AI and HealthCare, Author Interviews, Brain Cancer - Brain Tumors, Lancet, Mammograms / 30.01.2026
AI-Supported Mammography Screening Showed Consistently More Favourable outcomes Compared with Standard Screening
MedicalResearch.com Interview with:
[caption id="attachment_72182" align="alignleft" width="200"] Dr. Lång[/caption]
Kristina Lång MD PhD
Associate professor, Diagnostic Radiology
Translational Medicine, Lund University
Senior consultant, Unilabs Mammography Unit
Skåne University Hospital, Malmö, Sweden
MedicalResearch.com: What is the background for this study?
Response: Prior to the start of the trial, several retrospective studies had shown that AI could discriminate between screening mammograms at low and high risk of cancer, with performance comparable to that of average breast radiologists. These findings suggested a potential to improve both the efficiency and sensitivity of mammography screening. This motivated us to design and evaluate an AI-supported screening procedure in a randomised controlled trial. The MASAI trial was among the first prospective studies in this field and, to date, remains the only randomised trial with reported results on the use of AI in breast cancer screening.
In European breast cancer screening programmes, every mammogram is usually read by two radiologists, so called double reading, to ensure a high sensitivity. In the MASAI trial we compared AI-supported mammography screening to standard double reading without AI. I
n the AI-supported approach, mammograms identified as low-risk by the AI were read by a single radiologist, while high-risk mammograms underwent double reading, with AI providing additional detection support.
Dr. Lång[/caption]
Kristina Lång MD PhD
Associate professor, Diagnostic Radiology
Translational Medicine, Lund University
Senior consultant, Unilabs Mammography Unit
Skåne University Hospital, Malmö, Sweden
MedicalResearch.com: What is the background for this study?
Response: Prior to the start of the trial, several retrospective studies had shown that AI could discriminate between screening mammograms at low and high risk of cancer, with performance comparable to that of average breast radiologists. These findings suggested a potential to improve both the efficiency and sensitivity of mammography screening. This motivated us to design and evaluate an AI-supported screening procedure in a randomised controlled trial. The MASAI trial was among the first prospective studies in this field and, to date, remains the only randomised trial with reported results on the use of AI in breast cancer screening.
In European breast cancer screening programmes, every mammogram is usually read by two radiologists, so called double reading, to ensure a high sensitivity. In the MASAI trial we compared AI-supported mammography screening to standard double reading without AI. I
n the AI-supported approach, mammograms identified as low-risk by the AI were read by a single radiologist, while high-risk mammograms underwent double reading, with AI providing additional detection support.
 Dr. Lång[/caption]
Kristina Lång MD PhD
Associate professor, Diagnostic Radiology
Translational Medicine, Lund University
Senior consultant, Unilabs Mammography Unit
Skåne University Hospital, Malmö, Sweden
MedicalResearch.com: What is the background for this study?
Response: Prior to the start of the trial, several retrospective studies had shown that AI could discriminate between screening mammograms at low and high risk of cancer, with performance comparable to that of average breast radiologists. These findings suggested a potential to improve both the efficiency and sensitivity of mammography screening. This motivated us to design and evaluate an AI-supported screening procedure in a randomised controlled trial. The MASAI trial was among the first prospective studies in this field and, to date, remains the only randomised trial with reported results on the use of AI in breast cancer screening.
In European breast cancer screening programmes, every mammogram is usually read by two radiologists, so called double reading, to ensure a high sensitivity. In the MASAI trial we compared AI-supported mammography screening to standard double reading without AI. I
n the AI-supported approach, mammograms identified as low-risk by the AI were read by a single radiologist, while high-risk mammograms underwent double reading, with AI providing additional detection support.
Dr. Lång[/caption]
Kristina Lång MD PhD
Associate professor, Diagnostic Radiology
Translational Medicine, Lund University
Senior consultant, Unilabs Mammography Unit
Skåne University Hospital, Malmö, Sweden
MedicalResearch.com: What is the background for this study?
Response: Prior to the start of the trial, several retrospective studies had shown that AI could discriminate between screening mammograms at low and high risk of cancer, with performance comparable to that of average breast radiologists. These findings suggested a potential to improve both the efficiency and sensitivity of mammography screening. This motivated us to design and evaluate an AI-supported screening procedure in a randomised controlled trial. The MASAI trial was among the first prospective studies in this field and, to date, remains the only randomised trial with reported results on the use of AI in breast cancer screening.
