Author Interviews, Boehringer Ingelheim, NEJM, Pharmaceutical Companies, Pulmonary Disease / 30.05.2019
Systemic Sclerosis (scleroderma): Nintedanib Slowed Loss of Pulmonary Function
MedicalResearch.com Interview with:
[caption id="attachment_49455" align="alignleft" width="200"] Dr. Zoz[/caption]
Donald Zoz, M.D.,
Senior associate director
Clinical Development & Medical Affairs
Boehringer Ingelheim Pharmaceuticals, Inc.
MedicalResearch.com: What is the background for this study? How does nintedanib differ from other treatments for SSc-ILD? What are the main findings?
Response: SENSCIS is a Phase III double-blind, randomized placebo-controlled trial that included 576 patients in 32 countries. It is the largest trial to have been conducted in patients with systemic sclerosis associated interstitial lung disease (SSc-ILD). The primary endpoint was the annual rate of decline in forced vital capacity (FVC) over 52 weeks. At the end of the 52-week trial, patients receiving nintedanib had an adjusted annual rate of decline in FVC (mL/year) of -52.4 with nintedanib versus -93.3 with placebo (absolute difference 41.0mL/year [95% CI 2.9, 79.0]; p=0.04). This corresponds to a relative difference of 44% reduction in lung function decline.
There are currently no approved treatments for SSc-ILD., BI conducted the SENSCIS study to evaluate in SSc-ILD patients the impact of nintedanib. Nintedanib, a selective tyrosine kinase inhibitor, is an antifibrotic agent.
Results of the study, which were published in The New England Journal of Medicine and presented at the American Thoracic Society (ATS) International Conference, showed that nintedanib slowed the loss of pulmonary function by 44% in patients with SSc-ILD relative to placebo, as measured by FVC over 52 weeks.
Dr. Zoz[/caption]
Donald Zoz, M.D.,
Senior associate director
Clinical Development & Medical Affairs
Boehringer Ingelheim Pharmaceuticals, Inc.
MedicalResearch.com: What is the background for this study? How does nintedanib differ from other treatments for SSc-ILD? What are the main findings?
Response: SENSCIS is a Phase III double-blind, randomized placebo-controlled trial that included 576 patients in 32 countries. It is the largest trial to have been conducted in patients with systemic sclerosis associated interstitial lung disease (SSc-ILD). The primary endpoint was the annual rate of decline in forced vital capacity (FVC) over 52 weeks. At the end of the 52-week trial, patients receiving nintedanib had an adjusted annual rate of decline in FVC (mL/year) of -52.4 with nintedanib versus -93.3 with placebo (absolute difference 41.0mL/year [95% CI 2.9, 79.0]; p=0.04). This corresponds to a relative difference of 44% reduction in lung function decline.
There are currently no approved treatments for SSc-ILD., BI conducted the SENSCIS study to evaluate in SSc-ILD patients the impact of nintedanib. Nintedanib, a selective tyrosine kinase inhibitor, is an antifibrotic agent.
Results of the study, which were published in The New England Journal of Medicine and presented at the American Thoracic Society (ATS) International Conference, showed that nintedanib slowed the loss of pulmonary function by 44% in patients with SSc-ILD relative to placebo, as measured by FVC over 52 weeks.
 Dr. Zoz[/caption]
Donald Zoz, M.D.,
Senior associate director
Clinical Development & Medical Affairs
Boehringer Ingelheim Pharmaceuticals, Inc.
MedicalResearch.com: What is the background for this study? How does nintedanib differ from other treatments for SSc-ILD? What are the main findings?
Response: SENSCIS is a Phase III double-blind, randomized placebo-controlled trial that included 576 patients in 32 countries. It is the largest trial to have been conducted in patients with systemic sclerosis associated interstitial lung disease (SSc-ILD). The primary endpoint was the annual rate of decline in forced vital capacity (FVC) over 52 weeks. At the end of the 52-week trial, patients receiving nintedanib had an adjusted annual rate of decline in FVC (mL/year) of -52.4 with nintedanib versus -93.3 with placebo (absolute difference 41.0mL/year [95% CI 2.9, 79.0]; p=0.04). This corresponds to a relative difference of 44% reduction in lung function decline.
There are currently no approved treatments for SSc-ILD., BI conducted the SENSCIS study to evaluate in SSc-ILD patients the impact of nintedanib. Nintedanib, a selective tyrosine kinase inhibitor, is an antifibrotic agent.
Results of the study, which were published in The New England Journal of Medicine and presented at the American Thoracic Society (ATS) International Conference, showed that nintedanib slowed the loss of pulmonary function by 44% in patients with SSc-ILD relative to placebo, as measured by FVC over 52 weeks.
Dr. Zoz[/caption]
Donald Zoz, M.D.,
Senior associate director
Clinical Development & Medical Affairs
Boehringer Ingelheim Pharmaceuticals, Inc.
MedicalResearch.com: What is the background for this study? How does nintedanib differ from other treatments for SSc-ILD? What are the main findings?
Response: SENSCIS is a Phase III double-blind, randomized placebo-controlled trial that included 576 patients in 32 countries. It is the largest trial to have been conducted in patients with systemic sclerosis associated interstitial lung disease (SSc-ILD). The primary endpoint was the annual rate of decline in forced vital capacity (FVC) over 52 weeks. At the end of the 52-week trial, patients receiving nintedanib had an adjusted annual rate of decline in FVC (mL/year) of -52.4 with nintedanib versus -93.3 with placebo (absolute difference 41.0mL/year [95% CI 2.9, 79.0]; p=0.04). This corresponds to a relative difference of 44% reduction in lung function decline.
There are currently no approved treatments for SSc-ILD., BI conducted the SENSCIS study to evaluate in SSc-ILD patients the impact of nintedanib. Nintedanib, a selective tyrosine kinase inhibitor, is an antifibrotic agent.
Results of the study, which were published in The New England Journal of Medicine and presented at the American Thoracic Society (ATS) International Conference, showed that nintedanib slowed the loss of pulmonary function by 44% in patients with SSc-ILD relative to placebo, as measured by FVC over 52 weeks.


 . Dr. Jacob M. van Laar
Professor and Chair
Dept of Rheumatology & Clinical Immunology
University Medical Center Utrecht
MedicalResearch: What are the main findings of the study?
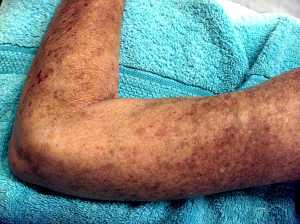
Prof. van Laar: The results of the ASTIS-trial demonstrate that stem cell transplantation in selected patients with early, diffuse cutaneous
. Dr. Jacob M. van Laar
Professor and Chair
Dept of Rheumatology & Clinical Immunology
University Medical Center Utrecht
MedicalResearch: What are the main findings of the study?
Prof. van Laar: The results of the ASTIS-trial demonstrate that stem cell transplantation in selected patients with early, diffuse cutaneous