Allergies, Author Interviews, Immunotherapy / 25.02.2019
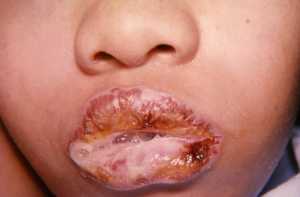
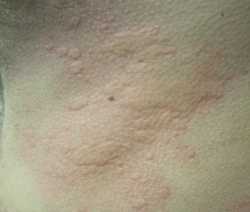
Boiled Peanut Immunotherapy For Peanut Allergy
MedicalResearch.com Interview with:
Dr Paul Turner FRACP PhD
MRC Clinician Scientist and Clinical Senior Lecturer, Imperial College London
Honorary Consultant in Paediatric Allergy & Immunology
Imperial College Healthcare NHS Trust
Hon Consultant, Royal Free Hospital / Royal Brompton & Harefield NHS Foundation Trust
Clinical trials specialist (Paediatrics), Public Health England
Clinical Associate Professor in Paediatrics, University of Sydney, Australia
Dr. Nandinee Patel, MD
Section of Paediatrics
Imperial College London
London, United Kingdom
MRC & Asthma UK Centre in Allergic Mechanisms of Asthma
London, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Current desensitisation protocols for peanut allergy use defatted roasted peanut flour, which can be difficult to accurately measure in very low doses needed for desensitisation (and thus has resulted in the development of AR101 by Aimmune which is likely cost many thousands of dollars for a course of treatment).
We have previously observed that some children with food allergy to roasted peanut (such as peanut butter) are nonetheless able to tolerate boiled peanuts without reacting. We performed in vitro protein analysis studies which demonstrated that boiling peanuts resulted in around 50% of protein leaching out of the peanut into the cooking water. Furthermore, we found evidence for preferential leaching of allergen epitopes such as Ara h 2 as well aggregation of proteins resulting in a hypoallergenic peanut product.
We therefore sought to assess whether boiled peanuts could be as effective and safe to induce desensitisation.



 Dr. Shenoy[/caption]
ESS= Erica S. Shenoy, MD, PhD
Harvard Medical School
Division of Infectious Diseases, Department of Medicine
Massachusetts General Hospital, Boston
[caption id="attachment_47011" align="alignleft" width="150"]
Dr. Shenoy[/caption]
ESS= Erica S. Shenoy, MD, PhD
Harvard Medical School
Division of Infectious Diseases, Department of Medicine
Massachusetts General Hospital, Boston
[caption id="attachment_47011" align="alignleft" width="150"] Dr. Blumenthal[/caption]
KGB= Kimberly G. Blumenthal MD, MSc
Division of Rheumatology, Allergy and Immunology
Department of Medicine, Massachusetts General Hospital,Boston
[caption id="attachment_47012" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
KGB= Kimberly G. Blumenthal MD, MSc
Division of Rheumatology, Allergy and Immunology
Department of Medicine, Massachusetts General Hospital,Boston
[caption id="attachment_47012" align="alignleft" width="100"] Dr. Macy[/caption]
EMM= Eric M. Macy MD, MS
Department of Allergy
Southern California Permanente Medical Group
San Diego Medical Center
[caption id="attachment_47013" align="alignleft" width="150"]
Dr. Macy[/caption]
EMM= Eric M. Macy MD, MS
Department of Allergy
Southern California Permanente Medical Group
San Diego Medical Center
[caption id="attachment_47013" align="alignleft" width="150"] Dr. Rowe[/caption]
TR= Theresa Rowe, DO, MS
General Internal Medicine and Geriatrics
Feinberg School of Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this review?
ESS: A key component of reducing antimicrobial resistance is improving how antimicrobials are prescribed—both reducing inappropriate use (i.e., not prescribing when not needed) and favoring the use of narrow-spectrum agents that are less likely to contribute to the development of antimicrobial resistance.
KGB: Because unverified penicillin allergy labels are so prevalent with greater than 32 million Americans affected, and these labels lead to the use of alternative antibiotics that are often more broad-spectrum, we now know that penicillin allergy evaluations are an emerging important component of antibiotic stewardship. When patients with a reported penicillin allergy are tested, more than 95% of them are not allergic, and thus could (and should) receive penicillins, and often related drugs, when appropriate.
Dr. Rowe[/caption]
TR= Theresa Rowe, DO, MS
General Internal Medicine and Geriatrics
Feinberg School of Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this review?
ESS: A key component of reducing antimicrobial resistance is improving how antimicrobials are prescribed—both reducing inappropriate use (i.e., not prescribing when not needed) and favoring the use of narrow-spectrum agents that are less likely to contribute to the development of antimicrobial resistance.
KGB: Because unverified penicillin allergy labels are so prevalent with greater than 32 million Americans affected, and these labels lead to the use of alternative antibiotics that are often more broad-spectrum, we now know that penicillin allergy evaluations are an emerging important component of antibiotic stewardship. When patients with a reported penicillin allergy are tested, more than 95% of them are not allergic, and thus could (and should) receive penicillins, and often related drugs, when appropriate.


 Mr. Butt[/caption]
Mr. Tosh Butt
Vice President, Respiratory
AstraZeneca
Mr. Butt discusses the recent announcement that the FDA has granted Orphan Drug Designation for Fasenra for the treatment of Eosinophilic Granulomatosis with Polyangiitis.
MedicalResearch.com: What is the background for this announcement? Can you tell us a little more about Eosinophilic Granulomatosis with Polyangiitis/Churg Strauss? How does it differ/resemble severe eosinophilic asthma?
Mr. Butt[/caption]
Mr. Tosh Butt
Vice President, Respiratory
AstraZeneca
Mr. Butt discusses the recent announcement that the FDA has granted Orphan Drug Designation for Fasenra for the treatment of Eosinophilic Granulomatosis with Polyangiitis.
MedicalResearch.com: What is the background for this announcement? Can you tell us a little more about Eosinophilic Granulomatosis with Polyangiitis/Churg Strauss? How does it differ/resemble severe eosinophilic asthma?


 Eliane Abou-Jaoude, MD
Allergy and Immunology Fellow
Henry Ford Health System
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Early life exposure to diverse types of microbes is necessary for healthy immune development and may impact the risk for developing allergic disorders.
Theoretically the transfer of parental microbes to their offspring during infancy can influence a child’s developing gut microbiome and subsequent immune response patterns.
We wished to investigate whether parental pacifier cleaning methods, reported at 6-months of age, were associated with altered serum IgE trajectory over the first 18 months of life.
Eliane Abou-Jaoude, MD
Allergy and Immunology Fellow
Henry Ford Health System
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Early life exposure to diverse types of microbes is necessary for healthy immune development and may impact the risk for developing allergic disorders.
Theoretically the transfer of parental microbes to their offspring during infancy can influence a child’s developing gut microbiome and subsequent immune response patterns.
We wished to investigate whether parental pacifier cleaning methods, reported at 6-months of age, were associated with altered serum IgE trajectory over the first 18 months of life.