Medical Billing, Neurological Disorders / 29.05.2026
What Neurological Patients Should Know Before Disputing a Medical Bill?
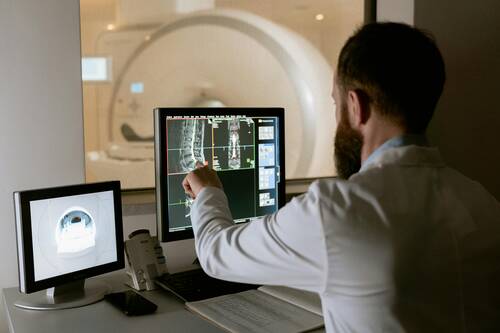
[caption id="attachment_74019" align="aligncenter" width="500"] Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.
Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.
 Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.
Photo by Kindel Media[/caption]
Medical billing errors affect an estimated 80% of hospital bills in the United States, according to a study published in the Journal of the American Medical Association. For neurological patients, the risk is even higher. Neurology involves a dense set of procedure codes, specialist fees, and payer-specific rules that create more opportunities for errors.
Disputing a neurology bill is not the same as disputing a general medical charge. The procedures involved, electroencephalograms (EEGs), electromyography (EMG), nerve conduction studies, and brain imaging, each carry specific Current Procedural Terminology (CPT) codes. A single miscoded test can add hundreds of dollars to a patient's bill.
This guide covers the most common neurology billing errors, how to read and challenge an itemized bill, and what New York patients specifically need to know about their legal rights. It also explains what proper neurology billing services look like from the provider side, and why that matters for what lands on your bill.