Author Interviews, Brigham & Women's - Harvard, Melatonin, Pediatrics, Sleep Disorders / 28.09.2022
Myths About Teenager Sleep Needs Are Common
MedicalResearch.com Interview with:
[caption id="attachment_59589" align="alignleft" width="150"] Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
 Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.



 Dr. Malin[/caption]
Steven K. Malin, PhD, FACSM (he/him)
Associate Professor
Department of Kinesiology and Health | School of Arts and Sciences
Division of Endocrinology, Metabolism and Nutrition | Robert Wood Johnson Medical School
Institute of Translational Medicine and Science
New Brunswick, NJ 08901
MedicalResearch.com: What is the background for this study?
Response: Type 2 diabetes is a condition where blood glucose (sugar) is elevated in the blood. This can be problematic as it leads to blood vessel damage and the promotion of cardiovascular disease. Nearly 30 million people in the U.S. have type 2 diabetes, making it a major public health issue. The cause is not entirely clear, but many, including our team view insulin resistance as a central culprit.
Insulin resistance is when the body does not respond well to the hormone insulin. Insulin is vital because it promotes glucose uptake into tissues, like skeletal muscle. Two reasons that are often used to explain the development of insulin resistance include: poor diet (e.g. high sugar and/or high fat coupled with excess calories) and a lack of physical activity. However, more recently, a lack of sleep has been raised as another critical behavioral factor contributing to insulin resistance. Thus, targeting a healthy diet, activity and sleep pattern is thought to prevent the transition from health to insulin resistance and type 2 diabetes.
Dr. Malin[/caption]
Steven K. Malin, PhD, FACSM (he/him)
Associate Professor
Department of Kinesiology and Health | School of Arts and Sciences
Division of Endocrinology, Metabolism and Nutrition | Robert Wood Johnson Medical School
Institute of Translational Medicine and Science
New Brunswick, NJ 08901
MedicalResearch.com: What is the background for this study?
Response: Type 2 diabetes is a condition where blood glucose (sugar) is elevated in the blood. This can be problematic as it leads to blood vessel damage and the promotion of cardiovascular disease. Nearly 30 million people in the U.S. have type 2 diabetes, making it a major public health issue. The cause is not entirely clear, but many, including our team view insulin resistance as a central culprit.
Insulin resistance is when the body does not respond well to the hormone insulin. Insulin is vital because it promotes glucose uptake into tissues, like skeletal muscle. Two reasons that are often used to explain the development of insulin resistance include: poor diet (e.g. high sugar and/or high fat coupled with excess calories) and a lack of physical activity. However, more recently, a lack of sleep has been raised as another critical behavioral factor contributing to insulin resistance. Thus, targeting a healthy diet, activity and sleep pattern is thought to prevent the transition from health to insulin resistance and type 2 diabetes.





 Dr. Cano[/caption]
Marlene Cano MD. PhD.
Post-Doctoral Research Fellow in Pulmonary Transplant Immunology
Division of Pulmonary and Critical Care
Department of Medicine
Washington University/Barnes-Jewish Hospital
Saint Louis, MO
MedicalResearch.com: What is the background for this study? How does this test differ from other tests for COVID-19?
Response: We know COVID-19 causes a wide spectrum of disease, and that while many develop only mild uncomplicated illness, others develop severe respiratory failure, multi-organ failure and death. These patients often require prolonged hospitalization, ICU level care and even mechanical intubation for respiratory support. However, we still do not have a great way to identify which patients are likely to develop severe disease. We felt it was important to have a test that could act as sort of a ‘biomarker’ that we could measure early in COVID-19 patients and would help predict which patients would develop severe disease. From prior work, we knew that mitochondrial DNA, which are proinflammatory molecules that are released into the circulation from damaged organs could be this such ‘biomarker’. So, we measured the levels of mitochondrial DNA circulating in the plasma of patients with COVID-19 at the time they first presented to the hospital. Then we investigated if higher levels of mitochondrial DNA indeed predict the development of more severe disease.
