Orthopedics, Pain Research / 08.04.2026
The Evolution of Evidence-Based Therapy for Knee Pain in Modern Orthopaedics
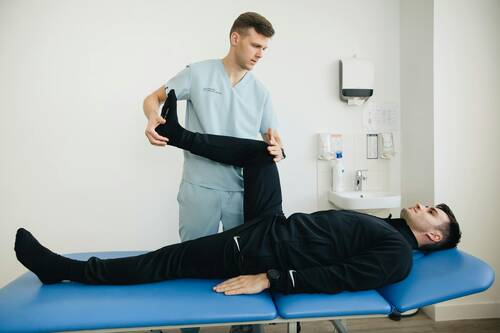
[caption id="attachment_73151" align="aligncenter" width="500"] Photo by Towfiqu barbhuiya[/caption]
Musculoskeletal research has undergone a significant transformation over the last decade. Historically, patients presenting with chronic joint degeneration were often directed toward invasive surgical procedures or relied heavily on pharmacological interventions to mask their symptoms. Today, clinical paradigms have shifted profoundly toward conservative joint preservation. Recent updates in orthopaedic care emphasise managing osteoarthritis pain without relying on medication, noting that targeted physical therapy, weight management, and customised movement regimens can be truly transformative in preserving long-term joint function.
This transition away from immediate surgery is not merely a passing medical trend but a rigorously validated approach supported by extensive clinical trials and peer-reviewed data. As the global population ages, researchers continue to explore robust pathways to delay or entirely prevent the need for joint replacements, focusing instead on sustainable biomechanical correction.
Photo by Towfiqu barbhuiya[/caption]
Musculoskeletal research has undergone a significant transformation over the last decade. Historically, patients presenting with chronic joint degeneration were often directed toward invasive surgical procedures or relied heavily on pharmacological interventions to mask their symptoms. Today, clinical paradigms have shifted profoundly toward conservative joint preservation. Recent updates in orthopaedic care emphasise managing osteoarthritis pain without relying on medication, noting that targeted physical therapy, weight management, and customised movement regimens can be truly transformative in preserving long-term joint function.
This transition away from immediate surgery is not merely a passing medical trend but a rigorously validated approach supported by extensive clinical trials and peer-reviewed data. As the global population ages, researchers continue to explore robust pathways to delay or entirely prevent the need for joint replacements, focusing instead on sustainable biomechanical correction.
 Photo by Towfiqu barbhuiya[/caption]
Musculoskeletal research has undergone a significant transformation over the last decade. Historically, patients presenting with chronic joint degeneration were often directed toward invasive surgical procedures or relied heavily on pharmacological interventions to mask their symptoms. Today, clinical paradigms have shifted profoundly toward conservative joint preservation. Recent updates in orthopaedic care emphasise managing osteoarthritis pain without relying on medication, noting that targeted physical therapy, weight management, and customised movement regimens can be truly transformative in preserving long-term joint function.
This transition away from immediate surgery is not merely a passing medical trend but a rigorously validated approach supported by extensive clinical trials and peer-reviewed data. As the global population ages, researchers continue to explore robust pathways to delay or entirely prevent the need for joint replacements, focusing instead on sustainable biomechanical correction.
Photo by Towfiqu barbhuiya[/caption]
Musculoskeletal research has undergone a significant transformation over the last decade. Historically, patients presenting with chronic joint degeneration were often directed toward invasive surgical procedures or relied heavily on pharmacological interventions to mask their symptoms. Today, clinical paradigms have shifted profoundly toward conservative joint preservation. Recent updates in orthopaedic care emphasise managing osteoarthritis pain without relying on medication, noting that targeted physical therapy, weight management, and customised movement regimens can be truly transformative in preserving long-term joint function.
This transition away from immediate surgery is not merely a passing medical trend but a rigorously validated approach supported by extensive clinical trials and peer-reviewed data. As the global population ages, researchers continue to explore robust pathways to delay or entirely prevent the need for joint replacements, focusing instead on sustainable biomechanical correction.