Author Interviews, Diabetes, NEJM / 09.02.2023
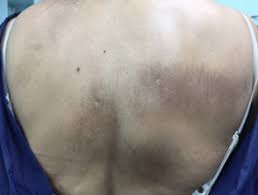
NEJM: New Oral Medication Addresses Common Itchy Back Condition
MedicalResearch.com Interview with:
[caption id="attachment_59985" align="alignleft" width="200"] Dr. Kim[/caption]
Brian S Kim, MD, MTR
Sol and Clara Kest Professor
Vice Chair of Research | Site Chair, Mount Sinai West and Morningside
Director, Mark Lebwohl Center for Neuroinflammation and Sensation
The Kimberly and Eric J. Waldman Department of Dermatology
Precision Immunology Institute | Friedman Brain Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: We generated preliminary data in mice that difelikefalin suppresses itch robustly with very little to no effect on inflammation in a model of atopic dermatitis. This led us to hypothesize that the primary mode of action of difelikefalin must be by direct modulation of sensory neurons to suppress itch and thus would be best suited for a neuropathic itch condition. These are conditions in which itch occurs relatively independently of skin inflammation as in atopic dermatitis due to hyperactive nerves.
Dr. Kim[/caption]
Brian S Kim, MD, MTR
Sol and Clara Kest Professor
Vice Chair of Research | Site Chair, Mount Sinai West and Morningside
Director, Mark Lebwohl Center for Neuroinflammation and Sensation
The Kimberly and Eric J. Waldman Department of Dermatology
Precision Immunology Institute | Friedman Brain Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: We generated preliminary data in mice that difelikefalin suppresses itch robustly with very little to no effect on inflammation in a model of atopic dermatitis. This led us to hypothesize that the primary mode of action of difelikefalin must be by direct modulation of sensory neurons to suppress itch and thus would be best suited for a neuropathic itch condition. These are conditions in which itch occurs relatively independently of skin inflammation as in atopic dermatitis due to hyperactive nerves.
 Dr. Kim[/caption]
Brian S Kim, MD, MTR
Sol and Clara Kest Professor
Vice Chair of Research | Site Chair, Mount Sinai West and Morningside
Director, Mark Lebwohl Center for Neuroinflammation and Sensation
The Kimberly and Eric J. Waldman Department of Dermatology
Precision Immunology Institute | Friedman Brain Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: We generated preliminary data in mice that difelikefalin suppresses itch robustly with very little to no effect on inflammation in a model of atopic dermatitis. This led us to hypothesize that the primary mode of action of difelikefalin must be by direct modulation of sensory neurons to suppress itch and thus would be best suited for a neuropathic itch condition. These are conditions in which itch occurs relatively independently of skin inflammation as in atopic dermatitis due to hyperactive nerves.
Dr. Kim[/caption]
Brian S Kim, MD, MTR
Sol and Clara Kest Professor
Vice Chair of Research | Site Chair, Mount Sinai West and Morningside
Director, Mark Lebwohl Center for Neuroinflammation and Sensation
The Kimberly and Eric J. Waldman Department of Dermatology
Precision Immunology Institute | Friedman Brain Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: We generated preliminary data in mice that difelikefalin suppresses itch robustly with very little to no effect on inflammation in a model of atopic dermatitis. This led us to hypothesize that the primary mode of action of difelikefalin must be by direct modulation of sensory neurons to suppress itch and thus would be best suited for a neuropathic itch condition. These are conditions in which itch occurs relatively independently of skin inflammation as in atopic dermatitis due to hyperactive nerves.

 Dr. Liedtke[/caption]
Wolfgang Liedtke, M.D., Ph.D.
Professor (tenured) of Neurology, Anesthesiology and Neurobiology
Dr. Liedtke[/caption]
Wolfgang Liedtke, M.D., Ph.D.
Professor (tenured) of Neurology, Anesthesiology and Neurobiology
 Dr. Yosipovitch[/caption]
Gil Yosipovitch, MD, Professor
Miami Itch Center
Lennar Medical Foundation
South Miami Clinic in Coral Gables
University of Miami Health System
MedicalResearch.com: What is the background for this study?
Response: Chronic Pruritus is a common and burdensome condition in patients with end stage chronic kidney disease (CKD). It is Present at all stages of CKD, not only in patients undergoing hemodialysis (including stage 3-5 CKD). There are no approved treatments for this condition in US and Europe. CKD pruritus has significant impact on quality of life of patients with higher mortality rates due to its effect on sleep.
Studies in the last 2 decades have shown that in patients with CKD pruritus there is an imbalance between endogenous mu opioids that are over expressed to Kappa Opioids that are down regulated.
Difelikefalin (DFK) is a novel peripherally selective kappa opioid receptor (KOR) agonist. Study of IV DFK administration in hemodialysis patients has recently been published and showed significant anti Pruritic effect ( NEJM Fishbane et al. 382: 289-290, 2020).
Dr. Yosipovitch[/caption]
Gil Yosipovitch, MD, Professor
Miami Itch Center
Lennar Medical Foundation
South Miami Clinic in Coral Gables
University of Miami Health System
MedicalResearch.com: What is the background for this study?
Response: Chronic Pruritus is a common and burdensome condition in patients with end stage chronic kidney disease (CKD). It is Present at all stages of CKD, not only in patients undergoing hemodialysis (including stage 3-5 CKD). There are no approved treatments for this condition in US and Europe. CKD pruritus has significant impact on quality of life of patients with higher mortality rates due to its effect on sleep.
Studies in the last 2 decades have shown that in patients with CKD pruritus there is an imbalance between endogenous mu opioids that are over expressed to Kappa Opioids that are down regulated.
Difelikefalin (DFK) is a novel peripherally selective kappa opioid receptor (KOR) agonist. Study of IV DFK administration in hemodialysis patients has recently been published and showed significant anti Pruritic effect ( NEJM Fishbane et al. 382: 289-290, 2020).