Currently there are no ‘biomarker’ tests specific for COVID-19. We do currently measure levels of other markers in the hospital that we feel might help us assess overall how sick patients may be, but these are very non-specific and assess only level of inflammation. This test instead can measure level of tissue injury.
Dr. Cano[/caption]
Marlene Cano MD. PhD.
Post-Doctoral Research Fellow in Pulmonary Transplant Immunology
Division of Pulmonary and Critical Care
Department of Medicine
Washington University/Barnes-Jewish Hospital
Saint Louis, MO
MedicalResearch.com: What is the background for this study? How does this test differ from other tests for COVID-19?
Response: We know COVID-19 causes a wide spectrum of disease, and that while many develop only mild uncomplicated illness, others develop severe respiratory failure, multi-organ failure and death. These patients often require prolonged hospitalization, ICU level care and even mechanical intubation for respiratory support. However, we still do not have a great way to identify which patients are likely to develop severe disease. We felt it was important to have a test that could act as sort of a ‘biomarker’ that we could measure early in COVID-19 patients and would help predict which patients would develop severe disease. From prior work, we knew that mitochondrial DNA, which are proinflammatory molecules that are released into the circulation from damaged organs could be this such ‘biomarker’. So, we measured the levels of mitochondrial DNA circulating in the plasma of patients with COVID-19 at the time they first presented to the hospital. Then we investigated if higher levels of mitochondrial DNA indeed predict the development of more severe disease.
Currently there are no ‘biomarker’ tests specific for COVID-19. We do currently measure levels of other markers in the hospital that we feel might help us assess overall how sick patients may be, but these are very non-specific and assess only level of inflammation. This test instead can measure level of tissue injury.


 Dr. Wei Shan Hoong[/caption]
Dr Caroline Wei Shan Hoong, MBBS, MRCP
Associate Consultant Endocrinologist
Department of General Medicine
Woodlands Health Campus
National Healthcare Group, Singapore
MedicalResearch.com: What is the background for this study?
Response: In the course of our clinical work, we have noticed a predominance of musculoskeletal complaints among some of COVID-19 patients who are otherwise clinically well, and a small subset of them who develop a viral arthralgia (joint pains) sometimes occurring separately from the onset of acute respiratory symptoms. Besides a few isolated case reports, there was not much described about COVID-19 associated viral arthralgia in the literature.
Clinicians are well aware of the need to test for COVID-19 when patients present with cough or shortness of breath. However, when they present as joint pains without any respiratory symptoms, a diagnosis of COVID-19 could easily be missed. Due to overlapping clinical features like low platelet count and elevated liver enzymes, they could easily be misdiagnosed as having other vector-borne infections such as dengue fever, if clinicians do not have a high clinical suspicion of COVID-19. Hence we decided to describe the epidemiology and various presentations of musculoskeletal manifestations of COVID-19 in our cohort of patients.
Dr. Wei Shan Hoong[/caption]
Dr Caroline Wei Shan Hoong, MBBS, MRCP
Associate Consultant Endocrinologist
Department of General Medicine
Woodlands Health Campus
National Healthcare Group, Singapore
MedicalResearch.com: What is the background for this study?
Response: In the course of our clinical work, we have noticed a predominance of musculoskeletal complaints among some of COVID-19 patients who are otherwise clinically well, and a small subset of them who develop a viral arthralgia (joint pains) sometimes occurring separately from the onset of acute respiratory symptoms. Besides a few isolated case reports, there was not much described about COVID-19 associated viral arthralgia in the literature.
Clinicians are well aware of the need to test for COVID-19 when patients present with cough or shortness of breath. However, when they present as joint pains without any respiratory symptoms, a diagnosis of COVID-19 could easily be missed. Due to overlapping clinical features like low platelet count and elevated liver enzymes, they could easily be misdiagnosed as having other vector-borne infections such as dengue fever, if clinicians do not have a high clinical suspicion of COVID-19. Hence we decided to describe the epidemiology and various presentations of musculoskeletal manifestations of COVID-19 in our cohort of patients. 
