[caption id="attachment_64663" align="aligncenter" width="500"] Source[/caption]
Own a dog? Then your vet must have shared a thing or two about the risks of ticks and even warned you about Lyme disease.
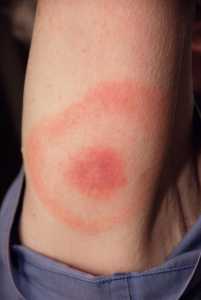
But is your furry friend only at risk of this bacterial infection? You’re wrong if you think so. Humans can also get Lyme disease if a black-legged tick carrying the borrelia bacteria bites them.
Just recently, the comedian and actress Miranda Hart opened up about how she struggled with chronic fatigue syndrome after she was diagnosed with Lyme disease.
Many other famous people say they have been struck by this tick-borne bacterial infection. Those include Real Housewives of Beverly Hills star Yolanda Hadid and her daughter, model Bella Hadid, comic Amy Schumer, actor Ben Stiller, and singer Justin Bieber.
As high-profile names share their struggles, awareness of Lyme is spreading fast. But so are the myths. So, let’s separate the facts from the fiction surrounding this disease.
Source[/caption]
Own a dog? Then your vet must have shared a thing or two about the risks of ticks and even warned you about Lyme disease.
But is your furry friend only at risk of this bacterial infection? You’re wrong if you think so. Humans can also get Lyme disease if a black-legged tick carrying the borrelia bacteria bites them.
Just recently, the comedian and actress Miranda Hart opened up about how she struggled with chronic fatigue syndrome after she was diagnosed with Lyme disease.
Many other famous people say they have been struck by this tick-borne bacterial infection. Those include Real Housewives of Beverly Hills star Yolanda Hadid and her daughter, model Bella Hadid, comic Amy Schumer, actor Ben Stiller, and singer Justin Bieber.
As high-profile names share their struggles, awareness of Lyme is spreading fast. But so are the myths. So, let’s separate the facts from the fiction surrounding this disease.
 Source[/caption]
Own a dog? Then your vet must have shared a thing or two about the risks of ticks and even warned you about Lyme disease.
But is your furry friend only at risk of this bacterial infection? You’re wrong if you think so. Humans can also get Lyme disease if a black-legged tick carrying the borrelia bacteria bites them.
Just recently, the comedian and actress Miranda Hart opened up about how she struggled with chronic fatigue syndrome after she was diagnosed with Lyme disease.
Many other famous people say they have been struck by this tick-borne bacterial infection. Those include Real Housewives of Beverly Hills star Yolanda Hadid and her daughter, model Bella Hadid, comic Amy Schumer, actor Ben Stiller, and singer Justin Bieber.
As high-profile names share their struggles, awareness of Lyme is spreading fast. But so are the myths. So, let’s separate the facts from the fiction surrounding this disease.
Source[/caption]
Own a dog? Then your vet must have shared a thing or two about the risks of ticks and even warned you about Lyme disease.
But is your furry friend only at risk of this bacterial infection? You’re wrong if you think so. Humans can also get Lyme disease if a black-legged tick carrying the borrelia bacteria bites them.
Just recently, the comedian and actress Miranda Hart opened up about how she struggled with chronic fatigue syndrome after she was diagnosed with Lyme disease.
Many other famous people say they have been struck by this tick-borne bacterial infection. Those include Real Housewives of Beverly Hills star Yolanda Hadid and her daughter, model Bella Hadid, comic Amy Schumer, actor Ben Stiller, and singer Justin Bieber.
As high-profile names share their struggles, awareness of Lyme is spreading fast. But so are the myths. So, let’s separate the facts from the fiction surrounding this disease.

 Dr. Dan P. Ly[/caption]
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA
MedicalResearch.com: What is the background for this study?
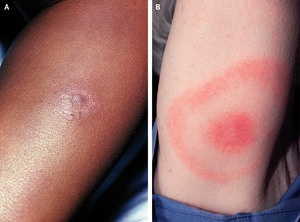
Response: Lyme disease presents first on the skin with the classic “bull’s-eye” rash. But such rashes in Black patients aren’t well-represented in medical textbooks. This may lead to physicians not recognizing such rashes in Black patients.
As a result, Black patients are more likely to present with later complications of Lyme disease when first diagnosed such as neurologic complications.
Dr. Dan P. Ly[/caption]
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA
MedicalResearch.com: What is the background for this study?
Response: Lyme disease presents first on the skin with the classic “bull’s-eye” rash. But such rashes in Black patients aren’t well-represented in medical textbooks. This may lead to physicians not recognizing such rashes in Black patients.
As a result, Black patients are more likely to present with later complications of Lyme disease when first diagnosed such as neurologic complications.