MRI, CT scans, and
PET scans provide critical insights into disease progression, treatment efficacy, and patient responses. These images help researchers visualize changes within the body that might not be evident through other data forms. However, the sheer volume and complexity of imaging data in clinical trials present challenges, including variability in image quality, differences in acquisition protocols, and subjective interpretation by different readers.
Why Expert Image Review Matters
Expert image review refers to the process where trained radiologists or imaging specialists carefully examine trial images to ensure they meet the highest standards of quality and consistency. This step helps to:
- Reduce Variability: Different sites and operators might acquire images differently. Expert reviewers ensure that images are standardized and comparable across sites.
- Improve Accuracy: Trained specialists are more adept at identifying subtle changes or abnormalities, reducing the risk of false positives or negatives.
- Ensure Compliance: Adhering to trial protocols and regulatory requirements is critical. Expert reviewers help maintain protocol compliance in image acquisition and analysis.
These factors combine to produce more reliable data, which translates into stronger evidence when evaluating a treatment’s efficacy or safety.













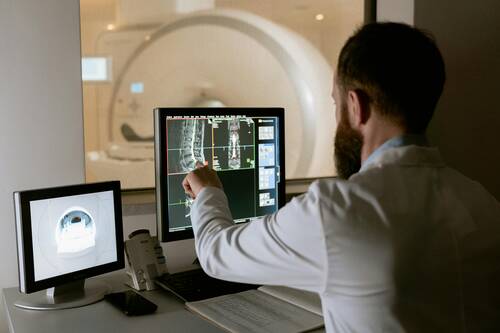
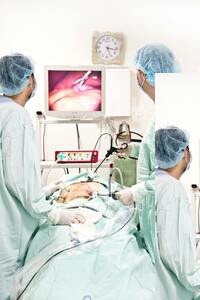







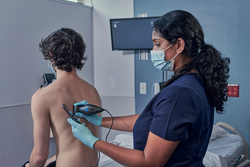
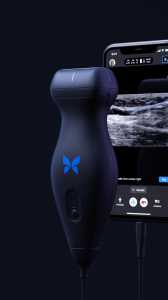 Response: Point-of-care ultrasound is one of the most significant advances in bedside patient care, and its use is expanding across nearly all fields of medicine. In order to best prepare medical students for residency and beyond, it is imperative to begin POCUS training as early as possible. At the Lewis Katz School of Medicine at Temple University, we introduced POCUS education over a decade ago and have expanded it since then.
By providing each student with a Butterfly iQ device, we can augment our curriculum significantly. In addition to our robust pre-clinical sessions, now we will expand into the clinical years highlighting the utility of POCUS with actual patients.
This gift was made possible by the incredible generosity of Dr. Ronald Salvitti, MD ’63.
Response: Point-of-care ultrasound is one of the most significant advances in bedside patient care, and its use is expanding across nearly all fields of medicine. In order to best prepare medical students for residency and beyond, it is imperative to begin POCUS training as early as possible. At the Lewis Katz School of Medicine at Temple University, we introduced POCUS education over a decade ago and have expanded it since then.
By providing each student with a Butterfly iQ device, we can augment our curriculum significantly. In addition to our robust pre-clinical sessions, now we will expand into the clinical years highlighting the utility of POCUS with actual patients.
This gift was made possible by the incredible generosity of Dr. Ronald Salvitti, MD ’63. 
 Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.
Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.

