Accidents & Violence, Brain Injury, Legal-Malpractice, Neurology / 23.02.2026
How Neuroinflammation Shapes Cognitive Outcomes Following Acute Trauma
[caption id="attachment_72574" align="aligncenter" width="500"] Pexels image[/caption]
Acute trauma has long been associated with visible physical damage. However, the invisible neurological consequences often shape long-term recovery just as strongly.
Cognitive symptoms such as memory lapses, reduced attention span, slower processing speed, and emotional instability emerge after traumatic events. Growing research suggests that neuroinflammation plays a central role in determining the impact on cognitive function.
For instance, the blood-brain barrier (BBB) can be affected by injury-induced inflammation. Studies have linked BBB disruption to cognitive decline. Some of the most associated factors are inflammation, metabolic imbalance, cellular aging, oxidative and nitrosative stress, and excitotoxicity.
Studies also suggest that altering BBB permeability can produce either protective or harmful neurological effects, depending on the context.
Understanding how inflammatory pathways respond to trauma offers insight into why some individuals regain their previous level of functioning while others don’t.
Pexels image[/caption]
Acute trauma has long been associated with visible physical damage. However, the invisible neurological consequences often shape long-term recovery just as strongly.
Cognitive symptoms such as memory lapses, reduced attention span, slower processing speed, and emotional instability emerge after traumatic events. Growing research suggests that neuroinflammation plays a central role in determining the impact on cognitive function.
For instance, the blood-brain barrier (BBB) can be affected by injury-induced inflammation. Studies have linked BBB disruption to cognitive decline. Some of the most associated factors are inflammation, metabolic imbalance, cellular aging, oxidative and nitrosative stress, and excitotoxicity.
Studies also suggest that altering BBB permeability can produce either protective or harmful neurological effects, depending on the context.
Understanding how inflammatory pathways respond to trauma offers insight into why some individuals regain their previous level of functioning while others don’t.
 Pexels image[/caption]
Acute trauma has long been associated with visible physical damage. However, the invisible neurological consequences often shape long-term recovery just as strongly.
Cognitive symptoms such as memory lapses, reduced attention span, slower processing speed, and emotional instability emerge after traumatic events. Growing research suggests that neuroinflammation plays a central role in determining the impact on cognitive function.
For instance, the blood-brain barrier (BBB) can be affected by injury-induced inflammation. Studies have linked BBB disruption to cognitive decline. Some of the most associated factors are inflammation, metabolic imbalance, cellular aging, oxidative and nitrosative stress, and excitotoxicity.
Studies also suggest that altering BBB permeability can produce either protective or harmful neurological effects, depending on the context.
Understanding how inflammatory pathways respond to trauma offers insight into why some individuals regain their previous level of functioning while others don’t.
Pexels image[/caption]
Acute trauma has long been associated with visible physical damage. However, the invisible neurological consequences often shape long-term recovery just as strongly.
Cognitive symptoms such as memory lapses, reduced attention span, slower processing speed, and emotional instability emerge after traumatic events. Growing research suggests that neuroinflammation plays a central role in determining the impact on cognitive function.
For instance, the blood-brain barrier (BBB) can be affected by injury-induced inflammation. Studies have linked BBB disruption to cognitive decline. Some of the most associated factors are inflammation, metabolic imbalance, cellular aging, oxidative and nitrosative stress, and excitotoxicity.
Studies also suggest that altering BBB permeability can produce either protective or harmful neurological effects, depending on the context.
Understanding how inflammatory pathways respond to trauma offers insight into why some individuals regain their previous level of functioning while others don’t.






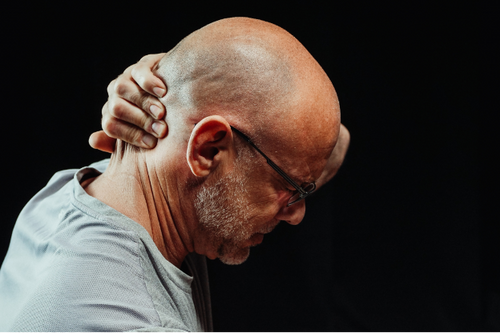
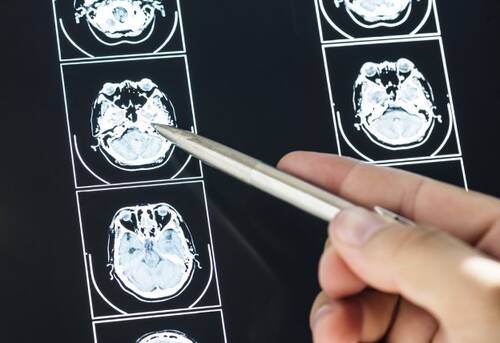

