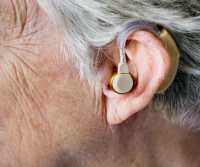
Living with tinnitus often feels like a constant battle against sounds that refuse to fade. Whether it’s a high-pitched ringing, a steady hum, or an unpredictable buzzing, the condition can disrupt nearly every part of daily life. Sleep becomes difficult, focus weakens, and the emotional toll can be overwhelming. For years, available treatments have focused more on managing symptoms than providing lasting relief.
Now, that’s beginning to change. Advances in neuroscience, medical research, and technology are uncovering the underlying causes of tinnitus, bringing a wave of new treatments that go beyond simply masking the noise. The potential for lasting relief—or even complete elimination—feels closer than ever.
Advancements in Neuromodulation Therapy
Neuromodulation is emerging as a leading approach to tinnitus treatment. Unlike conventional methods that focus on distraction or symptom management, this therapy targets the neural circuits responsible for generating phantom sounds. Techniques such as transcranial magnetic stimulation (TMS) and transcranial direct current stimulation (tDCS) aim to modify brain activity, potentially reducing tinnitus intensity.

One particularly exciting development is paired stimulation, which integrates sound therapy with electrical or magnetic pulses. This approach to tinnitus patients is designed to retrain the brain’s response to tinnitus by strengthening normal auditory pathways while weakening abnormal ones. Early studies suggest that regular sessions may lead to long-term improvements, even after treatment ends. Clinics like
Regain Hearing are closely monitoring these advancements, ensuring that individuals with tinnitus have access to the latest diagnostic tools and therapies as they become available.
While neuromodulation remains in the experimental stage, ongoing clinical trials continue to refine these techniques. Personalized therapies tailored to an individual’s specific tinnitus profile may soon become widely accessible, offering new options for those who have struggled to find effective solutions.
 Hearing loss often creeps in slowly. A person may start asking others to repeat themselves, miss parts of conversations in noisy rooms, or turn the television up a little more than before. That is one reason newer devices that blend hearing support into familiar objects are getting attention.
Hearing glasses are one of those devices. They are designed to combine eyewear with built-in hearing assistance, which can make them feel less medical and more natural to use in daily life. Still, the real question is not whether they sound innovative. It is whether they are actually effective for older adults.
In many cases, they can be helpful, especially for older adults with mild to moderate hearing loss who want something discreet and easier to work into everyday routines. But they are not a universal replacement for traditional hearing aids, and how well they work depends a lot on the user’s hearing needs, lifestyle, and expectations.
Hearing loss often creeps in slowly. A person may start asking others to repeat themselves, miss parts of conversations in noisy rooms, or turn the television up a little more than before. That is one reason newer devices that blend hearing support into familiar objects are getting attention.
Hearing glasses are one of those devices. They are designed to combine eyewear with built-in hearing assistance, which can make them feel less medical and more natural to use in daily life. Still, the real question is not whether they sound innovative. It is whether they are actually effective for older adults.
In many cases, they can be helpful, especially for older adults with mild to moderate hearing loss who want something discreet and easier to work into everyday routines. But they are not a universal replacement for traditional hearing aids, and how well they work depends a lot on the user’s hearing needs, lifestyle, and expectations.
 Hearing loss often creeps in slowly. A person may start asking others to repeat themselves, miss parts of conversations in noisy rooms, or turn the television up a little more than before. That is one reason newer devices that blend hearing support into familiar objects are getting attention.
Hearing glasses are one of those devices. They are designed to combine eyewear with built-in hearing assistance, which can make them feel less medical and more natural to use in daily life. Still, the real question is not whether they sound innovative. It is whether they are actually effective for older adults.
In many cases, they can be helpful, especially for older adults with mild to moderate hearing loss who want something discreet and easier to work into everyday routines. But they are not a universal replacement for traditional hearing aids, and how well they work depends a lot on the user’s hearing needs, lifestyle, and expectations.
Hearing loss often creeps in slowly. A person may start asking others to repeat themselves, miss parts of conversations in noisy rooms, or turn the television up a little more than before. That is one reason newer devices that blend hearing support into familiar objects are getting attention.
Hearing glasses are one of those devices. They are designed to combine eyewear with built-in hearing assistance, which can make them feel less medical and more natural to use in daily life. Still, the real question is not whether they sound innovative. It is whether they are actually effective for older adults.