 Dr. Spampinato[/caption]
Maria Vittoria Spampinato, MD
Neuroradiology Division Director
Department of Radiology and Radiological Science
Medical University of South Carolina
Charleston, SC 29425-3230
MedicalResearch.com: What is the background for this study? What are the main findings?
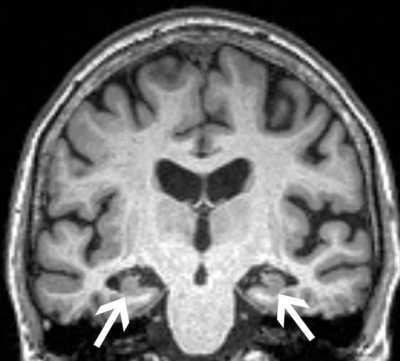
Response: Alzheimer’s disease (AD) represents a major public health crisis worldwide. More than 5 million people currently have AD in the United States. AD is a slowly progressing neurodegenerative brain disorder with a long preclinical phase. Many people with AD first suffer from mild cognitive impairment (MCI), a decline in cognitive abilities like memory and thinking skills that is greater than that associated with normal aging. A person with MCI is at an increased risk of developing AD or another dementia, although some individuals with MCI remain cognitively stable or improve.
Anxiety is frequently observed in individuals with MCI. The reported prevalence of anxiety in MCI patients varies between 10 and 50%. In this study we evaluated a cohort of 339 individuals with MCI participating in the Alzheimer’s Disease Neuroimaging Initiative study (ADNI2). During the five years of study participation, 72 patients experienced cognitive decline and were diagnosed with AD. We did not find difference in age, gender and education among patients with and without AD conversion. Patients who progressed had greater atrophy of the hippocampi and entorhinal cortex on their MRI scan, as expected (hippocampal atrophy is often used as a marker of neurodegeneration in AD), as well as greater prevalence of APOE4 is the strongest known genetic risk factor for AD. Patients who progressed to Alzheimer’s disease also had greater severity of anxiety during the study, as measured using the Neuropsychiatric Inventory-Questionnaire. Next we determined the effect of the MRI findings (hippocampal and entorhinal cortex atrophy), of the genetic risk factor (APOE4) and of the severity of anxiety on the time to progression to AD. We found that higher levels of anxiety were associated with faster progression from MCI to AD, independently of whether they had a genetic risk factor for Alzheimer’s disease or brain volume loss. We still need to understand better the association between anxiety disorders and cognitive decline. We do not know whether increased levels of anxiety are a consequence of cognitive decline or if anxiety exacerbates to cognitive decline. If we were able to find in the future that anxiety is actually contributing to cognitive decline, then we should more aggressively screen for anxiety disorders in the elderly population.
Dr. Spampinato[/caption]
Maria Vittoria Spampinato, MD
Neuroradiology Division Director
Department of Radiology and Radiological Science
Medical University of South Carolina
Charleston, SC 29425-3230
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Alzheimer’s disease (AD) represents a major public health crisis worldwide. More than 5 million people currently have AD in the United States. AD is a slowly progressing neurodegenerative brain disorder with a long preclinical phase. Many people with AD first suffer from mild cognitive impairment (MCI), a decline in cognitive abilities like memory and thinking skills that is greater than that associated with normal aging. A person with MCI is at an increased risk of developing AD or another dementia, although some individuals with MCI remain cognitively stable or improve.
Anxiety is frequently observed in individuals with MCI. The reported prevalence of anxiety in MCI patients varies between 10 and 50%. In this study we evaluated a cohort of 339 individuals with MCI participating in the Alzheimer’s Disease Neuroimaging Initiative study (ADNI2). During the five years of study participation, 72 patients experienced cognitive decline and were diagnosed with AD. We did not find difference in age, gender and education among patients with and without AD conversion. Patients who progressed had greater atrophy of the hippocampi and entorhinal cortex on their MRI scan, as expected (hippocampal atrophy is often used as a marker of neurodegeneration in AD), as well as greater prevalence of APOE4 is the strongest known genetic risk factor for AD. Patients who progressed to Alzheimer’s disease also had greater severity of anxiety during the study, as measured using the Neuropsychiatric Inventory-Questionnaire. Next we determined the effect of the MRI findings (hippocampal and entorhinal cortex atrophy), of the genetic risk factor (APOE4) and of the severity of anxiety on the time to progression to AD. We found that higher levels of anxiety were associated with faster progression from MCI to AD, independently of whether they had a genetic risk factor for Alzheimer’s disease or brain volume loss. We still need to understand better the association between anxiety disorders and cognitive decline. We do not know whether increased levels of anxiety are a consequence of cognitive decline or if anxiety exacerbates to cognitive decline. If we were able to find in the future that anxiety is actually contributing to cognitive decline, then we should more aggressively screen for anxiety disorders in the elderly population.