Allergies, Author Interviews, Dermatology / 06.12.2025
ACAAI: Remibrutinib As Oral option for Patients with Chronic Spontaneous Urticaria who have failed high dose antihistamines
[caption id="attachment_71677" align="alignleft" width="200"] Dr. Gogate[/caption]
MedicalResearch.com Interview with:
Dr. Shaila Gogate, MD
Colorado Allergy & Asthma Centers
Allergist
REMIX-1/-2 Investigator
MedicalResearch.com: What is the background for this study? What are the main findings?
A: The Phase III REMIX-1/-2 studies were randomized, double-blind, placebo-controlled studies assessing the efficacy and safety of oral remibrutinib 25 mg twice daily or placebo over a 24-week double-blind period, followed by a 28-week open-label remibrutinib treatment period.
The purpose of this pooled analysis was to examine the early and long-term efficacy data of remibrutinib vs. placebo over time, looking at the mean percentage change from baseline (CFB) in weekly scores of disease activity (UAS7), itch severity (ISS7) and hives severity (HSS7) over 52 weeks. This analysis demonstrated that remibrutinib showed reductions in urticaria symptoms vs. placebo as early as week 1:
Dr. Gogate[/caption]
MedicalResearch.com Interview with:
Dr. Shaila Gogate, MD
Colorado Allergy & Asthma Centers
Allergist
REMIX-1/-2 Investigator
MedicalResearch.com: What is the background for this study? What are the main findings?
A: The Phase III REMIX-1/-2 studies were randomized, double-blind, placebo-controlled studies assessing the efficacy and safety of oral remibrutinib 25 mg twice daily or placebo over a 24-week double-blind period, followed by a 28-week open-label remibrutinib treatment period.
The purpose of this pooled analysis was to examine the early and long-term efficacy data of remibrutinib vs. placebo over time, looking at the mean percentage change from baseline (CFB) in weekly scores of disease activity (UAS7), itch severity (ISS7) and hives severity (HSS7) over 52 weeks. This analysis demonstrated that remibrutinib showed reductions in urticaria symptoms vs. placebo as early as week 1:
 Dr. Gogate[/caption]
MedicalResearch.com Interview with:
Dr. Shaila Gogate, MD
Colorado Allergy & Asthma Centers
Allergist
REMIX-1/-2 Investigator
MedicalResearch.com: What is the background for this study? What are the main findings?
A: The Phase III REMIX-1/-2 studies were randomized, double-blind, placebo-controlled studies assessing the efficacy and safety of oral remibrutinib 25 mg twice daily or placebo over a 24-week double-blind period, followed by a 28-week open-label remibrutinib treatment period.
The purpose of this pooled analysis was to examine the early and long-term efficacy data of remibrutinib vs. placebo over time, looking at the mean percentage change from baseline (CFB) in weekly scores of disease activity (UAS7), itch severity (ISS7) and hives severity (HSS7) over 52 weeks. This analysis demonstrated that remibrutinib showed reductions in urticaria symptoms vs. placebo as early as week 1:
Dr. Gogate[/caption]
MedicalResearch.com Interview with:
Dr. Shaila Gogate, MD
Colorado Allergy & Asthma Centers
Allergist
REMIX-1/-2 Investigator
MedicalResearch.com: What is the background for this study? What are the main findings?
A: The Phase III REMIX-1/-2 studies were randomized, double-blind, placebo-controlled studies assessing the efficacy and safety of oral remibrutinib 25 mg twice daily or placebo over a 24-week double-blind period, followed by a 28-week open-label remibrutinib treatment period.
The purpose of this pooled analysis was to examine the early and long-term efficacy data of remibrutinib vs. placebo over time, looking at the mean percentage change from baseline (CFB) in weekly scores of disease activity (UAS7), itch severity (ISS7) and hives severity (HSS7) over 52 weeks. This analysis demonstrated that remibrutinib showed reductions in urticaria symptoms vs. placebo as early as week 1:
-
- 38.4% vs. 10.3% in UAS7
- 37.0% vs. 9.8% in ISS7
- 39.8% vs. 10.1% HSS7 Greater reductions vs. placebo were seen over 24 weeks and results were observed in the open-label period through week 52 in all remibrutinib-treated patients (including those transitioned from placebo).


