MedicalResearch.com Interview with:
[caption id="attachment_40475" align="alignleft" width="200"]
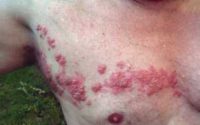
Herpes Zoster or Shingles of chest
Wikipedia[/caption]
Anthony. L. Cunningham, MD
The Westmead Institute for Medical Research
Westmead, NSW
University of Sydney, Sydney,
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study examines the reasons why the HZ subunit vaccine candidate (HZ/su vaccine) consisting of a single viral protein, varicella-zoster glycoprotein E, and and adjuvant (immunostimulant) combination AS01B is so effective as a vaccine to prevent shingles (>90%), especially in those over the age of 70 years and 80 years, as published in recent trials i.e. it combats the declining immunity in the aging which usually restricts vaccine efficacy to under 60% in these age groups.