 Dr. Kim[/caption]
Brian Kim, MD
Associate Professor of Dermatology
Co-Director, Center for the Study of Itch & Sensory Disorders
John T. Milliken Department of Internal Medicine
Washington University in St. Louis
MedicalResearch.com: What is the background for this study?
Response: Patients with eczema suffer from chronic itch due to the rashes they have on their body. However, as a physician, I have always noticed that patients with eczema will have sudden flares of their itching all over there body that is often triggered by what appear to be allergens – being around a cat, pollen, mold in a house, etc. Eczema is in the family of allergic diseases such as food allergy, asthma, and hay fever. All of these conditions are noted for patients being reactive to allergens by way of an antibody called IgE that coats a cell called the mast cell. Upon IgE binding an allergen, mast cells produce tons of histamine which can cause symptoms like itching. So we speculated that perhaps because patients with eczema have such misbehaving IgE, that exposure to allergen is what triggers this kind of severe itch flare that we see in patients.
Dr. Kim[/caption]
Brian Kim, MD
Associate Professor of Dermatology
Co-Director, Center for the Study of Itch & Sensory Disorders
John T. Milliken Department of Internal Medicine
Washington University in St. Louis
MedicalResearch.com: What is the background for this study?
Response: Patients with eczema suffer from chronic itch due to the rashes they have on their body. However, as a physician, I have always noticed that patients with eczema will have sudden flares of their itching all over there body that is often triggered by what appear to be allergens – being around a cat, pollen, mold in a house, etc. Eczema is in the family of allergic diseases such as food allergy, asthma, and hay fever. All of these conditions are noted for patients being reactive to allergens by way of an antibody called IgE that coats a cell called the mast cell. Upon IgE binding an allergen, mast cells produce tons of histamine which can cause symptoms like itching. So we speculated that perhaps because patients with eczema have such misbehaving IgE, that exposure to allergen is what triggers this kind of severe itch flare that we see in patients.




 Dr. Butler[/caption]
Jay C. Butler, MD, FAAP, MACP, FIDSA
Deputy Director for Infectious Diseases
Centers for Disease Control and Prevention
Atlanta, GA 30333
MedicalResearch.com: What is the background for this study?
Response: There are still disagreements about the significance of transmission of SARS-CoV-2 from asymptomatic persons. It has been known since at least March 2020 that, unlike the closely related coronavirus that causes SARS, transmission of COVID-19 from asymptomatic and presymptomatic persons occurs and that at least 30% of infected persons do not develop symptoms. Estimating the proportion of transmissions from persons without symptoms informs the decision analysis for prioritization of community mitigations opportunities: wearing of masks, social distancing, and hand hygiene. If only a low proportion of transmission occurs from people without symptoms, these interventions would be less likely to control transmission when broadly applied in the community. On the other hand, if a significant proportion of spread is from infected persons without symptoms, the value of these measures is enhanced.
Additionally, obtaining strategic and systematic screening tests for SARS-CoV-2 to identify and isolate persons without symptoms in selected settings, such as congregational housing settings, will have greater potential impact if spread from persons without symptoms is common.
Dr. Butler[/caption]
Jay C. Butler, MD, FAAP, MACP, FIDSA
Deputy Director for Infectious Diseases
Centers for Disease Control and Prevention
Atlanta, GA 30333
MedicalResearch.com: What is the background for this study?
Response: There are still disagreements about the significance of transmission of SARS-CoV-2 from asymptomatic persons. It has been known since at least March 2020 that, unlike the closely related coronavirus that causes SARS, transmission of COVID-19 from asymptomatic and presymptomatic persons occurs and that at least 30% of infected persons do not develop symptoms. Estimating the proportion of transmissions from persons without symptoms informs the decision analysis for prioritization of community mitigations opportunities: wearing of masks, social distancing, and hand hygiene. If only a low proportion of transmission occurs from people without symptoms, these interventions would be less likely to control transmission when broadly applied in the community. On the other hand, if a significant proportion of spread is from infected persons without symptoms, the value of these measures is enhanced.