 Dr. Mosnaim[/caption]
Dr. Giselle Mosnaim MD MS FACAAI
Allergist
Division of Allergy and Immunology
Department of Medicine
Northshore University Health System
REMIX-1/-2 Investigator
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Chronic spontaneous urticaria is a debilitating condition significantly affecting patient quality of life and is characterized by the presence of itch, hives, and/or angioedema (swelling) lasting for greater than 6 weeks, without identifiable trigger. Second-generation H1-antihistamines at standard doses are recommended as first-line treatment for patients with chronic spontaneous urticaria, and can be up-dosed to 4 times the standard dose. However, over 50% of patients continue to have symptoms despite this therapy. Both Remibrutinib and Dupilumab are FDA-approved for the treatment of chronic spontaneous urticaria in adult patients (Remibrutinib ≥ 18 years old and Dupilumab ≥ 12 years old) who remain symptomatic despite second-generation H1-antihistamine treatment.
The RECLAIM study is an ongoing head-to-head randomized controlled trial comparing the efficacy of Remibrutinib, an oral Bruton’s tyrosine kinase inhibitor, and Dupilumab, an injectable anti-interleukin-4 and anti-interleukin-13 inhibitor, at early timepoints (4 weeks and earlier) when administered as an add-on therapy in adults with moderate to severe chronic spontaneous urticaria inadequately controlled by second-generation H1-antihistamines.
Dr. Mosnaim[/caption]
Dr. Giselle Mosnaim MD MS FACAAI
Allergist
Division of Allergy and Immunology
Department of Medicine
Northshore University Health System
REMIX-1/-2 Investigator
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Chronic spontaneous urticaria is a debilitating condition significantly affecting patient quality of life and is characterized by the presence of itch, hives, and/or angioedema (swelling) lasting for greater than 6 weeks, without identifiable trigger. Second-generation H1-antihistamines at standard doses are recommended as first-line treatment for patients with chronic spontaneous urticaria, and can be up-dosed to 4 times the standard dose. However, over 50% of patients continue to have symptoms despite this therapy. Both Remibrutinib and Dupilumab are FDA-approved for the treatment of chronic spontaneous urticaria in adult patients (Remibrutinib ≥ 18 years old and Dupilumab ≥ 12 years old) who remain symptomatic despite second-generation H1-antihistamine treatment.
The RECLAIM study is an ongoing head-to-head randomized controlled trial comparing the efficacy of Remibrutinib, an oral Bruton’s tyrosine kinase inhibitor, and Dupilumab, an injectable anti-interleukin-4 and anti-interleukin-13 inhibitor, at early timepoints (4 weeks and earlier) when administered as an add-on therapy in adults with moderate to severe chronic spontaneous urticaria inadequately controlled by second-generation H1-antihistamines.


 Dr. Casale[/caption]
Thomas B. Casale, M.D.
Professor of Medicine and Pediatrics
Chief of Clinical and Translational Research
Division of Allergy and Immunology
USF Health Morsani College of Medicine
University of South Florida
Tampa, Florida
MedicalResearch.com: What is the background for this study?
Response: The data leading to FDA approval of neffy came from extensive pharmacokinetic and pharmacodynamic studies. As with previous epinephrine delivery devices, the FDA asked for data showing that after delivery of neffy the epinephrine blood levels and expected changes in pulse and blood pressure were similar to those achieved with injectable formulations of epinephrine. neffy performed as expected with blood levels of epinephrine bracketed by those achieved with EpiPen and a needle and syringe along with increases in pulse and blood pressure compatible with the epinephrine levels measured.
Additionally, clinicians are interested in whether neffy would perform similarly in real clinical situations. The data from the neffy experience program provides real-world assurance that neffy can effectively treat acute allergic reactions. Given the large number of patients and the similar findings to those achieved with injectable epinephrine in previous studies, the data should provide assurance that neffy can be an effective substitute for injectable epinephrine in patients that desire a needle-free option.
Dr. Casale[/caption]
Thomas B. Casale, M.D.
Professor of Medicine and Pediatrics
Chief of Clinical and Translational Research
Division of Allergy and Immunology
USF Health Morsani College of Medicine
University of South Florida
Tampa, Florida
MedicalResearch.com: What is the background for this study?
Response: The data leading to FDA approval of neffy came from extensive pharmacokinetic and pharmacodynamic studies. As with previous epinephrine delivery devices, the FDA asked for data showing that after delivery of neffy the epinephrine blood levels and expected changes in pulse and blood pressure were similar to those achieved with injectable formulations of epinephrine. neffy performed as expected with blood levels of epinephrine bracketed by those achieved with EpiPen and a needle and syringe along with increases in pulse and blood pressure compatible with the epinephrine levels measured.
Additionally, clinicians are interested in whether neffy would perform similarly in real clinical situations. The data from the neffy experience program provides real-world assurance that neffy can effectively treat acute allergic reactions. Given the large number of patients and the similar findings to those achieved with injectable epinephrine in previous studies, the data should provide assurance that neffy can be an effective substitute for injectable epinephrine in patients that desire a needle-free option.






