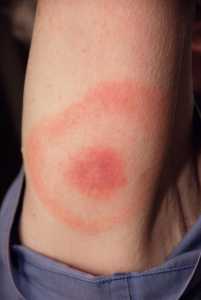
13 Mar New Lyme Disease Model Could Help Track Spread of Tick Disease to Midwest and South
MedicalResearch.com Interview with:
Donal Bisanzio PhD DVM
Senior Epidemiologist
RTI International
MedicalResearch.com: What is the background for this study?
Response: The number of reported cases of Lyme disease has steadily increased since the year 2000. The Centers for Disease Control Prevention (CDC) estimates that nearly 30,000 cases are reported each year with close to 270,000 unreported cases. The high fraction of unreported cases is linked with the absence of specific disease symptoms, which can deter physicians from an initial diagnosis. Another critical factor causing underreporting is the low accuracy of methods used to test Lyme disease. These factors show us that some counties that are currently considered Lyme disease-free may only have this status due to underreporting.
RTI International, in collaboration with Columbia University, built a model to show factors affecting the diffusion of case reporting in the north-eastern U.S. from 2000 to 2017 and identify which counties may be experiencing underreporting. The model used publicly available data published each year by the CDC on cases reported at the county-level merged with information on vector distribution and data obtained by satellite surveys. The model included 855 counties located in 31 states in the West North Central, East North Central, New England, Mid-Atlantic, and Southern regions of the U.S. The final product was a map showing the probability of counties of the north-eastern U.S. to report Lyme disease cases.
MedicalResearch.com: What are the main findings?
Response: Although some of the information has been shown in past studies, the study added a new layer of information—specifically, it took into account characteristics of neighboring counties. Counties that have the right environmental features and have previously reported cases significantly increase the probability of reporting Lyme disease in their neighboring counties. The results of the study could help to identify counties in which no cases have been reported—most likely due to underreporting.
MedicalResearch.com: What should readers take away from your report?
Response: The first aim of the publication is to increase the awareness of readers on the spread of Lyme disease across the North East to the Great Plains and to the South. Another goal was to show that counties without a sutiable habitat for ticks could be reporting cases that could possibly be linked to surrounding counties.
A county that does not have a suitable environment for transmission can still have a high probability of reporting cases if its neighboring counties, with suitable habitats, have reported cases. We believe that taking neighboring counties into account should be seen as a method for capturing people’s exposure outside of their county due to human movement; for example, cases are usually reported in the county where the individual resides, but the disease could have been acquired while they were visiting another county. Looking at our map, physicians may discover that disease-free counties should have already reported cases and may start asking patients more pointed questions about their travel history. The hope is that the data from our publication leads to a decrease in underreporting.
MedicalResearch.com: What recommendations do you have for future research as a result of this work?
Response: I think that future research on Lyme disease should start to account for human movement and its link with exposure to the tick vector in endemic areas. This would be an important step for studying Lyme disease and improving case detection. Mobile phone traffic and social media data from platforms like Twitter and Facebook are good tools to help capture human mobility and should be used in future research.
Another important factor is to identify new areas in which the occurrence of ticks has expanded due to climate change. Updating the map of the tick presence will allow public health institutions to improve surveillance and provide information to populations that do not currently know they could be at risk.
MedicalResearch.com: Is there anything else you would like to add?
Response: Our hope is that public health policy makers and providers use the maps we have created to inform the public and improve surveillance systems. Given the data presented, we should prepare to see an increase in reporting of Lyme disease cases across the U.S. Our hope is that our analyses help inform future studies and are utilized by public health officials in their decision-making process when creating policies involving Lyme disease across the U.S.
Citation:
To read the full study and for more information, please click here: https://www.rti.org/news/new-lyme-disease-model-could-help-identify-areas-high-risk-and-increase-awareness
[subscribe]
Last Modified: [last-modified]
The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.
Last Updated on March 13, 2020 by Marie Benz MD FAAD

