Author Interviews, Cancer Research, NEJM, NIH, OBGYNE / 05.12.2024
NEJM: Prenatal cell-free DNA Can Detect Occult Maternal Cancer
MedicalResearch.com Interview with:
[caption id="attachment_65321" align="alignleft" width="92"] Dr. Bianchi[/caption]
Diana W. Bianchi, M.D.
Senior Investigator
Center for Precision Health Research
Director,
Eunice Kennedy Shriver National Institute of Child Health and Human Development
National Institutes of Health
MedicalResearch.com: What is the background for this study?
Response: The ability of prenatal cell-free DNA (cfDNA) sequencing to incidentally detect maternal cancers has been demonstrated by several retrospective studies from commercial or national laboratories. However, there are no standardized approaches to the identification and medical management of prenatal screening results that might indicate a maternal cancer. We sought to prospectively identify DNA sequencing patterns and other biomarkers that could distinguish which women with nonreportable or unusual cfDNA sequencing results had cancer and to determine the best approach for diagnostic work-up of pregnant people who receive these results.
Dr. Bianchi[/caption]
Diana W. Bianchi, M.D.
Senior Investigator
Center for Precision Health Research
Director,
Eunice Kennedy Shriver National Institute of Child Health and Human Development
National Institutes of Health
MedicalResearch.com: What is the background for this study?
Response: The ability of prenatal cell-free DNA (cfDNA) sequencing to incidentally detect maternal cancers has been demonstrated by several retrospective studies from commercial or national laboratories. However, there are no standardized approaches to the identification and medical management of prenatal screening results that might indicate a maternal cancer. We sought to prospectively identify DNA sequencing patterns and other biomarkers that could distinguish which women with nonreportable or unusual cfDNA sequencing results had cancer and to determine the best approach for diagnostic work-up of pregnant people who receive these results.
 Dr. Bianchi[/caption]
Diana W. Bianchi, M.D.
Senior Investigator
Center for Precision Health Research
Director,
Eunice Kennedy Shriver National Institute of Child Health and Human Development
National Institutes of Health
MedicalResearch.com: What is the background for this study?
Response: The ability of prenatal cell-free DNA (cfDNA) sequencing to incidentally detect maternal cancers has been demonstrated by several retrospective studies from commercial or national laboratories. However, there are no standardized approaches to the identification and medical management of prenatal screening results that might indicate a maternal cancer. We sought to prospectively identify DNA sequencing patterns and other biomarkers that could distinguish which women with nonreportable or unusual cfDNA sequencing results had cancer and to determine the best approach for diagnostic work-up of pregnant people who receive these results.
Dr. Bianchi[/caption]
Diana W. Bianchi, M.D.
Senior Investigator
Center for Precision Health Research
Director,
Eunice Kennedy Shriver National Institute of Child Health and Human Development
National Institutes of Health
MedicalResearch.com: What is the background for this study?
Response: The ability of prenatal cell-free DNA (cfDNA) sequencing to incidentally detect maternal cancers has been demonstrated by several retrospective studies from commercial or national laboratories. However, there are no standardized approaches to the identification and medical management of prenatal screening results that might indicate a maternal cancer. We sought to prospectively identify DNA sequencing patterns and other biomarkers that could distinguish which women with nonreportable or unusual cfDNA sequencing results had cancer and to determine the best approach for diagnostic work-up of pregnant people who receive these results.




 Dr. Han[/caption]
Summer S Han, PhD
Associate Professor
Dr. Han[/caption]
Summer S Han, PhD
Associate Professor
 Dr. Choi[/caption]
Dr. Eunji Choi PhD
Instructor, Neurosurgery
Department: Adult Neurosurgery
Stanford University School of Medicine
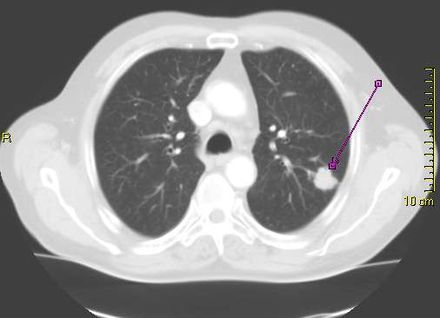
MedicalResearch.com: What is the background for this study?
Dr. Choi[/caption]
Dr. Eunji Choi PhD
Instructor, Neurosurgery
Department: Adult Neurosurgery
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study?