In European breast cancer screening programmes, every mammogram is usually read by two radiologists, so called double reading, to ensure a high sensitivity. In the MASAI trial we compared AI-supported mammography screening to standard double reading without AI. I
n the AI-supported approach, mammograms identified as low-risk by the AI were read by a single radiologist, while high-risk mammograms underwent double reading, with AI providing additional detection support.





















 Dr. Taylor-Phillips[/caption]
Dr Sian Taylor-Phillips PhD
Assistant Professor of Screening and Test Evaluation
Division of Health Sciences
Warwick Medical School
University of Warwick
Coventry
MedicalResearch.com: What is the background for this study?
Dr Taylor-Phillips : Psychologists have been investigating a phenomenon of a drop in performance with time on a task called ‘the vigilance decrement’ since World War 2. In those days radar operators searched for enemy aircraft and submarines (appearing as little dots of light on a radar screen). People thought that the ability to spot the dots might go down after too much time spent on the task. Many psychology experiments have found a vigilance decrement, but most of this research has not been in a real world setting.
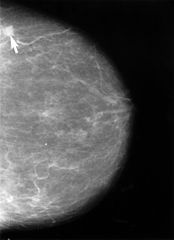
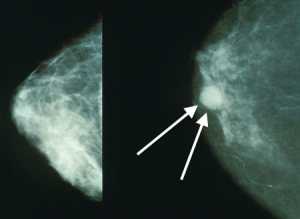
In this research we wanted to know whether there was a drop in performance with time on a task for breast screening readers looking at breast x-rays for signs of cancer. (Breast x-rays or mammograms show lots of overlapping tissue and cancers can be quite difficult to spot). This was a real-world randomised controlled study in UK clinical practice.
In the UK NHS Breast Screening Programme two readers examine each woman’s breast x-rays separately for signs of cancer. They look at batches of around 35 women’s x-rays. At the moment both readers look at the x-rays in the same order as each another, so if they both experience a drop in performance, it will happen at the same time. We tested a really simple idea of reversing the batch order for one of the readers, so that if they have a low ebb of performance it happens when they are looking at different women’s breast x-rays.
Dr. Taylor-Phillips[/caption]
Dr Sian Taylor-Phillips PhD
Assistant Professor of Screening and Test Evaluation
Division of Health Sciences
Warwick Medical School
University of Warwick
Coventry
MedicalResearch.com: What is the background for this study?
Dr Taylor-Phillips : Psychologists have been investigating a phenomenon of a drop in performance with time on a task called ‘the vigilance decrement’ since World War 2. In those days radar operators searched for enemy aircraft and submarines (appearing as little dots of light on a radar screen). People thought that the ability to spot the dots might go down after too much time spent on the task. Many psychology experiments have found a vigilance decrement, but most of this research has not been in a real world setting.
In this research we wanted to know whether there was a drop in performance with time on a task for breast screening readers looking at breast x-rays for signs of cancer. (Breast x-rays or mammograms show lots of overlapping tissue and cancers can be quite difficult to spot). This was a real-world randomised controlled study in UK clinical practice.
In the UK NHS Breast Screening Programme two readers examine each woman’s breast x-rays separately for signs of cancer. They look at batches of around 35 women’s x-rays. At the moment both readers look at the x-rays in the same order as each another, so if they both experience a drop in performance, it will happen at the same time. We tested a really simple idea of reversing the batch order for one of the readers, so that if they have a low ebb of performance it happens when they are looking at different women’s breast x-rays.
 Dr. Stamatia Destounis[/caption]
Stamatia Destounis, MD, FSBI, FACR
Elizabeth Wende Breast Care, LLC,
Clinical Professor of Imaging Sciences
University of Rochester
School of Medicine and Dentistry
Rochester NY 14620
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Destounis: Identification of women who have an increased risk of breast cancer is important, as they are often eligible for additional screening methods, such as breast MRI. One criterion for eligibility for screening breast MRI is >20% lifetime risk of breast cancer, as determined by risk assessment models through genetic counseling.