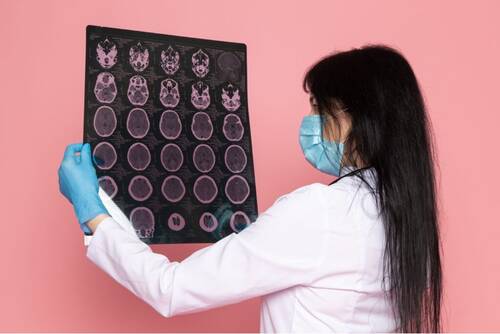
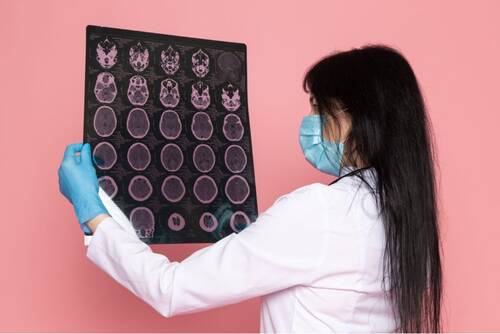




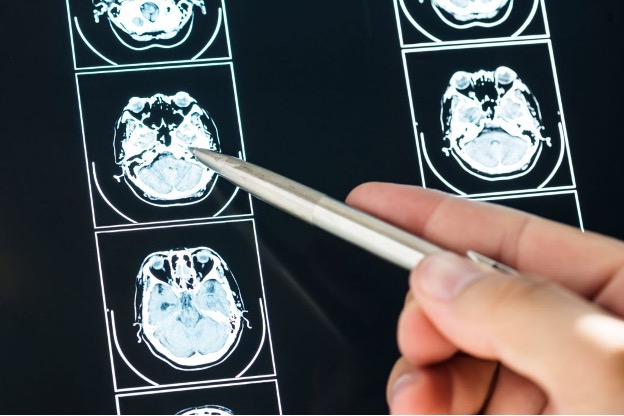



 If you've been in a scrape and your noggin took a knock, playing it tough and shaking it off isn't the way to go.
If you've been in a scrape and your noggin took a knock, playing it tough and shaking it off isn't the way to go. 