Additionally, obtaining strategic and systematic screening tests for SARS-CoV-2 to identify and isolate persons without symptoms in selected settings, such as congregational housing settings, will have greater potential impact if spread from persons without symptoms is common. 

 Dr. Magnusson[/caption]
Karin Magnusson PT, PhD
Associate Researcher
Lund University and
Norwegian Institute of Public Health
MedicalResearch.com: What is the background for this study?
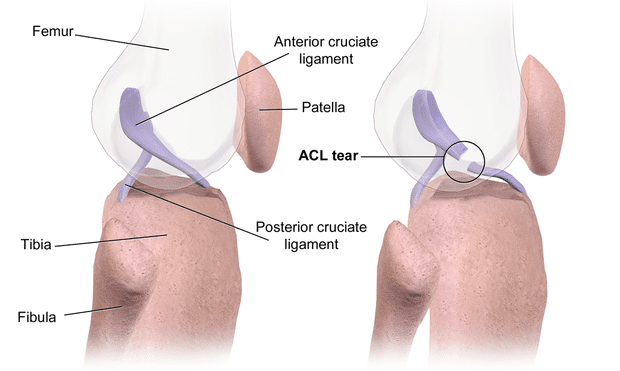
Response: Anterior cruciate ligament (ACL) injury is one of the most common knee injuries, for which very limited data has been presented on the genetic contribution. Based on our knowledge of the role of genetics in the development of ACL-rupture related traits, such as joint hypermobility and knee osteoarthritis, we hypothesized that heritability might play a role also in ACL injury.
Using the Swedish Twin Registry, which is the world's largest twin registry and in this study including more than 88.000 twins, we had unique data to for the first time reliably estimate the heritability for this common knee injury.
Dr. Magnusson[/caption]
Karin Magnusson PT, PhD
Associate Researcher
Lund University and
Norwegian Institute of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anterior cruciate ligament (ACL) injury is one of the most common knee injuries, for which very limited data has been presented on the genetic contribution. Based on our knowledge of the role of genetics in the development of ACL-rupture related traits, such as joint hypermobility and knee osteoarthritis, we hypothesized that heritability might play a role also in ACL injury.
Using the Swedish Twin Registry, which is the world's largest twin registry and in this study including more than 88.000 twins, we had unique data to for the first time reliably estimate the heritability for this common knee injury. 


 Dr. McHill[/caption]
Andrew W. McHill, PhD
Research Assistant Professor
Oregon Institute of Occupational Health Sciences
Oregon Health & Science University, Portland OR
Portland, OR 97239
MedicalResearch.com: What is the background for this study?
Response: It has long been known that there is a home court advantage in sports, whether it be due to the home fans cheering, playing within familiar settings, or travel of the opposing team. However, the contribution of travel to home-court advantage could never be fully teased apart due to all the confounds of the other aspects of playing at home.
In March, the National Basketball Association had to pause their season due to COVID-19 concerns, only to start again several months later with the top 22 teams playing in a “bubble” environment where no teams were required to travel. This created a ‘natural experiment’ wherein we could test the impact of travel on winning and performance before the COVID-19 shutdown with games played in the bubble environment with no travel.
Dr. McHill[/caption]
Andrew W. McHill, PhD
Research Assistant Professor
Oregon Institute of Occupational Health Sciences
Oregon Health & Science University, Portland OR
Portland, OR 97239
MedicalResearch.com: What is the background for this study?
Response: It has long been known that there is a home court advantage in sports, whether it be due to the home fans cheering, playing within familiar settings, or travel of the opposing team. However, the contribution of travel to home-court advantage could never be fully teased apart due to all the confounds of the other aspects of playing at home.
