MedicalResearch.com Interview with:
[caption id="attachment_49973" align="alignleft" width="163"]

Dr. Nemesure[/caption]
Barbara Nemesure, PhD
Professor, Department of Family, Population and Preventive Medicine
Division Head, Epidemiology and Biostatistics
Director, Cancer Prevention and Control Program
Director, Lung Cancer Program, Stony Brook Cancer Center
Renaissance School of Medicine
Stony Brook University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lung cancer is the most common cause of cancer death, claiming the lives of more than 150,000 people in the United States each year. While lung nodules are not uncommon, it has remained a challenge to differentiate those that will progress to cancer and those that will remain benign. Although numerous risk prediction models for lung cancer have been developed over the past 2 decades, the majority have been based on retrospective analyses or high risk groups with a strong history of tobacco use. To date, there have been a limited number of large-scale, prospective studies evaluating risk that a nodule will convert to cancer in the general population.
This investigation aimed to construct a population-based risk prediction model of incident lung cancer for patients found to have a lung nodule on initial CT scan. The derived model was determined to have high accuracy for predicting nodule progression to cancer and identified a combination of clinical and radiologic predictors including age, smoking history (pack-years), a personal history of cancer, the presence of chronic obstructive pulmonary disease (COPD), and nodule features such as size, presence of spiculation and ground glass opacity type.
When compared to patients in the low risk category, those defined as high risk had more than 14 times the risk of developing lung cancer. Quantification of reliable risk scores has high clinical utility, enabling physicians to better stratify treatment plans for their patients.
 Dr. Kooraki[/caption]
Soheil Kooraki MSR MS, MD
on behalf of Dr. Ali Gholamrezanezhad MD and co-authors
Department of Radiological Sciences,
David Geffen School of Medicine, University of California at Los Angeles
Los Angeles, California
MedicalResearch.com: What is the background for this study? What are the main findings?
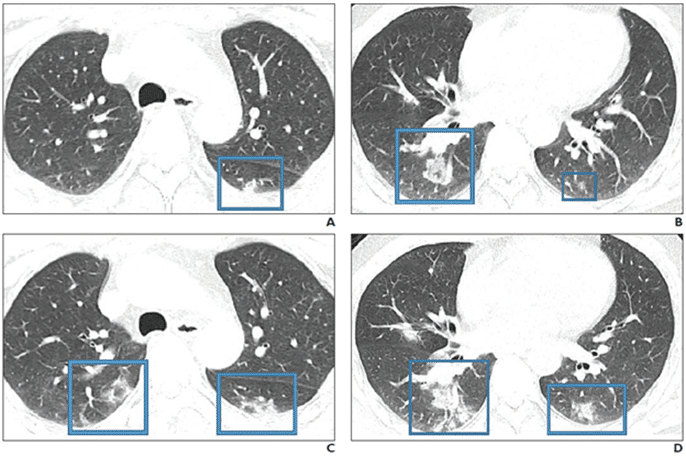
Response: COVID19 is a novel strain of the coronavirus family causing pneumonia. Two similar strains were discovered in 2003 and 2012 to cause the so-called SARS and MERS outbreaks, respectively. Radiologists need to be prepared for the escalating incidence of COVID-19. We reviewed the literature to extract the epidemiologic and imaging features of SARS and MERS in comparison with known imaging features of COVID-19 pneumonia to have a better understanding of the imaging features of the COVID19 pneumonia in acute and post-recovery stages.
Dr. Kooraki[/caption]
Soheil Kooraki MSR MS, MD
on behalf of Dr. Ali Gholamrezanezhad MD and co-authors
Department of Radiological Sciences,
David Geffen School of Medicine, University of California at Los Angeles
Los Angeles, California
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: COVID19 is a novel strain of the coronavirus family causing pneumonia. Two similar strains were discovered in 2003 and 2012 to cause the so-called SARS and MERS outbreaks, respectively. Radiologists need to be prepared for the escalating incidence of COVID-19. We reviewed the literature to extract the epidemiologic and imaging features of SARS and MERS in comparison with known imaging features of COVID-19 pneumonia to have a better understanding of the imaging features of the COVID19 pneumonia in acute and post-recovery stages.






















 Dr. Callaghan[/caption]
Dr. Callaghan[/caption]




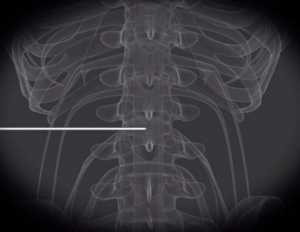 Probe being applied to nerve root.
Probe being applied to nerve root.