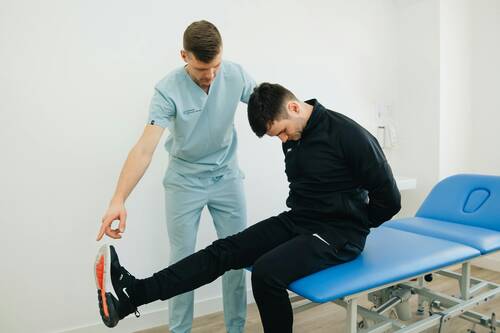
Please be sure to consult with your health care provider for new, severe, changing or unremitting pain.
You should coordinate your chiropractic care with your medical provider. Sponsored post provided for information only, not specific medical advice.

Chiropractic care offers a minimally invasive solution to musculoskeletal issues. Back, neck, and joint pain are some reasons people turn to chiropractic care. Through the alignment of the spinal column, the care promotes overall health. Repeating the treatments increase the function in the body and reduce the use of medication.
Beyond pain reduction, chiropractic care also ensures overall health by aiding nervous function. A well-aligned spinal column provides good communication between the body and the brain. A misaligned spinal column, in contrast, squishes the nervous tissues, resulting in discomfort and less function. Through the maintenance in spinal health, most people feel improved rest, improved digestive function, and improved energy.
One of the most powerful chiropractic treatments lies in the body's ability to heal from illness if only given the support necessary. Rather than simply masking the symptom through medication, this integrated approach targets the root cause of the discomfort. Patients typically suffer from less frequent and less painful episodes if proper care is administered. This makes the operation appealing to individuals who desire long-term remedy and who want to eliminate surgical intervention.
Comprehensive Services at Physio Collective
Physio Collective provides specialized care to accommodate the unique needs of each client. The team uses evidence-based techniques to enhance physical function. From rehabilitation from injury to the reduction of long-term discomfort, they offer treatments to suit each client.
Patients are provided hands-on corrections, therapeutic exercise, and life coaching. In addition to the typical chiropractic manipulations, Physio Collective also utilizes newer modalities to augment outcomes. Joint mobilization, rehabilitative exercise, and myofascial release are all applied in combination to rehabilitate the body.
The treatments re-educate the musculature, realign the posture, and decompress weakened tissues (read more:
https://musculardystrophynews.com/forums/forums/topic/md-and-chiropractors/). Patient education is the priority, and the team makes sure the individual fully understands the condition and how to prevent future issues.
For those who are injured in the office and the sporting world, Physio Collective offers specialized rehabilitation courses. Target rehabilitation to recover from inflammation, return to function, and overall strength building are all included in the course. Treating the symptom and the cause, they rehabilitate the body to optimal function and to reinjury. The model integrated offers each client a specialized course to rehabilitation.
 Dr. Binshtok[/caption]
MedicalResearch.com Interview with:
Prof. Alexander Binshtok PhD
Cecile and Seymour Alpert Professor in Pain Research
Hebrew University’s Faculty of Medicine and Center for Brain Sciences (ELSC)
MedicalResearch.com: What is the background for this study?
Response: Paracetamol (also known as acetaminophen) is one of the world’s most commonly used pain relievers and fever reducers, yet for decades, its precise biological mechanism has remained something of a mystery. Traditionally, scientists believed its analgesic effect stemmed from central nervous system activity—specifically through the action of its metabolite, AM404, on cannabinoid and TRPV1 receptors in the brain.
Dr. Binshtok[/caption]
MedicalResearch.com Interview with:
Prof. Alexander Binshtok PhD
Cecile and Seymour Alpert Professor in Pain Research
Hebrew University’s Faculty of Medicine and Center for Brain Sciences (ELSC)
MedicalResearch.com: What is the background for this study?
Response: Paracetamol (also known as acetaminophen) is one of the world’s most commonly used pain relievers and fever reducers, yet for decades, its precise biological mechanism has remained something of a mystery. Traditionally, scientists believed its analgesic effect stemmed from central nervous system activity—specifically through the action of its metabolite, AM404, on cannabinoid and TRPV1 receptors in the brain.