In March, the National Basketball Association had to pause their season due to COVID-19 concerns, only to start again several months later with the top 22 teams playing in a “bubble” environment where no teams were required to travel. This created a ‘natural experiment’ wherein we could test the impact of travel on winning and performance before the COVID-19 shutdown with games played in the bubble environment with no travel.
 Dr. Schmidt[/caption]
William K. Schmidt, Ph.D.
Senior VP Clinical Development
Dr. Schmidt[/caption]
William K. Schmidt, Ph.D.
Senior VP Clinical Development



 Dr. Reed[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Epidemiology
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: It is known that hearing aid ownership is relatively low in the United States at less than 20% of adults with hearing loss owning and using hearing aids. However, many national estimates of hearing aid ownership are based on data that is over 10 years old. Our team was interested in trying to understand whether ownership in hearing aids had changed over time. We used data from 2011 to 2018 in a nationally representative (United States) observational cohort (The National Health and Aging Trends Study) of Medicare Beneficiaries aged 70 years and older to estimate the change in hearing aid ownership.
In our analysis, the proportion of Medicare beneficiaries 70 years and older who reported owning and using their hearing aids increased 23.3% from 2011 to 2018. However, this growth in ownership was not equal across all older adults. For example, while White males saw a 28.7% increase in hearing aid ownership, Black females saw only a 5.8% increase over the same 8-year period. Moreover, adults living at less than 100% federal poverty level actually saw an overall 13.0% decrease in hearing aid ownership while those living at more than 200% federal poverty line saw an overall 30.6% increase.
Dr. Reed[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Epidemiology
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: It is known that hearing aid ownership is relatively low in the United States at less than 20% of adults with hearing loss owning and using hearing aids. However, many national estimates of hearing aid ownership are based on data that is over 10 years old. Our team was interested in trying to understand whether ownership in hearing aids had changed over time. We used data from 2011 to 2018 in a nationally representative (United States) observational cohort (The National Health and Aging Trends Study) of Medicare Beneficiaries aged 70 years and older to estimate the change in hearing aid ownership.
In our analysis, the proportion of Medicare beneficiaries 70 years and older who reported owning and using their hearing aids increased 23.3% from 2011 to 2018. However, this growth in ownership was not equal across all older adults. For example, while White males saw a 28.7% increase in hearing aid ownership, Black females saw only a 5.8% increase over the same 8-year period. Moreover, adults living at less than 100% federal poverty level actually saw an overall 13.0% decrease in hearing aid ownership while those living at more than 200% federal poverty line saw an overall 30.6% increase. 

 Prof. Bergee[/caption]
Martin J. Bergee
Professor and Associate Dean for Academic Affairs
School of Music
University of Kansas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The idea that listening, participating, or achieving in music makes you better at another subject, say, math, science, or reading, has been around for a while. Indeed, there’s a relationship between achievement in music and achievement in other content areas. But I’ve always assumed that the relationship was spurious, that is, driven my any number of such background influences as urbanicity, ethnicity, SES, level of parent education, the type of school one attends, and so forth. Essentially, I set out to demonstrate once and for all that with these background influences accounted for statistically, the relationship is considerably attenuated. Much to my surprise, however, music achievement’s relationships with reading and math achievement remained quite strong.
Prof. Bergee[/caption]
Martin J. Bergee
Professor and Associate Dean for Academic Affairs
School of Music
University of Kansas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The idea that listening, participating, or achieving in music makes you better at another subject, say, math, science, or reading, has been around for a while. Indeed, there’s a relationship between achievement in music and achievement in other content areas. But I’ve always assumed that the relationship was spurious, that is, driven my any number of such background influences as urbanicity, ethnicity, SES, level of parent education, the type of school one attends, and so forth. Essentially, I set out to demonstrate once and for all that with these background influences accounted for statistically, the relationship is considerably attenuated. Much to my surprise, however, music achievement’s relationships with reading and math achievement remained quite strong.