 The reaction triggers the symptoms you recognize as your allergy, such as a runny nose and itchy eyes.
The reaction triggers the symptoms you recognize as your allergy, such as a runny nose and itchy eyes. 

 Lone Star Tick Nymph-CDC image[/caption]
MedicalResearch.com: What is the background for this study? Would you briefly describe Alpha-gal Syndrome?
Response: Alpha-gal syndrome is an emerging and potentially life-threatening allergic condition that is associated with a tick bite. It is also called alpha-gal allergy, red meat allergy, or tick bite meat allergy.
Increasing case studies and anecdotal reports suggested that AGS was a growing concern, but, prior to these studies, information on clinician awareness and the number of people impacted was not available at a national level.
Lone Star Tick Nymph-CDC image[/caption]
MedicalResearch.com: What is the background for this study? Would you briefly describe Alpha-gal Syndrome?
Response: Alpha-gal syndrome is an emerging and potentially life-threatening allergic condition that is associated with a tick bite. It is also called alpha-gal allergy, red meat allergy, or tick bite meat allergy.
Increasing case studies and anecdotal reports suggested that AGS was a growing concern, but, prior to these studies, information on clinician awareness and the number of people impacted was not available at a national level.

 Dr. Greenhawt[/caption]
Matthew Greenhawt, MD, MBA, MSc
Professor of Pediatrics
Section of Allergy and Immunology
Director, Food Challenge and Research Unit
Children’s Hospital Colorado
University of Colorado School of Medicine
Anschutz Medical Campus
Dr. Greenhawt[/caption]
Matthew Greenhawt, MD, MBA, MSc
Professor of Pediatrics
Section of Allergy and Immunology
Director, Food Challenge and Research Unit
Children’s Hospital Colorado
University of Colorado School of Medicine
Anschutz Medical Campus


 Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).
Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).

 Dr. Chan[/caption]
Edmond S. Chan MD, FRCPC, FCSACI, FAAAAI
Head | Division of Allergy & Immunology | Department of Pediatrics, Faculty of Medicine
Clinical Professor, The University of British Columbia
Clinical Investigator, BC Children's Hospital Research Institute
BC Children's Hospital, Allergy Clinic
Vancouver, BC Canada
Treasurer, CSACI (Canadian Society of Allergy & Clinical Immunology)
MedicalResearch.com: What prompted you to look at the safety of peanut oral immunotherapy specifically in this patient population?
Response: Our previous research has investigated the overall safety of peanut oral immunotherapy (OIT) in preschool populations. However, we have not investigated the relationship between specific patient characteristics and the safety of OIT. Previous literature has shown that patient factors, such as age, gender, baseline sIgE levels, and atopic comorbidities have been shown to impact the safety of OIT for other food allergies and in older patients. However, no data exist on which factors predict safety of peanut OIT in preschool populations.
Dr. Chan[/caption]
Edmond S. Chan MD, FRCPC, FCSACI, FAAAAI
Head | Division of Allergy & Immunology | Department of Pediatrics, Faculty of Medicine
Clinical Professor, The University of British Columbia
Clinical Investigator, BC Children's Hospital Research Institute
BC Children's Hospital, Allergy Clinic
Vancouver, BC Canada
Treasurer, CSACI (Canadian Society of Allergy & Clinical Immunology)
MedicalResearch.com: What prompted you to look at the safety of peanut oral immunotherapy specifically in this patient population?
Response: Our previous research has investigated the overall safety of peanut oral immunotherapy (OIT) in preschool populations. However, we have not investigated the relationship between specific patient characteristics and the safety of OIT. Previous literature has shown that patient factors, such as age, gender, baseline sIgE levels, and atopic comorbidities have been shown to impact the safety of OIT for other food allergies and in older patients. However, no data exist on which factors predict safety of peanut OIT in preschool populations.
 Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.
Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.

 Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"] Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely.
Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely. 
 Dr. Leonard[/caption]
Dr. Cathy Leonard PhD
Department of Infection and Immunity
Luxembourg Institute of Health
Luxembourg
MedicalResearch.com: What is the background for this study?
Response: Cat allergy is a rapidly increasing phenomenon characterized by hypersensitivity and an excessive immune response to certain allergens associated with cats, among which the major allergen Fel d 1, a protein typically found in their saliva, on their skin and fur. Cat allergy manifestations can range from mild forms like itchy nose or sneezing to the development of severe symptoms such as rhinitis and asthma, with potentially fatal outcomes.
Only Allergen‐specific immunotherapy (AIT )can ensure an effective and longer lasting treatment in the more advanced cases. AIT typically consists in the subcutaneous injection of gradually increasing doses of the allergen of interest, until a critical quantity is reached that induces long-term immune tolerance. Nevertheless, there is still the need to improve cat AIT in terms of efficacy and safety. We hypothesized that immune tolerance to the allergen could be boosted by improving the adjuvanticity of AIT solutions, thereby optimizing the production of antibodies against Fel d 1, while minimizing inflammation.
Dr. Leonard[/caption]
Dr. Cathy Leonard PhD
Department of Infection and Immunity
Luxembourg Institute of Health
Luxembourg
MedicalResearch.com: What is the background for this study?
Response: Cat allergy is a rapidly increasing phenomenon characterized by hypersensitivity and an excessive immune response to certain allergens associated with cats, among which the major allergen Fel d 1, a protein typically found in their saliva, on their skin and fur. Cat allergy manifestations can range from mild forms like itchy nose or sneezing to the development of severe symptoms such as rhinitis and asthma, with potentially fatal outcomes.
Only Allergen‐specific immunotherapy (AIT )can ensure an effective and longer lasting treatment in the more advanced cases. AIT typically consists in the subcutaneous injection of gradually increasing doses of the allergen of interest, until a critical quantity is reached that induces long-term immune tolerance. Nevertheless, there is still the need to improve cat AIT in terms of efficacy and safety. We hypothesized that immune tolerance to the allergen could be boosted by improving the adjuvanticity of AIT solutions, thereby optimizing the production of antibodies against Fel d 1, while minimizing inflammation. 

 Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
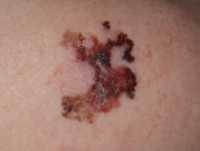
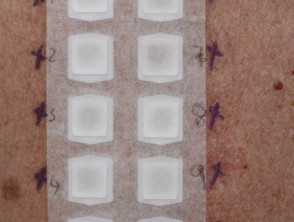
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series. Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.
Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.


 Dr. Senior[/caption]
Brent A. Senior, MD, FACS, FARS
Professor of Otolaryngology/Neurosurgery
Vice Chairman for Clinical Affairs
Nathaniel and Sheila Harris Distinguished Professor
Chief, Division of Rhinology, Allergy, and Endoscopic Skull Base Surgery
Department of Otolaryngology-Head and Neck Surgery
University of North Carolina at Chapel Hill
Chapel Hill, NC
MedicalResearch.com: What is the background for this study? How common is the problem of chronic rhinosinusitis with nasal polyps?
Response: Chronic rhinosinusitis (CRS) is a very common illness in the United States and around the world, estimated to impact 2-14% of the US population. Chronic rhinosinusitis with polyps is a particularly challenging form of the disease marked by significant impact on quality of life, and being challenging to treat with significant recurrences of symptoms despite standard medical and surgical treatment.
Inhaled intranasal steroids are standard therapy for patients with CRS including those with nasal polyps. However, many patients continue to have significant nasal symptoms despite treatment with these medications. This study was designed to answer the question of whether patients who had been receiving treatment with inhaled intranasal steroids and failed were improved by using EDS-FLU. Results were obtained by pooling data from two previous studies of the use of EDS-FLU in patients with CRS, called Navigate 1 and 2.
Dr. Senior[/caption]
Brent A. Senior, MD, FACS, FARS
Professor of Otolaryngology/Neurosurgery
Vice Chairman for Clinical Affairs
Nathaniel and Sheila Harris Distinguished Professor
Chief, Division of Rhinology, Allergy, and Endoscopic Skull Base Surgery
Department of Otolaryngology-Head and Neck Surgery
University of North Carolina at Chapel Hill
Chapel Hill, NC
MedicalResearch.com: What is the background for this study? How common is the problem of chronic rhinosinusitis with nasal polyps?
Response: Chronic rhinosinusitis (CRS) is a very common illness in the United States and around the world, estimated to impact 2-14% of the US population. Chronic rhinosinusitis with polyps is a particularly challenging form of the disease marked by significant impact on quality of life, and being challenging to treat with significant recurrences of symptoms despite standard medical and surgical treatment.
Inhaled intranasal steroids are standard therapy for patients with CRS including those with nasal polyps. However, many patients continue to have significant nasal symptoms despite treatment with these medications. This study was designed to answer the question of whether patients who had been receiving treatment with inhaled intranasal steroids and failed were improved by using EDS-FLU. Results were obtained by pooling data from two previous studies of the use of EDS-FLU in patients with CRS, called Navigate 1 and 2.