 Dr. Piper[/caption]
Brian J. Piper, PhD
Department of Medical Education
Center for Pharmacy Innovation & Outcomes
Geisinger College of Health Sciences
Scranton, PA 18509
MedicalResearch.com: What is the background for this study?
Dr. Piper: Tapentadol has an unusual mechanism of action. This opioid is similar to morphine in that it activates mu, the main opiate receptor which is important for pain. This drug also acts similar to an antidepressant like duloxetine (Cymbalta) with equal ability to block both the norepinephrine and the serotonin transporters (Figure 1). The combination of opioid and monoaminergic activity may influence both therapeutic and side effect profiles.
[caption id="attachment_68512" align="aligncenter" width="192"]
Dr. Piper[/caption]
Brian J. Piper, PhD
Department of Medical Education
Center for Pharmacy Innovation & Outcomes
Geisinger College of Health Sciences
Scranton, PA 18509
MedicalResearch.com: What is the background for this study?
Dr. Piper: Tapentadol has an unusual mechanism of action. This opioid is similar to morphine in that it activates mu, the main opiate receptor which is important for pain. This drug also acts similar to an antidepressant like duloxetine (Cymbalta) with equal ability to block both the norepinephrine and the serotonin transporters (Figure 1). The combination of opioid and monoaminergic activity may influence both therapeutic and side effect profiles.
[caption id="attachment_68512" align="aligncenter" width="192"] Figure 1. Biological mechanism of action of the atypical opioid tapentadol involves binding to the mu opiate receptor, blocking the norepinephrine transporter (NET), and blocking the serotonin transporter (SERT) [1].[/caption]Tapentadol is approved in the US for moderate to severe acute pain, moderate to severe chronic pain, and neuropathic pain associated with diabetic peripheral neuropathy. However, tapentadol is not generally considered first-line for any of these indications. Although this agent has a high potential for abuse and is classified as a Schedule II substance, a manufacturer of extended release tapentadol (Grunenthal) has conducted a misinformation campaign claiming tapentadol has a “minimum potential of abuse”, does not cause respiratory depression (a well-known opioid effect), does not cause any euphoric feelings, has no street value, and is not an opioid [2]. Prior pharmacoepidemiological studies have examined the use patterns of other prescription opioids that can be misused like oxycodone [3], fentanyl [4], meperidine [5] and methadone [6] but there is limited national information about the use of tapentadol.
Figure 1. Biological mechanism of action of the atypical opioid tapentadol involves binding to the mu opiate receptor, blocking the norepinephrine transporter (NET), and blocking the serotonin transporter (SERT) [1].[/caption]Tapentadol is approved in the US for moderate to severe acute pain, moderate to severe chronic pain, and neuropathic pain associated with diabetic peripheral neuropathy. However, tapentadol is not generally considered first-line for any of these indications. Although this agent has a high potential for abuse and is classified as a Schedule II substance, a manufacturer of extended release tapentadol (Grunenthal) has conducted a misinformation campaign claiming tapentadol has a “minimum potential of abuse”, does not cause respiratory depression (a well-known opioid effect), does not cause any euphoric feelings, has no street value, and is not an opioid [2]. Prior pharmacoepidemiological studies have examined the use patterns of other prescription opioids that can be misused like oxycodone [3], fentanyl [4], meperidine [5] and methadone [6] but there is limited national information about the use of tapentadol.


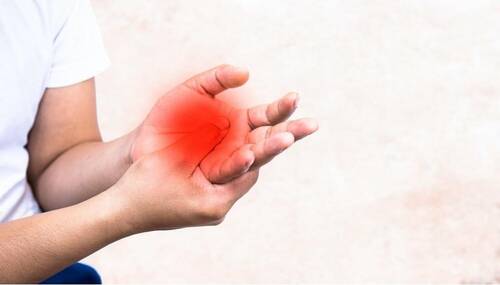


 Chiropractic care offers a minimally invasive solution to musculoskeletal issues. Back, neck, and joint pain are some reasons people turn to chiropractic care. Through the alignment of the spinal column, the care promotes overall health. Repeating the treatments increase the function in the body and reduce the use of medication.
Beyond pain reduction, chiropractic care also ensures overall health by aiding nervous function. A well-aligned spinal column provides good communication between the body and the brain. A misaligned spinal column, in contrast, squishes the nervous tissues, resulting in discomfort and less function. Through the maintenance in spinal health, most people feel improved rest, improved digestive function, and improved energy.
One of the most powerful chiropractic treatments lies in the body's ability to heal from illness if only given the support necessary. Rather than simply masking the symptom through medication, this integrated approach targets the root cause of the discomfort. Patients typically suffer from less frequent and less painful episodes if proper care is administered. This makes the operation appealing to individuals who desire long-term remedy and who want to eliminate surgical intervention.
Chiropractic care offers a minimally invasive solution to musculoskeletal issues. Back, neck, and joint pain are some reasons people turn to chiropractic care. Through the alignment of the spinal column, the care promotes overall health. Repeating the treatments increase the function in the body and reduce the use of medication.
Beyond pain reduction, chiropractic care also ensures overall health by aiding nervous function. A well-aligned spinal column provides good communication between the body and the brain. A misaligned spinal column, in contrast, squishes the nervous tissues, resulting in discomfort and less function. Through the maintenance in spinal health, most people feel improved rest, improved digestive function, and improved energy.
One of the most powerful chiropractic treatments lies in the body's ability to heal from illness if only given the support necessary. Rather than simply masking the symptom through medication, this integrated approach targets the root cause of the discomfort. Patients typically suffer from less frequent and less painful episodes if proper care is administered. This makes the operation appealing to individuals who desire long-term remedy and who want to eliminate surgical intervention.






 Dr. Cheryl Krause-Parello[/caption]
Cheryl A. Krause-Parello, PhD, RN, FAAN
Dr. Cheryl Krause-Parello[/caption]
Cheryl A. Krause-Parello, PhD, RN, FAAN