In many cases, they can be helpful, especially for older adults with mild to moderate hearing loss who want something discreet and easier to work into everyday routines. But they are not a universal replacement for traditional hearing aids, and how well they work depends a lot on the user’s hearing needs, lifestyle, and expectations.






 Living with tinnitus often feels like a constant battle against sounds that refuse to fade. Whether it’s a high-pitched ringing, a steady hum, or an unpredictable buzzing, the condition can disrupt nearly every part of daily life. Sleep becomes difficult, focus weakens, and the emotional toll can be overwhelming. For years, available treatments have focused more on managing symptoms than providing lasting relief.
Now, that’s beginning to change. Advances in neuroscience, medical research, and technology are uncovering the underlying causes of tinnitus, bringing a wave of new treatments that go beyond simply masking the noise. The potential for lasting relief—or even complete elimination—feels closer than ever.
Living with tinnitus often feels like a constant battle against sounds that refuse to fade. Whether it’s a high-pitched ringing, a steady hum, or an unpredictable buzzing, the condition can disrupt nearly every part of daily life. Sleep becomes difficult, focus weakens, and the emotional toll can be overwhelming. For years, available treatments have focused more on managing symptoms than providing lasting relief.
Now, that’s beginning to change. Advances in neuroscience, medical research, and technology are uncovering the underlying causes of tinnitus, bringing a wave of new treatments that go beyond simply masking the noise. The potential for lasting relief—or even complete elimination—feels closer than ever.



 Dr. Li Li[/caption]
Li Li, M.D., Ph.D., M.P.H
Walter M. Seward Professor
Chair of Family Medicine
Director of population health
University of Virginia School of Medicine
Editor-in-chief of The BMJ Family Medicine
Dr. Li joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Speech and language delays and disorders can be challenging for children and their families and can lead to difficulties with reading and writing as children grow up.
The Task Force looked at the evidence on screening for speech and language delays and, unfortunately, there is not enough evidence to tell us whether or not it is helpful to screen all children 5 years old and younger for speech and language delays and disorders.
Dr. Li Li[/caption]
Li Li, M.D., Ph.D., M.P.H
Walter M. Seward Professor
Chair of Family Medicine
Director of population health
University of Virginia School of Medicine
Editor-in-chief of The BMJ Family Medicine
Dr. Li joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Speech and language delays and disorders can be challenging for children and their families and can lead to difficulties with reading and writing as children grow up.
The Task Force looked at the evidence on screening for speech and language delays and, unfortunately, there is not enough evidence to tell us whether or not it is helpful to screen all children 5 years old and younger for speech and language delays and disorders.




 Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000.
Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000. 
 Dr. Chien-Wen Tseng[/caption]
Chien-Wen Tseng, M.D., M.P.H., M.S.E.E.
The Hawaii Medical Service Association Endowed Chair
Health Services and Quality Research
Professor, and Associate Research Director
Department of Family Medicine and Community Health
University of Hawaii John A. Burns School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
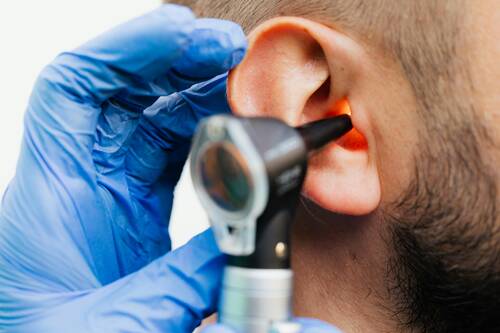
Response: Age-related hearing loss cannot be reversed and can be a significant problem for older adults. Four out of 10 adults who are age 70 and older report hearing loss and it can worsen isolation, cognitive decline, and quality of life, as well as interfere with someone’s ability to live independently. There are simple screening tests to detect hearing loss, so the Task Force did an extensive review of whether there are health benefits to screening for hearing loss in people who do not have symptoms before they notice any hearing problems.
The Task Force determined that there is not enough evidence to recommend for or against screening for hearing loss in adults who are age 50 and older and do not have signs or symptoms of hearing loss. This is an I statement.