 Dr. Mahncke[/caption]
Dr. Mahncke earned his PhD at UCSF in the lab where lifelong brain plasticity was discovered. At the request of his academic mentor, he currently leads a global team of more than 400 brain scientists engaged in designing, testing, refining, and validating the computerized brain exercises found in the BrainHQ app from Posit Science, where he serves as CEO.
Earlier this year, MedicalResearch.com interviewed Dr. Henry Mahncke about the BRAVE Study he led, which showed a digital health app (BrainHQ) was effective in addressing chronic cognitive issues in servicemembers who had been diagnosed with “mild” Traumatic Brain Injury. This week, MedicalResearch.com interviews Dr. Mahncke again about a new independent study among civilians showing similar results in patients with all kinds of Brain Injuries.
MedicalResearch.com: What is the background for this study?
Response: The Centers for Disease Control (CDC) estimates that about 5.3 million people currently live with a chronic disability from a Traumatic Brain Injury (TBI). While most people who suffer a blow to the head recover in a couple days or weeks, for some (estimated as high as 15 percent) the injury persists with a variety of life-disrupting symptoms, including impairments in cognitive abilities, behavior, emotions, and motor function affecting work, relationships, and daily function.
TBIs have been the signature injury of recent wars. Nearly 400,000 service members have been diagnosed with TBIs, of which 82% were diagnosed with so-called “mild” TBIs from concussions and blast injuries. More than a decade ago, we began being asked by military and Veterans organizations, to study whether our brain exercises – which had shown positive effects in measures of cognition, everyday function, mood, and motor function in healthy older adults – could have an impact on people with chronic symptoms from TBIs.
We talked earlier this year, when an 83-person, gold-standard, randomized controlled trial on mTBI (called the BRAVE Study) announced quite positive results from using BrainHQ exercises. That study was funded by the Department of Defense and run as five military and Veterans medical centers. The BRAVE Study found the BrainHQ group showed a statistically and clinically significant improvement on a standard measure of overall cognitive function (compared to a computer games control), and this benefit persisted for at least 12 weeks after training completed. Cognitive function improvements were nearly four times larger in the BrainHQ group than the control (as measured immediately following training) and grew to nearly five times larger (when measured again 12 weeks after training ended). On average, participants in the BrainHQ group improved on the cognitive performance composite measure by 24 percentile ranks – as though they went from the 50th percentile to the 74th percentile.
One large question left unanswered from the BRAVE study was whether this approach might also work for other categories of TBIs, such as moderate and severe TBIs. A new study from independent researchers at NYU answers that question.
Dr. Mahncke[/caption]
Dr. Mahncke earned his PhD at UCSF in the lab where lifelong brain plasticity was discovered. At the request of his academic mentor, he currently leads a global team of more than 400 brain scientists engaged in designing, testing, refining, and validating the computerized brain exercises found in the BrainHQ app from Posit Science, where he serves as CEO.
Earlier this year, MedicalResearch.com interviewed Dr. Henry Mahncke about the BRAVE Study he led, which showed a digital health app (BrainHQ) was effective in addressing chronic cognitive issues in servicemembers who had been diagnosed with “mild” Traumatic Brain Injury. This week, MedicalResearch.com interviews Dr. Mahncke again about a new independent study among civilians showing similar results in patients with all kinds of Brain Injuries.
MedicalResearch.com: What is the background for this study?
Response: The Centers for Disease Control (CDC) estimates that about 5.3 million people currently live with a chronic disability from a Traumatic Brain Injury (TBI). While most people who suffer a blow to the head recover in a couple days or weeks, for some (estimated as high as 15 percent) the injury persists with a variety of life-disrupting symptoms, including impairments in cognitive abilities, behavior, emotions, and motor function affecting work, relationships, and daily function.
TBIs have been the signature injury of recent wars. Nearly 400,000 service members have been diagnosed with TBIs, of which 82% were diagnosed with so-called “mild” TBIs from concussions and blast injuries. More than a decade ago, we began being asked by military and Veterans organizations, to study whether our brain exercises – which had shown positive effects in measures of cognition, everyday function, mood, and motor function in healthy older adults – could have an impact on people with chronic symptoms from TBIs.
We talked earlier this year, when an 83-person, gold-standard, randomized controlled trial on mTBI (called the BRAVE Study) announced quite positive results from using BrainHQ exercises. That study was funded by the Department of Defense and run as five military and Veterans medical centers. The BRAVE Study found the BrainHQ group showed a statistically and clinically significant improvement on a standard measure of overall cognitive function (compared to a computer games control), and this benefit persisted for at least 12 weeks after training completed. Cognitive function improvements were nearly four times larger in the BrainHQ group than the control (as measured immediately following training) and grew to nearly five times larger (when measured again 12 weeks after training ended). On average, participants in the BrainHQ group improved on the cognitive performance composite measure by 24 percentile ranks – as though they went from the 50th percentile to the 74th percentile.
One large question left unanswered from the BRAVE study was whether this approach might also work for other categories of TBIs, such as moderate and severe TBIs. A new study from independent researchers at NYU answers that question.