At my facility, we have incorporated a genetics program. Through the program we are flagging and identifying a large volume of patients who are potentially eligible for additional services. This study was conducted to determine the value of screening MRI in the patient subgroup who have undergone genetic counseling at my facility. In this group we found 50% of patients who were referred for counseling were also recommended to have screening MRI. However, only 21.3% of those recommended actually pursued the exam. Of those patients who did have a screening MRI, 4 were diagnosed with breast cancer, all of which were invasive and node negative. We ultimately had a 10% biopsy rate and 50% cancer detection rate in this subgroup.
Dr. Stamatia Destounis[/caption]
Stamatia Destounis, MD, FSBI, FACR
Elizabeth Wende Breast Care, LLC,
Clinical Professor of Imaging Sciences
University of Rochester
School of Medicine and Dentistry
Rochester NY 14620
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Destounis: Identification of women who have an increased risk of breast cancer is important, as they are often eligible for additional screening methods, such as breast MRI. One criterion for eligibility for screening breast MRI is >20% lifetime risk of breast cancer, as determined by risk assessment models through genetic counseling.
At my facility, we have incorporated a genetics program. Through the program we are flagging and identifying a large volume of patients who are potentially eligible for additional services. This study was conducted to determine the value of screening MRI in the patient subgroup who have undergone genetic counseling at my facility. In this group we found 50% of patients who were referred for counseling were also recommended to have screening MRI. However, only 21.3% of those recommended actually pursued the exam. Of those patients who did have a screening MRI, 4 were diagnosed with breast cancer, all of which were invasive and node negative. We ultimately had a 10% biopsy rate and 50% cancer detection rate in this subgroup.
 Dr. Elizabeth Rafferty[/caption]
Elizabeth A. Rafferty, MD
Department of Radiology,
Massachusetts General Hospital, Boston
Now with L&M Radiology, West Acton,
Massachusetts
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Rafferty: Breast tomosynthesis has been approved for mammographic screening in the United States for just over 5 years, and many single center studies have demonstrated its improved performance for screening outcomes over digital mammography alone. Our previously published multi-center analysis, (JAMA 2014;311(24), the largest study on this topic to date, demonstrated significantly improved cancer detection and reduced recall rates for women undergoing tomosynthesis compared with digital mammography alone. In the current issue of JAMA we evaluate the differential screening performance after implementation of breast tomosynthesis as a function of breast density.
While tomosynthesis continues to be increasingly available, questions remained about which women should be imaged with this technique. In particular, does this technology offer additional benefit for all women, or only for women with dense breasts. The size of the database compiled by the centers participating in this study allowed us to evaluate this important question.
The most critical finding of our study was that the use of tomosynthesis for breast cancer screening significantly improved invasive cancer detection rates while simultaneously significantly reducing recall rates both for women with dense and non-dense breast tissue. Having said that, the magnitude of the benefit was largest for women with heterogeneously dense breast tissue; for this population, tomosynthesis increased the detection of invasive cancers by 50% while simultaneously reducing the recall rate by 14%.
Dr. Elizabeth Rafferty[/caption]
Elizabeth A. Rafferty, MD
Department of Radiology,
Massachusetts General Hospital, Boston
Now with L&M Radiology, West Acton,
Massachusetts
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Rafferty: Breast tomosynthesis has been approved for mammographic screening in the United States for just over 5 years, and many single center studies have demonstrated its improved performance for screening outcomes over digital mammography alone. Our previously published multi-center analysis, (JAMA 2014;311(24), the largest study on this topic to date, demonstrated significantly improved cancer detection and reduced recall rates for women undergoing tomosynthesis compared with digital mammography alone. In the current issue of JAMA we evaluate the differential screening performance after implementation of breast tomosynthesis as a function of breast density.
While tomosynthesis continues to be increasingly available, questions remained about which women should be imaged with this technique. In particular, does this technology offer additional benefit for all women, or only for women with dense breasts. The size of the database compiled by the centers participating in this study allowed us to evaluate this important question.
The most critical finding of our study was that the use of tomosynthesis for breast cancer screening significantly improved invasive cancer detection rates while simultaneously significantly reducing recall rates both for women with dense and non-dense breast tissue. Having said that, the magnitude of the benefit was largest for women with heterogeneously dense breast tissue; for this population, tomosynthesis increased the detection of invasive cancers by 50% while simultaneously reducing the recall rate by 14%.