Dr. Chien-Wen Tseng[/caption]
Chien-Wen Tseng, M.D., M.P.H., M.S.E.E.
The Hawaii Medical Service Association Endowed Chair
Health Services and Quality Research
Professor, and Associate Research Director
Department of Family Medicine and Community Health
University of Hawaii John A. Burns School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Age-related hearing loss cannot be reversed and can be a significant problem for older adults. Four out of 10 adults who are age 70 and older report hearing loss and it can worsen isolation, cognitive decline, and quality of life, as well as interfere with someone’s ability to live independently. There are simple screening tests to detect hearing loss, so the Task Force did an extensive review of whether there are health benefits to screening for hearing loss in people who do not have symptoms before they notice any hearing problems.
The Task Force determined that there is not enough evidence to recommend for or against screening for hearing loss in adults who are age 50 and older and do not have signs or symptoms of hearing loss. This is an I statement.

 Dr. Reed[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Epidemiology
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: It is known that hearing aid ownership is relatively low in the United States at less than 20% of adults with hearing loss owning and using hearing aids. However, many national estimates of hearing aid ownership are based on data that is over 10 years old. Our team was interested in trying to understand whether ownership in hearing aids had changed over time. We used data from 2011 to 2018 in a nationally representative (United States) observational cohort (The National Health and Aging Trends Study) of Medicare Beneficiaries aged 70 years and older to estimate the change in hearing aid ownership.
In our analysis, the proportion of Medicare beneficiaries 70 years and older who reported owning and using their hearing aids increased 23.3% from 2011 to 2018. However, this growth in ownership was not equal across all older adults. For example, while White males saw a 28.7% increase in hearing aid ownership, Black females saw only a 5.8% increase over the same 8-year period. Moreover, adults living at less than 100% federal poverty level actually saw an overall 13.0% decrease in hearing aid ownership while those living at more than 200% federal poverty line saw an overall 30.6% increase.
Dr. Reed[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Epidemiology
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: It is known that hearing aid ownership is relatively low in the United States at less than 20% of adults with hearing loss owning and using hearing aids. However, many national estimates of hearing aid ownership are based on data that is over 10 years old. Our team was interested in trying to understand whether ownership in hearing aids had changed over time. We used data from 2011 to 2018 in a nationally representative (United States) observational cohort (The National Health and Aging Trends Study) of Medicare Beneficiaries aged 70 years and older to estimate the change in hearing aid ownership.
In our analysis, the proportion of Medicare beneficiaries 70 years and older who reported owning and using their hearing aids increased 23.3% from 2011 to 2018. However, this growth in ownership was not equal across all older adults. For example, while White males saw a 28.7% increase in hearing aid ownership, Black females saw only a 5.8% increase over the same 8-year period. Moreover, adults living at less than 100% federal poverty level actually saw an overall 13.0% decrease in hearing aid ownership while those living at more than 200% federal poverty line saw an overall 30.6% increase. 

 Dr. Wick[/caption]
Cameron C. Wick, MD
Assistant Professor, Otology/Neurotology
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What do you see as the primary message of your findings for the general public?
Response: Older adults not satisfied with their hearing aids achieved clinically meaningful improvement in both hearing and quality of life with a cochlear implant compared to an optimized bilateral hearing aid condition.
MedicalResearch.com: Do you see your findings as changing the way older adults with hearing loss are managed?
Response: Yes and partially because this study is unique in its design and the outcomes that were measured. Specifically the study is a prospective, multicenter clinical trial conducted at 13 locations across the United States. All patients were setup with a 30-day optimized hearing aid experience before cochlear implantation (context: sometimes hearing aids are not appropriately optimized so baseline testing may not reflect the "best" that hearing aids can do). This study assesses both hearing data as well as quality of life data before and 6-months after cochlear implantation. After implantation patients were tested in both the unilateral (cochlear implant alone) and bimodal (cochlear implant plus hearing aid in the opposite ear) conditions. My paper is a subanalysis of adults 65 years and older (range 65 - 91 years) enrolled in the clinical trial. The principal investigator of the clinical trial is Dr. Craig Buchman. Dr. Buchman and myself are at Washington University in St. Louis which was the lead center for the clinical trial.
