Author Interviews, Infections / 05.02.2025
NYMC Study Links Newly Discovered Resistant Yeast Infection to Travel from South Asia
MedicalResearch.com Interview with:
[caption id="attachment_66392" align="alignleft" width="200"] Prof. Chaturvedi[/caption]
Prof. Vishnu Chaturvedi, Ph.D., HCLD
Department of Pathology, Microbiology and Immunology
New York Medical College
Department of Pathology, Westchester Medical Center
Valhalla, New York,
MedicalResearch.com: What is the background for this study? How does Candida auris differ from Candida albicans, ie in clinical presentation or treatment?
Prof. Chaturvedi[/caption]
Prof. Vishnu Chaturvedi, Ph.D., HCLD
Department of Pathology, Microbiology and Immunology
New York Medical College
Department of Pathology, Westchester Medical Center
Valhalla, New York,
MedicalResearch.com: What is the background for this study? How does Candida auris differ from Candida albicans, ie in clinical presentation or treatment?
 Prof. Chaturvedi[/caption]
Prof. Vishnu Chaturvedi, Ph.D., HCLD
Department of Pathology, Microbiology and Immunology
New York Medical College
Department of Pathology, Westchester Medical Center
Valhalla, New York,
MedicalResearch.com: What is the background for this study? How does Candida auris differ from Candida albicans, ie in clinical presentation or treatment?
Prof. Chaturvedi[/caption]
Prof. Vishnu Chaturvedi, Ph.D., HCLD
Department of Pathology, Microbiology and Immunology
New York Medical College
Department of Pathology, Westchester Medical Center
Valhalla, New York,
MedicalResearch.com: What is the background for this study? How does Candida auris differ from Candida albicans, ie in clinical presentation or treatment?
- Candida aurisis a newly discovered yeast that is considered a global health threat by the CDC and WHO. The sudden emergence and rapid spread of this multidrug-resistant pathogen is being explained by several published hypotheses. These include global warming, salt water tolerance, or agriculture use of fungicides as plausible causes. In the US, the NY-NJ metropolitan area was the first to suffer from drug-resistant Candia auris clade I genotype. None of the earlier hypotheses could explain the appearance in NY-NJ. Here, we set out to answer two related questions: “why NY-NJ?” and “why clade I?”
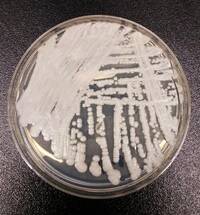
- Candida albicansis a well-known commensal yeast that frequents human mucosal surfaces in the mouth, vagina, etc. In contrast, Candida auris is a newly discovered yeast that colonizes the skin of hospitalized patients and long-term care residents. A small subset of those colonized develop Candida auris bloodstream and deep tissue infections.
- Candida auris differs from albicans in its ability to cause healthcare-associated infection outbreaks. Candida auris is also prone to rapid acquisition of the resistance of multiple antifungal drugs. Finally, C. auris bloodstream infections cause high mortality.


![MedicalResearch.com Interview with: David M. Aronoff, MD, FIDSA, FAAM Professor & Addison B. Scoville Jr. Chair in Medicine Director, Division of Infectious Diseases Department of Medicine Vanderbilt University Medical Center MedicalResearch.com: What is the background for this study? Response: Clostridium difficile infection (CDI) is a major cause of antibiotic-associated colitis and diarrhea and a leading cause of hospital-acquired infection. It is caused by the toxin-producing, anaerobic, spore-forming bacterium Clostridium difficile. Antibiotic use is a major risk factor for CDI but epidemiological studies suggest that other factors, some modifiable, some not, can also increase the risk for CDI. Older age is an example of a non-modifiable risk factor for CDI. Some epidemiological studies suggested that taking the prostaglandin synthesis inhibiting drugs called non-steroidal anti-inflammatory drugs (NSAIDs) might also increase the risk for CDI. NSAIDs include medications such as ibuprofen, naproxen, indomethacin, and others. Because NSAID use is so common, if it is a risk factor for the acquisition of, or severity of, CDI, that would be important because that would be a modifiable risk factor. We therefore sought to determine the impact of NSAID exposure on CDI severity in a mouse model of antibiotic-associated CDI. We also sought evidence for possible mechanisms whereby NSAIDs might increase the risk for CDI. MedicalResearch.com: What are the main findings? Response: Exposure of mice to indomethacin (an NSAID) for two days prior to infection with Clostridium difficile in antibiotic-exposed mice increased the severity of disease and this was associated with severe inflammation, changes to the bacterial populations in the colon and increased damage to the protective epithelial lining of the colon. MedicalResearch.com: What should readers take away from your report? Response: Our studies provide evidence in a mouse model of CDI that support human epidemiological studies linking NSAID use with CDI. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: Studies in humans are needed to see if NSAID use is indeed a causal risk factor for CDI acquisition or severity. MedicalResearch.com: Is there anything else you would like to add? Response: This work was funded by the National Institutes of Health and the Crohn’s and Colitis Foundation of America. Dr. Aronoff has served as Consultant for Synthetic Biologics, Inc, Biocidium, NAEJA-RGM and BLC-USA on projects unrelated to this study. He also has research funding from Pfizer unrelated to this study. Citation: Damian Maseda, Joseph P. Zackular, Bruno Trindade, Leslie Kirk, Jennifer Lising Roxas, Lisa M. Rogers, Mary K. Washington, Liping Du, Tatsuki Koyama, V. K. Viswanathan, Gayatri Vedantam, Patrick D. Schloss, Leslie J. Crofford, Eric P. Skaar, David M. Aronoff. Nonsteroidal Anti-inflammatory Drugs Alter the Microbiota and Exacerbate Clostridium difficile Colitis while Dysregulating the Inflammatory Response. mBio, 2019; 10 (1) DOI: 10.1128/mBio.02282-18 [wysija_form id="3"] [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/Dr-David-M.-Aronoff.jpg)