AACR, Author Interviews, Cancer Research / 08.05.2025
AACR25: Novel strategy for p53 mutant cancers leveraging their DNA damage response liabilities
MedicalResearch.com Interview with:
[caption id="attachment_68425" align="alignleft" width="150"] Dr. Andrei Bakin[/caption]
Andrei Bakin, PhD, Associate Professor of Oncology, Department of Cancer Genetics & Genomics, Roswell Park Comprehensive Cancer Center – first author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response” and senior author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”
Christos Fountzilas, MD, FACP, Associate Professor of Oncology, Department of Medicine, Roswell Park Comprehensive Cancer Center - and senior author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response”
Mohammed Alruwaili, MS, PhD, newly graduated doctoral candidate in Cancer Genetics & Genomics at Roswell Park Comprehensive Cancer Center, first author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”
Dr. Andrei Bakin[/caption]
Andrei Bakin, PhD, Associate Professor of Oncology, Department of Cancer Genetics & Genomics, Roswell Park Comprehensive Cancer Center – first author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response” and senior author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”
Christos Fountzilas, MD, FACP, Associate Professor of Oncology, Department of Medicine, Roswell Park Comprehensive Cancer Center - and senior author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response”
Mohammed Alruwaili, MS, PhD, newly graduated doctoral candidate in Cancer Genetics & Genomics at Roswell Park Comprehensive Cancer Center, first author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”
 Dr. Andrei Bakin[/caption]
Andrei Bakin, PhD, Associate Professor of Oncology, Department of Cancer Genetics & Genomics, Roswell Park Comprehensive Cancer Center – first author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response” and senior author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”
Christos Fountzilas, MD, FACP, Associate Professor of Oncology, Department of Medicine, Roswell Park Comprehensive Cancer Center - and senior author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response”
Mohammed Alruwaili, MS, PhD, newly graduated doctoral candidate in Cancer Genetics & Genomics at Roswell Park Comprehensive Cancer Center, first author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”
Dr. Andrei Bakin[/caption]
Andrei Bakin, PhD, Associate Professor of Oncology, Department of Cancer Genetics & Genomics, Roswell Park Comprehensive Cancer Center – first author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response” and senior author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”
Christos Fountzilas, MD, FACP, Associate Professor of Oncology, Department of Medicine, Roswell Park Comprehensive Cancer Center - and senior author of “A novel combination immunotherapy for p53 mutant metastatic breast cancer leveraging vulnerabilities in the DNA damage response”
Mohammed Alruwaili, MS, PhD, newly graduated doctoral candidate in Cancer Genetics & Genomics at Roswell Park Comprehensive Cancer Center, first author of “Novel triple-drug combination strategy for p53 mutant cancers leveraging their DNA damage response liabilities”




 Dr. Sundar[/caption]
Dr. Sundar[/caption]

 Dr. Tesi[/caption]
MedicalResearch.com Interview with:
RJ Tesi M.D.
CEO and Founder of
Dr. Tesi[/caption]
MedicalResearch.com Interview with:
RJ Tesi M.D.
CEO and Founder of 

 Dr. Ulhas Nair[/caption]
Nishanth Ulhas Nair, Ph.D.
Affiliation: Staff Scientist at Cancer Data Science Laboratory, Center for Cancer Research
National Cancer Institute (NCI), National Institutes of Health (NIH)
Bethesda, Maryland, USA. Date: April 22, 2021
Dr. Raffit Hassan and Dr. Eytan Ruppin at the National Cancer Institute (NCI) are the senior authors of this study.
MedicalResearch.com: What is the background for this study?
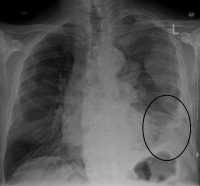
Response: Malignant mesothelioma is an aggressive cancer with limited treatment options and poor prognosis. An in-depth knowledge of genetic, transcriptomic and immunogenic events involved in mesothelioma is critical for successful development of prognostics and therapeutic modalities. In this study we aim to address this by exploring a new large scale patient tumor dataset of 122 mesothelioma patients, called NCI mesothelioma patient data, along with their genomic, transcriptomic, and phenotypic information. Unlike previous large-scale studies which have been focused on malignant pleural mesothelioma patients, our dataset contains an approximately equal representation of malignant pleural and peritoneal mesothelioma patients which allows to identify any differences between them.
Dr. Ulhas Nair[/caption]
Nishanth Ulhas Nair, Ph.D.
Affiliation: Staff Scientist at Cancer Data Science Laboratory, Center for Cancer Research
National Cancer Institute (NCI), National Institutes of Health (NIH)
Bethesda, Maryland, USA. Date: April 22, 2021
Dr. Raffit Hassan and Dr. Eytan Ruppin at the National Cancer Institute (NCI) are the senior authors of this study.
MedicalResearch.com: What is the background for this study?
Response: Malignant mesothelioma is an aggressive cancer with limited treatment options and poor prognosis. An in-depth knowledge of genetic, transcriptomic and immunogenic events involved in mesothelioma is critical for successful development of prognostics and therapeutic modalities. In this study we aim to address this by exploring a new large scale patient tumor dataset of 122 mesothelioma patients, called NCI mesothelioma patient data, along with their genomic, transcriptomic, and phenotypic information. Unlike previous large-scale studies which have been focused on malignant pleural mesothelioma patients, our dataset contains an approximately equal representation of malignant pleural and peritoneal mesothelioma patients which allows to identify any differences between them.










 Dr. Qing Chen[/caption]
Qing Chen, M.D., Ph.D.
Assistant Professor, Immunology, Microenvironment & Metastasis Program
Scientific Director, Imaging Facility
The Wistar Institute
MedicalResearch.com: What is the background for this study?
Response: We are focusing on how a specific type of brain cells, astrocytes, helps the cancer cells from melanoma and breast cancer to form metastatic lesions.
Dr. Qing Chen[/caption]
Qing Chen, M.D., Ph.D.
Assistant Professor, Immunology, Microenvironment & Metastasis Program
Scientific Director, Imaging Facility
The Wistar Institute
MedicalResearch.com: What is the background for this study?
Response: We are focusing on how a specific type of brain cells, astrocytes, helps the cancer cells from melanoma and breast cancer to form metastatic lesions.