The findings of the study are meaningful because they demonstrate clear superiority of cochlear implants over hearing aids in many key areas, such as understanding speech, hearing in background noise, and ability to communicate. Hearing loss, which becomes more prevalent as we age, can negatively impact communication leading to social isolation, depression, frustration, and possibly cognitive decline. This study highlights that if patients are not satisfied with their hearing aid performance then they should be referred to a center that can evaluate for cochlear implantation. Cochlear implant indications have evolved considerably since they were first FDA approved in 1984. This study emphasizes that patients do not have to be profoundly deaf to experience significant hearing and social benefits from cochlear implants. Also, it demonstrates that cochlear implant surgery is well tolerated even as adults age and acquire other health ailments.
Dr. Wick[/caption]
Cameron C. Wick, MD
Assistant Professor, Otology/Neurotology
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What do you see as the primary message of your findings for the general public?
Response: Older adults not satisfied with their hearing aids achieved clinically meaningful improvement in both hearing and quality of life with a cochlear implant compared to an optimized bilateral hearing aid condition.
MedicalResearch.com: Do you see your findings as changing the way older adults with hearing loss are managed?
Response: Yes and partially because this study is unique in its design and the outcomes that were measured. Specifically the study is a prospective, multicenter clinical trial conducted at 13 locations across the United States. All patients were setup with a 30-day optimized hearing aid experience before cochlear implantation (context: sometimes hearing aids are not appropriately optimized so baseline testing may not reflect the "best" that hearing aids can do). This study assesses both hearing data as well as quality of life data before and 6-months after cochlear implantation. After implantation patients were tested in both the unilateral (cochlear implant alone) and bimodal (cochlear implant plus hearing aid in the opposite ear) conditions. My paper is a subanalysis of adults 65 years and older (range 65 - 91 years) enrolled in the clinical trial. The principal investigator of the clinical trial is Dr. Craig Buchman. Dr. Buchman and myself are at Washington University in St. Louis which was the lead center for the clinical trial.
The findings of the study are meaningful because they demonstrate clear superiority of cochlear implants over hearing aids in many key areas, such as understanding speech, hearing in background noise, and ability to communicate. Hearing loss, which becomes more prevalent as we age, can negatively impact communication leading to social isolation, depression, frustration, and possibly cognitive decline. This study highlights that if patients are not satisfied with their hearing aid performance then they should be referred to a center that can evaluate for cochlear implantation. Cochlear implant indications have evolved considerably since they were first FDA approved in 1984. This study emphasizes that patients do not have to be profoundly deaf to experience significant hearing and social benefits from cochlear implants. Also, it demonstrates that cochlear implant surgery is well tolerated even as adults age and acquire other health ailments. 
 Dr. Blundon[/caption]
Elizabeth Blundon PhD
Department of Psychology
University of British Columbia – Vancouver
MedicalResearch.com: What is the background for this study?
Response: Many healthcare workers have noticed that dying patients appear to be comforted by the words of their loved ones, even when patients appear to be unconscious and are no longer able to communicate. There is a persistent belief, therefore, that hearing may persist into the last hours of someone's life. Our study attempts to detect evidence of hearing among a small group of unresponsive hospice patients at the end of life.
To do this, we compared the brain activity of young, healthy control participants, with the brain activity of hospice patients, both when the patients were awake and responsive, and again when they became unresponsive. The brain activity we measured was in response to a complex series of tone-patterns, where participants were asked to identify by pressing a button (control participants) or by counting (hospice patients) every time they heard a tone-pattern that was different from the rest of the series.
Dr. Blundon[/caption]
Elizabeth Blundon PhD
Department of Psychology
University of British Columbia – Vancouver
MedicalResearch.com: What is the background for this study?
Response: Many healthcare workers have noticed that dying patients appear to be comforted by the words of their loved ones, even when patients appear to be unconscious and are no longer able to communicate. There is a persistent belief, therefore, that hearing may persist into the last hours of someone's life. Our study attempts to detect evidence of hearing among a small group of unresponsive hospice patients at the end of life.
To do this, we compared the brain activity of young, healthy control participants, with the brain activity of hospice patients, both when the patients were awake and responsive, and again when they became unresponsive. The brain activity we measured was in response to a complex series of tone-patterns, where participants were asked to identify by pressing a button (control participants) or by counting (hospice patients) every time they heard a tone-pattern that was different from the rest of the series.