Author Interviews, Herpes Viruses, Inflammation, Vaccine Studies / 21.10.2025
ID Week 2025: Shingrix Vaccine for Shingles Associated with Fewer Heart and Brain Adverse Events
[caption id="attachment_71064" align="alignleft" width="200"] Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
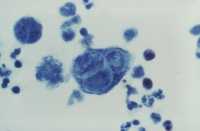
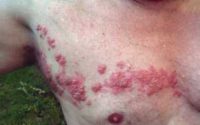
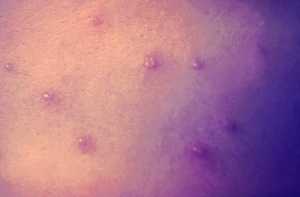
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"]
Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"] CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.
CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.
 Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"]
Dr. Dehghani[/caption]
MedicalResearch.com Interview with:
Ali Dehghani, DO
Department of Medicine
University Hospitals Cleveland Medical Center / Case Western Reserve University
Presenting Author, IDWeek 2025
MedicalResearch.com: What is the background for this study?
Response: Shingles (herpes zoster) is caused by reactivation of the varicella-zoster virus, which can inflame blood vessels and the nervous system. Evidence over the past decade has linked shingles to higher risks of heart attack, stroke, and dementia—but it was unclear whether the shingles vaccine might lessen those long-term effects.
[caption id="attachment_71061" align="aligncenter" width="500"] CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.
CDC PHIL Image[/caption]
MedicalResearch.com: What are the main findings?
Response: Using data from over 100 U.S. health systems, we followed adults age 50 and older for up to five years. We found that people who developed shingles had a 20–30% higher risk of cardiovascular events, vascular dementia, and death compared with similar adults without shingles.
Those who had received the recombinant zoster vaccine (Shingrix) before their infection had substantially lower long-term risks—about 25% fewer major cardiac events, 40% lower early mortality, and nearly 50% less vascular dementia over time.



 Dr. Gandhi[/caption]
Manoj Gandhi, MD PhD
Senior Medical Director of Genetic Testing Services,
Dr. Gandhi[/caption]
Manoj Gandhi, MD PhD
Senior Medical Director of Genetic Testing Services, 
 Dr. Stevermer[/caption]
James Stevermer, M.D., M.S.P.H.
Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
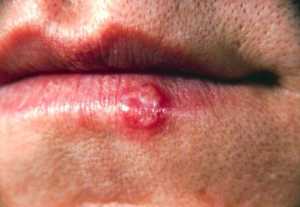
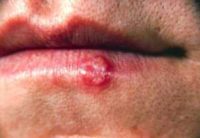
Response: Genital herpes is a common sexually transmitted infection (STI) that unfortunately has no cure and cannot accurately be detected in people who do not have signs of the condition. The current screening tests have limitations and there is a high chance that test results will say a person has the condition when they do not. In addition, the available treatments are focused on managing symptoms and preventing the condition from reoccurring. As a result, the Task Force concluded that the harms of screening outweigh the benefits.
Dr. Stevermer[/caption]
James Stevermer, M.D., M.S.P.H.
Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: Genital herpes is a common sexually transmitted infection (STI) that unfortunately has no cure and cannot accurately be detected in people who do not have signs of the condition. The current screening tests have limitations and there is a high chance that test results will say a person has the condition when they do not. In addition, the available treatments are focused on managing symptoms and preventing the condition from reoccurring. As a result, the Task Force concluded that the harms of screening outweigh the benefits.
 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
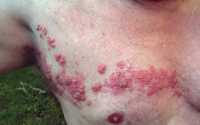
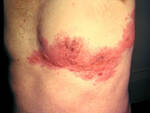
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.