 Dr. Maki Inoue-Choi,[/caption]
Maki Inoue-Choi, Ph.D., M.S., R.D.
Staff Scientist
Metabolic Epidemiology Branch
National Institutes of Health
MedicalResearch.com: What is the background for this study?
Response: Tea is rich in bioactive compounds that can possibly protect against health conditions such as cancer and heart disease. A lower risk of death was seen among tea drinkers than non-drinkers in previous studies, but these were largely in populations where green tea drinking is common. In contrast, the studies in populations where black tea drinking is more common have been limited and the findings from these studies have been inconsistent.
Dr. Maki Inoue-Choi,[/caption]
Maki Inoue-Choi, Ph.D., M.S., R.D.
Staff Scientist
Metabolic Epidemiology Branch
National Institutes of Health
MedicalResearch.com: What is the background for this study?
Response: Tea is rich in bioactive compounds that can possibly protect against health conditions such as cancer and heart disease. A lower risk of death was seen among tea drinkers than non-drinkers in previous studies, but these were largely in populations where green tea drinking is common. In contrast, the studies in populations where black tea drinking is more common have been limited and the findings from these studies have been inconsistent.

 Dr. Altan-Bonnet[/caption]
Nihal Altan-Bonnet, Ph.D.
Chief of the Laboratory of Host-Pathogen Dynamics
NHLBI
MedicalResearch.com: What is the background for this study? What are the main findings?
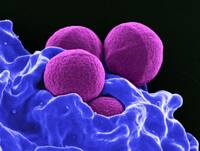
Response: Enteric viruses such as norovirus, rotavirus and astrovirus are responsible for nearly 1.5 billion global infections per year resulting in gastrointestinal illnesses and sometimes leading to death in the very young, in the elderly and in the immunocompromised. These viruses have been thought to traditionally infect and replicate only in the intestines, then shed into feces and transmit to others via the oral-fecal route (e.g. through ingestion of fecal contaminated food items).
Our findings reported in Nature, using animal models of norovirus, rotavirus and astrovirus infection, challenge this traditional view and reveal that these viruses can also replicate robustly in salivary glands, be shed into saliva in large quantities and transmit through saliva to other animals.
In particular we also show infected infants can transmit these viruses to their mothers mammary glands via suckling and this leads to both an infection in their mothers mammary glands but also a rapid immune response by the mother resulting in a surge in her milk antibodies. These milk antibodies may play a role in fighting the infection in their infants .
Dr. Altan-Bonnet[/caption]
Nihal Altan-Bonnet, Ph.D.
Chief of the Laboratory of Host-Pathogen Dynamics
NHLBI
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Enteric viruses such as norovirus, rotavirus and astrovirus are responsible for nearly 1.5 billion global infections per year resulting in gastrointestinal illnesses and sometimes leading to death in the very young, in the elderly and in the immunocompromised. These viruses have been thought to traditionally infect and replicate only in the intestines, then shed into feces and transmit to others via the oral-fecal route (e.g. through ingestion of fecal contaminated food items).
Our findings reported in Nature, using animal models of norovirus, rotavirus and astrovirus infection, challenge this traditional view and reveal that these viruses can also replicate robustly in salivary glands, be shed into saliva in large quantities and transmit through saliva to other animals.
In particular we also show infected infants can transmit these viruses to their mothers mammary glands via suckling and this leads to both an infection in their mothers mammary glands but also a rapid immune response by the mother resulting in a surge in her milk antibodies. These milk antibodies may play a role in fighting the infection in their infants .

 Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?
Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?

 Dr. Launer[/caption]
Lenore J. Launer, Ph.D.
Chief, Laboratory of Epidemiology and Population Sciences
Intramural Research Program, National Institute on Aging.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Identifying early risk factors and early changes in the brain will have a major impact on future clinical and public health priorities related to the looming epidemic of dementia. Several studies based on older populations suggest mid-life is an important period to start prevention measures. To date control of blood pressure levels has been the most robust and promising candidate to target for prevention of future cognitive impairment. Although several studies have looked at levels of blood pressure and risk for cognitive impairment, it was not known whether trajectories from young adulthood to middle age studies provided additional information about risk. To investigate possible biomarkers of future risk, we chose to examine the association of the mean arterial blood pressure trajectories to indicators of pathology seen on MRI and that are associated with cognition.
We highlight the results of the mean arterial blood pressure (MAP) measure, which is an integrated measure of systolic and diastolic blood pressure.
Dr. Launer[/caption]
Lenore J. Launer, Ph.D.
Chief, Laboratory of Epidemiology and Population Sciences
Intramural Research Program, National Institute on Aging.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Identifying early risk factors and early changes in the brain will have a major impact on future clinical and public health priorities related to the looming epidemic of dementia. Several studies based on older populations suggest mid-life is an important period to start prevention measures. To date control of blood pressure levels has been the most robust and promising candidate to target for prevention of future cognitive impairment. Although several studies have looked at levels of blood pressure and risk for cognitive impairment, it was not known whether trajectories from young adulthood to middle age studies provided additional information about risk. To investigate possible biomarkers of future risk, we chose to examine the association of the mean arterial blood pressure trajectories to indicators of pathology seen on MRI and that are associated with cognition.
We highlight the results of the mean arterial blood pressure (MAP) measure, which is an integrated measure of systolic and diastolic blood pressure.