 Prof. Stewart[/caption]
Willie Stewart, MBChB, PhD, DipFMS, FRCPath, FRCP Edin
Consultant Neuropathologist
Honorary Professor
Department of Neuropathology
Queen Elizabeth University Hospital
Glasgow, UK
MedicalResearch.com: What is the background for this study?
Response: There is concern over the association between participation in contact sports and later life risk of dementia and associated neurodegenerative disease. Much of this comes from observations of a specific form of neurodegenerative pathology - chronic traumatic encephalopathy (CTE)- linked to history of traumatic brain injury (TBI) and repetitive head impacts in autopsy studies of relatively small numbers of former athletes, including boxers and soccer players. Nevertheless, although this brain injury linked pathology is described, surprisingly little is known about what this might mean for later life health, specifically risk of dementia.
In a previous study published from our programme of research looking at "Football's Influence on Lifelong health and Dementia risk' (the FIELD Study), we demonstrated that former professional soccer players had an approximately three-and-a-half-fold higher mortality from neurodegenerative disease than matched general population controls. However, these mortality data did not allow us to consider the relationships between varying head injury/impact exposure variables, such as player position and career length, and risk of neurodegenerative disease.
Prof. Stewart[/caption]
Willie Stewart, MBChB, PhD, DipFMS, FRCPath, FRCP Edin
Consultant Neuropathologist
Honorary Professor
Department of Neuropathology
Queen Elizabeth University Hospital
Glasgow, UK
MedicalResearch.com: What is the background for this study?
Response: There is concern over the association between participation in contact sports and later life risk of dementia and associated neurodegenerative disease. Much of this comes from observations of a specific form of neurodegenerative pathology - chronic traumatic encephalopathy (CTE)- linked to history of traumatic brain injury (TBI) and repetitive head impacts in autopsy studies of relatively small numbers of former athletes, including boxers and soccer players. Nevertheless, although this brain injury linked pathology is described, surprisingly little is known about what this might mean for later life health, specifically risk of dementia.
In a previous study published from our programme of research looking at "Football's Influence on Lifelong health and Dementia risk' (the FIELD Study), we demonstrated that former professional soccer players had an approximately three-and-a-half-fold higher mortality from neurodegenerative disease than matched general population controls. However, these mortality data did not allow us to consider the relationships between varying head injury/impact exposure variables, such as player position and career length, and risk of neurodegenerative disease. 
 Dr. Kelley[/caption]
Mireille E. Kelley Ph.D.
Staff Consultant for Engineering Systems Inc.
MedicalResearch.com: What is the background for this study?
Response: Youth and high school football players can sustain hundreds of head impacts in a season and while most of these impacts do not result in any signs or symptoms of concussion, there is concern that these repetitive subconcussive impacts may have a negative effect on the brain.
The results of this study are part of an NIH-funded study to understand the effects of subconcussive head impact exposure on imaging data collected at pre- and post-season time points. The present study leveraged the longitudinal data that was collected in the parent study to understand how head impact exposure changes among athletes from season to season and how that relates to changes measured from imaging.
Dr. Kelley[/caption]
Mireille E. Kelley Ph.D.
Staff Consultant for Engineering Systems Inc.
MedicalResearch.com: What is the background for this study?
Response: Youth and high school football players can sustain hundreds of head impacts in a season and while most of these impacts do not result in any signs or symptoms of concussion, there is concern that these repetitive subconcussive impacts may have a negative effect on the brain.
The results of this study are part of an NIH-funded study to understand the effects of subconcussive head impact exposure on imaging data collected at pre- and post-season time points. The present study leveraged the longitudinal data that was collected in the parent study to understand how head impact exposure changes among athletes from season to season and how that relates to changes measured from imaging.

 Dr. Master[/caption]
Christina L. Master, MD, FAAP, CAQSM, FACSM
Professor of Clinical Pediatrics
Perelman School of Medicine at the University of Pennsylvania
Co-Director, Minds Matter Concussion Program
Pediatric and Adolescent Sports Medicine, Division of Pediatric Orthopedics
Attending Physician, Care Network - Karabots Center
The Children's Hospital of Philadelphia
Philadelphia, PA 19104
MedicalResearch.com: What is the background for this study?
Response: There have been multiple studies investigating potential sex differences in outcomes from concussion which have sometimes had conflicting results with some studies indicating that females take longer to recover than males and some studies reporting no difference in recovery between females and males, with most of these studies being conducted either retrospectively or prospectively in smaller cohorts. This large-scale multi-center prospective study in collegiate athletes provided an opportunity to compare females and males across comparable sports to examine both potential intrinsic or biologic factors (sex differences) or extrinsic (environmental or gender differences) that contribute to outcomes.
Dr. Master[/caption]
Christina L. Master, MD, FAAP, CAQSM, FACSM
Professor of Clinical Pediatrics
Perelman School of Medicine at the University of Pennsylvania
Co-Director, Minds Matter Concussion Program
Pediatric and Adolescent Sports Medicine, Division of Pediatric Orthopedics
Attending Physician, Care Network - Karabots Center
The Children's Hospital of Philadelphia
Philadelphia, PA 19104
MedicalResearch.com: What is the background for this study?
Response: There have been multiple studies investigating potential sex differences in outcomes from concussion which have sometimes had conflicting results with some studies indicating that females take longer to recover than males and some studies reporting no difference in recovery between females and males, with most of these studies being conducted either retrospectively or prospectively in smaller cohorts. This large-scale multi-center prospective study in collegiate athletes provided an opportunity to compare females and males across comparable sports to examine both potential intrinsic or biologic factors (sex differences) or extrinsic (environmental or gender differences) that contribute to outcomes.

 Dr. Joshi[/caption]
Nitin Joshi, Ph.D.
Engineering in Medicine/Department of Medicine
Brigham and Women's Hospital
[caption id="attachment_56349" align="alignleft" width="100"]
Dr. Joshi[/caption]
Nitin Joshi, Ph.D.
Engineering in Medicine/Department of Medicine
Brigham and Women's Hospital
[caption id="attachment_56349" align="alignleft" width="100"]