 Dr. Ulhas Nair[/caption]
Nishanth Ulhas Nair, Ph.D.
Affiliation: Staff Scientist at Cancer Data Science Laboratory, Center for Cancer Research
National Cancer Institute (NCI), National Institutes of Health (NIH)
Bethesda, Maryland, USA. Date: April 22, 2021
Dr. Raffit Hassan and Dr. Eytan Ruppin at the National Cancer Institute (NCI) are the senior authors of this study.
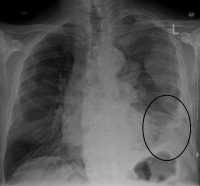
MedicalResearch.com: What is the background for this study?
Response: Malignant mesothelioma is an aggressive cancer with limited treatment options and poor prognosis. An in-depth knowledge of genetic, transcriptomic and immunogenic events involved in mesothelioma is critical for successful development of prognostics and therapeutic modalities. In this study we aim to address this by exploring a new large scale patient tumor dataset of 122 mesothelioma patients, called NCI mesothelioma patient data, along with their genomic, transcriptomic, and phenotypic information. Unlike previous large-scale studies which have been focused on malignant pleural mesothelioma patients, our dataset contains an approximately equal representation of malignant pleural and peritoneal mesothelioma patients which allows to identify any differences between them.
Dr. Ulhas Nair[/caption]
Nishanth Ulhas Nair, Ph.D.
Affiliation: Staff Scientist at Cancer Data Science Laboratory, Center for Cancer Research
National Cancer Institute (NCI), National Institutes of Health (NIH)
Bethesda, Maryland, USA. Date: April 22, 2021
Dr. Raffit Hassan and Dr. Eytan Ruppin at the National Cancer Institute (NCI) are the senior authors of this study.
MedicalResearch.com: What is the background for this study?
Response: Malignant mesothelioma is an aggressive cancer with limited treatment options and poor prognosis. An in-depth knowledge of genetic, transcriptomic and immunogenic events involved in mesothelioma is critical for successful development of prognostics and therapeutic modalities. In this study we aim to address this by exploring a new large scale patient tumor dataset of 122 mesothelioma patients, called NCI mesothelioma patient data, along with their genomic, transcriptomic, and phenotypic information. Unlike previous large-scale studies which have been focused on malignant pleural mesothelioma patients, our dataset contains an approximately equal representation of malignant pleural and peritoneal mesothelioma patients which allows to identify any differences between them.

 Dr. Garantziotis[/caption]
Stavros Garantziotis MD
Division of Intramural Research
National Institute of Environmental Health Sciences
Research Triangle Park, NC
MedicalResearch.com: What is the background for this study? How does hyaluronan differ from other medications for COPD? Is it used for other medical conditions?
Response: Hyaluronan is a natural sugar found in the human body, including in the lung. We have found that when the lungs are exposed to pollution, this sugar breaks down, and the breakdown fragments cause inflammation in the lung. We also found that if we give back the natural form of hyaluronan, it protects the lung from inflammation. Patients suffering from COPD also have a lot of hyaluronan breakdown in their lungs. We therefore reasoned, that giving them back the natural form of hyaluronan, as an inhalation treatment, would help them reduce inflammation. We tested this, as a first step, in the treatment acute inflammation of the lungs in COPD patients who are suffering an exacerbation of their disease.
Hyaluronan is different from existing medications in that it is a natural product of the body. It is used in Europe for conditions like cystic fibrosis, and after sinus surgery to humidify the airways. Because it is given by inhalation, it acts locally in the lungs.
Dr. Garantziotis[/caption]
Stavros Garantziotis MD
Division of Intramural Research
National Institute of Environmental Health Sciences
Research Triangle Park, NC
MedicalResearch.com: What is the background for this study? How does hyaluronan differ from other medications for COPD? Is it used for other medical conditions?
Response: Hyaluronan is a natural sugar found in the human body, including in the lung. We have found that when the lungs are exposed to pollution, this sugar breaks down, and the breakdown fragments cause inflammation in the lung. We also found that if we give back the natural form of hyaluronan, it protects the lung from inflammation. Patients suffering from COPD also have a lot of hyaluronan breakdown in their lungs. We therefore reasoned, that giving them back the natural form of hyaluronan, as an inhalation treatment, would help them reduce inflammation. We tested this, as a first step, in the treatment acute inflammation of the lungs in COPD patients who are suffering an exacerbation of their disease.
Hyaluronan is different from existing medications in that it is a natural product of the body. It is used in Europe for conditions like cystic fibrosis, and after sinus surgery to humidify the airways. Because it is given by inhalation, it acts locally in the lungs. 















